Abstract
The Ten Eleven Translocation (TET) enzymes have been found to be mutated in both diffuse large B-cell (DLBCL) and peripheral T-cell (PTCL) lymphomas resulting in DNA hypermethylation. Recent studies in embryonal stem cells showed that ascorbic acid (AA) is a cofactor for TET with a binding site at the catalytic domain, and enhances TET activity. We hypothesized that AA could potentially enhance TET activity in lymphoma cells to cause DNA demethylation, reactivate expression of tumor suppressor genes and enhance chemosensitivity. We demonstrate in vitro that AA treatment of DLBCL and PTCL cells using AA concentrations achievable intravenously increased TET activity leading to DNA demethylation. This epigenetic effect is independent of hydrogen peroxide. AA treatment increased the expression of SMAD1, a tumor suppressor gene known to be suppressed by methylation, and increased chemosensitivity of lymphoma cells. Twenty-nine percent (10/34) of unselected lymphoma patients had plasma AA levels that were deficient suggesting an additional clinical mechanism of TET hypofunction. These data indicate that AA has the potential to modify TET function in lymphoma and enhance chemosensitivity. In addition, the AA deficiency seen in some patients may further impair TET function and contribute to resistance. Clinical trials testing intravenous AA with chemotherapy are warranted.
Similar content being viewed by others
Introduction
Methylation of DNA is an important mechanism for control of gene expression. Changes in DNA methylation resulting in either silencing or activation of specific genes have been identified as a key mechanism of cancer progression. In diffuse large B-cell lymphoma (DLBCL) a high degree of methylation disruption and intra-tumor methylation heterogeneity has been found and is associated with inferior patient outcome.1 Low-dose DNA methyltransferase (DNMT) inhibitor therapy has been shown to reprogram chemoresistant cells to become chemosensitive by increasing the expression of tumor suppressor genes such as SMAD1 (a component of the Transforming Growth Factor- β pathway), that are suppressed by DNA methylation.2
TET (Ten Eleven Translocation) is a dioxygenase enzyme that converts 5-methylcytosine (5mC) to 5-hydroxymethylcytosine (5hmC) (Figure 1). This function of TET is a key step in DNA demethylation. 5hmC is further oxidized to 5-formylcytosine (5fC) and 5-carboxylcytosine (5caC) by TET. 5fC and 5caC are then converted to cytosine (C) by the base excision repair pathway involving the enzyme thymine DNA glycosylase. Loss of function of TET enzymes can occur with an inactivating mutation or hypoactivity of normal TET enzymes through inhibition by metabolic intermediates. Thus, a hypermethylated epigenome can be due to high DNMT expression/activity, low TET expression/activity or both. In lymphoma, TET-2 mutations are found most commonly in the T-cell lymphomas. For example, in angioimmunoblastic T-cell lymphoma TET-2 has been reported to be mutated in 76% of patients, with 50% harboring 2 or 3 mutations within the TET-2 gene.3 angioimmunoblastic T-cell lymphoma patients also have a high frequency of IDH2 mutations that can inhibit TET activity through the formation of 2-hydroxyglutarate.3 TET-2 mutation rate is also high in 38% of patients with peripheral T-cell lymphoma-not otherwise specified.4 Mutations in TET-2 have also been reported in 13% cases of DLBCL.5 This has been confirmed in a study of 1001 patients where missense and truncated mutations were present in 10% of cases.6 This signifies the critical role of TET in DNA demethylation in normal and malignant cells and highlights its potential as a translational target for epigenetic reprogramming.7 Currently, there are no clinically approved agents that can reactivate TET function.
Recent work in embryonic stem cells has demonstrated that ascorbic acid (AA) is a co-factor for the TET enzyme. Ascorbic acid binds to the catalytic domain of the TET enzyme to facilitate TET-mediated DNA demethylation.8, 9 This finding, together with the known high TET mutation rate in non-Hodgkin lymphoma (NHL) and the potential for clinical translation, led us to hypothesize that AA could enhance TET activity in lymphoma cells producing DNA demethylation and re-expression of important tumor suppressor genes with subsequent increase in chemosensitivity. We also sought to explore whether patients with lymphoma could be deficient in AA, potentially identifying another mechanism of TET hypofunction. In this report, we provide results of our studies that support this hypothesis and provide preclinical rationale for further studies.
Materials and methods
Cell culture
The DLBCL cell line OC-LY1 was a gift from Dr Louis Staudt (National Institutes of Health). The cells were cultured in Iscove’s modified Dulbecco’s medium supplemented with 20% v/v human serum and 1% penicillin/streptomycin. Karpas 299, a T-cell NHL line, was purchased from American Type Culture Collection and was cultured in RPMI1640 media supplemented with 10% v/v fetal bovine serum and 1% v/v penicillin/streptomycin. Jeko, a mantle cell NHL line was obtained from the American Type Culture Collection (ATCC, Manassas, VA, USA) and grown in RPMI-1640 with 10% fetal bovine serum.
Nuclear protein extraction and in vitro TET enzymatic activity analysis
Cells were treated with different concentrations of pH neutralized AA, with or without catalase. Exposure time to 1 mM AA was 2 h (taking into account the plasma concentration curve with intravenous (i.v.) AA10 and potential differences between plasma concentrations with that of tumor microenvironment) followed by the cells being washed and incubated in fresh media for 24 h. Nuclear protein was then isolated from cells using the EpiQuik nuclear extraction kit (Epigentek Group Inc, Farmingdale, NY, USA), according to the manufacturer’s instructions. TET enzymatic activity was measured by using the Enzyme Linked ImmunoSorbent Assay (ELISA)-based Epigenase 5mC Hydroxylase TET Activity/Inhibition Assay Kit (Fluorometric) according to the manufacturer’s instructions. This technique relies on the conversion of methylated products at the bottom of the wells to hydroxymethylated products by the TET enzyme present in the nuclear extract. Thus the amount of hydroxymethylated products formed is a measure of the TET activity of the nuclear extract harvested from the cells being tested. Incubation time of nuclear lysates was 90 min. Six micrograms of nuclear lysate was used per well for measurement of TET activity.
Measurement of 5mC and 5hmC levels by mass spectrometry
DNA hydrolysis was performed as previously described.11 Briefly, 1 μg of genomic DNA was first denatured by heating at 100 °C. Five units of Nuclease P1 (Sigma-Aldrich, St Louis, MO, USA, Cat # N8630) were added and the mixture incubated at 45 °C for 1 h. A 1/10 volume of 1 M ammonium bicarbonate and 0.002 units of venom phosphodiesterase 1 (Sigma-Aldrich, Cat # P3243) were added to the mixture and the incubation continued for 2 h at 37 °C. Next, 0.5 units of alkaline phosphatase (Invitrogen, Carlsbad, CA, USA, Cat # 18009-027) were added, and the mixture incubated for 1 h at 37 °C. Quantification was performed using a Liquid Chromatography Electrospray Ionization Tandem Mass Spectrometry (LC-ESI-MS/MS) system in the multiple reaction monitoring mode as described11 with some modifications. Before injection into the Zorbax Eclipse Plus C18 2.1 mm × 150 mm column (1.8 μm particle size) (Agilent, Santa Clara, CA, USA, Cat # 959759-902), the reactions were diluted 10-fold to dilute out the salts and the enzymes. Samples were analyzed on an Agilent 1290 series liquid chromatography instrument in tandem with the Agilent 6490 triple quadrupole mass spectrometer.
Cell viability assays
Cells were incubated at varying concentrations and time periods with L-ascorbic acid (Sigma-Aldrich, Cat# 50-81-7) with or without catalase at 100 μg/ml (Sigma-Aldrich, Cat# 9001-05-2). Viability was assessed by addition of Cell Titer Blue (Promega, Madison, WI, USA) and measured via Fluostar Omega Microplate reader (BMG Labtech, Offenburg, Germany). We found that antioxidant drugs interfere with cell viability measurements by assays that rely on the reducing property of viable cells.12 They directly reduce the reagent substrate to the reduced fluorescent form, giving spurious results. The protocol modification to counter this interference has been described12, 13 and was used in this study. Cell viability was also assessed with trypan blue staining and manual counting under the microscope, with viable cells preventing the permeation of trypan blue stain through the membrane.
qRT-PCR for SMAD1
Total RNA was extracted from 5 × 106 cells with the use of the RNeasy Mini Plus kit (Qiagen, Hilden, Germany) and eluted in RNAse-free water. cDNA was synthesized using high capacity RNA-to-cDNA kit (Applied Biosystems, Foster City, CA, USA). SMAD1 mRNA expression was measured by qRT-PCR using the SYBR Green method with gene-specific primers. The data was normalized using HPRT as housekeeping gene and ddCT method. SMAD1 forward primer: 5′-TGAACCATGGATTTGAGACAG-3′ and reverse primer: 5′-ACATCCTGGCGGTGGTATT-3′
Plasma ascorbic acid levels in lymphoma patients
Plasma AA levels were measured in patients with known lymphoma who had provided written informed consent to be enrolled in the Mayo Clinic/Iowa Lymphoma SPORE. This study includes permission for patient record review and periodic blood sampling. This protocol was approved by the Mayo Clinic IRB. Clinical information on lymphoma type and presence of bulky disease was obtained through patient record review. The AA levels were measured in the Mayo Medical Laboratories using fresh samples and standard assay procedures. The normal range is 0.4–2.0 mg/dl.
Results
AA enhances TET activity in LY-1 and Karpas 299 lymphoma cell lines leading to genome-wide demethylation and an increase in the hydroxymethylcytosine fraction
Given that AA is a cofactor for TET function, we tested the ability of AA supplementation to produce DNA demethylation in the DLBCL LY-1 and T-cell NHL Karpas 299 cell lines. Exposure of the LY-1 and Karpas 299 lymphoma cells to pH neutralized AA increased TET activity (Figures 2a and b). To determine the consequence of this AA-induced increased TET activity on DNA methylation, mass spectrometry (LC-ESI-MS/MS) was performed to measure genome-wide 5mC and 5hmC content. AA treatment produced a progressive decrease in DNA methylation and an increase in the hydroxymethylation fraction in a dose-dependent manner, correlating with the increase in TET activity (Figures 2c and d).
AA enhances TET activity in lymphoma cell lines LY-1 and Karpas 299 leading to demethylation and increase in hydroxymethylation fraction: (a and b) TET activity of LY-1 and Karpas 299 cells with and without ascorbic acid (AA) treatment. Cultured cells were exposed to 1 mM pH neutralized AA for 2 h, then washed and cultured in fresh media for 24 h prior to harvesting the nuclear extract. The fresh nuclear extract was immediately tested for TET activity using the Epigentek TET activity kit, as described in the Methods section. (c and d) Genome-wide DNA methylation/hydroxymethylation levels were assessed with and without AA treatment by mass spectrometry (LC-ESI-MS/MS described in the ‘Methods’ section). Total 5mC levels decrease and 5hmc/C levels increase with increasing concentration of AA. (paired t-test; *P<0.05; **P<0.005; ***P<0.0005; n=2).
AA-induced epigenetic effects are independent of hydrogen peroxide (H2O2)
AA, when added to culture media, generates H2O2 through the following reactions:
1. Ascorbate reduces catalytic metal ions such as ferric ions to ferrous ions.

2. The ferrous ions react with oxygen to form superoxide radical

3. Superoxide radicals then dismutes to H2O2 and O2

H2O2 is toxic to cells; therefore, while studying the epigenetic effects of AA in vitro, it becomes important to have a control with catalase to neutralize the H2O2 that is generated. Addition of catalase did not change the epigenetic effects of AA (Figure 3), proving that the effect was independent of H2O2.
Epigenetic effects of AA are independent of hydrogen peroxide (H2O2): Addition of catalase to 1 mM AA does not change the %5hmC. 10 mM AA produces more 5hmC/C+mC+hmC even in the presence of catalase. It should be noted that 10 mM AA could not be tested without the addition of catalase due to H2O2-induced cytotoxicity. (paired t test; *P<0.05; n=2).
AA reactivates SMAD1, a critical contributor of chemosensitization in DLBCL cells
SMAD1, a component the TGF/BMP pathway, has been shown to be hypermethylated and suppressed in chemoresistant DLBCL cell lines (including LY-1) and chemoresistant patient samples.2 Reactivation of epigenetically silenced SMAD1 with the DNMT inhibitor azacytidine, as well as SMAD1 transfection, has been shown to contribute to chemosensitization to conventional anti-tumor agents.2 We found that treatment of LY-1 cells with pharmacologic doses of AA leads to the reactivation of SMAD1, likely through TET-mediated demethylation. Addition of catalase had no effect on transcript abundance, again indicating that the upregulation of SMAD1 was independent of H2O2 (Figure 4).
AA treatment increases expression of SMAD1: Exposure of LY-1 cells to increasing concentrations of AA treatment for 2 h followed by 24 h incubation with fresh media led to increased SMAD1 transcripts as measured by quantitative RT-PCR. Addition of catalase to inactivate H2O2- mediated cytotoxicity did not change the transcript abundance, indicating that the upregulation of SMAD1 with 1 mM AA was not mediated by H2O2. 10 mM AA+ catalase significantly increased expression of SMAD1 compared to control (paired t-test: P=0.004; n=2). 10 mM AA without catalase is very cytotoxic to the cells due to the amount of H2O2 generated and therefore cannot be used by itself to study epigenetic effects.
High dose AA is cytotoxic to lymphoma cells and decreases cell viability
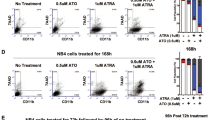
The dual mechanisms of AA action (H2O2 generation and TET activation) led us to test the cytotoxic effects of AA specifically on lymphoma cell lines. Lymphoma cell lines LY-1 (DLBCL), Karpas 299 (T-cell NHL) and Jeko (mantle cell NHL) were exposed to pH neutralized AA at concentrations ranging between 0.1 and 10 mM for 2 h. The 0.1 mM level represents physiologic AA levels; the AA concentration of 10 mM is attainable only with IV administration at 1 g/kg due to tight gastrointestinal regulation.10 AA levels of 0.1 mM were ineffective at inducing cytotoxicity; however, there were no viable cells detected after the 10 mM AA exposure (Figure 5a). Addition of catalase along with the 10 mM AA resulted in almost complete reversal of the cytotoxicity, confirming that the acute cytotoxicity seen in vitro with short-term AA exposure is due to H2O2 generation when AA is added to the media (Figures 5b and c). The reversal of short-term exposure cytotoxicity was confirmed by a second method using the Cell Titer blue cell viability assay (Figure 5d).
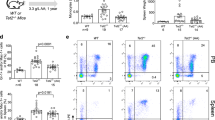
(a) AA is cytotoxic to lymphoma cell lines through H2O2 (with short-term exposure) and non-H2O2 mechanisms (with longer term exposure): Cell viability as measured by cell count after trypan blue staining. LY-1 (diffuse large B-cell lymphoma), Karpas 299 (T-cell lymphoma) and Jeko (mantle cell) lymphoma cells were exposed to pH neutralized AA at 0.1 mM and 1 mM for 2 h. Cells were then washed and cultured in fresh media for 24 h after treatment and the number of viable cells manually counted under the microscope. (b) LY-1 and Karpas 299 exposed to 10 mM AA, with and without catalase. (c) Cell viability measured with Cell Titer Blue assay revealed reduction of metabolic viability with 1 mM AA exposure for 2 h that was reversed by catalase. (d) LY-1 cells exposed to high dose AA with catalase for 24 h. (e) LY-1 cells exposed to 5 mM AA with catalase for 72 h; relative viability compared to control (with catalase) at 24 and 72 h (paired t-test; *P<0.05; **P<0.005, ***P<0.0005; n=2).
In order to investigate the epigenetic effects of high dose AA on lymphoma cell proliferation inhibition, we used catalase to nullify the H2O2 effects. Exposure to 1 mM and 5 mM AA with catalase for 24 h resulted in reduced LY-1 cell viability compared to catalase control (Figure 5e). Furthermore, exposure to 5 mM AA over 72 h with catalase resulted in progressive reduction in cell viability (Figure 5f). These results support the notion that AA could exert anti-tumor effects through non-H2O2 mechanisms with a longer term exposure.
AA has a chemosensitizing effect in lymphoma cell lines
To learn if AA could sensitize lymphoma cells to doxorubicin and cisplatin (agents commonly used in salvage lymphoma therapy), we pretreated cells with AA for 6 h with and without catalase. AA enhanced the sensitivity of Karpas 299 to doxorubicin (P=0.02) and the LY-1 cell line to cisplatin (P=0.01) (Figure 6).
AA pretreatment enhances chemosensitivity: Pre-treatment of Karpas 299 cell line with 1 mM AA plus catalase for 6 h increased the chemosensitivity to doxorubicin (paired t-test; P=0.02 comparing doxorubicin to doxorubicin+ pre-treatment with AA+C). Pre-treatment of the LY-1 cell line with 1 mM AA plus catalase for 6 h increases the sensitivity to cisplatin (paired t-test; P=0.01 comparing cisplatin to cisplatin+ pre-treatment with AA+c). Catalase pre-treatment by itself did not enhance chemosensitivity. Taken together, AA treatment even after H2O2 neutralization, enhanced chemosensitivity to doxorubicin and cisplatin in vitro in these cell lines (paired t-test; *P<0.05; **P<0.005, ***P<0.0005; n=2).
Low plasma AA levels are frequent in lymphoma patients with high bulk disease
Plasma samples were collected from 34 unselected patients with lymphoma. The disease types included 31 NHL and 3 Hodgkin lymphoma. Within the NHL group there were 9 DLBCL, 7 high grade NOS, 2 MCL, 3 T-cell NHL, 1 Burkitt lymphoma and 9 low grade/indolent NHL.
Twenty-nine percent (10/34) of the patients had AA insufficiency (levels <0.4 mg/dl). Sixty-four percent (9/14) of patients with clinical high-burden lymphoma had low AA levels (mean=0.39 mg/dl; range 0–1.2 mg/dl) compared to 5% (1/20) of those with low burden disease (mean 1.1 (range 0.2–2); P<0.001) (Figure 7).
Discussion
Despite significant advances over the last two decades, the treatment of NHL, especially in the relapsed/refractory setting, remains inadequate. Recent progress in the field has been accomplished with the development of novel agents that target a specific signal transduction pathway or modulate the immune system for host benefit. Examples of these advances include inhibitors of the PI3K/mTOR pathway;14, 15, 16 Bruton’s tyrosine kinase inhibitors,17 immunomodulatory agents that have multiple effects on normal and malignant cells18, 19, 20 and immune checkpoint inhibitors.21
Targeting the DNA hypermethylation in lymphoma has to date been limited to inhibitors of the DNMT enzyme. Clozel et al.2 demonstrated in vitro that azacytidine could inhibit DNMT and sensitize lymphoma cells to standard chemotherapy agents. Based on those preclinical studies, azacytidine is currently being studied days 1–5 before standard RCHOP delivered on day 8 in a phase I/II study for newly diagnosed DLBCL (NCT01004991). In our study, we have demonstrated that demethylation can be induced in vitro by enhancement of TET activity with AA. The theoretical advantage of this approach is that it removes existing methyl groups from the cytosine residues rather than inhibiting methylation in future generations of cells with the DNMT inhibitor approach.
TET-2 mutation has been found in variable frequencies (76% in angioimmunoblastic T-cell lymphoma,3 38% in peripheral T-cell lymphoma-not otherwise specified,4 13% in DLBCL5) depending on the type of NHL. Apart from inactivating mutations, the activity of TET can also be suppressed through the accumulation of abnormal metabolic intermediates. This mechanism occurs through competitive inhibition of 2-oxoglutarate, a component of the Krebs cycle, that also serves as a cofactor for the TET enzymes. TET and its cofactors—AA, Fe2+ and 2-oxoglutarate—play a central role in DNA demethylation thereby influencing the expression of key tumor suppressor genes. Increasing TET enzyme activity, either through the wild-type allele in TET mutated lymphoma or the unmutated but inhibited enzyme, represents potential therapeutic opportunities.
The recent demonstration that AA is a direct cofactor for the TET enzyme with a binding site at the enzyme’s catalytic domain9 led us to investigate whether AA could enhance TET function in lymphoma cells. We used an ELISA-based method to demonstrate that TET function in vitro can indeed be enhanced with AA treatment. We further corroborated these data by showing an increase in the 5hmC fraction of AA-treated lymphoma cells by mass spectrometry (LC/ESI-MS/MS). Furthermore, we demonstrate that AA induces reactivation of SMAD1, an important chemosensitizing tumor suppressor gene, known to be suppressed through methylation in resistant/refractory DLBCL. The epigenetic effects were more profound with doses achieved through the IV route with the short exposure time, mimicking the bioavailability curves of IV AA10 and considering potential differences between plasma concentrations and that of the tumor microenvironment.
Our results reveal that the H2O2 generated when AA is added to culture media does not play a role in the epigenetic activities of AA. This is an important observation since H2O2 is responsible for the acute cytotoxicity of cancer cells induced with short-term in vitro exposure to AA. This was demonstrated in this study and others,22, 23, 24 by showing the complete reversal of short-term exposure cytotoxicity with catalase. AA thus mediates cancer cell inhibition through at least two mechanisms—epigenetic and H2O2. The relative importance of these mechanisms in vivo remains unclear. In order for AA to generate H2O2, it requires the presence of free catalytic metal ions (as shown in reactions 1–3 above), that are plentiful in vitro but may be restricted in the tumor microenvironment.
TET dioxygenase could also be less functional in lymphoma cells due to a loss of cofactor (AA) availability. Older studies (summarized in the review by Cameron and Pauling25) and limited recent studies26, 27 have suggested the possibility that cancer patients may have low plasma AA levels in vivo compared to the general population.28 In a small pilot study, we prospectively analyzed plasma AA levels from patients with lymphoma and confirmed that AA deficiency can occur and appears to be associated with high-bulk active disease (Figure 7). Prospective studies are needed to clarify the true incidence of AA deficiency by tumor type and stage, how AA levels relate to clinical outcome, how blood levels relate to the methylation landscape of the tumor, and whether replacement of AA by oral or i.v. could contribute to reactivation of TET activity and patient benefit. When AA is delivered i.v. at doses of 1–1.25 g/kg over 90 min, peak AA concentrations are reached that are more than 100-fold higher than the oral route (due to tight gastrointestinal regulation) or the normal range.22, 23, 24, 29, 30 Early phase trials in solid tumors have demonstrated that these i.v. AA doses are not only well-tolerated with potential anti-cancer activity, but can also reduce the toxicity of the standard chemotherapy agents delivered along with the i.v. AA.10, 31, 32, 33
It is unclear at this point whether intra-tumor methylation reprogramming can be accomplished in vivo with AA or what dose and schedule is needed. However, the rationale to pursue these trials is strong based on our preclinical studies in lymphoma. Given that the epigenetic effects of AA in vitro were more profound with doses achieved with the i.v. route, the potential additional benefit with H2O2 generation with i.v., the results to date in solid tumors demonstrating reasonable tolerance of the i.v. schedule, and the lack of effect in cancer patients with oral AA when taken together provide strong rationale for future clinical trials of the i.v. schedule.
Considering the TET-mediated demethylation effect, AA could potentially also be a promising therapeutic strategy against other hypermethylated malignancies such as chronic myelomonogenous leukemia (60–70% of cases with TET2 mutations),34 myelodysplastic syndrome,35 TET-2 mutated and IDH mutated acute myelogeneous leukemia (2-hydroxyglutarate mediated suppression of TET),36, 37 clear cell renal cell carcinoma,38, 39 and succinate dehydrogenase mutated paraganglioma.40 Given that most of these TET-2 mutations are uniallelic, it is possible that the activity of the wild-type copy could be optimized by AA and produce therapeutic benefit.
The results of these new insights into AA biology and the results of our studies indicate that i.v. AA may have a therapeutic role in combination with conventional chemotherapy for relapsed NHL. We have proposed a phase 2 study combining i.v. AA with salvage chemotherapy in relapsed/refractory DLBCL with appropriate correlative research studies that aim to demonstrate whether AA can contribute to improvement of salvage therapy outcome through these novel mechanisms of action.
References
De S, Shaknovich R, Riester M, Elemento O, Geng H, Kormaksson M et al. Aberration in DNA methylation in B-cell lymphomas has a complex origin and increases with disease severity. PLoS Genet 2013; 9: e1003137.
Clozel T, Yang S, Elstrom RL, Tam W, Martin P, Kormaksson M et al. Mechanism-based epigenetic chemosensitization therapy of diffuse large B-cell lymphoma. Cancer Discov 2013; 3: 1002–1019.
Odejide O, Weigert O, Lane AA, Toscano D, Lunning MA, Kopp N et al. A targeted mutational landscape of angioimmunoblastic T-cell lymphoma. Blood 2014; 123: 1293–1296.
Lemonnier F, Couronne L, Parrens M, Jais JP, Travert M, Lamant L et al. Recurrent TET2 mutations in peripheral T-cell lymphomas correlate with TFH-like features and adverse clinical parameters. Blood 2012; 120: 1466–1469.
Cerami E, Gao J, Dogrusoz U, Gross BE, Sumer SO, Aksoy BA et al. The cBio cancer genomics portal: an open platform for exploring multidimensional cancer genomics data. Cancer Discov 2012; 2: 401–404.
Jenny Zhang AR, Love C, Moffitt AB, Rajagopalan D, Leppä S, Pasanen A et al. Integrative genetic and clinical analysis through whole exome sequencing in 1001 diffuse large B cell lymphoma (DLBCL) patients reveals novel disease drivers and risk groups. Blood 2016; 128: 1087.
Scourzic L, Mouly E, Bernard OA . TET proteins and the control of cytosine demethylation in cancer. Genome Med 2015; 7: 9.
Blaschke K, Ebata KT, Karimi MM, Zepeda-Martinez JA, Goyal P, Mahapatra S et al. Vitamin C induces Tet-dependent DNA demethylation and a blastocyst-like state in ES cells. Nature 2013; 500: 222–226.
Yin R, Mao SQ, Zhao B, Chong Z, Yang Y, Zhao C et al. Ascorbic acid enhances Tet-mediated 5-methylcytosine oxidation and promotes DNA demethylation in mammals. J Am Chem Soc 2013; 135: 10396–10403.
Hoffer LJ, Levine M, Assouline S, Melnychuk D, Padayatty SJ, Rosadiuk K et al. Phase I clinical trial of i.v. ascorbic acid in advanced malignancy. Ann Oncol 2008; 19: 1969–1974.
Figueroa ME, Abdel-Wahab O, Lu C, Ward PS, Patel J, Shih A et al. Leukemic IDH1 and IDH2 mutations result in a hypermethylation phenotype, disrupt TET2 function, and impair hematopoietic differentiation. Cancer Cell 2010; 18: 553–567.
Shenoy N, Stenson M, Lawson J, Abeykoon J, Patnaik M, Wu X et al. Drugs with anti-oxidant properties can interfere with cell viability measurements by assays that rely on the reducing property of viable cells. Lab Invest 2017; e-pub ahead of print 27 February 2017; doi:10.1038/labinvest.2017.18.
Shenoy N, Wu X, Witzig T . Protocol modification to determine the cytotoxic potential of drugs using cell viability assays that rely on the reducing property of viable cells. Protoc Exch 2017; e-pub ahead of print 20 March 2017; doi:10.1038/protex.2017.029.
Gopal AK, Kahl BS, de Vos S, Wagner-Johnston ND, Schuster SJ, Jurczak WJ et al. PI3Kdelta inhibition by idelalisib in patients with relapsed indolent lymphoma. N Engl J Med 2014; 370: 1008–1018.
Johnston PB, LaPlant B, McPhail E, Habermann TM, Inwards DJ, Micallef IN et al. Everolimus combined with R-CHOP-21 for new, untreated, diffuse large B-cell lymphoma (NCCTG 1085 [Alliance]): safety and efficacy results of a phase 1 and feasibility trial. Lancet Haematol 2016; 3: e309–e316.
Witzig TE, LaPlant B, Habermann TM, McPhail E, Inwards DJ, Micallef IN et al. High rate of event-free survival at 24 months (EFS24) with everolimus/RCHOP for untreated diffuse large B-cell lymphoma: updated results from NCCTG N1085 (Alliance). Blood Cancer J 2017; 7: e576.
Aalipour A, Advani RH . Bruton's tyrosine kinase inhibitors and their clinical potential in the treatment of B-cell malignancies: focus on ibrutinib. Therapeut Adv Hematol 2014; 5: 121–133.
Gribben JG, Fowler N, Morschhauser F . Mechanisms of action of lenalidomide in B-cell non-Hodgkin lymphoma. J Clin Oncol 2015; 33: 2803–2811.
Wiernik PH, Lossos IS, Tuscano JM, Justice G, Vose JM, Cole CE et al. Lenalidomide monotherapy in relapsed or refractory aggressive non-Hodgkin's lymphoma. J Clin Oncol 2008; 26: 4952–4957.
Witzig TE, Nowakowski GS, Habermann TM, Goy A, Hernandez-Ilizaliturri FJ, Chiappella A et al. A comprehensive review of lenalidomide therapy for B-cell non-Hodgkin lymphoma. Ann Oncol 2015; 26: 1667–1677.
Thanarajasingam G, Thanarajasingam U, Ansell SM . Immune checkpoint blockade in lymphoid malignancies. FEBS J 2016; 283: 2233–2244.
Chen Q, Espey MG, Krishna MC, Mitchell JB, Corpe CP, Buettner GR et al. Pharmacologic ascorbic acid concentrations selectively kill cancer cells: action as a pro-drug to deliver hydrogen peroxide to tissues. Proc Natl Acad Sci USA 2005; 102: 13604–13609.
Chen Q, Espey MG, Sun AY, Lee JH, Krishna MC, Shacter E et al. Ascorbate in pharmacologic concentrations selectively generates ascorbate radical and hydrogen peroxide in extracellular fluid in vivo. Proc Natl Acad Sci USA 2007; 104: 8749–8754.
Chen Q, Espey MG, Sun AY, Pooput C, Kirk KL, Krishna MC et al. Pharmacologic doses of ascorbate act as a prooxidant and decrease growth of aggressive tumor xenografts in mice. Proc Natl Acad Sci USA 2008; 105: 11105–11109.
Cameron E, Pauling L, Leibovitz B . Ascorbic acid and cancer: a review. Cancer Res 1979; 39: 663–681.
Liu M, Ohtani H, Zhou W, Orskov AD, Charlet J, Zhang YW et al. Vitamin C increases viral mimicry induced by 5-aza-2'-deoxycytidine. Proc Natl Acad Sci USA 2016; 113: 10238–10244.
Huijskens MJ, Wodzig WK, Walczak M, Germeraad WT, Bos GM . Ascorbic acid serum levels are reduced in patients with hematological malignancies. Results Immunol 2016; 6: 8–10.
Hampl JS, Taylor CA, Johnston CS . Vitamin C deficiency and depletion in the United States: the Third National Health and Nutrition Examination Survey, 1988 to 1994. Am J Public Health 2004; 94: 870–875.
Du J, Cullen JJ, Buettner GR . Ascorbic acid: chemistry, biology and the treatment of cancer. Biochim Biophys Acta 2012; 1826: 443–457.
Verrax J, Calderon PB . Pharmacologic concentrations of ascorbate are achieved by parenteral administration and exhibit antitumoral effects. Free Radic Biol Med 2009; 47: 32–40.
Monti DA, Mitchell E, Bazzan AJ, Littman S, Zabrecky G, Yeo CJ et al. Phase I evaluation of intravenous ascorbic acid in combination with gemcitabine and erlotinib in patients with metastatic pancreatic cancer. PLoS One 2012; 7: e29794.
Stephenson CM, Levin RD, Spector T, Lis CG . Phase I clinical trial to evaluate the safety, tolerability, and pharmacokinetics of high-dose intravenous ascorbic acid in patients with advanced cancer. Cancer Chemother Pharmacol 2013; 72: 139–146.
Ma Y, Chapman J, Levine M, Polireddy K, Drisko J, Chen Q . High-dose parenteral ascorbate enhanced chemosensitivity of ovarian cancer and reduced toxicity of chemotherapy. Sci Transl Med 2014; 6: 222ra18.
Patnaik MM, Zahid MF, Lasho TL, Finke C, Ketterling RL, Gangat N et al. Number and type of TET2 mutations in chronic myelomonocytic leukemia and their clinical relevance. Blood Cancer J 2016; 6: e472.
Issa JP . Epigenetic changes in the myelodysplastic syndrome. Hematol/oncol clin North Am 2010; 24: 317–330.
Rasmussen KD, Jia G, Johansen JV, Pedersen MT, Rapin N, Bagger FO et al. Loss of TET2 in hematopoietic cells leads to DNA hypermethylation of active enhancers and induction of leukemogenesis. Genes Dev 2015; 29: 910–922.
Schoofs T, Berdel WE, Muller-Tidow C . Origins of aberrant DNA methylation in acute myeloid leukemia. Leukemia 2014; 28: 1–14.
Hu CY, Mohtat D, Yu Y, Ko YA, Shenoy N, Bhattacharya S et al. Kidney cancer is characterized by aberrant methylation of tissue-specific enhancers that are prognostic for overall survival. Clin Cancer Res 2014; 20: 4349–4360.
Shenoy N, Vallumsetla N, Zou Y, Galeas JN, Shrivastava M, Hu C et al. Role of DNA methylation in renal cell carcinoma. J Hematol Oncol 2015; 8: 88.
Letouze E, Martinelli C, Loriot C, Burnichon N, Abermil N, Ottolenghi C et al. SDH mutations establish a hypermethylator phenotype in paraganglioma. Cancer Cell 2013; 23: 739–752.
Acknowledgements
This work was supported in part by National Institutes of Health Grant No. P50 CA97274 to the University of Iowa/Mayo Clinic Lymphoma Specialized Program of Research Excellence, the Henry J. Predolin Foundation and NIH SIG grant for the Triple Quadrupole Mass Spectrometer System (1S10RR029398).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Shenoy, N., Bhagat, T., Nieves, E. et al. Upregulation of TET activity with ascorbic acid induces epigenetic modulation of lymphoma cells. Blood Cancer J. 7, e587 (2017). https://doi.org/10.1038/bcj.2017.65
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bcj.2017.65
This article is cited by
-
High-Dose Vitamin C Prevents Secondary Brain Damage After Stroke via Epigenetic Reprogramming of Neuroprotective Genes
Translational Stroke Research (2022)
-
TETology: Epigenetic Mastermind in Action
Applied Biochemistry and Biotechnology (2021)
-
Anticancer mechanisms of phytochemical compounds: focusing on epigenetic targets
Environmental Science and Pollution Research (2021)
-
Targeting cancer vulnerabilities with high-dose vitamin C
Nature Reviews Cancer (2019)
-
Reversal of TET-mediated 5-hmC loss in hypoxic fibroblasts by ascorbic acid
Laboratory Investigation (2019)