Abstract
Background:
Molecular characterisation of single circulating tumour cells (CTCs) holds considerable promise for predictive biomarker assessment and to explore CTC heterogeneity. We evaluate a new method, the DEPArray system, that allows the dielectrophoretic manipulation and isolation of single and 100% purified groups of CTCs from pre-enriched blood samples and explore the feasibility of their molecular characterisation.
Methods:
Samples containing known numbers of two cell populations were used to assess cell loss during sample loading. Cultured breast cancer cells were isolated from spiked blood samples using CellSearch CTC and Profile kits. Single tumour cells and groups of up to 10 tumour cells were recovered with the DEPArray system and subjected to transcriptional and mutation analysis.
Results:
On average, 40% cell loss was observed when loading samples to the DEPArray system. Expected mutations in clinically relevant markers could be obtained for 60% of single recovered tumour cells and all groups of tumour cells. Reliable gene expression profiles were obtained from single cells and groups of up to 10 cells for 2 out of 3 spiked breast cancer cell lines.
Conclusion:
We describe a semiautomated workflow for the isolation of small groups of 1 to 10 tumour cells from whole blood samples and provide proof of principle for the feasibility of their comprehensive molecular characterisation.
Similar content being viewed by others
Main
Advances in molecular biology have revolutionised medical oncology. Genome-wide expression profiling and next-generation sequencing studies have revealed considerable, often reproducible, heterogeneity in the molecular constitution of many tumour types (Reis-Filho and Pusztai, 2011; Collisson et al, 2012). In addition, the presence or absence of several specific molecular alterations have been shown to predict response to molecularly targeted treatments (La Thangue and Kerr, 2011). As a consequence, documentation of several of these markers, such as HER2 amplification in patients with breast cancer or the absence of activating KRAS mutations in patients with metastatic colorectal cancer, are now prerequisites before starting treatments targeting the HER2 and EGFR pathway.
Most of our current knowledge on tumour biology originates from the interrogation of the primary tumour, although in general cancer mortality occurs because of the development of metastatic disease (Mehlen and Puisieux, 2006). In clinical practice, the analysis of predictive biomarkers is performed on archival tissue samples from the primary tumour rather than biopsies taken at the time of metastatic progression. Sampling metastatic lesions is often technically difficult or not without risk because of anatomical constraints. Several studies comparing predictive biomarkers on archival primary tumour tissue and metastatic lesions in patients with metastatic breast cancer have documented discordances in up to 25% of cases (Amir et al, 2012; Higgins et al, 2012; Niikura et al, 2012). Even if a biopsy for biomarker assessment is obtained at the time of metastatic disease, patients often exhibit multiple lesions that might be composed of different subclones of tumour cells harbouring different molecular characteristics (Marusyk et al, 2012). In addition, resistance to the selected treatment will eventually occur in virtually all patients. The occurrence of re-responses to EGFR tyrosine kinase inhibitors following previous discontinuation of treatment because of disease progression in patients with non-small-cell lung cancer (Kurata et al, 2004; Riely et al, 2007) further illustrates the dynamics of this process over time. Hence, repetitive probing of drug targets and potential biomarkers for monitoring drug sensitivity and emerging resistance on contemporary tumour samples is essential to allow for more dynamic, individualised treatment planning and monitoring (Diaz et al, 2012; Misale et al, 2012; Shah et al, 2012).
Circulating tumour cells (CTCs) isolated from the blood of patients with metastatic carcinomas provide an attractive source of tumour cells available for such contemporary and repeatable tumour biopsies. The enumeration of CTCs, as performed by the CellSearch System (Veridex LLC, Raritan, NJ, USA), has FDA-approved clinical utility as a prognostic marker in patients with metastatic breast cancer (Cristofanilli et al, 2004), colorectal cancer (Cohen et al, 2008) and prostate cancer (de Bono et al, 2008). In addition, genotypic and phenotypic characterisation of therapeutically or biologically relevant biomarkers expressed by CTCs has been shown to be feasible (Maheswaran et al, 2008; Attard et al, 2009; Ignatiadis et al, 2011; Sieuwerts et al, 2011). Preclinical data furthermore suggest that CTCs seem a more relevant reflection of the dominant subclone of tumour cells in the metastatic compartment (Yu et al, 2012).
The major challenge for the accurate molecular profiling of CTCs is CTC purification. CTCs are outnumbered by white blood cells (WBCs) by a factor of at least 106. Current protocols and technologies enrich rather than purify CTCs, imposing limitations on the feasibility and reliability of measuring CTC-specific markers within the overwhelming WBC background. Potentially even more important, most of the currently available assays do not allow for the evaluation of clonal and molecular heterogeneity within the CTC population.
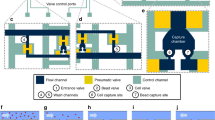
Recently, the DEPArray system (Di-Electro-Phoretic Array system; Silicon Biosystems (SB, Bologna, Italy)), a semiautomated system that allows the isolation of rare cells, such as CTCs, from mixed-cell populations at the single-cell level was developed (Fuchs et al, 2006). With this technique, fluorescently labelled cells can be visualised and isolated by means of a chip consisting of various microelectrodes creating electric cages in which individual CTCs are trapped. Alternatively activating and deactivating the microelectrodes on the chip results in moving the caged cells to a position in the chip that allows the recovery of these cells in a medium suitable for downstream analysis.
The aim of this study was to explore the feasibility to isolate and to molecularly characterise single tumour cells from human blood samples using this technique in a continuous workflow downstream of the CellSearch system, the currently most widely used CTC isolation and enumeration method. We report on the basic analytical aspects of the system and provide proof-of-principle data showing the feasibility to perform both mutation and transcriptional analysis of single tumour cells or small groups of up to 10 tumour cells isolated with the DEPArray from immunomagnetically pre-enriched blood samples.
MATERIALS AND METHODS
Cell lines and culture conditions
The ER+/PR-/HER2+ MDA-MB-361, the ER+/PR+/HER2− MCF7 and the triple-negative MDA-MB-231 human breast cancer cell lines were used for blood spiking experiments. Cell lines were chosen based on the presence of known mutations in the MDA-MB-231 cell line (COSMIC Database: http://www.sanger.ac.uk/perl/genetics/CGP/cosmic?action=sample&id=905960&display=mutation) and their distinct transcriptional profiles (Neve et al, 2006). Cell lines were cultured in RPMI-1640 medium containing 10% FBS, 1% glutamine and 1% antibiotics and antimycotics (all from Invitrogen, Gent, Belgium) at 37 °C in a 5% CO2 atmosphere.
Blood spiking experiments
A total of 7.5 ml blood samples spiked with 103 cells of the above-mentioned cell lines were used for the isolation of tumour cells for mutation and transcriptional analysis. Blood samples were collected from two healthy volunteers. Tumour cells were harvested from near-confluent culture flasks according to the ATCC guidelines (ATCC, Manassas, VA, USA). The number of harvested cells was determined using a Fuchs-Rosenthal counting chamber (Marienfeld-Superior, Lauda-Königshofen, Germany). Cells were washed once, resuspended and serially diluted in RPMI-1640 to a final concentration of 103 cells per 100 μl culture medium. From this final cell suspension, 100 μl was subsequently added to a 7.5-ml normal blood sample and processed immediately on the CellSearch system as described below. From each culture flask used for harvesting tumour cells for spiking experiments, an additional 3–5 million cells were harvested for the isolation of DNA and RNA – performed with the AllPrep DNA/RNA Micro Kit (Qiagen, Valencia, CA, USA) – that served as a positive internal control in the downstream analyses.
Immunomagnetic enrichment and sample staining procedures
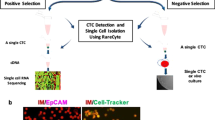
The overall experimental workflow is illustrated in Figure 1. To allow both mutation and transcriptional analysis of isolated tumour cells, two different sample preparation procedures were used.
Schematic of overall experimental workflow. Step 1: Tumour cells of three different human cultured breast cancer cell lines were spiked in healthy donor blood at a concentration of 103 tumour cells per 7.5 ml whole blood. Step 2: Tumour cells were immunomagnetically enriched using either the CellSearch CTC kit or the CellSearch Profile kit followed by a manual staining procedure. Step 3: Cells were reconstituted in a final volume of 14 μl and loaded in a DEPArray cartridge. Step 4: Analysis and sorting procedures were performed on the DEPArray system. Step 5: Single cells and groups of cells of interest were isolated with the DEPArray system. Step 6: Mutation or transcriptional analysis of isolated tumour cells.
In the first procedure, standard protocols and reagents for CTC isolation and enumeration with the FDA-approved CellSearch CTC kit (Veridex LLC) were used. Briefly, tumour cells were spiked in 7.5 ml healthy donor blood collected in a CellSave Preservative Tube (Veridex LLC). Tumour cell isolation and enumeration were performed using the CellSearch CTC Kit. With this assay, EpCAM-based immunomagnetically enriched cells are fluorescently counter labelled with DAPI, which stains the cell nucleus, PE-conjugated antibodies directed against cytokeratins (CKs) 8/18/19 and APC-conjugated antibodies directed against CD45, which stains remaining WBCs. After processing the samples on the CellSearch system, Veridex cartridges were stored protected from light at 4 °C until further use. Sample aspiration from the CellSearch cartridge and volume adjustment for transfer into the DEPArray cartridge were performed as described below under the section ‘Sample transfer from CellSearch to DEPArray cartridges’.
As CellSave Preservative tubes and the CellSearch CTC kit contain preservative and fixation reagents that might inversely affect RNA quality, a separate procedure was developed to enable the isolation of tumour cells that could be used for both mutation and transcriptional analysis. For this procedure, tumour cells were spiked in 7.5 ml EDTA anti-coagulated healthy donor blood and isolated using the CellSearch Profile Kit (Veridex LLC). Samples were subsequently stained using a manual staining protocol. Briefly, samples were centrifuged for 15 min at 300 g and the pellet was resuspended in 80 μl autoMACS Running Buffer (Miltenyi Biotec, GmbH, Bergisch Gladbach, Germany). Samples were incubated with 20 μl PE-conjugated anti-EpCAM antibody (clone 0.N.276, Santa Cruz Biotechnology, Santa Cruz, CA, USA) for 10 min at 4 °C and 10 μl APC-conjugated anti-CD45 antibody (clone 5B1, Miltenyi Biotec) for another 10 min at 4 °C. After blocking the reaction by adding 1 ml of autoMACS Running Buffer, 1 μl Hoechst 33342 (Sigma, St Louis, MO, USA) (10 mg ml−1 concentration) was added and samples were incubated for 5 min at room temperature. After 10 min of centrifugation at 300 g, cells were washed in RPMI-1640 culture medium and finally resuspended in 14 μl of RPMI-1640.
Sample transfer from CellSearch to DEPArray cartridges
To allow loading of samples from CellSearch cartridges – containing 325–350 μl of sample – in a DEPArray cartridge – typically loaded with 14 μl of sample – CellSearch CTC samples were aspirated from their CellSearch cartridge using a 200 μl gel loading tip pre-rinsed in a 2% BSA in PBS solution. To ensure maximal cell transfer, CellSearch cartridges were rinsed twice with a 325 μl aliquot of SB115 buffer (SB), a proprietary low-conductivity buffer for sorting fixed cells in the DEPArray cartridge. The whole suspension was centrifuged for 10 min at 300 g, cells were washed once in 1 ml of SB115 buffer and finally resuspended in 14 μl of SB115 buffer.
DEPArray procedure
Cell sorting experiments were performed as described in the manufacturer’s instructions. Briefly, DEPArray cartridges were manually loaded with 14 μl of sample and 800 μl of the buffer solution in which purified or single tumour cells had to be recovered. After loading the cartridge into the DEPArray system, ∼9.26 μl of sample was automatically injected by the system into a microchamber of the cartridge where the cells were spontaneously organised into a preprogrammed electric field consisting of 16 000 electrical cages in which individual cells are trapped. Image frames covering the entire surface area of the microchamber for each of three fluorescent filter cubes (PE, APC and DAPI/Hoechst) and bright field images were captured. Cells were automatically detected by the system based on a DAPI/Hoechst fluorescence threshold and were assigned a unique cell ID. Captured images were digitally processed and presented in a software module that enables selection of cells of interest by the operator. Next, for recovery selected cells were moved simultaneously to a parking area adjacent to the main microchamber in the cartridge. Individual cells or groups of cells were subsequently moved to a recovery area where a last visual confirmation of cell presence can be performed. To recover a cell or group of cells, the content of the recovery area was flushed with two drops of buffer (ca. 30–40 μl) into a 200 μl PCR tube. The entire cell routing process was monitored under bright field imaging. Routing paths were automatically calculated by the software. Routing parameters such as speed can be manually adjusted according to the observed cellular moving properties.
Evaluation of cell loss during loading of DEPArray cartridges
To evaluate the extent of cell loss that occurs during loading of a DEPArray cartridge and sample injection into the main microchamber, counting experiments were performed using CellSearch CTC control samples (CellSearch CTC control kit, Veridex LLC), processed with the CellSearch CTC kit as an internal quality control for routine CellSearch CTC analysis in our lab. Each of these samples contain two populations of fixed SK-BR-3 breast cancer cells at different concentrations that can be distinguished from each other by use of fluorescent dyes specific for each population (i.e., one population of APC-positive cells present at a concentration of ±60 cells per sample and another population of FITC-positive cells present at a concentration of ±1000 cells per sample). After enrichment and enumeration of both cell populations on the CellSearch system, CellSearch cartridges were removed from their Magnest (Veridex LLC) and stored protected from light at 4 °C until enumeration of the same sample was performed on the DEPArray. Sample transfer from the CellSearch cartridge to the DEPArray cartridge was performed as described above. The percentage of cells enumerated on the CellSearch system that could be re-identified on the DEPArray system was used as a measure to estimate the total extent of cell loss.
Mutation analysis of DEPArray-purified MDA-MB-231 cells pre-enriched with the CellSearch CTC kit
A total of 1000 MDA-MB-231 cells harbouring known mutations in the BRAF, KRAS, TP53 and NF2 genes were spiked in 7.5 ml blood. The sample was processed with the CellSearch CTC kit and the CellSearch cartridge was stored at 4 °C for 8 days. Tumour cells visualised on the DEPArray were defined using standard CellSearch CTC criteria as described elsewhere (Riethdorf et al, 2007). Isolations of 3 single tumour cells and 1 group of 10 tumour cells were performed with the DEPArray in SB115 buffer. Recovered samples were 1 : 3 diluted with molecular grade water and centrifuged for 30 min at maximum speed in a microcentrifuge. Subsequently, 100 μl of supernatant was aspirated, leaving ∼20 μl of diluted buffer, and samples were stored at −80 °C until further use. To allow genotyping analysis on the nuclear material of as few as a single cell, whole genome amplification (WGA) was performed using the Ampli1 WGA kit (SB). Samples were thawed on ice and vacuum centrifuged in a SpeedVac concentrator (Thermo Savant, Thermo Scientific, Waltham, MA, USA) for ∼20 min to concentrate the sample volume to ∼1 μl, the starting volume of the WGA procedure. Global amplification consisting of DNA isolation, MseI restriction digest, adaptor ligation and PCR amplification were performed as described in the manufacturer’s instructions. Whole genome amplification products were subjected to an end-point PCR for two control genomic DNA sequences of 373 and 167 bp, respectively (Ampli1 Quality Control kit; SB) and PCR products were analysed by gel electrophoresis on an Agilent 2100 Bioanalyzer using the DNA 1000 kit (Agilent Technologies, Santa Clara, CA, USA). Only samples positive for both PCR products were considered to contain successfully amplified genomic material suitable for mutation analysis. DNA concentrations of the final WGA products were measured using a Nanodrop ND1000 (NanoDrop Technologies, Waltham, MA, USA) and 50 ng of the amplified DNA product was subjected to mutation analysis for a panel of 10 mutations (Table 2) using a Sequenom MALDI-TOF MassARRAY multiplex PCR and genotyping assay (iPlex assay; Sequenom Inc., San Diego, CA, USA) as described previously (Reumers et al, 2011).
Mutation analysis of DEPArray-purified MDA-MB-231 cells pre-enriched with the CellSearch Profile kit
A total of 1000 MDA-MB-231 tumour cells were spiked in 7.5 ml EDTA anti-coagulated blood and processed according to the CellSearch Profile procedure in two different experiments. Samples were sorted on the DEPArray in RPMI-1640 medium. In each experiment, 11 recoveries were performed consisting of 1 blank buffer sample acting as the negative template control (NTC), 5 single tumour cells, 1 group of 5 tumour cells, 1 group of 10 tumour cells and 2 groups of 20 WBCs. An additional buffer sample was isolated between the last tumour cell recovery and the first recovery of WBCs to check for contamination between recoveries. Samples were briefly spun down in a microcentrifuge, diluted with 100 μl of PBS and centrifuged at maximum speed for 30 min after which supernatant was carefully aspirated to leave ∼1 μl. Samples were stored at −80 °C until further use. Quality control and WGA were performed using the Ampli1 WGA kit as described above. Half of the amplified DNA was subjected to KRAS mutation analysis using a TheraScreen KRAS PCR kit (Qiagen).
Transcriptional analysis of DEPArray-purified tumour cells pre-enriched with the CellSearch Profile kit
A total of 1000 MDA-MB-231 cells, MDA-MB-361 cells and MCF7 cells were spiked in 7.5 ml EDTA anti-coagulated blood and processed according to the CellSearch Profile procedure in three different experiments. Samples were sorted on the DEPArray in RPMI-1640 and isolations of 1 or 2 single tumour cells, groups of 3 to 10 tumour cells and a group of 10 WBCs were performed. Transcriptional analysis was performed as described previously (Sieuwerts et al, 2009b). Briefly, cells were lysed immediately after isolation with the DEPArray in 250 μl RLT buffer Plus (Qiagen) and stored at −80 °C. RNA isolation was performed with the RNeasy Micro Kit (Qiagen). The cDNA synthesis and 15 cycles of pre-amplification were performed with the RevertAid H Minus First Strand cDNA Synthesis Kit (Fermentas, Thermo Fisher Scientific, Waltham, MA, USA) and the TaqMan PreAmp amplification method (Applied Biosystems (ABI, Foster City, CA, USA)), respectively. Pre-amplified cDNA products were subjected to real-time PCR amplification for nine marker genes and five reference genes (ACTB, TBP, GUSB, HMBS and HPRT1) to control for sample loading and RNA integrity. Marker genes were chosen based on their potential to cover clinically relevant heterogeneity in CTC populations and included the epithelial-specific marker EPCAM; adhesion and invasion markers CDH1 and CDH2; markers specific for breast cancer subgroups CAV1, ESR1, GATA3, ERBB2 and GRB7; and the WBC marker PTPRC, the gene encoding for CD45. Assay IDs of TaqMan Gene Expression Assays (ABI) can be found in Supplementary Table 1. Fluorigenic PCR reactions were performed in 40 cycles in a final volume of 20 μl using TaqMan Gene Expression Assays and Taqman Universal PCR Master Mix No AmpErase UNG according to the manufacturer’s instructions on a 7900HT Fast Real-time PCR System (all from ABI). Each sample was analysed in duplicate and mean Ct values were used for further analysis. Negative controls included an RPMI-1640 buffer sample and minus RT samples from pools of RNA of each cell line. Only samples with a Ct value of <35 for each of the individual five reference genes, and a median Ct value for all reference genes of <30, were considered of sufficient quality and quantity to be included for further analyses. Gene expression values were quantified relative to a standard curve constructed for each marker transcript with a four-fold serial dilution of cDNA reverse transcribed from QPCR Human Reference Total RNA (Agilent Technologies) at an input ranging from 20 ng RNA to 20 pg total RNA. Calculated relative gene expression values with a corresponding Ct value of ⩾35 were set to zero and data were autoscaled as such that, for each marker, the median relative gene expression level and the s.d. across all samples equalled 0 and 1, respectively. Normalised gene expression levels were compared across samples using the Mann–Whitney U-test. Correlations of gene expression data between samples were calculated using Pearson’s correlation statistics. Unsupervised hierarchical clustering was performed based on the Pearson’s correlation distance between samples with complete linkage as the dendrogram drawing method.
RESULTS
Evaluation of cell loss during loading of DEPArray cartridges
The DEPArray cartridges are typically loaded with 14 μl of a fluorescently labelled single-cell suspension. To prevent the injection of air in the main microchamber of the cartridge where the visualisation and sorting of the cells occur, only ∼9.26 μl of the total 14 μl is injected into this microchamber by the system. As this implies an analytically dead volume of 4.74 μl in the microfluidic channels of the cartridge, a cell loss of ∼34% is expected. Additional cell loss might also occur because of manual sample volume adjustments and pipetting errors. In order to estimate the realistic extent of cell loss during this entire sample loading step, we first performed counting experiments using CellSearch CTC control samples processed with the CellSearch CTC kit. After being processed on the CellSearch System, CellSearch cartridges were stored at 4 °C for a mean duration of 5 days (maximum 15 days) before analysis on the DEPArray system. Results of 10 different experiments are summarised in Table 1. Representative images of cells visualised by the DEPArray system are shown in Supplementary Figure 1. On average, a cell re-identification rate – defined as the percentage of cells counted on the CellSearch system that were available for cell sorting after loading into the DEPArray cartridge – of 62–63% was obtained. An acceptable degree of variation (CV 19–20%) was observed between samples, with a minimum recovery of 37% (63% cell loss) in one experiment. Similar recovery rates were obtained for the sparse APC-positive cells as well as for the more abundant FITC-positive cell population.
Mutation analysis of DEPArray-purified MDA-MB-231 cells pre-enriched with the CellSearch CTC kit
To explore the feasibility to perform mutation analysis on single CTCs isolated with the DEPArray from CellSearch cartridges processed for standard CellSearch CTC enumeration, MDA-MB-231 cells were purified from a spiked blood sample pre-enriched with the CellSearch CTC kit. Three single tumour cells and one group of 10 tumour cells were isolated with the DEPArray and analysed for the presence of 10 different mutations in 6 genes with a customised iPlex assay. Mutation profiles were compared with that of genomic DNA extracted from 3 to 5 million cells harvested from the same culture flask. Illustrative cell images are shown in Figure 2. Results of the mutation analysis are summarised in Table 2. Call rates of the amplified genomic sequences were 80% for the single-cell samples and 100% for the 10-cell sample. Of the 10 mutations covered by the iPlex assay, 4 (BRAF_G1391T, KRAS_G38A, TP53_G839A and NF2_G691T) have been documented in the MDA-MB-231 cell line (COSMIC Database). All expected mutations were reliably detected in 2 out of 3 single-cell samples and the 10-cell sample. In one single-cell sample, two mutations remained undetected. In this sample, for BRAF, only wild-type sequence was detected, whereas no reliable call could be obtained for NF2.
Composite image gallery showing staining characteristics of MDA-MB-231 cells and WBCs from a CellSearch cartridge after immunomagnetic enrichment with the CellSearch CTC kit visualised on the DEPArray system. (A) Tumour cells were defined using standard CellSearch CTC criteria being (1) round to oval shape, (2) presence of a clear DAPI-stained nucleus, (3) at least 50% overlap between the CK-PE-positive cytoplasm and the nucleus and (4) CD45-APC negativity. Separate images for PE, DAPI and APC fluorescence and bright field channels and merged CK-PE/DAPI and CD45-APC/DAPI images of three single MDA-MB-231 cells (top 3 rows) and two WBC (bottom 2 rows) are shown. (B) Scatter plot of mean fluorescence intensities for CK-PE (y axis) and CD45-APC (x axis) staining by the DEPArray software. Rectangular gates can be applied to aid quick identification of cells or populations of cells for cell sorting. Green dots represent CK+/CD45− MDA-MB-231 cells selected by the user. Red dots represent CK−/CD45+ WBCs. Grey dots represent unselected events.
Mutation analysis of DEPArray-purified MDA-MB-231 cells pre-enriched with the CellSearch Profile kit
To enable the transcriptional analysis of tumour cells isolated with the DEPArray, a separate workflow that allows the isolation of unfixed tumour cells using the CellSearch Profile kit and a manual staining procedure was developed. To evaluate the performance of this protocol, we first subjected MDA-MB-231 tumour cells isolated with this procedure to a mutation analysis with the TheraScreen KRAS PCR kit (Qiagen), which allows detection of the G38A KRAS mutation, heterozygously present in this cell line (COSMIC Database). Results of two different experiments are summarised in Table 3. In line with their known low constitutive EPCAM expression (Sieuwerts et al, 2009a), an extremely poor EpCAM staining was observed for the MDA-MB-231 cells during visualisation on the DEPArray. As a consequence, tumour cells were selected mainly based on morphological criteria such as size and high nuclear–cytoplasmic rate and the absence of CD45-APC staining. A total of 5 single tumour cells, 2 groups of 5 to 10 tumour cells and 2 groups of 20 WBCs were isolated and subjected to WGA in each experiment. In both experiments, genomic DNA was successfully amplified according to Ampli1 end-point PCR criteria, in 3 out of 5 (60%) single tumour cells and all groups of 5–10 tumour cells and WBCs (Figure 3). No amplification product of either of the two control PCR fragments could be detected in two single-cell samples in each experiment, suggesting cell loss due to aspiration of the cell during the preparation for the WGA procedure. No control PCR product was detected in any of the blank buffer samples that served as NTC and carryover control between tumour cell and WBC recoveries. The G38A KRAS mutation was detected in all successfully amplified tumour cell samples and in none of the four successfully amplified WBC samples, indicating 100% purity of the sorted samples.
Composite gel images of Ampli1 QC end-point PCR products of Ampli1 whole-genome amplified DNA of five single MDA-MB-231 tumour cells and two groups of tumour cells and WBCs used for KRAS mutation analysis, analysed on the Agilent 2100 Bioanalyzer. Genomic DNA of samples was considered to be successfully amplified if both of two control genomic DNA sequences were visualised. In this example, no amplification product was obtained in two single-cell samples and both negative control samples. No mutated or wild-type allele sequences were detected with the Therascreen KRAS mutation test in both single-cell samples that failed to pass Ampli1 amplification check (Table 3, experiment 1). NTC=negative template control; TC=tumour cell; WBC=white blood cell.
Transcriptional analysis of DEPArray-purified tumour cells pre-enriched with the CellSearch Profile kit
Finally, we investigated the feasibility to perform transcriptional analysis of single cells enriched from spiked blood samples with the CellSearch Profile kit and further purified with the DEPArray system. For this purpose, we performed spiking experiments with three human breast cancer cell lines exhibiting strongly different expression levels for nine marker transcripts. Single tumour cells, groups of tumour cells and groups of WBCs were isolated and subjected to quantitative real-time RT–PCR analysis. For the samples of the MDA-MB-361 cell line, reliable qPCR amplification could not be obtained for three out of five reference genes, indicating poor RNA quality. These samples were excluded from further analysis. Examples of the staining characteristics of MDA-MB-231, MCF7 cells and WBCs and results of the gene expression analysis are shown in Figure 4. Similar to what was observed in the previous experiment, EpCAM-PE staining intensity was poor to absent in a majority of MCF7 tumour cells and in almost all MDA-MB-231 tumour cells. Therefore, tumour cells had to be distinguished from WBCs mainly based on morphological criteria including larger size and nuclear–cytoplasmic rate and strict CD45-APC negativity. On gene expression analysis, all tumour cell samples of both cell lines were negative for PTPRC whereas groups of WBCs were strongly positive (P=0.012). Significantly higher gene expression values were observed in luminal MCF7 cells as compared with triple-negative MDA-MB-231 cells for CDH1 (P=0.019), ESR1 (P=0.018), GATA3 (P=0.029) and EPCAM (P=0.020). Conversely, CAV1 (P=0.020) was expressed at significantly higher levels in MDA-MB-231 cells as compared with MCF7 cells. Gene expression profiles of single cells and groups of cells were highly correlated with gene expression profiles obtained from positive control samples (Pearson R2 (mean±s.d.) for MCF7 cells and MDA-MB-231 cells, respectively: 0.82±0.20 and 0.62±0.11). Hierarchical clustering of the gene expression profiles of these MDA-MB-231 and MCF7 samples together with a WBC sample from each of both experiments demonstrated a clear separation between the three different cell types, driven by the differential gene expression of ESR1, GATA3, CDH1, EPCAM, CAV1 and PTPRC.
(A) Composite image gallery of MDA-MB-231 cells, MCF7 cells and WBCs from manually stained CellSearch Profile samples visualised on the DEPArray system. Images of a single MCF7 cell showing faint EPCAM-PE staining (row 1), a single MDA-MB-231 cell showing no EPCAM staining (row 2) and two EPCAM-/CD45+ WBCs (rows 3 and 4) are shown. (B) Unsupervised hierarchical clustering analysis comparing gene expression profiles of 1 to 10 MDA-MB-231 cells, MCF7 cells and WBCs isolated from spiked blood samples with the CellSearch Profile kit and the DEPArray system and corresponding positive control samples (PC). Data have been subjected to median normalisation for each individual marker across all samples. Red colour indicates a transcript level above the median and green colour indicates a transcript level below the median of the particular assay as measured in all samples. (C) Boxplots of normalised gene expression values of 1 to 10 MDA-MB-231 and MCF7 cells and two groups of 10 WBCs for the 9 marker transcripts. PC=positive control sample cDNA of 3–5 million MDA-MB-231 cells harvested from the same culture flask as the one used to perform the isolation of single cells and groups of tumour cells); NTC=negative template control; TC=tumour cell(s); WBC=white blood cell.
DISCUSSION
We describe a new method for the isolation of single tumour cells and completely purified groups of multiple tumour cells from immunomagnetically pre-enriched blood samples using two different sample preparation workflows. With this approach, we provide proof of principle demonstrating the feasibility to molecularly characterise 1 to 10 tumour cells on both genomic and transcriptional levels. Taken together, expected mutations could be detected in 60% of the recovered (n=13) and all successfully whole genome amplified (n=9) single tumour cells and groups of tumour cells (n=5) isolated from both fixed and unfixed cell samples. Importantly, all carryover control samples and WBC samples were negative for epithelial markers, indicating high purity of the samples and specificity of the applied procedures. Additionally, reliable gene expression profiles for a limited set of 9 markers could be obtained for single tumour cells and groups of tumour cells from two out of three blood spiked breast cancer cell lines.
Standardised and reliable methods for the isolation and molecular characterisation of CTCs at the single-cell level are of considerable interest to CTC research for several reasons. First, CTCs encompass an extremely rare cell population. Therefore, technologies capable of handling small numbers of cells are needed in order to be able to maximise the amount of information that can be derived from them. Second, single-cell isolation allows the complete elimination of the WBC background resulting in pure CTC samples, a considerable advantage for molecular analysis. Third, single-cell resolution provides clinicians and researchers with the unique opportunity to directly investigate the molecular heterogeneity of CTCs on a cell per cell basis, the smallest functional unit of cancer.
Several techniques for the manipulation and isolation of single micrometastatic tumour cells such as CTCs and their disseminated counterparts in the bone marrow of patients with cancer have been described. The frequently used strategies include micromanipulation (Klein et al, 2002; Pierga et al, 2005; Hannemann et al, 2011; Powell et al, 2012) and laser capture microdissection (Kroneis et al, 2011; Sakaizawa et al, 2012) in combination with some antibody-based or physical pre-enrichment procedure. Many of these techniques have shown promising results with respect to the information that can be derived from single cells from both a biological and a clinical perspective. In addition, several microfluidic devices enabling single tumour cell manipulation, sorting and analysis have been described (Wlodkowic and Cooper, 2010). Direct comparisons between different single-cell isolation techniques are currently lacking. The choice of which technique is best to be used in a specific setting will depend to a large extent on the purpose of the analysis (research or clinical use), the throughput needed, compatibility with downstream applications and available upstream sample preparation procedures as well as personal experience. From our point of view, the most important advantages of the DEPArray system are the ability to obtain multiparametric immunofluorescent staining characteristics of individual cells before isolation, the ease of operating the system and the possibility to implement the system in a continuous semiautomated workflow with, for example, the CellSearch system. Interestingly, in this study CellSearch cartridges were stored for up to 15 days without inversely affecting processing on the DEPArray system, providing valuable flexibility in the planning of isolation experiments if such techniques are to be applied in a multicentre or clinical setting. Furthermore, all imaging data obtained before recovering the cells are digitally stored, allowing integration of staining characteristics of therapeutically relevant targets such as the level of HER2 protein expression with molecular information of the same cells.
However, the multiparametric imaging and isolation capabilities of single CTCs that can be achieved with the DEPArray system come at a cost. An important issue when studying rare cell populations such as CTCs is the degree of cell loss that occurs during the preparation and isolation of samples. Therefore, we have tried to estimate the extent of cell loss that has to be taken into account when processing CellSearch samples on the DEPArray. CellSearch CTC Control samples that had been enumerated on the CellSearch system were chosen as a model for this because they contain known numbers of two distinct cell populations in different concentrations. Our results indicate that on average 40% cell loss has to be taken into account in this setting. An acceptable degree of variability was observed between different samples with a minimum cell loss of ∼20% and a maximum cell loss of ∼60% observed across 10 experiments. As this is an artificial model, it is unclear how this reflects the true extent of cell loss that can be expected when analysing CellSearch CTC samples from patients on the DEPArray. It can however be anticipated that cell loss might be more sample dependent in this setting as CTCs are likely to exhibit more variation in morphology and immunofluorescent staining characteristics hampering their unambiguous identification. It therefore stands to reason that, although it is not clear to define any specific lower limit for the number of CTCs at this moment, the clinical applicability of this workflow will likely be restricted to a limited subgroup of patients with metastatic carcinomas in whom relatively high numbers of CTCs can be found in the blood with the currently available enrichment procedures.
Another point of notice is the long duration of DEPArray sorting experiments, which in our experience amounts up to ∼1 working day to obtain the current technical maximum of 18 isolations. This becomes particularly relevant when transcriptional analysis is to be performed on the isolated tumour cells, as it is unclear to what extent RNA integrity will be affected and how gene expression profiles might change under these conditions. Regardless of these potential caveats, our results indicate that reliable transcriptional analysis of tumour cells isolated with the DEPArray is at least feasible if stringent criteria for RNA quality are applied. Based on a limited set of nine well-chosen markers, gene expression profiles of MDA-MB-231 cells were clearly separated from those of MCF7 cells and WBCs. Observed gene expression profiles of cells from both breast cancer cell lines were in agreement with those expected from literature (Neve et al, 2006). Reassuringly, key molecular characteristics such as the overexpression of ER cluster genes ESR1 and GATA3 in luminal MCF7 cells and of CAV1 in basal-like MDA-MB-231 cells, as well as the previously reported differences in EPCAM expression between luminal and basal-like breast cancer cell lines (Sieuwerts et al, 2009a), were highly preserved down to the single-cell level. This further highlights the potential of this single cell approach for capturing heterogeneity in the CTC population when appropriate markers are selected.
More research and further optimisation are however needed before these workflows can be applied to patient samples containing unknown numbers and phenotypes of CTCs. First, an important question to address for future research will be to explore the molecular heterogeneity for specific biomarkers in clinical CTC samples and how this heterogeneity compares with primary and/or metastatic disease sites. Only such data will allow determining the minimum number of CTCs that has to be characterised to obtain clinically meaningful results from CTC-based biomarker analysis. An important technical hurdle that has to be overcome is the low performance of the applied EPCAM staining in CellSearch pre-enriched cell samples. Workflows will also have to be optimised to allow faster processing of samples and to minimise cell loss in single-cell samples during the buffer reduction procedure when preparing samples for downstream analysis. Furthermore, to prepare samples for mutation analysis, a restriction-based, ligation-mediated PCR amplification method was used. Although we do not have specific data for this kit, all currently known WGA methods are expected to deliver a method-specific genome coverage and allelic representations (Spits and Sermon, 2009; Vanneste et al, 2012), which might explain the failed detection or misidentification of two out of four expected mutations in one of the successfully amplified single-cell sample with the iPlex assay. Evaluating different WGA methods might prove important to circumvent this problem. Finally, in this study, the EPCAM-based CellSearch system was used as the starting point for the CTC purification and characterisation workflow. Using a model system of human breast cancer cell lines, it has however been shown that breast cancer cells of the normal-like subtype lack EPCAM expression and that tumour cells of this breast cancer subtype are consequently missed when using the standard CellSearch assay (Sieuwerts et al, 2009a). It is furthermore suggested that in order to be able to complete the different steps of tumour cell dissemination, epithelial cancer cells can undergo phenotypic changes that are associated with the loss of epithelial markers, a process often referred to as epithelial–mesenchymal transition (EMT) (Berx et al, 2007). Elevated gene expression of EMT-related transcription factors and higher percentages of cells expressing stem cell markers have recently been described in EPCAM- and CD45-depleted peripheral blood cell fractions of patients with HER2+ MBC, suggesting indeed the existence of an EPCAM-negative EMT-like subpopulation of CTCs (Giordano et al, 2012). It will therefore be of major interest for future research to combine different pre-enrichment strategies with DEPArray cell sorting in order to be able to specifically address questions regarding the relative representation, molecular profile and biological properties of both EPCAM-positive and EPCAM-negative CTC fractions isolated from blood samples of patients with metastatic carcinomas.
In conclusion, we report on our first experiences with the DEPArray system, a new dielectrophoretic cell sorter that allows the isolation of single or small groups of cells from mixed-cell suspensions. We describe analytical characteristics of the system and provide proof of principle showing the feasibility to isolate and molecularly characterise single tumour cells and groups of up to 10 tumour cells from CellSearch pre-enriched blood samples. Whereas the merits of the system for complete elimination of the WBC background from pre-enriched CTC samples and the opportunities for translational research to study CTC heterogeneity are clearly demonstrated, more research and further optimisation are needed before these techniques can be applied in a clinical setting.
Change history
02 April 2013
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Amir E, Miller N, Geddie W, Freedman O, Kassam F, Simmons C, Oldfield M, Dranitsaris G, Tomlinson G, Laupacis A, Tannock IF, Clemons M (2012) Prospective study evaluating the impact of tissue confirmation of metastatic disease in patients with breast cancer. J Clin Oncol 30: 587–592
Attard G, Swennenhuis JF, Olmos D, Reid AHM, Vickers E, A'Hern R, Levink R, Coumans F, Moreira J, Riisnaes R, Oommen NB, Hawche G, Jameson C, Thompson E, Sipkema R, Carden CP, Parker C, Dearnaley D, Kaye SB, Cooper CS, Molina A, Cox ME, LWMM Terstappen, de Bono JS (2009) Characterization of ERG, AR and PTEN gene status in circulating tumor cells from patients with castration-resistant prostate cancer. Cancer Res 69: 2912–2918
Berx G, Raspé E, Christofori G, Thiery JP, Sleeman JP (2007) Pre-EMTing metastasis? Recapitulation of morphogenetic processes in cancer. Clin Exp Metastasis 24: 587–597
Cohen SJ, Punt CJ, Iannotti N, Saidman BH, Sabbath KD, Gabrail NY, Picus J, Morse M, Mitchell E, Miller MC, Doyle GV, Tissing H, Terstappen LW, Meropol NJ (2008) Relationship of circulating tumor cells to tumor response, progression-free survival, and overall survival in patients with metastatic colorectal cancer. J Clin Oncol 26: 3213–3221
Collisson EA, Cho RJ, Gray JW (2012) What are we learning from the cancer genome? Nat Rev Clin Oncol 9: 621–630
Cristofanilli M, Budd GT, Ellis MJ, Stopeck A, Matera J, Miller MC, Reuben JM, Doyle GV, Allard WJ, LWMM Terstappen, Hayes DF (2004) Circulating tumor cells, disease progression, and survival in metastatic breast cancer. N Engl J Med 351: 781–791
de Bono JS, Scher HI, Montgomery RB, Parker C, Miller MC, Tissing H, Doyle GV, Terstappen LWWM, Pienta KJ, Raghavan D (2008) Circulating tumor cells predict survival benefit from treatment in metastatic castration-resistant prostate cancer. Clin Cancer Res 14: 6302–6309
Diaz LA, Williams RT, Wu J, Kinde I, Hecht JR, Berlin J, Allen B, Bozic I, Reiter JG, Nowak MA, Kinzler KW, Oliner KS, Vogelstein B (2012) The molecular evolution of acquired resistance to targeted EGFR blockade in colorectal cancers. Nature 486: 537–540
Fuchs AB, Romani A, Freida D, Medoro G, Abonnenc M, Altomare L, Chartier I, Guergour D, Villiers C, Marche PN, Tartagni M, Guerrieri R, Chatelain F, Manaresi N (2006) Electronic sorting and recovery of single live cells from microlitre sized samples. Lab Chip 6: 121–126
Giordano A, Gao H, Anfossi S, Cohen E, Mego M, Lee BN, Tin S, De Laurentiis M, Parker CA, Alvarez RH, Valero V, Ueno NT, De Placido S, Mani SA, Esteva FJ, Cristofanilli M, Reuben JM (2012) Epithelial-mesenchymal transition and stem cell markers in patients with HER2-positive metastatic breast cancer. Mol Cancer Ther 11: 2526–2534
Hannemann J, Meyer-Staeckling S, Kemming D, Alpers I, Joosse SA, Pospisil H, Kurtz S, Görndt J, Püschel K, Riethdorf S, Pantel K, Brandt B (2011) Quantitative high-resolution genomic analysis of single cancer cells. PLoS One 6: e26362
Higgins MJ, Jelovac D, Barnathan E, Blair B, Slater S, Powers P, Zorzi J, Jeter SC, Oliver GR, Fetting J, Emens L, Riley C, Stearns V, Diehl F, Angenendt P, Huang P, Cope L, Argani P, Murphy KM, Bachman KE, Greshock J, Wolff AC, Park BH (2012) Detection of tumor PIK3CA status in metastatic breast cancer using peripheral blood. Clin Cancer Res 18: 3462–3469
Ignatiadis M, Rothé F, Chaboteaux C, Durbecq V, Rouas G, Criscitiello C, Metallo J, Kheddoumi N, Singhal SK, Michiels S, Veys I, Rossari J, Larsimont D, Carly B, Pestrin M, Bessi S, Buxant F, Liebens F, Piccart M, Sotiriou C (2011) HER2-positive circulating tumor cells in breast cancer. PLoS One 6: e15624
Klein CA, Blankenstein TJF, Schmidt-Kittler O, Petronio M, Polzer B, Stoecklein NH, Riethmüller G (2002) Genetic heterogeneity of single disseminated tumour cells in minimal residual cancer. Lancet 360: 683–689
Kroneis T, Geigl JB, El-Heliebi A, Auer M, Ulz P, Schwarzbraun T, Dohr G, Sedlmayr P (2011) Combined molecular genetic and cytogenetic analysis from single cells after isothermal whole-genome amplification. Clin Chem 57: 1032–1041
Kurata T, Tamura K, Kaneda H, Nogami T, Uejima H, Asai G, Nakagawa K, Fukuoka M (2004) Effect of re-treatment with gefitinib (‘Iressa,’ ZD1839) after acquisition of resistance. Ann Oncol 15: 173–174
La Thangue NB, Kerr DJ (2011) Predictive biomarkers: a paradigm shift towards personalized cancer medicine. Nat Rev Clin Oncol 8: 587–596
Maheswaran S, Sequist LV, Nagrath S, Ulkus L, Brannigan B, Collura CV, Inserra E, Diederichs S, Iafrate AJ, Bell DW, Digumarthy S, Muzikansky A, Irimia D, Settleman J, Tompkins RG, Lynch TJ, Toner M, Haber DA (2008) Detection of mutations in EGFR in circulating lung-cancer cells. N Engl J Med 359: 366–377
Marusyk A, Almendro V, Polyak K (2012) Intra-tumour heterogeneity: a looking glass for cancer? Nat Rev Cancer 12: 323–334
Mehlen P, Puisieux A (2006) Metastasis: a question of life or death. Nat Rev Cancer 6: 449–458
Misale S, Yaeger R, Hobor S, Scala E, Janakiraman M, Liska D, Valtorta E, Schiavo R, Buscarino M, Siravegna G, Bencardino K, Cercek A, Chen C-T, Veronese S, Zanon C, Sartore-Bianchi A, Gambacorta M, Gallicchio M, Vakiani E, Boscaro V, Medico E, Weiser M, Siena S, Di Nicolantonio F, Solit D, Bardelli A (2012) Emergence of KRAS mutations and acquired resistance to anti-EGFR therapy in colorectal cancer. Nature 486: 532–536
Neve RM, Chin K, Fridlyand J, Yeh J, Baehner FL, Fevr T, Clark L, Bayani N, Coppe J-P, Tong F, Speed T, Spellman PT, De Vries S, Lapuk A, Wang NJ, Kuo W-L, Stilwell JL, Pinkel D, Albertson DG, Waldman FM, McCormick F, Dickson RB, Johnson MD, Lippman M, Ethier S, Gazdar A, Gray JW (2006) A collection of breast cancer cell lines for the study of functionally distinct cancer subtypes. Cancer Cell 10: 515–527
Niikura N, Liu J, Hayashi N, Mittendorf EA, Gong Y, Palla SL, Tokuda Y, Gonzalez-Angulo AM, Hortobagyi GN, Ueno NT (2012) Loss of human epidermal growth factor receptor 2 (HER2) expression in metastatic sites of HER2-overexpressing primary breast tumors. J Clin Oncol 30: 593–599
Pierga J-Y, Bonneton C, Magdelénat H, Vincent-Salomon A, Nos C, Boudou E, Pouillart P, Thiery J-P, De Cremoux P (2005) Real-time quantitative PCR determination of urokinase-type plasminogen activator receptor (uPAR) expression of isolated micrometastatic cells from bone marrow of breast cancer patients. Int J Cancer 114: 291–298
Powell AA, Talasaz AH, Zhang H, Coram MA, Reddy A, Deng G, Telli ML, Advani RH, Carlson RW, Mollick JA, Sheth S, Kurian AW, Ford JM, Stockdale FE, Quake SR, Pease RF, Mindrinos MN, Bhanot G, Dairkee SH, Davis RW, Jeffrey SS (2012) Single cell profiling of circulating tumor cells: transcriptional heterogeneity and diversity from breast cancer cell lines. PLoS One 7: e33788
Reis-Filho JS, Pusztai L (2011) Gene expression profiling in breast cancer: classification, prognostication, and prediction. Lancet 378: 1812–1823
Reumers J, De Rijk P, Zhao H, Liekens A, Smeets D, Cleary J, Van Loo P, Van Den Bossche M, Catthoor K, Sabbe B, Despierre E, Vergote I, Hilbush B, Lambrechts D, Del-Favero J (2011) Optimized filtering reduces the error rate in detecting genomic variants by short-read sequencing. Nat Biotechnol 30: 61–68
Riely GJ, Kris MG, Zhao B, Akhurst T, Milton DT, Moore E, Tyson L, Pao W, Rizvi NA, Schwartz LH, Miller VA (2007) Prospective assessment of discontinuation and reinitiation of erlotinib or gefitinib in patients with acquired resistance to erlotinib or gefitinib followed by the addition of everolimus. Clin Cancer Res 13: 5150–5155
Riethdorf S, Fritsche H, Müller V, Rau T, Schindlbeck C, Rack B, Janni W, Coith C, Beck K, Jänicke F, Jackson S, Gornet T, Cristofanilli M, Pantel K (2007) Detection of circulating tumor cells in peripheral blood of patients with metastatic breast cancer: a validation study of the CellSearch system. Clin Cancer Res 13: 920–928
Sakaizawa K, Goto Y, Kiniwa Y, Uchiyama A, Harada K, Shimada S, Saida T, Ferrone S, Takata M, Uhara H, Okuyama R (2012) Mutation analysis of BRAF and KIT in circulating melanoma cells at the single cell level. Br J Cancer 106: 939–946
Shah SP, Roth A, Goya R, Oloumi A, Ha G, Zhao Y, Turashvili G, Ding J, Tse K, Haffari G, Bashashati A, Prentice LM, Khattra J, Burleigh A, Yap D, Bernard V, McPherson A, Shumansky K, Crisan A, Giuliany R, Heravi-Moussavi A, Rosner J, Lai D, Birol I, Varhol R, Tam A, Dhalla N, Zeng T, Ma K, Chan SK, Griffith M, Moradian A, Cheng S-WG, Morin GB, Watson P, Gelmon K, Chia S, Chin S-F, Curtis C, Rueda OM, Pharoah PD, Damaraju S, Mackey J, Hoon K, Harkins T, Tadigotla V, Sigaroudinia M, Gascard P, Tlsty T, Costello JF, Meyer IM, Eaves CJ, Wasserman WW, Jones S, Huntsman D, Hirst M, Caldas C, Marra MA, Aparicio S (2012) The clonal and mutational evolution spectrum of primary triple-negative breast cancers. Nature 486: 395–399
Sieuwerts AM, Kraan J, Bolt J, van der Spoel P, Elstrodt F, Schutte M, Martens JWM, Gratama J-W, Sleijfer S, Foekens JA (2009a) Anti-epithelial cell adhesion molecule antibodies and the detection of circulating normal-like breast tumor cells. J Natl Cancer Inst 101: 61–66
Sieuwerts AM, Kraan J, Bolt-De Vries J, van der Spoel P, Mostert B, Martens JWM, Gratama J-W, Sleijfer S, Foekens JA (2009b) Molecular characterization of circulating tumor cells in large quantities of contaminating leukocytes by a multiplex real-time PCR. Breast Cancer Res Treat 118: 455–468
Sieuwerts AM, Mostert B, Bolt-De Vries J, Peeters D, de Jongh FE, JML Stouthard, Dirix LY, van Dam PA, Van Galen A, de Weerd V, Kraan J, van der Spoel P, Ramírez-Moreno R, van Deurzen CHM, Smid M, Yu JX, Jiang J, Wang Y, Gratama JW, Sleijfer S, Foekens JA, JWM Martens (2011) mRNA and microRNA expression profiles in circulating tumor cells and primary tumors of metastatic breast cancer patients. Clin Cancer Res 17: 3600–3618
Spits C, Sermon K (2009) PGD for monogenic disorders: aspects of molecular biology. Prenat Diagn 29: 50–56
Vanneste E, Bittman L, Van der Aa N, Voet T, Vermeesch JR (2012) New array approaches to explore single cells genomes. Front Genet 3: 44
Wlodkowic D, Cooper JM (2010) Tumors on chips: oncology meets microfluidics. Curr Opin Chem Biol 14: 556–567
Yu M, Ting DT, Stott SL, Wittner BS, Ozsolak F, Paul S, Ciciliano JC, Smas ME, Winokur D, Gilman AJ, Ulman MJ, Xega K, Contino G, Alagesan B, Brannigan BW, Milos PM, Ryan DP, Sequist LV, Bardeesy N, Ramaswamy S, Toner M, Maheswaran S, Haber DA (2012) RNA sequencing of pancreatic circulating tumour cells implicates WNT signalling in metastasis. Nature 487: 510–513
Acknowledgements
Dieter Peeters is a research assistant of the Fund for Scientific Research Flanders (FWO Vlaanderen). We thank Roberto Salgado and Aurore Dubois (Department of Pathology, Institut Jules Bordet, Brussels, Belgium) for their assistance with the Therascreen analyses. We gratefully acknowledge Elena Peruzzi and Manuela Banzi (both from Silicon Biosystems, Bologna, Italy) for their help with protocols and DEPArray system operation.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License.
Supplementary Information accompanies this paper on British Journal of Cancer website
Supplementary information
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Peeters, D., De Laere, B., Van den Eynden, G. et al. Semiautomated isolation and molecular characterisation of single or highly purified tumour cells from CellSearch enriched blood samples using dielectrophoretic cell sorting. Br J Cancer 108, 1358–1367 (2013). https://doi.org/10.1038/bjc.2013.92
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2013.92
Keywords
This article is cited by
-
Interrogating breast cancer heterogeneity using single and pooled circulating tumor cell analysis
npj Breast Cancer (2022)
-
Functional analysis of circulating tumour cells: the KEY to understand the biology of the metastatic cascade
British Journal of Cancer (2022)
-
Circulating tumor cells and palbociclib treatment in patients with ER-positive, HER2-negative advanced breast cancer: results from a translational sub-study of the TREnd trial
Breast Cancer Research (2021)
-
Using single-cell sequencing technology to detect circulating tumor cells in solid tumors
Molecular Cancer (2021)
-
Towards developing forensically relevant single-cell pipelines by incorporating direct-to-PCR extraction: compatibility, signal quality, and allele detection
International Journal of Legal Medicine (2021)