Abstract
Aim:
To examine the involvement of K+ channels and endothelium in the vascular effects of magnesium lithospermate B (MLB), a hydrophilic active component of Salviae miltiorrhiza Radix.
Methods:
Isolated rat mesenteric artery rings were employed to investigate the effects of MLB on KCl- or norepinephrine-induced contractions. Conventional whole-cell patch-clamp technique was used to study the effects of MLB on K+ currents in single isolated mesenteric artery myocytes.
Results:
MLB produced a concentration-dependent relaxation in mesenteric artery rings precontracted by norepinephrine (1 μmol/L) with an EC50 of 111.3 μmol/L. MLB-induced relaxation was reduced in denuded artery rings with an EC50 of 224.4 μmol/L. MLB caused contractions in KCl-precontracted artery rings in the presence of N-nitro-L-arginine methyl ester (L-NAME) with a maximal value of 130.3%. The vasodilatory effect of MLB was inhibited by tetraethylammonium (TEA) in both intact and denuded artery rings. In single smooth muscle cells, MLB activated BKCa currents (EC50 156.3 μmol/L) but inhibited KV currents (IC50 26.1 μmol/L) in a voltage- and concentration-dependent manner.
Conclusion:
MLB dilated arteries by activating BKCa channels in smooth muscle cells and increasing NO release from endothelium, but it also contracted arteries precontracted with KCl in the presence of L-NAME.
Similar content being viewed by others
Introduction
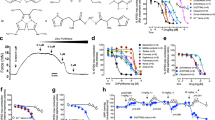
Salviae miltiorrhiza Radix (Danshen) is a traditional Chinese herbal medicine used mainly to treat cardiovascular diseases. In recent decades, attention has focused on its water-soluble ingredients, the main efficacious components in decoctions of Danshen1. Among these, magnesium lithospermate B (MLB, Mw: 741) is the most abundant active component2 (Figure 1).
MLB exhibits free radical–scavenging3, 4, 5, hypotensive6, renal function-improving7, and angiotensin-converting enzyme-inhibiting8 activities. Previous findings on the pharmacologic mechanisms of MLB are inconsistent. It was reported that MLB induced endothelium-dependent vasodilatation in vitro9 and decreased blood pressure in rats in vivo6. However, others reported that the vasodilator effect of Danshen crude extract was not affected by L-NAME or mechanical removal of the endothelium in rat isolated femoral artery rings10. In guinea pig single ventricular myocytes, MLB was reported to inhibit voltage-dependent L-type Ca2+ channels, with no significant effects on other ion channels11, whereas another study showed that MLB activated iberiotoxin-sensitive BKCa channels in porcine coronary artery smooth muscle cells12.
In the present study, we investigated the effects of MLB on vascular functions in vitro and the involvement of K+ channels and endothelium in the vascular response to MLB.
Materials and methods
Reagents and solutions
Magnesium lithospermate B (MLB, brown powder with 99.7% purity) was obtained from the Research Center of Traditional Chinese Medicine Modernization, Shanghai Institute of Materia Medica. Norepinephrine, ACh, L-NAME, papain, dithiothreitol, bovine serum albumin (BSA), EGTA, taurine, sodium deoxycholate, 4-aminopyridine (4-AP), iberiotoxin, and tetraethylammonium chloride were from Sigma-Aldrich China Inc. MLB was dissolved in the appropriate external solutions to produce the desired concentrations just before experiments. Krebs solution for perfusion of artery rings contained the following (in mmol/L): 118 NaCl, 4.7 KCl, 2.5 CaCl2, 1.2 MgSO4, 1.18 KH2PO4, 25 NaHCO3, 10 glucose. The composition of the dissociation medium for enzymatic cell isolation and the external solution for patch-clamp studies was as follows (in mmol/L): 130 NaCl, 4.2 KCl, 0.5 MgCl2, 10 NaHCO3, 1.8 (or 0.16) CaCl2, 1.2 KH2PO4, 10 HEPES, and 5.5 glucose (pH 7.4 with NaOH), with an osmolality of 298±2 mOsm/L. The pipette solution contained the following (in mmol/L): 100 K gluconate, 30 KCl, 5 NaCl, 1 MgCl2, 1 CaCl2, 3 (or 0.3 for BKCa) EGTA, 10 HEPES, 10 glucose (pH 7.2, titrated with KOH), with an osmolality of 303±2 mOsm/L.
Rats
Male Sprague-Dawley rats, weighing 250–300 g, were purchased from Shanghai Experimental Animal Center (SPF, Certificate No SCXK 2007-0005, conferred by Animal Management Committee, Chinese Academy of Sciences).
Isolation of rat mesenteric artery and tone recording
Male Sprague-Dawley rats were killed by injecting a lethal dose (80 mg/kg) of sodium pentobarbitone. The superior mesenteric arteries were carefully removed and placed in Krebs solution. Adherent adipose and connective tissue were then removed. Vessel rings of about 1.5 mm in length were cut from each artery and mounted in 20-mL bath chambers of an integrated myograph system (AD instrument PowerLab 4/20) for tone recording. Bath chambers were filled with Krebs solution at 37 °C and aerated with 95% O2+5% CO2 to maintain a pH of 7.4. Tone signals were relayed to a PowerLab 4 amplifier and saved in a computer (sampling rate, 100 Hz). To remove vascular endothelium, artery rings were perfused with 1.80 mg/mL sodium deoxycholate in saline for 30 s. Artery rings were then rinsed with sodium deoxycholate–free Krebs solution for 40 min. Chemical removal of the endothelium was assessed by the lack of a relaxant response to 1 nmol/L acetylcholine.
During the initial 1-h equilibration, artery rings were stretched until the resting tension remained steady at 1.5 g. Artery rings were evaluated for a reproducible contractile response to 1 μmol/L norepinephrine and were washed several times. Next, 30 mmol/L KCl or 1 μmol/L norepinephrine was applied to establish a stable contractile tone. Subsequently, cumulative concentration–response curves of MLB were constructed by cumulative application of MLB to artery rings at 8-min intervals. In the experiment investigating the involvement of nitric oxide (NO) in artery dilation, artery rings were incubated with L-NAME (100 μmol/L), an inhibitor of nitric oxide synthase (NOS), for 30 min before applying KCl. In the experiment investigating the involvement of potassium channels, tetraethylammonium (TEA, 1 mmol/L) was used to incubate the artery rings for 10 min before applying norepinephrine.
Isolation of vascular smooth muscle cells
Single mesenteric artery cells were isolated using an enzymatic dissociation method as described previously, with slight modifications13. The mesenteric artery was dissected and placed in dissociation medium containing a low concentration of Ca2+ (160 μmol/L). Connective tissue was carefully removed. Next, the cleaned vessel was cut along its longitudinal axis and cut into small strips. Muscle strips were allowed to stay in fresh dissociation medium for 6–10 min at room temperature, and then they were transferred into enzyme solution in a tightly capped glass bottle and stored overnight at 4 °C. The enzyme solution contained 1% papain (type IV, 14.5 units/mg protein) and 0.02% BSA (type V, essentially fatty acid–free) in 5 mL dissociation medium. The following morning, dithiothreitol (DDT, 0.1 mmol/L) was added to the bottle, and the strips were incubated at 37 °C for 2–4 min in a shaking water bath. Strips were subsequently transferred to fresh dissociation medium and gently triturated with a wide-bore (2–3 mm) pipette. Long and relaxed single cells were obtained and then stored in dissociation medium at 4 °C. Approximately 70% of the cells remained relaxed for several hours after Ca2+ recovered to physiological levels.
Electrophysiological recording
Whole-cell K+ currents were measured with the conventional patch-clamp technique14. A small aliquot of vascular smooth muscle cells was placed in a 3-mL chamber mounted on the stage of a microscope (Optiphot-2; Nikon, Japan) and superfused with external solution via a PBS-8 solution exchange system (ALA Scientific Instruments Inc, USA) at 3 mL/min. Patch pipettes were pulled using a P-97 microelectrode puller (Shutter Instruments Co, USA) with a tip resistance of 1–5 MΩ. The pipette tip was positioned near the center of mesenteric smooth muscle cells using an oil-based hydraulic micromanipulator (Narishige Scientific Instruments, Japan). After gigaseal formation (seal resistance >1 GΩ), the membrane was ruptured with gentle suction to obtain whole-cell voltage-clamp configuration. Voltage command protocols were provided by the pClamp 6.0.4 software package (Axon Instruments, USA) via a DigiData-1200 interface. Capacitance compensation was routinely optimized, and series resistance was compensated by 40%–80%. Linear leaks were subtracted digitally online. Currents were filtered at 1 kHz and sampled at 3 kHz. Cell capacitance was measured using a short hyperpolarizing ramp pulse (5 mV for 5 ms) from a holding potential of -60 mV. The membrane capacitance of smooth muscle cells ranged from 8 to 20 pF. Currents during the last 400 ms in each step of two or three voltage-clamp trials were sampled and averaged before analysis. Currents were normalized to cell capacitance to obtain the current densities. Allowing for equilibration of the pipette solution with the cell interior, all recordings were initiated 5 min after establishing the whole-cell configuration. Most experiments were performed within 40 min after attaining the whole-cell configuration. During this time, the macroscopic K+ current amplitude of the control cells remained stable. To separate BKCa and KV from total currents, IK was recorded from different holding potentials (−20 to +80 mV for BKCa and -60 to +40 mV for KV).
Statistical analysis
Artery responses were measured as a reduction or increment in grams upon the norepinephrine- (or KCl-) preconstricted tones and are expressed as means±SD. Patch-clamp data are presented as means±SEM. Data analyses were performed using Clampfit 9.0 (Axon Instruments, USA). The concentration of MLB yielding a 50% effect (EC50 or IC50) was obtained by fitting the concentration–response relationship to the equation X=1/{1+[(C)/IC50]n}, where X is the normalized response, (C) is the concentration of MLB and n is the Hill coefficient. Differences were compared using the Student's t-test or one-way ANOVA, followed by Bonferroni post-hoc test, as appropriate. All tests were two-tailed, and a value of P<0.05 was considered as statistically significant.
Results
MLB enhances KCl-induced vasoconstriction in the presence of L-NAME
The addition of MLB (400 μmol/L) to the bath solution produced a relaxation response in the artery rings precontracted by 30 μmol/L KCl (Figure 2A). However, in the presence of L-NAME (100 μmol/L), MLB produced a substantial contraction in a concentration-dependent manner, with a maximal contraction amplitude of 130.3% (Figure 2A). When L-NAME was applied to artery rings before KCl, tones increased slightly and were readjusted to baseline.
MLB causes relaxation or constriction of isolated artery rings. (A) Artery rings were precontracted by KCl. ○ Saline water was applied to intact artery rings as a control; • MLB was applied to intact artery rings; ▪ MLB was applied to artery rings pretreated with L-NAME. (B) Artery rings were precontracted by norepinephrine. ○ Saline water was applied to intact artery rings as a control; • MLB was applied to intact artery rings; □ MLB was applied to denuded artery rings; ▴ MLB was applied to intact artery rings pretreated with TEA; △ MLB was applied to denuded artery rings pretreated with TEA. The maximal contraction induced by KCl or norepinephrine before applying saline water or MLB was taken as 100. Cumulative concentration of MLB: 12.5, 25, 50, 100, 200, or 400 μmol/L. bP<0.05, cP<0.01 vs control (○); eP<0.05, fP<0.01 vs MLB (•) (n=10).
MLB relaxes norepinephrine-induced vasoconstriction
Tones produced by 1 μmol/L norepinephrine (1.97±0.55 g) were sustained over the course of the experiment. Cumulative application of MLB induced concentration-dependent relaxation, with an EC50 of 111.3 μmol/L (95% confidence interval: 97.6–126.3 μmol/L). Meanwhile, in denuded artery rings the vasodilator response was reduced (EC50 224.4 μmol/L, 95% CI: 198.1–248.0 μmol/L) (Figure 2B). TEA was used to examine whether K+ channels are involved in the MLB-induced vasodilation. Application of TEA induced a slight increase in tones, which was adjusted to baseline. In the presence of TEA, the vasodilation induced by MLB was largely inhibited in either intact or denuded artery rings: 400 μmol/L MLB dilated intact mesenteric arteries by 92.3% in the absence of TEA but only by 25.8% in the presence of 1 mmol/L TEA (Figure 2B).
MLB activates large-conductance Ca2+-activated K+ (BKCa) currents
In single smooth muscle cells from rat mesenteric arteries, 500-ms voltage steps from a holding potential of -20 mV to test potentials in the range of -10 to +80 mV were adopted to activate BKCa currents. As the availability of KV channels is voltage-dependent, IK measured from a holding potential of -20 mV was primarily determined by BKCa channels, where the contribution of KV channels to whole-cell IK was negligible. A family of voltage-dependent, high-amplitude, high-noise outward K+ currents were elicited, which were inhibited by 1 mmol/L TEA (n=5) and 1 nmol/L iberiotoxin (n=5) (Figure 3D). MLB produced a gradual voltage-dependent increment of currents, which reached a plateau within approximately 3 min. The densities of currents recorded at +80 mV were 9.57±3.6 pA/pF, which increased to 15.95±4.09 pA/pF after exposure to 100 μmol/L MLB (n=8, P<0.01). This MLB-induced increment of currents was partially recovered upon washout (Figure 3C). The outward currents were sustained during the depolarization pulse. The I–V relationship was plotted (Figure 4A). BKCa currents at +70 and +80 mV were significantly larger in the presence of MLB than in controls. A single depolarization pulse from -20 to +70 mV was adopted to obtain the concentration-response curve, and the results showed that the stimulatory effect of MLB on BKCa was concentration-dependent, with an EC50 of 156.3 μmol/L (95% CI: 136.9–175.3 μmol/L).
MLB activates BKCa currents in a concentration- and voltage-dependent manner. (A) Current–voltage (I–V) curves before and after applying 100 μmol/L MLB. (B) Concentration–response curve of BKCa currents to MLB. Cumulative concentration of MLB: 25, 50, 100, 200, or 400 μmol/L (n=8). (C) Representative BKCa currents before and after applying MLB. bP<0.05, cP<0.01 vs control (○).
MLB inhibits KV currents
A family of voltage-dependent outward K+ currents was elicited by depolarization from a holding potential of -60 mV to a series of command potentials from -50 to +40 mV. The representative currents in response to MLB (100 μmol/L) are illustrated (Figure 5A). Application of 3 mmol/L 4-AP suppressed the currents almost completely, which is characteristic of KV currents15, 16. The IK was sampled between 450 and 490 ms (steady state) to exclude any possibility of A-current contribution to the measured amplitude. The I–V curve shows that MLB inhibited KV significantly (Figure 5B).
The time-course of response to MLB showed that inhibition of KV currents was reversible (Figure 6B). The depolarizing pulse of 500 ms from a holding potential of -60 mV to a test potential of +30 mV was used to obtain the concentration–response relationship (Figure 6C). The IC50 was 26.1 μmol/L (95% CI: 20.4–34.8 μmol/L) (n=8).
MLB inhibits KV currents in a reversible and concentration-dependent manner. (A) Representative KV currents before and after applying MLB (100 μmol/L). (B) Time-course of the response to application and washout of MLB (100 μmol/L). (C) Concentration–response curve of KV currents to MLB (25, 50, 100, 200, or 400 μmol/L) (n=8). bP<0.05, cP<0.01 vs control (○).
Discussion
Force and membrane potential are closely coupled in arterial smooth muscle, and K+ conductance plays a major role in determining membrane potential15. Low concentrations (≤1 mmol/L) of TEA selectively block BKCa17. In the present study, the relaxant responses of both the denuded and the intact artery rings to MLB were inhibited almost completely by pre-incubation with TEA (1 mmol/L), suggesting the involvement of K+ channels. We also found MLB activated BKCa currents in a reversible, concentration- and voltage-dependent manner in whole-cell patch-clamp experiments. The results from artery rings and patch-clamp experiments were consistent, indicating BKCa currents are involved in the vasodilator process and activation of BKCa is the primary vasodilator mechanism in rat mesenteric arteries.
The vasoconstriction in response to MLB in artery rings precontracted with KCl is a novel finding of this study. BKCa currents are much smaller than KV currents within the physiological membrane potential range, and activation of KV channels is the initial inhibitory mechanism upon depolarization in arteriolar smooth muscle cells18. The vasocontraction induced by KCl is due to depolarization of smooth muscle cells. Our patch-clamp experiments showed that MLB inhibited KV currents. Inhibition of K+ currents would cause depolarization and vasoconstriction16, 19. Therefore, it is reasonable to presume that in artery rings precontracted with KCl, MLB caused further vasocontraction by inhibiting KV currents. Without precontraction with KCl, artery rings were not contracted by MLB (data not shown), implying the vasoconstriction to MLB might be situation-dependent.
Although KV channels are dominant in the artery, the inhibitory effects of Ca2+ on KV channels lead to a shift of dominance to BKCa channels once the intracellular Ca2+ levels rise substantially20, 21. This could be the reason that MLB relaxed artery rings precontracted with norepinephrine but contracted artery rings precontracted with KCl.
In cardiovascular disease, K+ channels functionally change22, 23, 24. Hypertension develops, with functional down-regulation of KV channels but up-regulation of BKCa in smooth muscle25. Activating BKCa but inhibiting KV channels might have important pharmacologic and therapeutic implications.
Previous findings indicate MLB causes endothelium-dependent vasodilatation in vitro9. Meanwhile, another study demonstrated that its vasodilatory action is not endothelium-dependent but primarily by works by inhibiting Ca2+ inflow26. In this study, the involvement of endothelium was investigated using both denuded artery rings and L-NAME. In denuded artery rings precontracted with norepinephrine, the vasodilatory effect of MLB was reduced significantly compared with intact artery rings. In artery rings incubated with L-NAME, an inhibitor of NOS, and precontracted by KCl, MLB induced vasoconstriction. Conversely, without L-NAME, application of MLB dilated artery rings. These results demonstrate that endothelium and endothelial NO participate in the vasodilation process of MLB. By contrast, compared with the effect of TEA, the removal of endothelium caused a relatively minor effect. NO stimulates smooth muscle soluble guanylate to produce cGMP, which consequently activates BKCa and induces vasodilatation7, 27. Furthermore, NO can activate BKCa directly27. So far, however, it is still unknown how NO participates in the vasodilatory action of MLB.
In conclusion, our data provide evidence that MLB, a hydrophilic constituent of S miltiorrhiza, dilates artery rings primarily by activating iberiotoxin-sensitive BKCa channels in smooth muscle cells and increasing NO release from endothelium. MLB also contracts arteries precontracted with KCl in the presence of L-NAME.
Author contribution
Yi-ping WANG designed the research; Guo-yuan HU and Xue-qing CHEN provided equipment and technical support; Hai-fei ZHANG performed the research and analyzed the data; Yi-ping WANG and Hai-fei ZHANG wrote the paper.
References
Lu Y, Foo LY . Polyphenolics of Salvia — a review. Phytochemistry 2002; 59: 117–40.
Kasimu R, Tanaka K, Tezuka Y, Gong ZN, Li JX, Basnet P, et al. Comparative study of seventeen Salvia plants: aldose reductase inhibitory activity of water and MeOH extracts and liquid chromatography-mass spectrometry (LC-MS) analysis of water extracts. Chem Pharm Bull (Tokyo) 1998; 46: 500–4.
Chen CP, Yokozawa T, Chung HY . Inhibitory effect of caffeic acid analogues isolated from Salviae Miltiorrhizae Radix against 1,1-diphenyl-2-picrylhydrazyl radical. Exp Toxicol Pathol 1999; 51: 59–63.
Yokozawa T, Chung HY, Dong E, Oura H . Confirmation that magnesium lithospermate B has a hydroxyl radical-scavenging action. Exp Toxicol Pathol 1995; 47: 341–4.
Wu XJ, Wang YP, Wang W, Sun WK, Xu YM, Xuan LJ . Free radical scavenging and inhibition of lipid peroxidation by magnesium lithospermate B. Acta Pharmacol Sin 2000; 21: 855–8.
Kamata K, Noguchi M, Nagai M . Hypotensive effects of lithospermic acid B isolated from the extract of Salviae miltiorrhizae Radix in the rat. Gen Pharmacol 1994; 25: 69–73.
Yokozawa T, Zhou JJ, Hattori M, Inaba S, Okada T, Oura H, et al. Effects of a Dan Shen component, magnesium lithospermate B, in nephrectomized rats. Nippon Jinzo Gakkai Shi 1995; 37: 105–11.
Soung DY, Rhee SH, Kim JS, Lee JY, Yang HS, Choi JS, et al. Peroxynitrite scavenging activity of lithospermate B from Salvia miltiorrhiza. J Pharm Pharmacol 2003; 55: 1427–32.
Kamata K, Iizuka T, Nagai M, Kasuya Y . Endothelium-dependent vasodilator effects of the extract from Salviae Miltiorrhizae radix. A study on the identification of lithospermic acid B in the extracts. Gen Pharmacol 1993; 24: 977–81.
Lam FF, Yeung JH, Cheung JH . Mechanisms of the dilator action of Danshen (Salvia miltiorrhiza) on rat isolated femoral artery. J Cardiovasc Pharmacol 2005; 46: 361–8.
Wang W, Hu GY, Wang YP . Selective modulation of L-type calcium current by magnesium lithospermate B in guinea-pig ventricular myocytes. Life Sci 2006; 78: 2989–97.
Lam FF, Seto SW, Kwan YW, Yeung JH, Chan P . Activation of the iberiotoxin-sensitive BKCa channels by salvianolic acid B of the porcine coronary artery smooth muscle cells. Eur J Pharmacol 2006; 546: 28–35.
Clapp LH, Gurney AM . Outward currents in rabbit pulmonary artery cells dissociated with a new technique. Exp Physiol 1991; 76: 677–93.
Hamill OP, Marty A, Neher E, Sakmann B, Sigworth FJ . Improved patch-clamp techniques for high-resolution current recording from cells and cell-free membrane patches. Pflugers Arch 1981; 391: 85–100.
Jackson WF . Ion channels and vascular tone. Hypertension 2000; 35: 173–8.
Nelson MT, Quayle JM . Physiological roles and properties of potassium channels in arterial smooth muscle. Am J Physiol 1995; 268: C799–822.
Brayden JE . Potassium channels in vascular smooth muscle. Clin Exp Pharmacol Physiol 1996; 23: 1069–76.
Cheong A, Quinn K, Dedman AM, Beech DJ . Activation thresholds of K(V), BK and Cl(Ca) channels in smooth muscle cells in pial precapillary arterioles. J Vasc Res 2002; 39: 122–30.
Nelson MT, Patlak JB, Worley JF, Standen NB . Calcium channels, potassium channels, and voltage dependence of arterial smooth muscle tone. Am J Physiol 1990; 259: C3–18.
Cox RH, Petrou S . Ca2+ influx inhibits voltage-dependent and augments Ca2+-dependent K+ currents in arterial myocytes. Am J Physiol 1999; 277: C51–63.
Gelband CH, Hume JR . [Ca2+]i inhibition of K+ channels in canine renal artery. Novel mechanism for agonist-induced membrane depolarization. Circ Res 1995; 77: 121–30.
Jackson WF . Potassium channels and regulation of the microcirculation. Microcirculation 1998; 5: 85–90.
Loeb AL, Godeny I, Longnecker DE . Functional evidence for inward-rectifier potassium channels in rat cremaster muscle arterioles. Microvasc Res 2000; 59: 1–6.
Paterno R, Faraci FM, Heistad DD . Role of Ca2+-dependent K+ channels in cerebral vasodilatation induced by increases in cyclic GMP and cyclic AMP in the rat. Stroke 1996; 27: 1603–7; discussion 1607–8.
Martens JR, Gelband CH . Alterations in rat interlobar artery membrane potential and K+ channels in genetic and nongenetic hypertension. Circ Res 1996; 79: 295–301.
Lam FF, Yeung JH, Kwan YW, Chan KM, Or PM . Salvianolic acid B, an aqueous component of danshen (Salvia miltiorrhiza), relaxes rat coronary artery by inhibition of calcium channels. Eur J Pharmacol 2006; 553: 240–5.
Feletou M, Vanhoutte PM . Endothelium-dependent hyperpolarization of vascular smooth muscle cells. Acta Pharmacol Sin 2000; 21: 1–18.
Acknowledgements
We would like to thank Prof Li-jiang XUAN of the Department of Phytochemistry, Shanghai Institute of Materia Medica for providing the sample of MLB.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, Hf., Chen, Xq., Hu, Gy. et al. Magnesium lithospermate B dilates mesenteric arteries by activating BKCa currents and contracts arteries by inhibiting KV currents. Acta Pharmacol Sin 31, 665–670 (2010). https://doi.org/10.1038/aps.2010.40
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2010.40
Keywords
This article is cited by
-
Magnesium lithospermate B ameliorates microcirculation perfusion in rats by promoting vascular NO production via activating the PI3K/AKT pathway
Acta Pharmacologica Sinica (2019)
-
Magnesium lithospermate B protects the endothelium from inflammation-induced dysfunction through activation of Nrf2 pathway
Acta Pharmacologica Sinica (2019)
-
Pharmacological actions and therapeutic applications of Salvia miltiorrhiza depside salt and its active components
Acta Pharmacologica Sinica (2012)