Abstract
Background:
Patients with high-grade gliomas are treated with surgery followed by chemoradiation. The risk factors and implications of neurological side effects are not known.
Methods:
Acute and late ⩾ grade 3 neurological toxicities (NTs) were analysed among 2761 patients from 14 RTOG trials accrued from 1983 to 2003. The association between acute and late toxicity was analysed using a stepwise logistic regression model. The association between the occurrence of acute NT and survival was analysed as an independent variable.
Results:
There were 2610 analysable patients (86% glioblastoma, 10% anaplastic astrocytoma). All received a systemic agent during radiation (83% chemotherapy, 17% biological agents). Median radiation dose was 60 Gy. There were 182 acute and 83 late NT events. On univariate analysis, older age, poor performance status, aggressive surgery, pre-existing neurological dysfunction, poor mental status and twice-daily radiation were associated with increased acute NT. In a stepwise logistic regression model the occurrence of acute NT was significantly associated with late NT (OR=2.40; 95% CI=1.2–4.8; P=0.014). The occurrence of acute NT predicted poorer overall survival, independent of recursive partitioning analysis class (median 7.8 vs 11.8 months).
Interpretation:
Acute NT is significantly associated with both late NT and overall survival.
Similar content being viewed by others
Main
Second to meningioma, high-grade gliomas (WHO grade 3, 4) are the most frequent type of primary brain tumours in adults. Treatment consists of maximal safe resection followed by partial brain radiation. Following the introduction of concomitant and adjuvant temozolomide, long-term survival for grade 4 gliomas (glioblastoma, GBM) has improved, with almost 10% of subjects now living 5 years (Stupp et al, 2009). The long-term toxicity of treatment is, therefore, of increasing importance.
Patients with high-grade glioma undergoing chemoradiation experience various side effects, including dermatological, endocrine, systemic and neurological events. Dermatological side effects such as radiation dermatitis and alopecia occur early and are generally transient, although alopecia may take several months to reverse. These rarely interfere with functional independence, but may contribute significantly to a reduction in quality of life because of a diminution in self-worth. Endocrine side effects are usually delayed by several months to years, are gradual in onset and often subtle, in terms of clinical presentation, and hence are underdiagnosed; they are more frequent in children than adults (Cross and Glantz, 2003). Systemic side effects such as myelosuppression and diarrhoea are generally attributable to chemotherapy.
Neurological side effects occur both early and late. Acute effects (within 90 days of the commencement of therapy) are often transient and include fatigue, headache, nausea, motor/sensory disturbances, raised intracranial pressure, cranial nerve palsies, visual disturbances, seizures and subtle changes in short-term memory. Late side effects (more than 90 days after the commencement of therapy) include many of the same symptoms, with the addition of cognitive decline (Taphoorn and Klein, 2004), cerebellar dysfunction and the consequences of white matter atrophy such as normal pressure hydrocephalus; these are rarely reversible.
It is often impossible to determine whether such neurological symptoms are side effects of radiation therapy (RT), surgery, chemotherapy, medications (e.g., anti-epileptics), an effect of the tumour itself or a combination of the above. The pathophysiology of radiation-induced neurological damage is complex and imperfectly understood; it is thought to involve (1) an increase in permeability of the blood–brain barrier, (2) death of oligodendroglial precursor cells leading to demyelination, (3) subtle changes in neuronal activity and vascular damage leading to frank radiation necrosis and (4) loss of radio-sensitive stem cell compartments, which under the inflammatory stress, induced by radiation, preferentially undergo gliogenic maturation, as opposed to participating in neurogenesis (Mizumatsu et al, 2003; Soussain et al, 2009).
A recent review across a wide range of tumour types suggested that risk factors for radiation-induced neurological toxicity (NT) include both treatment variables (radiation dose, fraction size, conformality index, volume treated, overall treatment time, chemotherapy use) and patient variables (older age, diabetes mellitus) (Lawrence et al, 2010). We are not aware of any large studies that have specifically examined the NT of radiation treatment in subjects with high-grade gliomas, with a view to identifying risk factors and associations between acute and late toxicity, and eventual survival.
Purpose
By performing a retrospective analysis of RTOG high-grade glioma studies we sought to answer the following questions:
-
1)
What is the incidence of acute and late NT following RT for high-grade glioma?
-
2)
What are the risk factors for acute and late NT following RT for high-grade glioma?
-
3)
Is there an association between acute and late NT?
-
4)
What are the long-term implications of acute NT?
Materials and methods
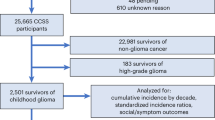
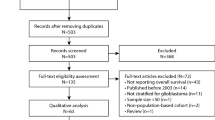
Patient data was pooled from 14 RTOG high-grade glioma trials that accrued a total of 2761 subjects (Table 1). Eligibility criteria were consistent in all of the studies: histologically confirmed supratentorial malignant glioma; age of at least 18 years; normal hepatic, renal and bone marrow function; and an interval of 6 weeks or less from surgery to initiation of radiotherapy. Ineligibility criteria included previous malignancies (except skin carcinomas), previous chemotherapy, or head and neck irradiation. All the trials combined RT with systemic anti-tumour therapy.
Definition of acute and late neurological toxicity
‘Acute toxicity’ is defined as adverse events that occurred within 3 months of commencing therapy; events occurring after this were classified as ‘late’. RTOG Acute Morbidity Scoring Criteria and RTOG/EORTC Late Radiation Morbidity Scoring Schema were used for the following studies: 8302, 8409, 9006, 9305, 9411, 9417, 9513, 9602 and 9710. NCI – CTC version 2.0 and RTOG/EORTC Late Radiation Morbidity Scoring Schema were used for the following studies: 9803, 9806, 0013, 0021 and 0023. For the purposes of this report, we only considered NTs of grade 3 or greater, without regard to attribution. Owing to the database's design we were unable to scrutinise details of the NTs.
The trials analysed used a range of doses and fractionation schemes. The effects of different fractionation schemes on the normal brain were compared by calculating the biological-equivalent dose (BED) (Fowler, 1989) using a normal tissue alpha/beta ratio of 3 (Lee et al, 1998). The RTOG trial 9305 combined fractionated therapy (60 Gy, BED 100) with a single-fraction radiosurgical boost. Although there is no accepted way to convert this into a BED, we considered the BED to be ‘above 120’ for the purposes of statistical analysis.
Statistical methods
Frequency distributions of patient survival time (survive ⩾3 month vs survive <3 months) for two groups (acute NT vs no acute NT) were compared using χ2-tests. McNemar's test was used to test the difference between two correlated proportions – occurrence/no occurrence of acute and late NTs. Logistic regression was used to assess the relationship between acute and late NTs. It was also used to assess the relationship between pre-treatment characteristics, treatment options and the occurrence of acute NTs. For the survival end point, the Kaplan–Meier method was used to estimate the rates, and the log-rank test was used to compare them between the two patient groups (acute NT vs no acute NT). The Cox proportional hazards (PH) model was used to estimate the hazard ratio (HR) associated with overall survival while adjusting patient-specific factors. A two-sided test was used at a significance level of 0.05 for all the evaluations.
Patients dying within 3 months of RT are by definition not able to develop late NT; they were therefore excluded from analyses of late toxicity.
Results
A total of 2761 patients were accrued; 151 patients (5%) were excluded from the analysis because of being ineligible, no protocol treatment or withdrawal of consent leaving 2610 patients. Baseline characteristics are listed in Table 2.
Median follow-up of all subjects was 11.2 months; median follow-up of the 279 patients censored subjects who were still alive at last follow-up was 57.3 months (this difference in length of follow-up between all subjects (censored and uncensored) and censored subjects reflects the fact that the risk of dying apparently decreases after living up to a certain time). The 265 patients who lived less than 3 months were excluded from analyses of late toxicity. A total of 182 cases (7.0%, crude rate) of acute NT and 83 cases (3.5%, crude rate) of late NT were reported.
Pretreatment characteristics and treatment options were assessed in logistic regression models to predict the occurrence of acute CNS toxicities. Table 3 lists the results, based on the univariate logistic regression analyses. Histology, chemotherapy and BED were considered as non-statistically significant at the significance level of 0.1 and not included in the further multivariate logistic regression analysis. In a stepwise logistic regression model considering the remaining six variables, Zubrod performance status, previous surgery type, neurological function, mental status and twice-daily (BID) radiation were significantly associated with acute NT (Table 3).
Pretreatment characteristics, treatment-related variables and the occurrence of acute NT were assessed in logistic regression models to predict the occurrence of late CNS toxicities. The following variables were considered in the univariate logistic regression analysis: age at diagnosis (<50 vs ⩾50), surgery type (biopsy vs partial/total resection), neurological dysfunction (no dysfunction/minor vs moderate/severe), mental status (normal function vs minor/confusion), once-daily radiation (yes vs no), Zubrod performance status (0 vs 1/2/3), histology (GBM vs anaplastic astrocytoma), chemotherapy (yes vs no), BED (⩽120 vs >120) and acute CNS toxicities (yes vs no). Age, Zubrod performance status, type of surgery, neurological function, mental status and histology were considered non-statistically significant at a significance level of 0.1 and not included in further multivariate logistic regression analysis. In a stepwise logistic regression model considering the four remaining variables, once-daily radiation, BED and previous occurrence of acute NT were all statistically associated with late NT (Table 4).
The association between acute and late toxicity amongst subjects who survived at least 3 months was examined by means of McNemar's test. Among the 148 patients experiencing acute NT, 10 (7%) patients experienced late NT; among the 2197 patients not experiencing acute NT, only 73 (3%) patients experienced late NT, P<0.0001, suggesting that acute CNS toxicities are statistically associated with late CNS toxicities.
When the two patient groups (patients with and without acute NT) were compared with regard to overall survival, based on the log-rank test, a statistical difference was found (HR=1.77; 95% CI=1.52–2.06; P<0.0001). The median survival times were 7.8 and 11.8 months, respectively. The Kaplan–Meier curve is presented in Figure 1. Subjects with acute CNS toxicities were more likely to die within 3 months of treatment. Approximately 19% of patients with acute CNS toxicities died within 3 months, whereas 10% of patients without acute CNS toxicities died within 3 months, P<0.001.
Recursive partitioning analysis (RPA) class (a combination of age, histology, Zubrod performance status, mental status, neurological function, symptom time and previous surgery) has been robustly established as a prognostic scale for patients with newly diagnosed high-grade glioma (Curran et al, 1993; Scott et al, 1998b; Mirimanoff et al, 2006). Recursive partitioning analysis class, BID radiation (yes vs no), chemotherapy (yes vs no), BED (⩽120 vs >120) and the occurrence of acute NT were assessed in a PH Cox model for overall survival (Table 5, Figure 2). Twice-daily radiation and BED were considered non-statistically significant and were not included in the multivariate Cox analysis. In a stepwise multivariate Cox model considering RPA class, chemotherapy and acute CNS toxicities, only RPA class and acute NT remained statistically associated with the overall survival (HR=1.43; 95% CI=1.2–1.7; P<0.0001) after adjusting for the RPA classes (Table 5).
Discussion
We performed an analysis of the RTOG database to understand the risk factors and consequences of acute NT in patients with high-grade gliomas undergoing RT.
We found that both early and late toxicity are comparatively rare (3–7%) – in agreement with published experience (Dinapoli et al, 1993; Stupp et al, 2005; Keime-Guibert et al, 2007). Risk factors for acute NT that remained significant in the multivariate analysis were both patient (functional status, neurological function, mental status) and treatment (biopsy only, BID radiation) related. These findings, though novel in the field of brain tumours, are in keeping with the general oncology literature that frail patients experience more toxicity (Brian et al, 1995; Artz et al, 2006; Kumar Pal et al, 2010). The lack of association between chemotherapy and toxicity differs with the findings of the pivotal EORTC/NCIC phase III trial that established temozolomide and radiation as the standard of care. In that trial, in-field acute grade 3 and 4 toxicities (dermatological, infection and vision and nausea/vomiting) occurred in 7 and 14% of subjects in the control and temozolomide arms, respectively, (Stupp et al, 2005). This difference may reflect the type and extended duration of chemotherapy in the EORTC/NCIC trial. Conversely the rate of late toxicity reported by us (3.5%) is much higher than that reported in each arm of the EORTC/NCIC trial (<1%), it is not clear whether this is due to differences in treatment, population (the EORTC trial excluded older patients) or reporting practices. An important difference is that the statistics from the Stupp trial refer to any non-haematological toxic event, whereas the data presented here are specifically for NT.
Risk factors for late toxicity, significant in multivariate analysis, were once-daily radiation, high total radiation dose and previous acute NT. It is interesting to compare our findings with the recently published QUANTEC meta-analysis of the tolerance of the normal brain to irradiation, which investigated risk factors for late brain toxicity (Lawrence et al, 2010). Many of the studies analysed by the QUANTEC team involved the treatment of non-primary brain tumours (e.g., brain metastases and nasopharyngeal carcinoma). The QUANTEC authors demonstrated a sharp incidence in radiation necrosis when the BED rose above 120. Although the end points are not identical, in the current study we likewise found that a BED above 120, doubled the risk of late toxicity.
The association between acute and late toxicity has not previously been reported, and challenges the classic teaching that acute toxicity is fully reversible. A possible explanation is that these acute toxicities were so severe that healing was not possible; alternatively this may reflect a predisposition to toxicity amongst certain patients, possibly related to either tumour location (e.g., close to critical structures) or genetic makeup.
The relationship between acute NT and overall survival was unexpected. Patients who did not experience acute NT were found to have a 4 month longer median survival than those who experienced NT (of at least grade 3). This survival advantage was independent of RPA class. Although we lack a complete explanation, this may demonstrate the importance of normal tissue damage in determining long-term survival. A recent study likewise demonstrated that GBM patients who acquired motor or language deficits post-operatively had poorer overall survival than those who remained neurologically intact (Shinoda et al, 2001).
Our findings are in contrast with the association between pseudo-progression and improved prognosis in high-grade gliomas (Gerstner et al, 2009). Pseudoprogression is generally defined as radiological progression (oedema and sometimes contrast enhancement on MRI) soon after the completion of RT in patients with malignant gliomas, which is followed by spontaneous recovery and stabilisation (Brandsma et al, 2008). Pathologically it is thought to represent a mild form of radiation necrosis. Possible explanations for the difference between our findings and those associating pseudoprogression with a good prognosis are (1) pseudoprogression is especially associated with the use of temozolomide (Chamberlain et al, 2007; Brandsma et al, 2008). None of the patients in our study received this agent; rather the most frequently used systemic agent was BCNU, which appears to be much less potent. (2) Our patients were universally symptomatic, whereas most patients with pseudoprogression are asymptomatic. Hence, whereas pseudoprogression may be a form of intra-tumour necrosis, we suspect that the ‘acute toxicity’ cases described here represent damage to surrounding normal tissues. A more thorough understanding would require a case-by-case review of imaging, which unfortunately is not possible.
Despite the fact that our study dates from the pre-temozolomide era, we found that the use of chemotherapy was associated with increased survival (Figure 2). Of those who received chemotherapy, 93% received BCNU. As this association was only found on univariate, but not in multivariate analysis, its significance is unclear. Nevertheless, the association is in agreement with previous meta-analyses that have likewise identified methylating agents to be effective radiosensitsers in this disease (Chang et al, 1983; Fine et al, 1993; Spiegel et al, 2007).
A weakness of this retrospective study is our inability to assess completeness of reporting, and accurate attribution of neurological events. The definition of NT varied between the studies depending on the toxicity scale used; further we do not have descriptions of these events. A possible explanation of our findings associating acute NT with long-term survival is ‘misclassification bias’, that is, the treating physicians had difficulty distinguishing treatment-related side effects from tumour symptoms, and that what was reported as ‘acute toxicity’ was in fact early tumour progression. A close reading of our results however, supports the fact that these were indeed true treatment-related side effects: (1) We found that compared with once-daily radiation, BID radiation produced increased acute toxicity, but decreased late toxicity. This is entirely in keeping with classic radiobiology teaching of normal tissue damage. The lack of impact of fractionation scheme on overall survival (Table 5) further supports the supposition that this is related to normal tissue injury and not tumour control. (2) Conversely, histology (GBM vs anaplastic astrocytoma) had no impact on either acute or late toxicity, despite the more aggressive nature of GBM. If ‘NT’ was in fact a measure of ‘tumour progression’, a correlation would have been expected. (3) This ‘misclassification’ bias would be expected to especially affect subjects whose tumours progressed very early. Nevertheless, if patients who died within the first 3 months are excluded from the analysis, the survival benefit associated with lack of acute toxicity remains (HR=1.69; 95% CI=1.43–2.01; P<0.0001, Supplementary Figure).
A further weakness of our study is the small number of patients encountering toxicity. Although we analysed 2610 subjects, there were only 182 acute toxic events and 83 late toxic events. Confirmatory studies from other large databases, or population-based cohorts are therefore needed to validate our findings.
In conclusion we have elucidated the risk factors for NT amongst patients with high-grade glioma undergoing RT. These should be considered when designing eligibility criteria for clinical trials. The finding that acute NT predicts for both late NT and poor overall survival in patients not receiving temozolomide is provocative and requires validation. This phenomenon appears to be distinct to the ‘pseudoprogression’ seen when temozolomide is combined with RT.
Change history
29 March 2012
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Artz AS, Pollyea DA, Kocherginsky M, Stock W, Rich E, Odenike O, Zimmerman T, Smith S, Godley L, Thirman M, Daugherty C, Extermann M, Larson R, van Besien K (2006) Performance status and comorbidity predict transplant-related mortality after allogeneic hematopoietic cell transplantation. Biol Blood Marrow Transplant 12: 954–964
Brandsma D, Stalpers L, Taal W, Sminia P, van den Bent MJ (2008) Clinical features, mechanisms, and management of pseudoprogression in malignant gliomas. Lancet Oncol 9: 453–461
Brian NS, Nicholas JP, Harold OD, Deborah LD, Giuseppina A, Neal JM (1995) Age and sex are independent predictors of 5-fluorouracil toxicity. Analysis of a large scale phase III trial. Cancer 75: 11–17
Cardinale R, Won M, Choucair A, Gillin M, Chakravarti A, Schultz C, Souhami L, Chen A, Pham H, Mehta M (2006) A phase II trial of accelerated radiotherapy using weekly stereotactic conformal boost for supratentorial glioblastoma multiforme: RTOG 0023. Int J Radiat Oncol Biol Phys 65: 1422–1428
Chamberlain MC, Glantz MJ, Chalmers L, Van Horn A, Sloan AE (2007) Early necrosis following concurrent Temodar and radiotherapy in patients with glioblastoma. J Neurooncol 82: 81–83
Chang CH, Horton J, Schoenfeld D, Salazer O, Perez-Tamayo R, Kramer S, Weinstein A, Nelson JS, Tsukada Y (1983) Comparison of postoperative radiotherapy and combined postoperative radiotherapy and chemotherapy in the multidisciplinary management of malignant gliomas. A joint Radiation Therapy Oncology Group and Eastern Cooperative Oncology Group study. Cancer 52: 997–1007
Colman H, Berkey BA, Maor MH, Groves MD, Schultz CJ, Vermeulen S, Nelson DF, Mehta MP, Yung WK (2006) Phase II Radiation Therapy Oncology Group trial of conventional radiation therapy followed by treatment with recombinant interferon-beta for supratentorial glioblastoma: results of RTOG 9710. Int J Radiat Oncol Biol Phys 66: 818–824
Coughlin C, Scott C, Langer C, Coia L, Curran W, Rubin P (2000) Phase II, two-arm RTOG trial (94-11) of bischloroethyl-nitrosourea plus accelerated hyperfractionated radiotherapy (64.0 or 70.4 Gy) based on tumor volume (>20 or ≤20 cm(2), respectively) in the treatment of newly-diagnosed radiosurgery-ineligible glioblastoma multiforme patients. Int J Radiat Oncol Biol Phys 48: 1351–1358
Cross NE, Glantz MJ (2003) Neurologic complications of radiation therapy. Neurol Clin 21: 249–277
Curran Jr WJ, Scott CB, Horton J, Nelson JS, Weinstein AS, Fischbach AJ, Chang CH, Rotman M, Asbell SO, Krisch RE, Nelson DF (1993) Recursive partitioning analysis of prognostic factors in three Radiation Therapy Oncology Group malignant glioma trials. J Natl Cancer Inst 85: 704–710
Curran Jr WJ, Scott CB, Nelson JS, Weinstein AS, Phillips TL, Murray K, Fischbach AJ, Yakar D, Schwade JG, Powlis WD, Nelson DF (1992) A randomized trial of accelerated hyperfractionated radiation therapy and bis-chloroethyl nitrosourea for malignant glioma. A preliminary report of Radiation Therapy Oncology Group 83-02. Cancer 70: 2909–2917
Del Rowe J, Scott C, Werner-Wasik M, Bahary JP, Curran WJ, Urtasun RC, Fisher B (2000) Single-arm, open-label phase II study of intravenously administered tirapazamine and radiation therapy for glioblastoma multiforme. J Clin Oncol 18: 1254–1259
Dinapoli RP, Brown LD, Arusell RM, Earle JD, O′Fallon JR, Buckner JC, Scheithauer BW, Krook JE, Tschetter LK, Maier JA (1993) Phase III comparative evaluation of PCNU and carmustine combined with radiation therapy for high-grade glioma. J Clin Oncol 11: 1316–1321
Fine HA, Dear KB, Loeffler JS, Black PM, Canellos GP (1993) Meta-analysis of radiation therapy with and without adjuvant chemotherapy for malignant gliomas in adults. Cancer 71: 2585–2597
Fisher B, Won M, Macdonald D, Johnson DW, Roa W (2002) Phase II study of topotecan plus cranial radiation for glioblastoma multiforme: results of Radiation Therapy Oncology Group 9513. Int J Radiat Oncol Biol Phys 53: 980–986
Fowler JF (1989) The linear-quadratic formula and progress in fractionated radiotherapy. Br J Radiol 62: 679–694
Gerstner E, McNamara M, Norden A, LaFrankie D, Wen P (2009) Effect of adding temozolomide to radiation therapy on the incidence of pseudo-progression. J Neurooncol 94: 97–101
Keime-Guibert F, Chinot O, Taillandier L, Cartalat-Carel S, Frenay M, Kantor G, Guillamo J-S, Jadaud E, Colin P, Bondiau P-Y, Menei P, Loiseau H, Bernier V, Honnorat J, Barrie M, Mokhtari K, Mazeron J-J, Bissery A, Delattre J-Y, The Association of French-Speaking N-O (2007) Radiotherapy for glioblastoma in the elderly. N Engl J Med 356: 1527–1535
Kumar Pal S, Katheria V, Hurria A (2010) Evaluating the older patient with cancer: understanding frailty and the geriatric assessment. CA Cancer J Clin 60: 120–132
Langer CJ, Ruffer J, Rhodes H, Paulus R, Murray K, Movsas B, Curran W (2001) Phase II radiation therapy oncology group trial of weekly paclitaxel and conventional external beam radiation therapy for supratentorial glioblastoma multiforme. Int J Radiat Oncol Biol Phys 51: 113–119
Lawrence YR, Li XA, el Naqa I, Hahn CA, Marks LB, Merchant TE, Dicker AP (2010) Radiation dose-volume effects in the brain. Int J Radiat Oncol Biol Phys 76: S20–S27
Lee AW, Foo W, Chappell R, Fowler JF, Sze WM, Poon YF, Law SC, Ng SH, O SK, Tung SY, Lau WH, Ho JH (1998) Effect of time, dose, and fractionation on temporal lobe necrosis following radiotherapy for nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys 40: 35–42
Mirimanoff RO, Gorlia T, Mason W, Van den Bent MJ, Kortmann RD, Fisher B, Reni M, Brandes AA, Curschmann J, Villa S, Cairncross G, Allgeier A, Lacombe D, Stupp R (2006) Radiotherapy and temozolomide for newly diagnosed glioblastoma: recursive partitioning analysis of the EORTC 26981/22981-NCIC CE3 phase III randomized trial. J Clin Oncol 24: 2563–2569
Mizumatsu S, Monje ML, Morhardt DR, Rola R, Palmer TD, Fike JR (2003) Extreme sensitivity of adult neurogenesis to low doses of X-irradiation. Cancer Res 63: 4021–4027
Robins HI, Won M, Seiferheld WF, Schultz CJ, Choucair AK, Brachman DG, Demas WF, Mehta MP (2006) Phase 2 trial of radiation plus high-dose tamoxifen for glioblastoma multiforme: RTOG protocol BR-0021. Neuro Oncol 8: 47–52
Scott C, Curran JW, Yung W, Scarantino C, Urtasun R, Movsas B, Jones C, Simpson J, Fischbach A, Petito C, Nelson J (1998a) Long term results of RTOG 9006: a randomized trial of hyperfractionated radiotherapy (RT) to 72.0 Gy & carmustine vs standard RT & carmustine for malignant glioma patients with emphasis on anaplastic astrocytoma (AA) patients. (Abstract 1546) Proc Am Soc Clin Oncol
Scott CB, Scarantino C, Urtasun R, Movsas B, Jones CU, Simpson JR, Fischbach AJ, Curran Jr WJ (1998b) Validation and predictive power of Radiation Therapy Oncology Group (RTOG) recursive partitioning analysis classes for malignant glioma patients: a report using RTOG 90-06. Int J Radiat Oncol Biol Phys 40: 51–55
Shinoda J, Sakai N, Murase S, Yano H, Matsuhisa T, Funakoshi T (2001) Selection of eligible patients with supratentorial glioblastoma multiforme for gross total resection. J Neurooncol 52: 161–171
Souhami L, Seiferheld W, Brachman D, Podgorsak EB, Werner-Wasik M, Lustig R, Schultz CJ, Sause W, Okunieff P, Buckner J, Zamorano L, Mehta MP, Curran Jr WJ (2004) Randomized comparison of stereotactic radiosurgery followed by conventional radiotherapy with carmustine to conventional radiotherapy with carmustine for patients with glioblastoma multiforme: report of Radiation Therapy Oncology Group 93-05 protocol. Int J Radiat Oncol Biol Phys 60: 853–860
Soussain C, Ricard D, Fike JR, Mazeron J-J, Psimaras D, Delattre J-Y (2009) CNS complications of radiotherapy and chemotherapy. Lancet 374: 1639–1651
Spiegel BM, Esrailian E, Laine L, Chamberlain MC (2007) Clinical impact of adjuvant chemotherapy in glioblastoma multiforme : a meta-analysis. CNS Drugs 21: 775–787
Stupp R, Hegi ME, Mason WP, van den Bent MJ, Taphoorn MJ, Janzer RC, Ludwin SK, Allgeier A, Fisher B, Belanger K, Hau P, Brandes AA, Gijtenbeek J, Marosi C, Vecht CJ, Mokhtari K, Wesseling P, Villa S, Eisenhauer E, Gorlia T, Weller M, Lacombe D, Cairncross JG, Mirimanoff RO (2009) Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. Lancet oncol 10: 459–466
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJ, Belanger K, Brandes AA, Marosi C, Bogdahn U, Curschmann J, Janzer RC, Ludwin SK, Gorlia T, Allgeier A, Lacombe D, Cairncross JG, Eisenhauer E, Mirimanoff RO (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352: 987–996
Tapazoglou E, Lee M, Simpson J, Mohiuddin M, Nelson J, Kinzie J, Al-Sarraf M (1998) Concurrent azirdinyl-benzoquinone (AZQ) chemotherapy and radiotherapy (RT) in patients with malignant gliomas: RTOG Study. ASCO Annual Meeting, Los Angeles
Taphoorn MJB, Klein M (2004) Cognitive deficits in adult patients with brain tumours. Lancet Neurol 3: 159–168
Tsien C, Moughan J, Michalski JM, Gilbert MR, Purdy J, Simpson J, Kresel JJ, Curran WJ, Diaz A, Mehta MP (2009) Phase I three-dimensional conformal radiation dose escalation study in newly diagnosed glioblastoma: Radiation Therapy Oncology Group Trial 98-03. Int J Radiat Oncol Biol Phys 73: 699–708
Yung AW, Seiferheld W, Donahue B, Richards R, Kerlin K, Hug EB, Curran JW, Fine H (2001) A RTOG (Radiation Therapy Oncology Group) Phase II Study of Conventional Radiation Therapy Plus Thalidomide Followed by Thalidomide Post XRT for Supratentorial Glioblastoma. (Abstract 206) Proc Am Soc Clin Oncol 20
Acknowledgements
This study was supported by a RTOG grant U10 CA21661, CCOP grant U10 CA37422 and ATC grant U24 CA81647 from the National Cancer Institute. This manuscript's contents are solely the responsibility of us and do not necessarily represent the official views of the National Cancer Institute. YR Lawrence is supported by The ASCO Cancer Foundation Young Investigator Award. Any opinions, findings and conclusions expressed in this material are by us and do not necessarily reflect those of the American Society of Clinical Oncology or the ASCO Cancer Foundation. P Dicker is supported by the National Institutes of Health Grant CA10663, Tobacco Research Settlement Fund (State of Pennsylvania) and the Christine Baxter Fund.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Minesh Mehta has or has had the following roles in the last 2 years (2009–2010); Consultant: Adnexus, Bayer, Merck, Roche and Tomotherapy; Stock options: Colby, Pharmacyclics, Procertus and Stemina Tomotherapy; Data Safety Monitoring Boards: Apogenix; Board of Directors: Pharmacyclics; Medical Advisory Boards: Colby, Stemina and Procertus; Speaker: Merck. The other authors, including Dr Lawrence, declare no conflict of interest. Dr Lawrence had full access to all the data in the study and had final responsibility for the decision to submit for publication.
Additional information
Supplementary Information accompanies the paper on British Journal of Cancer website
Supplementary information
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Lawrence, Y., Wang, M., Dicker, A. et al. Early toxicity predicts long-term survival in high-grade glioma. Br J Cancer 104, 1365–1371 (2011). https://doi.org/10.1038/bjc.2011.123
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2011.123
Keywords
This article is cited by
-
Association between microRNAs 10b/21/34a and acute toxicity in glioblastoma patients treated with radiotherapy and temozolomide
Scientific Reports (2022)
-
SIRT in 2025
CardioVascular and Interventional Radiology (2022)
-
Yttrium-90 radioembolization as a possible new treatment for brain cancer: proof of concept and safety analysis in a canine model
EJNMMI Research (2020)
-
Provocative Question: Should Ketogenic Metabolic Therapy Become the Standard of Care for Glioblastoma?
Neurochemical Research (2019)
-
Treatment of Glioblastoma in the Elderly
Drugs & Aging (2018)