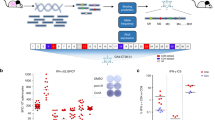
Abstract
Cancer vaccines are a promising approach to treating tumors or preventing tumor relapse through induction of an immune response against tumor-associated antigens (TAA). One major obstacle to successful therapy is the immunological tolerance against self-antigens which limits an effective antitumor immune response. As a transient reduction of immunological tolerance may enable more effective vaccination against self-tumor antigens, we explored this hypothesis in a CEA tolerant animal model with an adenovirus expressing CEA vaccine in conjunction with inactivation of CD4+CD25+ regulatory T cells. This vaccination modality resulted in increased CEA-specific CD8+, CD4+ T cells and antibody response. The appearance of a CD4+ T-cell response correlated with a stronger memory response. The combined CD25+ inactivation and genetic vaccination resulted in significant tumor protection in a metastatic tumor model. Non-invasive tumor visualization showed that not only primary tumors were reduced, but also hepatic metastases. Our results support the viability of this cancer vaccine strategy as an adjuvant treatment to prevent tumor relapse in cancer patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Waldmann TA . Effective cancer therapy through immunomodulation. Annu Rev Med 2006; 57: 65–81.
Sakaguchi S . Naturally arising CD4+ regulatory t cells for immunologic self-tolerance and negative control of immune responses. Annu Rev Immunol 2004; 22: 531–562.
Antony PA, Piccirillo CA, Akpinarli A, Finkelstein SE, Speiss PJ, Surman DR et al. CD8+ T cell immunity against a tumor/self-antigen is augmented by CD4+ T helper cells and hindered by naturally occurring T regulatory cells. J Immunol 2005; 174: 2591–2601.
McHugh RS, Shevach EM . Cutting edge: depletion of CD4+CD25+ regulatory T cells is necessary, but not sufficient, for induction of organ-specific autoimmune disease. J Immunol 2002; 168: 5979–5983.
Casares N, Arribillaga L, Sarobe P, Dotor J, Lopez-Diaz de Cerio A, Melero I et al. CD4+/CD25+ regulatory cells inhibit activation of tumor-primed CD4+ T cells with IFN-gamma-dependent antiangiogenic activity, as well as long-lasting tumor immunity elicited by peptide vaccination. J Immunol 2003; 171: 5931–5939.
Antony PA, Restifo NP . CD4+CD25+ T regulatory cells, immunotherapy of cancer, and interleukin-2. J Immunother 2005; 28: 120–128.
Kohm AP, McMahon JS, Podojil JR, Begolka WS, DeGutes M, Kasprowicz DJ et al. Cutting Edge: Anti-CD25 monoclonal antibody injection results in the functional inactivation, not depletion, of CD4+CD25+ T regulatory cells. J Immunol 2006; 176: 3301–3305.
Mennuni C, Calvaruso F, Facciabene A, Aurisicchio L, Storto M, Scarselli E et al. Efficient induction of T-cell responses to carcinoembryonic antigen by a heterologous prime-boost regimen using DNA and adenovirus vectors carrying a codon usage optimized cDNA. Int J Cancer 2005; 17: 444–455.
Facciabene A, Aurisicchio L, La Monica N . Baculovirus vectors elicit antigen-specific immune responses in mice. J Virol 2004; 78: 8663–8672.
Clarke P, Mann J, Simpson JF, Rickard-Dickson K, Primus FJ . Mice transgenic for human carcinoembryonic antigen as a model for immunotherapy. Cancer Res 1998; 58: 1469–1477.
Sallusto F, Lenig D, Forster R, Lipp M, Lanzavecchia A . Two subsets of memory T lymphocytes with distinct homing potentials and effector functions. Nature 1999; 401: 708–712.
Kaech SM, Hemby S, Kersh E, Ahmed R . Molecular and functional profiling of memory CD8T cell differentiation. Cell 2002; 111: 837–851.
Klebanoff CA, Gattinoni L, Torabi-Parizi P, Kerstann K, Cardones AR, Finkelstein SE et al. Central memory self/tumor-reactive CD8+ T cells confer superior antitumor immunity compared with effector memory T cells. Proc Natl Acad Sci USA 2005; 102: 9571–9576.
Youil R, Toner TJ, Su Q, Chen M, Tang A, Bett AJ et al. Hexon gene switch strategy for the generation of chimeric recombinant adenovirus. Hum Gene Ther 2002; 13: 311–320.
Hodge JW, Grosenbach DW, Aarts WM, Poole DJ, Schlom J . Vaccine therapy of established tumors in the absence of autoimmunity. Clin Cancer Res 2003; 9: 1837–1849.
Golgher D, Jones E, Powrie F, Elliott T, Gallimore A . Depletion of CD25+ regulatory cells uncovers immune responses to shared murine tumor rejection antigens. Eur J Immunol 2002; 32: 3267–3275.
Facciabene A, Aurisicchio L, Elia L, Palombo F, Mennuni C, Ciliberto G et al. DNA and adenoviral vectors encoding carcinoembryonic antigen fused to immunoenhancing sequences augment antigen-specific immune response and confer tumor protection. Hum Gene Ther 2006; 17: 81–92.
Zhou H, Luo Y, Mizutani M, Mizutani N, Becker JC, Primus FJ et al. A novel transgenic mouse model for immunological evaluation of carcinoembryonic antigen-based DNA minigene vaccines. J Clin Invest 2004; 113: 1792–1798.
Kass E, Schlom J, Thompson J, Guadagni F, Graziano P, Greiner JW . Induction of protective host immunity to carcinoembryonic antigen (CEA), a self-antigen in CEA transgenic mice, by immunizing with a recombinant vaccinia-CEA virus. Cancer Res 1999; 59: 676–683.
Bos R, van Duikeren S, van Hall T, Kaaijk P, Taubert R, Kyewski B et al. Expression of a natural tumor antigen by thymic epithelial cells impairs the tumor-protective CD4+ T-cell repertoire. Cancer Res 2005; 65: 6443–6449.
Tanaka H, Tanaka J, Kjaergaard J, Shu S . Depletion of CD4+ CD25+ regulatory cells augments the generation of specific immune T cells in tumor-draining lymph nodes. J Immunother 2002; 25: 207–217.
Shimizu J, Yamazaki S, Sakaguchi S . Induction of tumor immunity by removing CD25+CD4+ T cells: a common basis between tumor immunity and autoimmunity. J Immunol 1999; 163: 5211–5218.
Jones E, Dahm-Vicker M, Simon AK, Green A, Powrie F, Cerundolo V et al. Depletion of CD25+ regulatory cells results in suppression of melanoma growth and induction of autoreactivity in mice. Cancer Immun 2002; 2: 1.
Tawara I, Take Y, Uenaka A, Noguchi Y, Nakayama E . Sequential involvement of two distinct CD4+ regulatory T cells during the course of transplantable tumor growth and protection from 3-methylcholanthrene-induced tumorigenesis by CD25-depletion. Jpn J Cancer Res 2002; 93: 911–916.
Kudo-Saito C, Schlom J, Camphausen K, Coleman CN, Hodge JW . The requirement of multimodal therapy (vaccine, local tumor radiation, and reduction of suppressor cells) to eliminate established tumors. Clin Cancer Res 2005; 11: 4533–4544.
Toka FN, Suvas S, Rouse BT . CD4+ CD25+ T cells regulate vaccine-generated primary and memory CD8+ T-cell responses against herpes simplex virus type 1. J Virol 2004; 78: 13082–13089.
Kursar M, Bonhagen K, Fensterle J, Kohler A, Hurwitz R, Kamradt T et al. Regulatory CD4+CD25+ T cells restrict memory CD8+ T cell responses. J Exp Med 2002; 196: 1585–1592.
Sakaguchi S, Takahashi T, Yamazaki S, Kuniyasu Y, Itoh M, Sakaguchi N et al. Immunologic self tolerance maintained by T-cell-mediated control of self-reactive T cells: implications for autoimmunity and tumor immunity. Microbes Infect 2001; 3: 911–918.
Wei WZ, Jacob JB, Zielinski JF, Flynn JC, Shim KD, Alsharabi G et al. Concurrent induction of antitumor immunity and autoimmune thyroiditis in CD4+ CD25+ regulatory T cell-depleted mice. Cancer Res 2005; 65: 8471–8478.
Dannull J, Su Z, Rizzieri D, Yang BK, Coleman D, Yancey D et al. Enhancement of vaccine-mediated antitumor immunity in cancer patients after depletion of regulatory T cells. J Clin Invest 2005; 115: 3623–3633.
Lyons SK . Advances in imaging mouse tumour models in vivo. J Pathol 2005; 205: 194–205.
Acknowledgements
We thank Fabrizio Colaceci and Walter Castaldi for animal care and Janet Clench for editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Elia, L., Aurisicchio, L., Facciabene, A. et al. CD4+CD25+ regulatory T-cell-inactivation in combination with adenovirus vaccines enhances T-cell responses and protects mice from tumor challenge. Cancer Gene Ther 14, 201–210 (2007). https://doi.org/10.1038/sj.cgt.7701004
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cgt.7701004
Keywords
This article is cited by
-
Neoantigen cancer vaccine augments anti-CTLA-4 efficacy
npj Vaccines (2022)
-
Psychopharmacology: neuroimmune signaling in psychiatric disease-developing vaccines against abused drugs using toll-like receptor agonists
Psychopharmacology (2019)
-
Inhibition and promotion of tumor growth with adeno-associated virus carcinoembryonic antigen vaccine and Toll-like receptor agonists
Cancer Gene Therapy (2011)
-
Tumour hypoxia promotes tolerance and angiogenesis via CCL28 and Treg cells
Nature (2011)
-
An oral TLR7 agonist is a potent adjuvant of DNA vaccination in transgenic mouse tumor models
Cancer Gene Therapy (2009)