Abstract
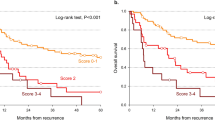
The prognostic weight of histological and biological factors was compared with that of known clinical prognostic factors in a population of 108 consecutive previously untreated patients with head and neck squamous cell carcinoma. Parameters studied were: tumour vascularisation, mitotic index, histological differentiation, nuclear grade, keratinisation, desmoplasia, growth pattern, inflammation, tumour emboli in peripheral vessels, keratins 6, 13, 19 immunohistochemical expression, cytofluorometric ploidy and S-phase. In multivariate analysis (Cox), only age and nodal status had a significant impact on the overall survival, whereas T stage was the only significant factor associated with locoregional failure. The cumulative incidence of metastases was correlated not only with age, T and N stage, but also with histological differentiation. All the other histological and biological factors studied failed to provide further prognostic information. These findings may help to select patients with high metastatic risk.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Janot, F., Klijanienko, J., Russo, A. et al. Prognostic value of clinicopathological parameters in head and neck squamous cell carcinoma: a prospective analysis. Br J Cancer 73, 531–538 (1996). https://doi.org/10.1038/bjc.1996.92
Issue Date:
DOI: https://doi.org/10.1038/bjc.1996.92
This article is cited by
-
P-Cadherin and WNT5A expression in assessment of lymph node metastasis in oral squamous cell carcinoma
Clinical Oral Investigations (2022)
-
The utility of MRI histogram and texture analysis for the prediction of histological diagnosis in head and neck malignancies
Cancer Imaging (2019)
-
Combinational chromosomal aneuploidies and HPV status for prediction of head and neck squamous cell carcinoma prognosis in biopsies and cytological preparations
Journal of Cancer Research and Clinical Oncology (2018)
-
The clinical relevance of Ki-67 expression in laryngeal squamous cell carcinoma
European Archives of Oto-Rhino-Laryngology (2015)