Abstract
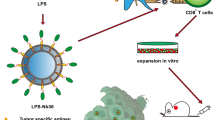
T-cell suppression derived from tumor-secreted immunosuppressive interleukin (IL)-10 becomes a major barrier to CD8+ T-cell immunotherapy of tumors. Tumor necrosis factor-alpha (TNF-α) is a multifunctional cytokine capable of activating T and dendritic cells (DCs) and counteracting IL-10-mediated DC inhibition and regulatory T-cell-mediated immune suppression. In this study, we constructed a recombinant adenovirus MFAdVTNF with fiber-gene modified by RGD insertion into the viral knob's H1 loop and a melanoma cell line B16OVA/IL−10 engineered to express ovalbumin (OVA) and to secrete IL-10 (2.2 ng/ml/106 cells/24 h). We transfected OVA-specific CD8+ T cells with MFAdVTNF, and found a fivefold increase in transgene human TNF-α secretion (4.3 ng/ml/106 cells/24 h) by the engineered CD8+ TTNF cells transfected with MFAdVTNF, compared to that (0.8 ng/ml/106 cells/24 h) by CD8+ T cells transfected with the original AdVTNF without viral fiber modification. The engineered CD8+ TTNF cells exhibited enhanced cytotoxicity and elongated survival in vivo after adoptive transfer. TNF-α derived from both the donor CD8+ T cells and the host cells plays an important role in donor CD8+ T-cell survival in vivo after adoptive transfer. We also demonstrated that the transfected B16OVA/IL−10 tumor cells secreting IL-10 are more resistant to in vivo CD8+ T-cell therapy than the original B16OVA tumor cells without IL-10 expression. Interestingly, the engineered CD8+ TTNF cells secreting transgene-coded TNF-α, but not the control CD8+ Tcontrol cells without any transgene expression eradicated IL-10-secreting 12-day lung micrometastasis in all 10/10 mice and IL-10-secreting solid tumors (∼5 mm in diameter) in 6/10 mice. Transfer of the engineered CD8+ TTNF cells further induced both donor- and host-derived memory CD8+ T cells, leading to a stronger long-term antitumor immunity against the IL-10-secreting B16OVA/IL−10 tumor cell challenges. Therefore, CD8+ T cells engineered to secrete TNF-α may be useful when designing strategies for adoptive T-cell therapy of solid tumors.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Plautz GE, Touhalisky JE, Shu S . Treatment of murine gliomas by adoptive transfer of ex vivo activated tumor-draining lymph node cells. Cell Immunol 1997; 178: 101–107.
Peng L, Shu S, Krauss JC . Treatment of subcutaneous tumor with adoptively transferred T cells. Cell Immunol 1997; 178: 24–32.
Tanaka H, Yoshizawa H, Yamaguchi Y, Ito K, Kagamu H, Suzuki E et al. Successful adoptive immunotherapy of murine poorly immunogenic tumor with specific effector cells generated from gene-modified tumor-primed lymph node cells. J Immunol 1999; 162: 3574–3582.
Eck SC, Turka LA . Adoptive transfer enables tumor rejection targeted against a self-antigen without the induction of autoimmunity. Cancer Res 2001; 61: 3077–3083.
Dobrzanski MJ, Reome JB, Dutton RW . Type 1 and type 2 CD8+ effector T cell subpopulations promote long-term tumor immunity and protection to progressively growing tumor. J Immunol 2000; 164: 916–925.
Becker C, Pohla H, Frankenberger B, Schuler T, Assenmacher M, Schendel DJ et al. Adoptive tumor therapy with T lymphocytes enriched through an IFN-gamma capture assay. Nat Med 2001; 7: 1159–1162.
Gastl GA, Abrams JS, Nanus DM, Oosterkamp R, Silver J, Liu F et al. Interleukin-10 production by human carcinoma cell lines and its relationship to interleukin-6 expression. Int J Cancer 1993; 55: 96–101.
Smith DR, Kunkel SL, Burdick MD, Wilke CA, Orringer MB, Whyte RI et al. Production of interleukin-10 by human bronchogenic carcinoma. Am J Pathol 1994; 145: 18–25.
Taga K, Mostowski H, Tosato G . Human interleukin-10 can directly inhibit T-cell growth. Blood 1993; 81: 2964–2971.
Steinbrink K, Graulich E, Kubsch S, Knop J, Enk AH . CD4(+) and CD8(+) anergic T cells induced by interleukin-10-treated human dendritic cells display antigen-specific suppressor activity. Blood 2002; 99: 2468–2476.
Groux H, Bigler M, de Vries JE, Roncarolo MG . Interleukin-10 induces a long-term antigen-specific anergic state in human CD4+ T cells. J Exp Med 1996; 184: 19–29.
Hsieh CL, Chen DS, Hwang LH . Tumor-induced immunosuppression: a barrier to immunotherapy of large tumors by cytokine-secreting tumor vaccine. Hum Gene Ther 2000; 11: 681–692.
Hara M, Kingsley CI, Niimi M, Read S, Turvey SE, Bushell AR et al. IL-10 is required for regulatory T cells to mediate tolerance to alloantigens in vivo. J Immunol 2001; 166: 3789–3796.
Yang AS, Lattime EC . Tumor-induced interleukin 10 suppresses the ability of splenic dendritic cells to stimulate CD4 and CD8 T-cell responses. Cancer Res 2003; 63: 2150–2157.
Kawamura K, Bahar R, Natsume W, Sakiyama S, Tagawa M . Secretion of interleukin-10 from murine colon carcinoma cells suppresses systemic antitumor immunity and impairs protective immunity induced against the tumors. Cancer Gene Ther 2002; 9: 109–115.
Garcia-Hernandez ML, Hernandez-Pando R, Gariglio P, Berumen J . Interleukin-10 promotes B16-melanoma growth by inhibition of macrophage functions and induction of tumour and vascular cell proliferation. Immunology 2002; 105: 231–243.
Chau GY, Wu CW, Lui WY, Chang TJ, Kao HL, Wu LH et al. Serum interleukin-10 but not interleukin-6 is related to clinical outcome in patients with resectable hepatocellular carcinoma. Ann Surg 2000; 231: 552–558.
De Vita F, Orditura M, Galizia G, Romano C, Lieto E, Iodice P et al. Serum interleukin-10 is an independent prognostic factor in advanced solid tumors. Oncol Rep 2000; 7: 357–361.
Robinet E, Branellec D, Termijtelen AM, Blay JY, Gay F, Chouaib S et al. Evidence for tumor necrosis factor-alpha involvement in the optimal induction of class I allospecific cytotoxic T cells. J Immunol 1990; 144: 4555–4561.
Lahn M, Kalataradi H, Mittelstadt P, Pflum E, Vollmer M, Cady C et al. Early preferential stimulation of gamma delta T cells by TNF-alpha. J Immunol 1998; 160: 5221–5230.
Zhang W, Chen Z, Li F, Kamencic H, Juurlink B, Gordon JR et al. Tumour necrosis factor-alpha (TNF-alpha) transgene-expressing dendritic cells (DCs) undergo augmented cellular maturation and induce more robust T-cell activation and anti-tumour immunity than DCs generated in recombinant TNF-alpha. Immunology 2003; 108: 177–188.
Lyakh LA, Koski GK, Telford W, Gress RE, Cohen PA, Rice NR et al. Bacterial lipopolysaccharide, TNF-alpha, and calcium ionophore under serum-free conditions promote rapid dendritic cell-like differentiation in CD14+ monocytes through distinct pathways that activate NK-kappa B. J Immunol 2000; 165: 3647–3655.
Sepulveda H, Cerwenka A, Morgan T, Dutton RW . CD28, IL-2-independent costimulatory pathways for CD8 T lymphocyte activation. J Immunol 1999; 163: 1133–1142.
Brunner C, Seiderer J, Schlamp A, Bidlingmaier M, Eigler A, Haimerl W et al. Enhanced dendritic cell maturation by TNF-alpha or cytidine-phosphate-guanosine DNA drives T cell activation in vitro and therapeutic anti-tumor immune responses in vivo. J Immunol 2000; 165: 6278–6286.
Brossart P, Zobywalski A, Grunebach F, Behnke L, Stuhler G, Reichardt VL et al. Tumor necrosis factor alpha and CD40 ligand antagonize the inhibitory effects of interleukin 10 on T-cell stimulatory capacity of dendritic cells. Cancer Res 2000; 60: 4485–4492.
Wright P, Braun R, Babiuk L, Littel-van den Hurk SD, Moyana T, Zheng C et al. Adenovirus-mediated TNF-alpha gene transfer induces significant tumor regression in mice. Cancer Biother Radiopharm 1999; 14: 49–57.
Xiang J, Huang H, Liu Y . A new dynamic model of CD8+ T effector cell responses via CD4+ T helper-antigen-presenting cells. J Immunol 2005; 174: 7497–7505.
Li M, Davey GM, Sutherland RM, Kurts C, Lew AM, Hirst C et al. Cell-associated ovalbumin is cross-presented much more efficiently than soluble ovalbumin in vivo. J Immunol 2001; 166: 6099–6103.
He TC, Zhou S, da Costa LT, Yu J, Kinzler KW, Vogelstein B et al. A simplified system for generating recombinant adenoviruses. Proc Natl Acad Sci USA 1998; 95: 2509–2514.
Liu Y, Ye T, Sun D, Maynard J, Deisseroth A . Conditionally replication-competent adenoviral vectors with enhanced infectivity for use in gene therapy of melanoma. Hum Gene Ther 2004; 15: 637–647.
Chan T, Sami A, El-Gayed A, Guo X, Xiang J . HER-2/neu-gene engineered dendritic cell vaccine stimulates stronger HER-2/neu-specific immune responses compared to DNA vaccination. Gene ther 2006; 13: 1391–1402.
Zeng M, Smith SK, Siegel F, Shi Z, Van Kampen KR, Elmets CA et al. AdEasy system made easier by selecting the viral backbone plasmid preceding homologous recombination. Biotechniques 2001; 31: 260–262.
Huang H, Liu Y, Xiang J . Synergistic effect of adoptive T-cell therapy and intratumoral interferon gamma-inducible protein-10 transgene expression in treatment of established tumors. Cell Immunol 2002; 217: 12–22.
Chen Z, Huang H, Chang T, Carsen S, Saxena A, Marr R et al. Enhanced HER-2/neu-specific antitumor immunity by cotransduction of mouse dendritic cells with two genes encoding HER-2/neu and alpha tumor necrosis factor. Cancer Gene Ther 2002; 9: 778–786.
Liu Y, Huang H, Chen Z, Zong L, Xiang J . Dendritic cells engineered to express the Flt3 ligand stimulate type I immune response, and induce enhanced cytoxic T and natural killer cell cytotoxicities and antitumor immunity. J Gene Med 2003; 5: 668–680.
Xia D, Hao S, Xiang J . CD8+ cytotoxic T-APC stimulate central memory CD8+ T cell responses via acquired peptide-MHC class I complexes and CD80 costimulation and IL-2 secretion. J Immunol 2006; 177: 2976–2984.
Speiser DE, Romero P . Toward improved immunocompetence of adoptively transferred CD8+ T cells. J Clin Invest 2005; 115: 1467–1469.
Zammit DJ, Cauley LS, Pham QM, Lefrancois L . Dendritic cells maximize the memory CD8 T cell response to infection. Immunity 2005; 22: 561–570.
Dyer MR, Herrling PL . Progress and potential for gene-based medicines. Mol Ther 2000; 1: 213–224.
Marshall E . Gene therapy. Second child in French trial is found to have leukemia. Science 2003; 299: 320.
Bergelson JM, Cunningham JA, Droguett G, Kurt-Jones EA, Krithivas A, Hong JS et al. Isolation of a common receptor for Coxsackie B viruses and adenoviruses 2 and 5. Science 1997; 275: 1320–1323.
Wickham TJ, Mathias P, Cheresh DA, Nemerow GR . Integrins alpha v beta 3 and alpha v beta 5 promote adenovirus internalization but not virus attachment. Cell 1993; 73: 309–319.
Nemerow GR . Cell receptors involved in adenovirus entry. Virology 2000; 274: 1–4.
Huang S, Endo RI, Nemerow GR . Upregulation of integrins alpha v beta 3 and alpha v beta 5 on human monocytes and T lymphocytes facilitates adenovirus-mediated gene delivery. J Virol 1995; 69: 2257–2263.
Huang S, Kamata T, Takada Y, Ruggeri ZM, Nemerow GR . Adenovirus interaction with distinct integrins mediates separate events in cell entry and gene delivery to hematopoietic cells. J Virol 1996; 70: 4502–4508.
Okada N, Saito T, Masunaga Y, Tsukada Y, Nakagama S, Mizuguchi H et al. Efficient antigen gene transduction using Arg-Gly-Asp fiber-mutant adenovirus vectors can potentiate antitumor vaccine efficacy and maturation of murine dendritic cells. Cancer Res 2001; 61: 7913–7919.
Okada N, Masunaga Y, Okada Y, Iiyama S, Mori N, Tsuda T et al. Gene transduction efficiency and maturation status in mouse bone marrow-derived dendritic cells infected with conventional or RGD fiber-mutant adenovirus vectors. Cancer Gene Ther 2003; 10: 421–431.
Kagi D, Vignaux F, Ledermann B, Burki K, Depraetere V, Nagata S et al. Fas and perforin pathways as major mechanisms of T cell-mediated cytotoxicity. Science 1994; 265: 528–530.
Huang H, Li F, Gordon JR, Xiang J . Synergistic enhancement of antitumor immunity with adoptively transferred tumor-specific CD4+ and CD8+ T cells and intratumoral lymphotactin transgene expression. Cancer Res 2002; 62: 2043–2051.
Huang H, Bi XG, Yuan JY, Xu SL, Guo XL, Xiang J . Combined CD4+ Th1 effect and lymphotactin transgene expression enhance CD8+ Tc1 tumor localization and therapy. Gene Ther 2005; 12: 999–1010.
Winter H, Hu HM, Urba WJ, Fox BA . Tumor regression after adoptive transfer of effector T cells is independent of perforin or Fas ligand (APO-1L/CD95L). J Immunol 1999; 163: 4462–4472.
Poehlein CH, Hu HM, Yamada J, Assmann I, Alvord WG, Urba WJ et al. TNF plays an essential role in tumor regression after adoptive transfer of perforin/IFN-gamma double knockout effector T cells. J Immunol 2003; 170: 2004–2013.
Hollenbaugh JA, Dutton RW . IFN-gamma regulates donor CD8 T cell expansion, migration, and leads to apoptosis of cells of a solid tumor. J Immunol 2006; 177: 3004–3011.
Blohm U, Potthoff D, van der Kogel AJ, Pircher H . Solid tumors ‘melt’ from the inside after successful CD8 T cell attack. Eur J Immunol 2006; 36: 468–477.
Prevost-Blondel A, Roth E, Rosenthal FM, Pircher H . Crucial role of TNF-alpha in CD8 T cell-mediated elimination of 3LL-A9 Lewis lung carcinoma cells in vivo. J Immunol 2000; 164: 3645–3651.
Sarraf C . Tumor necrosis factor and cell death in tumors. Int J Oncol 1994; 5: 1333–1339.
Tracey KJ, Cerami A . Tumor necrosis factor: a pleiotropic cytokine and therapeutic target. Annu Rev Med 1994; 45: 491–503.
Ruegg C, Yilmaz A, Bieler G, Bamat J, Chaubert P, Lejeune FJ et al. Evidence for the involvement of endothelial cell integrin alpha V beta 3 in the disruption of the tumor vasculature induced by TNF and IFN-gamma. Nat Med 1998; 4: 408–414.
Denekamp J . Review article: angiogenesis, neovascular proliferation and vascular pathophysiology as targets for cancer therapy. Br J Radiol 1993; 66: 181–196.
Valencia X, Stephens G, Goldbach-Mansky R, Wilson M, Shevach EM, Lipsky PE . TNF downmodulates the function of human CD4+CD25hi T-regulatory cells. Blood 2006; 108: 253–261.
Walter EA, Greenberg PD, Gilbert MJ, Finch RJ, Watanabe KS, Thomas ED et al. Reconstitution of cellular immunity against cytomegalovirus in recipients of allogeneic bone marrow by transfer of T-cell clones from the donor. N Engl J Med 1995; 333: 1038–1044.
Dudley ME, Wunderlich J, Nishimura MI, Yu D, Yang JC, Topalian SL et al. Adoptive transfer of cloned melanoma-reactive T lymphocytes for the treatment of patients with metastatic melanoma. J Immunother 2001; 24: 363–373.
Sprent J, Tough DF . T cell death and memory. Science 2001; 293: 245–248.
Zhang HG, Liu C, Su K, Yu S, Zhang L, Zhang S et al. A membrane form of TNF-alpha presented by exosomes delays T cell activation-induced cell death. J Immunol 2006; 176: 7385–7393.
Dobrzanski MJ, Reome JB, Hollenbaugh JA, Dutton RW . Tc1 and Tc2 effector cell therapy elicit long-term tumor immunity by contrasting mechanisms that result in complementary endogenous type 1 antitumor responses. J Immunol 2004; 172: 1380–1390.
Acknowledgements
This study was supported by research grants (MOP 67230/81228) of the Canadian Institutes of Health Research to JX. We thank Mark Boyd for his excellent technical support of flow cytometric analysis.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ye, Z., Shi, M., Chan, T. et al. Engineered CD8+ cytotoxic T cells with fiber-modified adenovirus-mediated TNF-α gene transfection counteract immunosuppressive interleukin-10-secreting lung metastasis and solid tumors. Cancer Gene Ther 14, 661–675 (2007). https://doi.org/10.1038/sj.cgt.7701039
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cgt.7701039
Keywords
This article is cited by
-
Efficient gene transfer into T lymphocytes by fiber-modified human adenovirus 5
BMC Biotechnology (2019)
-
Platelets promote tumour metastasis via interaction between TLR4 and tumour cell-released high-mobility group box1 protein
Nature Communications (2014)
-
Transgene expression of α tumor necrosis factor with mutations D142N and A144R under control of human telomerase reverse transcriptase promoter eradicates well-established tumors and induces long-term antitumor immunity
Cancer Gene Therapy (2009)