Abstract
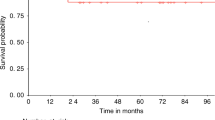
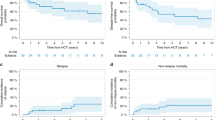
Surveillance of hematopoietic chimerism following hematopoietic SCT (HSCT) with nonmyeloablative (NMA) preparative regimens is standard to assess the need for clinical intervention. Monitoring of donor chimerism following HSCT with myeloablative (MA) preparative regimens is, however, not considered useful because engraftment is thought to occur rapidly and consistently. This study compares the timing of donor hematopoietic cell engraftment in patients undergoing NMA conditioning with fludarabine and TBI with those receiving MA conditioning with BU- or TBI-based regimens. Achievement of ⩾90% donor leukocyte chimerism occurred rapidly and consistently in all three groups and time to achievement of ⩾90% donor T cells was similar among the three groups (P=0.57). Achievement of ⩾90% donor leukocyte chimerism was not associated with risk of acute or chronic GVHD, graft rejection, relapse or all cause mortality in multivariate analyses. Donor T-cell chimerism of ⩾90% was significantly associated with development of extensive chronic GVHD. The value of routine surveillance of chimerism following any of the preparative regimens used in this study should be reevaluated.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Antin JH, Childs R, Filipovich AH, Giralt S, Mackinnon S, Spitzer T et al. Establishment of complete and mixed donor chimerism after allogeneic lymphohematopoietic transplantation: recommendations from a workshop at the 2001 Tandem Meetings of the International Bone Marrow Transplant Registry and the American Society of Blood and Marrow Transplantation. Biol Blood Marrow Transplant 2001; 7: 473–485.
Champlin R, Khouri I, Shimoni A, Gajewski J, Kornblau S, Molldrem J et al. Harnessing graft-versus-malignancy: non-myeloablative preparative regimens for allogeneic haematopoietic transplantation, an evolving strategy for adoptive immunotherapy. Br J Haematol 2000; 111: 18–29.
McSweeney PA, Niederwieser D, Shizuru JA, Sandmaier BM, Molina AJ, Maloney DG et al. Hematopoietic cell transplantation in older patients with hematologic malignancies: replacing high-dose cytotoxic therapy with graft-versus-tumor effects. Blood 2001; 97: 3390–3400.
Mossallam GI, Kamel AM, Storer B, Martin PJ . Prognostic utility of routine chimerism testing at 2 to 6 months after allogeneic hematopoietic cell transplantation. Biol Blood Marrow Transplant 2009; 15: 352–359.
Doney K, Loken M, Bryant E, Smith A, Appelbaum F . Lack of utility of chimerism studies obtained 2-3 months after myeloablative hematopoietic cell transplantation for ALL. Bone Marrow Transplant 2008; 42: 271–274.
Lamba R, Abella E, Kukuruga D, Klein J, Savasan S, Abidi MH et al. Mixed hematopoietic chimerism at day 90 following allogenic myeloablative stem cell transplantation is a predictor of relapse and survival. Leukemia 2004; 18: 1681–1686.
Baron F, Sandmaier BM . Chimerism and outcomes after allogeneic hematopoietic cell transplantation following nonmyeloablative conditioning. Leukemia 2006; 20: 1690–1700.
Sobecks RM, Dean R, Rybicki LA, Chan J, Theil KS, Macklis R et al. 400 cGy TBI with fludarabine for reduced-intensity conditioniong allogeneic hematopoietic stem cell transplantation. Bone Marrow Transplant 2008; 42: 715–722.
Spitzer TR . Nonmyeloablative allogeneic stem cell transplant strategies and the role of mixed chimerism. Oncologist 2000; 5: 215–223.
Sykes M, Preffer F, McAfee S, Saidman SL, Weymouth D, Andrews DM et al. Mixed lymphohaemopoietic chimerism and graft-versus-lymphoma effects after non-myeloablative therapy and HLA-mismatched bone-marrow transplantation. Lancet 1999; 353: 1755–1759.
Maris M, Sandmaier BM, Maloney DG, McSweeney PA, Woolfrey A, Chauncey T et al. Non-myeloablative hematopoietic stem cell transplantation. Transfus Clin Biol 2001; 8: 231–234.
Svenberg P, Mattsson J, Ringden O, Uzunel M . Allogeneic hematopoietic SCT in patients with non-malignant diseases, and importance of chimerism. Bone Marrow Transplant 2009; 44: 757–763.
Saito B, Fukuda T, Yokoyama H, Kurosawa S, Takahashi T, Fuji S et al. Impact of T cell chimerism on clinical outcome in 117 patients who underwent allogeneic stem cell transplantation with a busulfan-containing reduced-intensity conditioning regimen. Biol Blood Marrow Transplant 2008; 14: 1148–1155.
Sugita J, Tanaka J, Hashimoto A, Shiratori S, Yasumoto A, Wakasa K et al. Influence of conditioning regimens and stem cell sources on donor-type chimerism early after stem cell transplantation. Ann Hematol 2008; 87: 1003–1008.
Deeg HJ . Transplantation conditioning regimens: can we say it better? Biol Blood Marrow Transplant 2009; 15: 653–655.
Baron F, Storb R, Gooley T, Sandmaier B, Gisburne S, Shin S et al. Assessing donor chimerism level among CD3 T, CD4 T, CD8 T, and NK cells predicts subsequent graft rejection, GVHD, and relapse after allogeneic HCT with nonmyeloablative conditioning. Biol Blood Marrow Transplant 2005; 11: 11.
Acknowledgements
We thank Shawnda Tench for information related to dosing regimens and Sheila Serafino for information related to laboratory chimerism tests.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Mickelson, D., Sproat, L., Dean, R. et al. Comparison of donor chimerism following myeloablative and nonmyeloablative allogeneic hematopoietic SCT. Bone Marrow Transplant 46, 84–89 (2011). https://doi.org/10.1038/bmt.2010.55
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2010.55
Keywords
This article is cited by
-
Importance of day 21 BM chimerism in sustained neutrophil engraftment following double-unit cord blood transplantation
Bone Marrow Transplantation (2012)
-
Reduced-intensity allografting in patients with therapy-related myeloid neoplasms and active primary malignancies
Bone Marrow Transplantation (2011)