Abstract
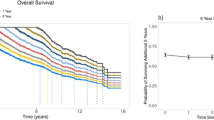
To assess the impact of CR on survival in multiple myeloma. Retrospective evaluation of response and survival among 758 consecutive patients with multiple myeloma treated at a single center, of whom 395 patients received intensive therapy supported by autologous stem cells within the first year. Survival times were calculated after 1 and 2 years from the start of chemotherapy. On the basis of the response status after a 2-year landmark, the subsequent median survival was 9.7 years for patients with CR, 4.4 years for those with PR and 2.7 years for patients with NR (P<0.001). Longer survival was attributed in part to intensive therapy that converted the myeloma of 67% of patients with NR to PR or CR, and induced CR in 26% of patients with PR. Intensive therapy did not prolong survival for patients with CR after primary therapy. For patients with multiple myeloma, Cox regression analyses showed that CR was the dominant prognostic factor for long survival, followed by stage I disease, PR and intensive treatment as independent factors. A cure fraction of 2% was identified for nine patients who have remained in CR >10 years.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Attal M, Harousseau JL, Stoppa AM, Sotto JJ, Fuzibet JG, Rossi JF et al. A prospective, randomized trial of autologous bone marrow transplantation and chemotherapy in multiple myeloma. N Engl J Med 1996; 335: 91–97.
Child J, Morgan G, Davies F, Owen R, Bell S, Hawkins K et al. High-dose chemotherapy with hematopoietic stem-cell rescue for multiple myeloma. N Engl J Med 2003; 348: 1875–1883.
Alexanian R, Barlogie B, Tucker S . VAD-based regimens as primary treatment for multiple myeloma. Am J Hematol 1990; 33: 86–89.
Alexanian R, Dimopoulos M, Delasalle K, Barlogie B . Primary dexamethasone treatment of multiple myeloma. Blood 1992; 80: 887–890.
Weber D, Rankin K, Gavino M, Delasalle K, Alexanian R . Thalidomide alone or with dexamethasone for previously untreated multiple myeloma. J Clin Oncol 2003; 21: 16–19.
Alexanian R, Weber D, Giralt S, Dimopoulos M, Delasalle K, Smith T et al. Impact of complete remission with intensive therapy in patients with responsive multiple myeloma. Bone Marrow Transplant 2001; 27: 1037–1043.
Alexanian R, Weber D, Delasalle K, Handy B, Champlin R, Giralt S . Clinical outcomes with intensive therapy for patients with primary resistant multiple myeloma. Bone Marrow Transplant 2004; 34: 229–234.
Greipp PR, San Miguel J, Durie BG, Crowly J, Barlogie B, Bladé J et al. International staging system for multiple myeloma. J Clin Oncol 2005; 23: 3412–3420.
Blade J, Samson D, Reece D, Apperley J, Björkstrand B, Gahrton G et al. Criteria for evaluating disease response and progression in patients with multiple myeloma treated by high-dose therapy and haemopoietic stem cell transplantation. Br J Haematol 1998; 102: 1115–1123.
Kaplan E, Meier P . Nonparametric estimation from incomplete observations. J Am Stat Assoc 1958; 53: 457–481.
Mantel N . Evaluation of survival data and two new rank order statistics arising in its consideration. Cancer Chemotherapy Rep 1966; 50: 163–170.
Anderson J, Cain K, Gelber R . Analysis of survival by tumor response. J Clin Oncol 1983; 1: 710–719.
Cox D . Regression models and life tables. J Royal Stat Soc 1972; 34: 187–220.
Desikan R, Barlogie B, Sawyer J, Ayers D, Tricot G, Badros A et al. Results of high-dose therapy for 1000 patients with multiple myeloma: durable complete remissions and superior survival in the absence of chromosome 13 abnormalities. Blood 2000; 95: 4008–4010.
Fermand JP, Katsahian S, Divine M, Leblond V, Dreyfus F, Macro M et al. High-dose therapy and autologous blood stem cell transplantation compared with conventional treatment in myeloma patients aged 55–65 years: long-term results of a randomized control trail from the Group Myeloma-Autogreffe. J Clin Oncol 2005; 23: 9227–9233.
Vesole D, Crowley S, Catchatourian R, Stiff P, Johnson D, Cromer J et al. High-dose melphalan with autotransplantation for refractory multiple myeloma. J Clin Oncol 1999; 17: 2173–2179.
Singhal S, Powles R, Sirohi B, Treleaven J, Kulkarni S, Mehta J . Response to induction chemotherapy is not essential to obtain survival benefit from high-dose melphalan and auto-transplantation in myeloma. Bone Marrow Transplant 2002; 30: 673–679.
Kumar S, Lacy MQ, Dispenzieri A, Rajkumar S, Fonseca R, Geyer S et al. High-dose therapy and autologous stem cell transplantation for multiple myeloma poorly responsive to initial therapy. Haematologica 2004; 34: 161–167.
Attal M, Harousseau JL, Facon T, Guilhot F, Doyen C, Fuzibet J et al. Single versus double autologous stem-cell transplantation for multiple myeloma. N Engl J Med 2003; 349: 2495–2502.
Dingli D, Pacheco J, Nowakowski G, Kumar S, Dispenzieri A, Hayman S et al. Relationship between depth of response and outcome in multiple myeloma. J Clin Oncol 2007; 25: 4933–4937.
Kim J, Kim K, Cheong J, Min Y, Suh C, Kim H et al. Complete remission status before autologous stem cell transplantation is an important prognostic factor in patients with multiple myeloma undergoing upfront single autologous transplantation. Biol Blood Marrow Transplant 2009; 15: 463–470.
Lahuerta J, Mateos M, Martinez-Lopez J, Rosiñol L, Sureda A, de la Rubia J et al. Influence of pre- and post-transplantation responses on outcome of patients with multiple myeloma: sequential improvement of response and achievement of complete response are associated with longer survival. J Clin Oncol 2008; 26: 5775–5782.
Kumar S, Dingli D, Dispenzieri A, Lacy M, Hayman S, Buadi F et al. Impact of additional cytoreduction following autologous SCT in multiple myeloma. Bone Marrow Transplant 2008; 42: 259–264.
Durie B, Jacobson J, Barlogie B, Crowley J . Magnitude of response with myeloma frontline therapy does not predict outcomes. J Clin Oncol 2004; 22: 1857–1863.
Barlogie B, Anaissie E, Haessler J, van Rhee F, Pineda-Roman M, Hollmig K et al. Complete remission sustained for 3 years from treatment initiation is a powerful surrogate marker for extended survival in multiple myeloma. Cancer 2008; 113: 355–359.
Barlogie B, Tricot G, van Rhee F, Angtuaco E, Walker R, Epstein J et al. Long-term outcome results of the first tandem autotransplant trial for multiple myeloma. Br J Haemat 2006; 135: 158–164.
Acknowledgements
We are indebted to Monica Miller for typing this paper. This study was supported in part by grants from the National Cancer Institute, CA16672 and 5U01HL69334-08.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, M., Delasalle, K., Feng, L. et al. CR represents an early index of potential long survival in multiple myeloma. Bone Marrow Transplant 45, 498–504 (2010). https://doi.org/10.1038/bmt.2009.176
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2009.176
Keywords
This article is cited by
-
Diffusion-weighted imaging (DWI) in diagnosis, staging, and treatment response assessment of multiple myeloma: a systematic review and meta-analysis
Skeletal Radiology (2023)
-
Benefits of additional cycles of bortezomib/thalidomide/dexamethasone (VTD) induction therapy compared to four cycles of VTD for newly diagnosed multiple myeloma
Bone Marrow Transplantation (2019)
-
Multiple myeloma patients in long-term complete response after autologous stem cell transplantation express a particular immune signature with potential prognostic implication
Bone Marrow Transplantation (2017)
-
Bendamustine, etoposide and dexamethasone to mobilize peripheral blood hematopoietic stem cells for autologous transplantation in patients with multiple myeloma
Bone Marrow Transplantation (2016)
-
Impact of CR before and after allogeneic and autologous transplantation in multiple myeloma: results from the EBMT NMAM2000 prospective trial
Bone Marrow Transplantation (2015)