Abstract
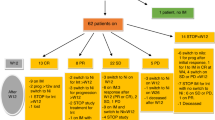
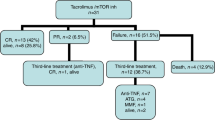
Treatment options for steroid-refractory GVHD (SR-GVHD) are unsatisfactory and prognosis is poor. Inflammatory cytokines IL-2 and TNF-α are important mediators of GVHD and may be critical targets for therapy. We retrospectively reviewed our experience using combination anti-cytokine therapy of daclizumab and infliximab. Seventeen evaluable patients had a median age of 47 years (range 35–63). The conditioning regimen was myeloablative in 13 and non-myeloablative in 4 cases. GVHD occurred at a median of 49 days after transplant in 12 patients (range 21–231 days) and at a median of 46 days (range 25–119 days) after donor lymphocyte infusion in 5 patients. All patients had persistent or progressive GVHD despite 1–2 mg/kg/day of corticosteroids for a median of 7 days (range 2–26 days). They received a combination of daclizumab and infliximab for acute GVHD IBMTR severity index B (3), C (10) or D (4). Of the 17 patients analyzed, 47% responded to treatment, 24% had complete resolution of symptoms and 24% had partial responses. Survival was limited and all the patients died a median of 6.7 months (range 1.6–26) from transplant and 35 days from initiation of daclizumab/infliximab. This retrospective analysis suggests that combination anti-cytokine therapy with daclizumab/infliximab has significant activity in SR-GVHD, but outcomes remain poor. New methods to prevent and treat GVHD are urgently needed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Martin PJ, Schoch G, Fisher L, Byers V, Anasetti C, Appelbaum FR et al. A retrospective analysis of therapy for acute graft-versus-host disease: initial treatment. Blood 1990; 76: 1464–1472.
Weisdorf D, Haake R, Blazar B, Miller W, McGlave P, Ramsay N et al. Treatment of moderate/severe acute graft-versus-host disease after allogeneic bone marrow transplantation: an analysis of clinical risk features and outcome. Blood 1990; 75: 1024–1030.
Roy J, McGlave PB, Filipovich AH, Miller WJ, Blazar BR, Ramsay NK et al. Acute graft-versus-host disease following unrelated donor marrow transplantation: failure of conventional therapy. Bone Marrow Transplant 1992; 10: 77–82.
MacMillan ML, Weisdorf DJ, Wagner JE, DeFor TE, Burns LJ, Ramsay NK et al. Response of 443 patients to steroids as primary therapy for acute graft-versus-host disease: comparison of grading systems. Biol Blood Marrow Transplant 2002; 8: 387–394.
Arai S, Margolis J, Zahurak M, Anders V, Vogelsang GB . Poor outcome in steroid-refractory graft-versus-host disease with antithymocyte globulin treatment. Biol Blood Marrow Transplant 2002; 8: 155–160.
Khoury H, Kashyap A, Adkins DR, Brown RA, Miller G, Vij R et al. Treatment of steroid-resistant acute graft-versus-host disease with anti-thymocyte globulin. Bone Marrow Transplant 2001; 27: 1059–1064.
Martin PJ, Schoch G, Fisher L, Byers V, Appelbaum FR, McDonald GB et al. A retrospective analysis of therapy for acute graft-versus-host disease: secondary treatment. Blood 1991; 77: 1821–1828.
Deeg HJ . How I treat refractory acute GVHD. Blood 2007; 109: 4119–4126.
Ferrara JL, Cooke KR, Teshima T . The pathophysiology of acute graft-versus-host disease. Int J Hematol 2003; 78: 181–187.
Couriel D, Saliba R, Hicks K, Ippoliti C, de Lima M, Hosing C et al. Tumor necrosis factor-alpha blockade for the treatment of acute GVHD. Blood 2004; 104: 649–654.
Przepiorka D, Kernan NA, Ippoliti C, Papadopoulos EB, Giralt S, Khouri I et al. Daclizumab, a humanized anti-interleukin-2 receptor alpha chain antibody, for treatment of acute graft-versus-host disease. Blood 2000; 95: 83–89.
Pidala J, Kim J, Field T, McBride A, Kharfan-Dabaja M, Perkins J et al. Infliximab for managing steroid-refractory acute graft-versus-host disease. Biol Blood Marrow Transplant 2009; 15: 1116–1121.
Perales MA, Ishill N, Lomazow WA, Weinstock DM, Papadopoulos EB, Dastigir H et al. Long-term follow-up of patients treated with daclizumab for steroid-refractory acute graft-vs-host disease. Bone Marrow Transplant 2007; 40: 481–486.
Srinivasan R, Chakrabarti S, Walsh T, Igarashi T, Takahashi Y, Kleiner D et al. Improved survival in steroid-refractory acute graft versus host disease after non-myeloablative allogeneic transplantation using a daclizumab-based strategy with comprehensive infection prophylaxis. Br J Haematol 2004; 124: 777–786.
Rodriguez V, Anderson PM, Trotz BA, Arndt CA, Allen JA, Khan SP . Use of infliximab-daclizumab combination for the treatment of acute and chronic graft-versus-host disease of the liver and gut. Pediatr Blood Cancer 2007; 49: 212–215.
Przepiorka D, Weisdorf D, Martin P, Klingemann HG, Beatty P, Hows J et al. 1994 Consensus conference on acute GVHD grading. Bone Marrow Transplant 1995; 15: 825–828.
Rowlings PA, Przepiorka D, Klein JP, Gale RP, Passweg JR, Henslee-Downey PJ et al. IBMTR severity index for grading acute graft-versus-host disease: retrospective comparison with Glucksberg grade. Br J Haematol 1997; 97: 855–864.
Kaplan EL MP . Non parametric estimation from incomplete observations. J Am Stat Assoc 1958; 53: 457–481.
Cornfield J GT, Smith WW . Quantal response curves for experimentally uncontrolled variables. Bull Int Stat Inst 1961; 38: 97–115.
Antin JH, Chen A, Couriel D, Ho V, Nash RA, Weisdorf D . Novel approaches to the therapy of steroid-resistant acute graft-versus-host disease. Biol Blood Marrow Transplantation 2004; 10: 655–668.
Bordigoni P, Dimicoli S, Clement L, Baumann C, Salmon A, Witz F et al. Daclizumab, an efficient treatment for steroid-refractory acute graft-versus-host disease. Br J Haematol 2006; 135: 382–385.
Kobbe G, Schneider P, Rohr U, Fenk R, Neumann F, Aivado M et al. Treatment of severe steroid refractory acute graft-versus-host disease with infliximab, a chimeric human/mouse antiTNFalpha antibody. Bone Marrow Transplant 2001; 28: 47–49.
Patriarca F, Sperotto A, Damiani D, Morreale G, Bonifazi F, Olivieri A et al. Infliximab treatment for steroid-refractory acute graft-versus-host disease. Haematologica 2004; 89: 1352–1359.
Schmidt-Hieber M, Fietz T, Knauf W, Uharek L, Hopfenmuller W, Thiel E et al. Efficacy of the interleukin-2 receptor antagonist basiliximab in steroid-refractory acute graft-versus-host disease. Br J Haematol 2005; 130: 568–574.
Willenbacher W, Basara N, Blau IW, Fauser AA, Kiehl MG . Treatment of steroid refractory acute and chronic graft-versus-host disease with daclizumab. Br J Haematol 2001; 112: 820–823.
Wolff D, Roessler V, Steiner B, Wilhelm S, Weirich V, Brenmoehl J et al. Treatment of steroid-resistant acute graft-versus-host disease with daclizumab and etanercept. Bone Marrow Transplant 2005; 35: 1003–1010.
Srinivasan R, Geller N, Dorrance C, Espinoza-Delgado I, Barrett AJ, Takahashi Y et al. High response rates and acute steroid refractory graft-versus-host disease (GVHD) following combined tumor necrosis factor alpha (TNF-a) and interleukin-2 (IL-2) blockade. Blood 2005; 106: 1801a.
Rao K, Rao A, Karlsson H, Jagani M, Veys P, Amrolia PJ . Improved survival and preserved antiviral responses after combination therapy with daclizumab and infliximab in steroid-refractory graft-versus-host disease. J Pediatr Hematol Oncol 2009; 31: 456–461.
Marty FM, Lee SJ, Fahey MM, Alyea EP, Soiffer RJ, Antin JH et al. Infliximab use in patients with severe graft-versus-host disease and other emerging risk factors of non-Candida invasive fungal infections in allogeneic hematopoietic stem cell transplant recipients: a cohort study. Blood 2003; 102: 2768–2776.
Lee SJ, Zahrieh D, Agura E, MacMillan ML, Maziarz RT, McCarthy Jr PL et al. Effect of up-front daclizumab when combined with steroids for the treatment of acute graft-versus-host disease: results of a randomized trial. Blood 2004; 104: 1559–1564.
Alousi AM, Weisdorf DJ, Logan BR, Bolanos-Meade J, Carter S, Difronzo N et al. Etanercept, mycophenolate, denileukin, or pentostatin plus corticosteroids for acute graft-versus-host disease: a randomized phase 2 trial from the blood and marrow transplant clinical trials network. Blood 2009; 114: 511–517.
Acknowledgements
This work was supported in part by a grant from the NIH (K24 CA11787901; to DLP).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Rager, A., Frey, N., Goldstein, S. et al. Inflammatory cytokine inhibition with combination daclizumab and infliximab for steroid-refractory acute GVHD. Bone Marrow Transplant 46, 430–435 (2011). https://doi.org/10.1038/bmt.2010.117
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2010.117
Keywords
This article is cited by
-
Treatment and unmet needs in steroid-refractory acute graft-versus-host disease
Leukemia (2020)
-
Ileostomy for steroid-resistant acute graft-versus-host disease of the gastrointestinal tract
Annals of Hematology (2019)
-
The use of basiliximab–infliximab combination for the treatment of severe gastrointestinal acute GvHD
Bone Marrow Transplantation (2016)
-
Ruxolitinib in corticosteroid-refractory graft-versus-host disease after allogeneic stem cell transplantation: a multicenter survey
Leukemia (2015)
-
Long-term follow-up of corticosteroid refractory acute GVHD treated with an Inolimomab-based algorithm: a single center experience
Bone Marrow Transplantation (2013)