Abstract
Aim:
To reinvestigate the characteristics of reserpine-induced gastric mucosal lesions (GMLs).
Methods:
The GML-inducing effect of reserpine and the time-course of recovery from reserpine-induced GMLs were examined in Sprague-Dawley (SD) rats. The GML-inducing and blood pressure-decreasing effects of Compound Hypotensive Tablets (CHTs) were investigated in spontaneously hypertensive rats (SHRs). Intracerebroventricular (icv) injection and vagotomy were performed to verify the central vagal mechanism in reserpine-induced GMLs.
Results:
Single intraperitoneal (ip) injections of reserpine (0.25, 0.5, 1, 2, 4, and 6 mg/kg) dose-dependently induced GMLs in SD rats. Both single and repeated (2 weeks) oral administrations of reserpine led to slight GMLs at doses of 24 mg/kg and 10 mg/kg, respectively. Blood pressure was significantly decreased in SHRs after 2 months of CHT administration (0.01 and 0.03 mg/kg; doses were expressed as the amount of reserpine in the CHT). CHT doses of 0.3 mg/kg induced GMLs, but 0.1 mg/kg did not. Examining the time course of recovery from GMLs, severe GMLs occurred 18 h after ip reserpine (4 mg/kg), obviously lessened at 1 week and healed spontaneously at 3 weeks. Intracerebroventricular injections of reserpine caused GMLs at much lower doses (0.08 and 0.4 mg/kg), and reserpine-induced GMLs were greatly inhibited by vagotomy, suggesting the involvement of a central vagal mechanism.
Conclusion:
Reserpine-induced GMLs were dose-dependent, and the lesions healed spontaneously within 3 weeks. Long-term treatment with CHT at doses adequate to decrease blood pressure will not induce GMLs. A central vagal mechanism was involved in reserpine-induced GMLs.
Similar content being viewed by others
Introduction
Hypertension is one of the major risk factors for the leading causes of death in adult populations worldwide. If not properly treated, hypertension can lead to stroke, heart attack, heart failure and kidney disease1, 2, 3, 4, 5. Hypertension often requires lifelong treatment with one or more antihypertensive medications. Treatment with medication for hypertension can reduce the incidence of stroke (by about 35%−40%), heart attack (by 20%–25%), and heart failure (by more than 50%)6.
Sixty years ago, people suffered from hypertension because of a lack of antihypertensive drugs. Reserpine, first isolated from the root of the medicinal plant Rauvolfia serpentina in 1952, revolutionized the treatment of hypertension. In the following two decades, reserpine was used extensively to manage hypertension7, 8. However, overdose and long-term use of reserpine can produce adverse effects, such as gastric mucosal lesions (GMLs), depression and sexual dysfunction9, 10, 11. These side effects restricted its clinical use. At present, reserpine is not the first-line antihypertensive drug and is seldom used alone. However, many antihypertensive compounds containing reserpine, such as Compound Hypotensive Tablets (CHTs) and Compound Reserpine Tablets are still widely used in China because of their effectiveness and low cost. The doses of reserpine used in the antihypertensive compounds are very low compared with the doses of reserpine that were used 40 years ago. Therefore, it is necessary to re-evaluate the side effects of different doses of reserpine. The present work focused mainly on the GMLs induced by reserpine and CHT.
It is considered that reserpine induces gastric damage by reducing sympathetic tone and increasing cholinergic tone, which leads to excessive acid secretion12, 13, 14. In this study, vagotomy and intracerebroventricular (icv) injection of reserpine were performed to further demonstrate the role of a central vagal mechanism in reserpine-induced GMLs. In addition, to investigate the characteristics of reserpine-induced GMLs in detail, the dose-effect of reserpine in causing GMLs was examined in two administration routes: intraperitoneal (ip) and oral. The time course of recovery from reserpine-induced GMLs was also studied. Finally, the blood pressure-reducing and GML-inducing effect of CHT, a combination drug that includes reserpine, were evaluated to determine its clinical safety.
Materials and methods
Animals and drugs
Male Sprague-Dawley (SD) rats (weighing 200–240 g) were purchased from Sino-British SIPPR/BK Lab Animal Ltd. Male spontaneously hypertensive rats (SHRs, 4–5 months old) were provided by the Animal Center of the Second Military Medical University (Shanghai, China). The animals were housed under controlled conditions (temperature, 23–25 °C; in light from 8:00 to 20:00) and received standard animal chow and tap water ad libitum. All animals used in this study received humane care in compliance with the Institutional Guidelines for the Health and Care of Experimental Animals.
Reserpine and CHT were provided by Beijing Shuanghe Pharmaceutical Co, Ltd (Beijing, China). The composition (mg/tablet) of CHT is as follows: hydrochlorothiazide 12.5, triamterene 12.5, hydralazine 12.5, and reserpine 0.1. In this study, the CHT dose is expressed as the amount of reserpine in the tablet.
GML evaluation
Animal was sacrificed and the stomach was removed from the abdomen after the pyloric sphincter was tied with a surgical suture. From the esophagus side, 5 mL of 10% formalin solution was injected into the stomach. The distended stomach was then immediately tied on the esophagus side with another surgical suture to prevent formalin leakage. The stomach was immersed in 10% formalin solution to fix the outer layer. 24 h later, each stomach was dissected along the greater curvature and rinsed with tap water to remove the gastric contents. The ulcerative lesion index of each rat was calculated by adding the values in Table 1, according to methodology described by Gamberini et al15.
Intracerebroventricular injection
The rats were anesthetized intraperitoneally with a combination of ketamine (40 mg/kg) and diazepam (6 mg/kg) and fixed with a stereotaxic frame. The scalp skin was incised, and the periosteum was separated from the cranium. A single dose of reserpine (5 μL, 4 mg/mL, or 20 mg/mL) was stereotaxically injected into the lateral cerebral ventricle of the rat. In control rats, vehicle (dimethyl sulfoxide, 5 μL) was injected into the lateral cerebral ventricle. The coordinates were 0.9 mm posterior to bregma, 1.6 mm lateral from the midline and 3.7 mm below the surface of the skull16, 17, 18, 19, 20.
Vagotomy
The rats were anesthetized intraperitoneally with a combination of ketamine (40 mg/kg) and diazepam (6 mg/kg). A midline abdominal incision was made, and the stomach was exposed. The gastric branches of the vagus nerve were resected at the esophagus, just above the stomach. The area was also covered with 5% phenol to destroy nerves that were overlooked in the surgery21. In control rats, a sham operation was performed with the midline abdominal incision and the exposure of stomach, but the vagus nerve was not resected.
Blood pressure measurement
Systolic blood pressure (SBP), diastolic blood pressure (DBP) and heart rate (HR) were measured in conscious rats by the indirect tail-cuff method. The rats were warmed for 10 min at 37 °C in a thermostatically controlled heating cabinet for better detection of the tail artery pulse. A cuff was placed around the tail, and the ventral surface of the tail was contacted to a pulse transducer, through which the waves of the tail artery were converted into impulses and then visualized through an amplifier as rhythmic waves. SBP, DBP and HR were digitized automatically by the system after the tails were pressurized through the cuff. The final values were obtained by averaging 5 or 6 successful readings22, 23.
Experimental protocols
Experiment 1: GMLs induced by a single dose of reserpine, administered intraperitoneally in SD rats
Sixty rats were randomly divided into 6 groups and fasted for 24 h with free access to water. A single dose of reserpine (0.25, 0.5, 1, 2, 4, or 6 mg/kg) was then injected intraperitoneally, and GMLs were evaluated 18 h later.
Experiment 2: GMLs induced by a single dose of reserpine, administered intragastrically in SD rats
Thirty rats were randomly divided into 3 groups and fasted for 24 h with free access to water. A single dose of reserpine (12, 24, or 48 mg/kg) was administered intragastrically, and GMLs were evaluated 18 h later.
Experiment 3: GMLs induced by reserpine administered intragastrically for 2 weeks in SD rats
Twenty-four rats were randomly divided into 3 groups and fasted for 24 h before the first administration of reserpine. Reserpine was administered intragastrically (1, 3, or 10 mg/kg) daily for 2 weeks. The rats were then killed and GMLs were evaluated.
Experiment 4: Evaluation of the blood pressure-reducing effect and the GML-inducing effect of CHT in SHRs
Blood pressure levels were assessed in 14 SHRs. They were divided into 2 groups on the basis of SBP level and received rat chow containing 0.01 and 0.03 mg/kg of CHT, respectively, for 2 months. At the end of treatment, SBP, DBP, and HR values were determined in conscious rats to examine the effect of CHT on blood pressure. In addition, 14 other SHRs were divided into two groups. These animals received rat chow containing 0.1 and 0.3 mg/kg of CHT, respectively, for 2 months, after which the GML-inducing effect of CHT was evaluated.
Experiment 5: Time course of recovery from GMLs in SD rats
Forty-one rats were fasted for 24 h, and a single dose of reserpine (4 mg/kg) was injected intraperitoneally to induce GMLs. Seven rats were sacrificed 18 h later and evaluated for GMLs. The remaining rats were killed 1, 2, or 3 weeks later and evaluated for GMLs.
Experiment 6: GMLs induced by icv injection of reserpine in SD rats
Twenty rats were divided into 3 groups and fasted for 24 h with free access to water. They were given an icv injection of reserpine (0.08 or 0.4 mg/kg; n=7) or dimethyl sulfoxide (n=6) and sacrificed 18 h later, after which they were evaluated for GMLs.
Experiment 7: Effect of vagotomy on reserpine-induced GMLs in SD rats
Rats were randomly divided into 2 groups and fasted for 24 h. Vagotomy was performed in one group; the other served as a control group. Reserpine (ip, 4 mg/kg) was injected 6 h after vagotomy. Rats were sacrificed 18 h later and evaluated for GMLs.
Statistical analysis
All data were expressed as mean±SEM. A statistical analysis was performed with Student's t-test. P<0.05 was considered statistically significant.
Results
GMLs induced by ip and oral administration of reserpine in SD rats
The GML-inducing effect of reserpine was evaluated for two different drug administration methods. The results indicated that GMLs were induced dose-dependently by a single ip injection of 0.5 mg/kg to 6 mg/kg of reserpine, and no effects were observed in rats given 0.25 mg/kg of reserpine (Figure 1A). The GML-inducing effect of orally administered reserpine was much weaker. A single oral administration of 12 mg/kg of reserpine did not induce GMLs. Reserpine doses of 24 mg/kg and 48 mg/kg induced only slight GMLs (Figure 1B). When reserpine was orally administered at a dose of 10 mg/kg for 2 weeks, GMLs was caused; however, at lower doses (1 mg/kg or 3 mg/kg daily), reserpine did not induce gastric lesions (Figure 1C).
Evaluation of the bloodpressure-reducing and the GML-inducing effects of CHT
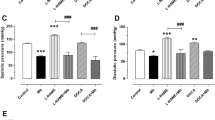
Long-term (2 months) treatment with CHT significantly decreased blood pressure in conscious SHRs. SBP/DBP decreased by 16/11 mmHg in rats treated with CHT 0.01 mg/kg daily and by 21/22 mmHg in rats treated with CHT 0.03 mg/kg daily. In the GML experiment, lesions developed only with a large dose of CHT (0.3 mg/kg daily for 2 months), resulting in a GML index of 4.6±0.8. In rats treated with 0.1 mg/kg of CHT, the stomachs were intact and no GMLs were found (Figure 2, Table 2).
Effect of CHT administered intragastrically for 2 months on SBP, DBP, HR, and GML in SHRs. Open bars, pre-drug administration; solid bars, post-drug administration. Data are expressed as means±SEM. n=7 in each group. SBP, systolic blood pressure; DBP, diastolic blood pressure; HR, heart rate. bP<0.05, cP<0.01 vs pre-drug administration.
Time course of recovery from reserpine-induced GMLs
Severe GMLs were found 18 h after reserpine injection (4 mg/kg ip). Of the seven sacrificed rats, six had large ulcers and petechial points in the stomach. The GML index was 6.4±1.8. One week after reserpine injection, GMLs were noticeably diminished. The GML indexes were 0.44±0.17 on day 8 and 0.29±0.13 on day 15. No ulcers or petechial points were observed in the stomach, but slight mucosal edema and hyperemia were found in some rats at these time points. Three weeks later, the rats had completely recovered from reserpine-induced GMLs. Their stomachs were intact and no injuries were found (Figure 3).
GMLs induced by icv injection of reserpine
Intracerebroventricular injection of vehicle did not induce GMLs in rats, and icv reserpine produced GMLs similar to those found after ip injection, but at much lower doses (Figure 4). The GML index of 0.08 mg/kg of icv reserpine was comparable to that of 2 mg/kg of ip reserpine (2.1±0.14 and 2.6±0.98, respectively). The GML index of 0.4 mg/kg of icv reserpine was 9.1±1.4, slightly higher than that of 4 mg/kg of ip reserpine (8.0±2.4). These results indicate that a central mechanism is involved in the GML-inducing effect of reserpine. Typical lesions resulting from icv reserpine are shown in Figure 4A and 4B.
Effect of vagotomy on reserpine-induced GMLs
Reserpine-induced GMLs were partly inhibited by gastric vagotomy (Figure 5). After the gastric vagus was resected, the reserpine-induced GML index was reduced to 20% of that of the control group. Figure 5A and 5B show the typical lesions observed in control rats and vagotomized rats.
Discussion
The main findings of the present work can be summarized as follows: (1) reserpine-induced GMLs were highly dependent on the dose, route and duration of the drug administration, as well as on the individual's gastric status. The small dose of reserpine in CHT did not induce GMLs during the treatment of hypertension. (2) Reserpine-induced GMLs healed spontaneously within 3 weeks. (3) The effect of reserpine on GMLs was mediated by the central vagal nervous system.
NSAIDs are the primary cause of drug-induced GMLs. Recently, Helicobacter pylori has been proven to play an important role in the pathogenesis of GMLs. At present, reserpine is seldom used alone. However, because many antihypertensive compounds contain reserpine, it is important to understand the nature of reserpine-induced GMLs.
Given the low bioavailability of reserpine, the doses that inducing GMLs with ip and intragastric administration were very different. GMLs were induced with single doses of 0.5 mg/kg of ip reserpine and 24 mg/kg of intragastric reserpine. This represents a 48-fold difference between these two administration routes. In both administration routes, a close dose-effect relationship existed in terms of inducing GMLs. In this study, rats were fasted for 24 h before the reserpine administration, and a single oral dose of reserpine 24 mg/kg produced GMLs. However, in our preliminary experiment, this dose of reserpine did not induce GMLs when the rats were not fasted before drug administration (data not shown). These results confirm the clinical necessity of taking the drug after meals.
CHT, a compound drug containing a small dose of reserpine, has been one of the most widely used antihypertensive drugs in China for more than 30 years. An estimated 900 million CHTs were consumed in each of the past 5 years. In this study, we found that blood pressure significantly decreased with 0.01 mg/kg of CHT. When rats were treated with 0.1 mg/kg of CHT for 2 months, no gastric injury was detected. GMLs occurred in the rats treated with 0.3 mg/kg of CHT for 2 months. Thus, the dose of CHT required to induce GMLs is 30 times higher than is necessary to decrease blood pressure. Generally, the dose of CHT (mainly reserpine) used to treat hypertension is not enough to induce GMLs. However, CHT should be avoided to be used in hypertensive patients with histories of gastric ulcers.
We also found that reserpine-induced gastric injury consisted mostly of mucosal lesions. As many other drug-induced side effects, this gastric injury can heal spontaneously after the drug withdrawal. It was found that this injury decreased significantly 1 week after the drug was administered and completely disappeared within 3 weeks. It should be noted that in this study, a single large dose of reserpine (4 mg/kg) was used to induce GMLs. The resulting injuries may be different from the GMLs induced by long-term treatment. Clinically, if gastric injury occurs during CHT treatment, we should withdraw the drug and give anti-ulcer treatment when necessary. The prognosis of this gastric injury is generally good.
Yamaguchi et al reported that reserpine increased acid secretion in rats13, which was a possible mechanism leading to mucosal lesions. However, the exact mechanism is not yet clear. Reserpine was believed to exhaust the monoamines at the ends of sympathetic nerves, leading to overactivity of the vagal nervous system at the peripheral level. This may lead to an oversecretion of gastric acid. On the other hand, reserpine may exhaust the monoamines in the central nervous system, resulting in inhibition of sympathetic nerve outflow and the activation of the vagus. In this study, we found that gastric mucosal injury was partially inhibited by vagotomy. This result was consistent with Kim's report that reserpine-induced gastric acid secretion was greatly reduced, but not completely blocked, by vagotomy14. In addition, we found that icv reserpine 0.08 mg/kg produced gastric lesions in SD rats. This dose was much lower than the ip dose (0.25 mg/kg) that did not induce GMLs. We can deduce from these results that reserpine centrally inhibits the sympathetic nervous system, leading to an activation of vagal nerves and other factors that regulate gastric-acid secretion and inducing GMLs.
Author contribution
Ding-feng SU designed the research; Xiu-juan MA, Xiang ZHENG, Zhi-peng WEN, Shu-wei SONG, Wei LIU, and Qian-zhou LÜ performed the research; and Xiu-juan MA and Guo-cai LU wrote the paper.
References
Jia Q, Liu LP, Wang YJ . Stroke in China. Clin Exp Pharmacol Physiol 2010; 37: 259–64.
Luepker RV, Arnett DK, Jacobs DR Jr, Duval SJ, Folsom AR, Armstrong C, et al. Trends in blood pressure, hypertension control, and stroke mortality: the Minnesota Heart Survey. Am J Med 2006; 119: 42–9.
Bansal D, Chahoud G, Smith ES, Mehta JL . Prevention of heart failure. Curr Opin Cardiol 2006; 21: 510–6.
Tocci G, Sciarretta S, Volpe M . Development of heart failure in recent hypertension trials. J Hypertens 2008; 26: 1477–86.
Zoungas S, Asmar RP . Arterial stiffness and cardiovascular outcome. Clin Exp Pharmacol Physiol 2007; 34: 647–51.
Neal B, MacMahon S, Chapman N . Effects of ACE inhibitors, calcium antagonists, and other blood-pressure-lowering drugs: results of prospectively designed overviews of randomized trials. Lancet 2000; 356: 1955–64.
Sheldon MB, Kotte JH . Effect of rauwolfia serpentina and reserpine on the blood pressure in essential hypertension: a long-term double-blind study. Circulation 1957; 16: 200–6.
Finnerty FA Jr, Kakaviatos N, Chupkovich V . Value of chlorthalidone plus reserpine in moderately severe and severe hypertension: a two-year study. Circulation 1965; 32: 13–8.
Dillon D, Swain JM . Gastro-intestinal hemorrhage as a complication of reserpine administration: report of two cases. Am J Psychiatry 1956; 113: 462–3.
Locket S . Oral preparations of Reuwolfia serpentina in treatment of essential hypertension. Br Med J 1955; 1: 809–16.
Bulpitt CJ, Dollery CT . Side effects of hypotensive agents evaluated by a self administered questionnaire. Br Med J 1973; 3: 485–90.
Sandor V, Cuparencu B . Analysis of the mechanism of the protective activity of some sympathomimetic amines in experimental ulcers. Pharmacology 1977; 15: 208–17.
Yamaguchi Y, Hirio J, Puke H, Kumada S . Mechanism of gastric secretagogue effect of reserpine in rats. J Pharmacol Exp Ther 1978; 205: 710–7.
Kim KS, Shore PA . Mechanism of action of reserpine and insulin on gastric amines and gastric acid secretion, and the effect of monoamine oxidase inhibition. J Pharmacol Exp Ther 1963; 141: 321–5.
Gamberini MT, Skorupa LA, Souccar C, Lapa AJ . Inhibition of gastric secretion by a water extract from Baccharis triptera, Mart. Mem Inst Oswaldo Cruz 1991; 86 Suppl 2: 137–9.
Ma XJ, Shen FM, Liu AJ, Shi KY, Wu YL, Su DF . Clonidine, moxonidine, folic acid, and mecobalamin improve baroreflex function in stroke-prone, spontaneously hypertensive rats. Acta Pharmacol Sin 2007; 28: 1550–8.
Zheng RM, Zou CJ, Zhu SG . p38 MAPK mediates cardiovascular and behavioral responses induced by central IL-1 beta and footshock in conscious rats. Acta Pharmacol Sin 2004; 25: 266–70.
Li HL, Kang YM, Yu L, Xu HY, Zhao H . Melatonin reduces blood pressure in rats with stress-induced hypertension via GABAA receptors. Clin Exp Pharmacol Physiol 2009; 36: 436–40.
Yalcin M, Aydin C . Cardiovascular effects of centrally administered arachidonic acid in haemorrhage-induced hypotensive rats: investigation of a peripheral mechanism. Clin Exp Pharmacol Physiol 2009; 36: 447–53.
Wang JL, Wang L, Wu ZT, Yuan WJ, Su DF, Ni X, et al. Low dose of moxonidine within the rostral ventrolateral medulla improves the baroreflex sensitivity control of sympathetic activity in hypertensive rat. Acta Pharmacol Sin 2009; 30: 1594–600.
Onoma M, Yogo K, Ozaki K, Kamei K, Akima M, Koga H, et al. Oral mitemcinal (GM-611), an erythromycin-derived prokinetic, accelerates normal and experimentally delayed gastric emptying in conscious dogs. Clin Exp Pharmacol Physiol 2008; 35: 35–42.
Wang XQ, Zhang HG, Cheng YQ, Li XH . Inhibition of left ventricular remodelling in spontaneously hypertensive rats by G alpha q-protein carboxyl terminus imitation polypeptide GCIP-27 is not entirely dependent on blood pressure. Clin Exp Pharmacol Physiol 2008; 35: 1215–21.
Krug S, Zhang Y, Mori TA, Croft KD, Vickers JJ, Langton LK, et al. N-Acetylcysteine prevents but does not reverse dexamethasone-induced hypertension. Clin Exp Pharmacol Physiol 2008; 35: 979–81.
Acknowledgements
This study was supported by grants from the National Science and Technology Major Project (No 2009ZX09303-002), the China Postdoctoral Science Foundation Funded Project (No 20080441303) and the Shanghai Postdoctoral Sustentation Fund (No 08R214101).
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Ma, Xj., Lu, Gc., Song, Sw. et al. The features of reserpine-induced gastric mucosal lesions. Acta Pharmacol Sin 31, 938–943 (2010). https://doi.org/10.1038/aps.2010.74
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2010.74
Keywords
This article is cited by
-
Impact of depositional environment and diagenesis on the Upper Triassic Xujiahe tight-sand reservoir in Guang’an area, Central Sichuan Basin, SW China
Carbonates and Evaporites (2019)
-
Characteristics of the tight sand reservoirs in the delta front in the Xu-2 Member of the Upper Triassic Xujiahe Formation (Hechuan area of the central Sichuan Basin, SW China)
Arabian Journal of Geosciences (2018)