Abstract
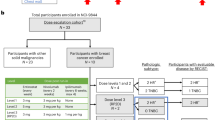
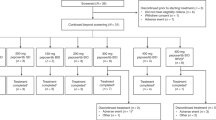
Lonidamine is a substituted indazole carboxylic acid with a unique mechanism of action and early clinical studies have reported anti-tumour activity. In a phase II study 32 patients with previously treated advanced breast cancer were given Lonidamine in a daily divided oral dose of 600 mg. Of 28 patients evaluable for response, three (11%) achieved a partial response (4-24+ months) and three (11%) a minor response. Two patients have stable disease (greater than 3 months) and 20 progressed. Toxicity was very mild. Sixteen (53%) of 31 patients had myalgia which lasted a median of 2 weeks. This was investigated with nuclear magnetic resonance spectroscopy in four patients but the changes were unrelated to the degree of myalgia. No other major side-effect was seen, and no dose reduction was required. Lonidamine pharmacokinetics have been investigated in 17 patients 1 month after the start of therapy. Lonidamine was detected in the plasma of all patients, but there was no clear relationship between Lonidamine levels and clinical response or toxicity. Lonidamine appears to be active against advanced breast cancer and its low toxicity would allow combination studies with chemotherapy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Mansi, J., de Graeff, A., Newell, D. et al. A phase II clinical and pharmacokinetic study of Lonidamine in patients with advanced breast cancer. Br J Cancer 64, 593–597 (1991). https://doi.org/10.1038/bjc.1991.356
Issue Date:
DOI: https://doi.org/10.1038/bjc.1991.356
This article is cited by
-
Directly targeting ASC by lonidamine alleviates inflammasome-driven diseases
Journal of Neuroinflammation (2022)
-
Targeting lonidamine to mitochondria mitigates lung tumorigenesis and brain metastasis
Nature Communications (2019)
-
Relative cytotoxicities of Adriamycin and epirubicin in combination with lonidamine against human bladder cancer cell lines
Urological Research (1995)