Abstract
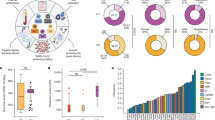
Various biomarkers have been investigated with regard to their ability to predict the outcome of allogeneic hematopoietic SCT (HSCT). In this study, we retrospectively reviewed 90 recipients who received HSCT between 2007 and 2011 in our institution, and evaluated the predictive value of the baseline serum C-reactive protein (CRP) levels just before the initiation of conditioning for transplant-related complications after allogeneic HSCT. A receiver-operating characteristic curve revealed that the baseline serum CRP levels had an excellent predictive value for non-relapse mortality (NRM), with an area under the curve of 0.83. The sensitivity and specificity for NRM were 80% and 87%, respectively, with a cutoff of 0.6 mg/dL. With this cutoff value, multivariate analyses revealed that a higher baseline CRP level was an independent risk factor for NRM (HR 6.21, P<0.01), grade III–IV acute GVHD (HR 3.91, P=0.03) and poor overall survival (HR 3.27, P=0.0018). On the other hand, the baseline CRP level did not predict infectious events. These findings suggested that CRP levels before conditioning may be a useful predictive biomarker for poor survival.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Pepys MB, Baltz ML . Acute phase proteins with special reference to C-reactive protein and related proteins (pentaxins) and serum amyloid A protein. Adv Immunol 1983; 34: 141–212.
Sato M, Kako S, Oshima K, Sato K, Terasako K, Kimura S et al. Prediction of infectious events by high-sensitivity C-reactive protein level before undergoing chemotherapy for acute myeloid leukaemia. Scand J Infect Dis 2010; 42: 97–101.
Przepiorka D, Weisdorf D, Martin P, Klingemann HG, Beatty P, Hows J et al. 1994 Consensus Conference on Acute GVHD. Bone Marrow Transplant 1995; 15: 825–828.
Kanda J, Saji H, Fukuda T, Kobayashi T, Miyamura K, Eto T et al. Related transplantation with HLA-1 Ag mismatch in the GVH direction and HLA-8/8 allele-matched unrelated transplantation: a nationwide retrospective study. Blood 2012; 119: 2409–2416.
Nakai K, Kanda Y, Fukuhara S, Sakamaki H, Okamoto S, Kodera Y et al. Value of chemotherapy before allogeneic hematopoietic stem cell transplantation from an HLA-identical sibling donor for myelodysplastic syndrome. Leukemia 2005; 19: 396–401.
Remberger M, Mattsson J . C-reactive protein levels before reduced-intensity conditioning predict outcome after allogeneic stem cell transplantation. Int J Hematol 2010; 92: 161–167.
Artz AS, Wickrema A, Dinner S, Godley LA, Kocherginsky M, Odenike O et al. Pretreatment C-reactive protein is a predictor for outcomes after reduced-intensity allogeneic hematopoietic cell transplantation. Biol Blood Marrow Transplant 2008; 14: 1209–1216.
Kanda J, Mizumoto C, Ichinohe T, Kawabata H, Saito T, Yamashita K et al. Pretransplant serum ferritin and C-reactive protein as predictive factors for early bacterial infection after allogeneic hematopoietic cell transplantation. Bone Marrow Transplant 2010; 46: 208–216.
Ferrara JL, Levine JE, Reddy P, Holler E . Graft-versus-host disease. Lancet 2009; 373: 1550–1561.
Drahovsky D, Dunzendorfer U, Ziegenhagen G, Drahovsky M, Kellen JA . Reevaluation of C-reactive protein in cancer sera by radioimmunoassay and radial immunodiffusion. I. Diagnostic value and use in battery of conventional tumor markers. Oncology 1981; 38: 286–291.
Limper M, de Kruif MD, Duits AJ, Brandjes DP, van Gorp EC . The diagnostic role of procalcitonin and other biomarkers in discriminating infectious from non-infectious fever. J Infect 2010; 60: 409–416.
Koya J, Nannya Y, Ichikawa M, Kurokawa M . The clinical role of procalcitonin in hematopoietic SCT. Bone Marrow Transplant 2012; 47: 1326–1331.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Sato, M., Nakasone, H., Oshima, K. et al. Prediction of transplant-related complications by C-reactive protein levels before hematopoietic SCT. Bone Marrow Transplant 48, 698–702 (2013). https://doi.org/10.1038/bmt.2012.193
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2012.193
Keywords
This article is cited by
-
Evaluation of pre-transplant risk assessments in allogeneic hematopoietic cell transplant
Bone Marrow Transplantation (2022)
-
High CRP-albumin ratio predicts poor prognosis in transplant ineligible elderly patients with newly diagnosed acute myeloid leukemia
Scientific Reports (2022)
-
Serum albumin and C-reactive protein as significant predictors of non-relapse mortality in lower gastrointestinal graft-versus-host disease
Annals of Hematology (2020)
-
Net reclassification improvement with serial biomarkers and bed-sided spirometry to early predict the need of organ support during the early post-transplantation in-hospital stay in allogeneic HCT recipients
Bone Marrow Transplantation (2019)
-
Patterns of infection and infection-related mortality in patients with steroid-refractory acute graft versus host disease
Bone Marrow Transplantation (2017)