Abstract
Objective:
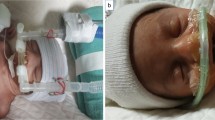
Respiratory distress syndrome (RDS) and bronchopulmonary dysplasia (BPD) are frequent complications of prematurity. To decrease ventilator-induced lung injury, we evaluated the safety, efficacy and neonatal outcomes of a heated humidified high-flow nasal cannula (HFNC) system and an early extubation protocol (EEP) designed for preterm infants 25 to 29 weeks’ gestational age (GA).
Study Design:
The Vapotherm (VT) high-flow humidification system was introduced to our unit in March 2004. After 10 months of VT use, an EEP was developed to begin January 2005. Infants 25 to 29 weeks of GA, intubated for RDS, were enrolled in January–December 2005 to extubate to VT following the EEP. Exclusion criteria were: major congenital anomalies, asphyxia and a 5 min Apgar score <5. Variables examined included BPD, growth and infection. Subjects were compared to historical controls, admitted January to December 2003, prior to the use of VT.
Result:
Inclusion criteria were met by 49/57 infants in the control group and 65/75 infants in the HFNC group. The groups had similar demographics, perinatal conditions, birthweight, GA, timing and total doses of surfactant. There were no differences in rates of extubation failure, patent ductus arteriosus, intraventricular hemorrhage, periventricular leukomalacia, necrotizing enterocolitis, laser eye surgery, sepsis, BPD at 28 days and 36 weeks and death. The groups did not differ in oxygen use, i.v. steroid days, or parenteral nutrition days. Days to reach full feeds were similar. Infants in the HFNC group were extubated from a higher ventilator rate (32.6±8.5 vs 28±7.5, P=0.003) and spent fewer days on the ventilator (11.4±12.8 vs 18.5±21, P=0.028). Rates of ventilator-associated pneumonia were higher in the control group (P=0.018). Discharge weights were greater in the HFNC group (P=0.016) despite similar length of stay and GA at discharge.
Conclusion:
High-flow nasal cannula use appears safe and well-tolerated. Infants extubated to HFNC spent fewer days on the ventilator. Additional benefits may include a decreased rate of ventilator associated with pneumonia and improved growth.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Abbreviations
- BPD:
-
bronchopulmonary dysplasia
- CPAP:
-
continuous positive airway pressure
- EEP:
-
early extubation protocol
- FiO2:
-
fraction of inspired oxygen
- HFNC:
-
high-flow nasal cannula
- NCPAP:
-
nasal continuous positive airway pressure
- NICU:
-
neonatal intensive care unit
- PDA:
-
patent ductus arteriosus
- RDS:
-
respiratory distress syndrome
- VT:
-
Vapotherm.
References
Gilmore MM . Preterm VLBW infants: post-extubation respiratory support. J Perinatol 2006; 26: 449–451.
Saslow JG, Aghai ZH, Nakhla TA, Hart JJ, Lawrysh R, Stahl GE et al. Work of breathing using high-flow nasal cannula in preterm infants. J Perinatol 2006; 26: 476–480.
Woodhead DD, Lambert DK, Clark JM, Christensen RD . Comparing two methods of delivering high-flow gas therapy by nasal cannula following endotracheal extubation: a prospective, randomized, masked, crossover trial. J Perinatol 2006; 26: 481–485.
Shoemaker MT, Pierce MR, Yoder BA, DiGeronimo RJ . High flow nasal cannula versus nasal continuous positive airway pressure for neonatal respiratory disease: a retrospective study. J Perinatol 2007; 27: 85–91.
Papile LA, Burstein J, Burstein R, Koffler H . Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with weight less than 1500 grams. J Pediatr 1978; 92: 529–534.
Volpe JJ . Hypoxic–ischemic encephalopathy: neuropathology and pathogenesis. Neurology of the Newborn 4th edn. WB Saunders: Philadelphia, PA, 2001 p. 307–315.
Bell MJ . Neonatal necrotizing enterocolitis: therapeutic decisions based on clinical staging. Ann Surg 1978; 187: 1–7.
Gole GA, Ells AL, Katz X, Holstrom G, Fielder AR, Capone A et al. An international committee for the classification of retinopathy of prematurity. The international classification of retinopathy revisited. Arch Ophthalmol 2005; 123: 991–999.
Gitterman M, Fusch C, Gitterman A, Regazzoni B, Moessinger A . Early continuous positive airway pressure treatment reduces the need for intubation in very low birth weight infants. Eur J Pediatr 1997; 156: 384–388.
Kamper J, Wulff K, Larsen C, Lindequist S . Early treatment with nasal continuous positive airway pressure in very low birth weight infants. Acta Paediatr 1993; 82: 193–197.
Davis PG, Henderson-Smart DJ . Nasal continuous positive airway pressure immediately after extubation for preventing morbidity in preterm infants. Cochrane Database of Syst Rev 2000; 3: CD000143.
Polin RA, Sahni R . Newer experience with CPAP. Semin Neonatol 2002; 7: 379–389.
Thompson MA . Early nasal continuous positive airway pressure to minimize the need for endotracheal intubation and ventilation. Neoreviews 2005; 6: e184–e188.
Goldsmith JP . Assisted Ventilation of the Neonate 4th edn. WB Sanders: Philadelphia, PA, 2003; 127–147.
Waugh JB, Granger WM . An evaluation of two devices for nasal high-flow gas therapy. Respir Care 2004; 49: 902–906.
Gilmore M . Pre-term very low birth weight infants: post-extubation support. J Perinatol 2006; 26: 449–451.
Finer NN . Nasal cannula use in the preterm infant; oxygen or pressure? Pediatrics 2005; 116 (5): 1216–1217.
Graham PL, Begg MD, Larson E, Della-Latta P, Allen A, Saiman L . Risk factors for late onset Gram-negative sepsis in low birth weight infants hospitalized in the neonatal intensive care unit. Pediatr Infect Dis J 2006; 25: 113–117.
Tooley J, Dyke M . Randomized study of nasal continuous positive airway pressure in the preterm infant with respiratory distress syndrome. Acta Paedriatr 2003; 92: 1170–1174.
Premer DM, Georgieff MK . Nutrition for ill neonates. Pediatr Rev 1999; 20: e56–e62.
Acknowledgements
This study was conducted at the Loyola University Medical Center. The study was designed, conducted and analyzed independently of the company. None of the authors received any compensation from Vapotherm, or hold stock in the company. This work was presented in poster format at the American Academy of Pediatrics National Conference, Atlanta, GA, October 2006.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Holleman-Duray, D., Kaupie, D. & Weiss, M. Heated humidified high-flow nasal cannula: use and a neonatal early extubation protocol. J Perinatol 27, 776–781 (2007). https://doi.org/10.1038/sj.jp.7211825
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7211825
Keywords
This article is cited by
-
Peri-extubation settings in preterm neonates: a systematic review and meta-analysis
Journal of Perinatology (2024)
-
Consensus approach to nasal high-flow therapy in neonates
Journal of Perinatology (2017)
-
Applications of Nasal High-Flow Oxygen Therapy in Critically ill Adult Patients
Lung (2016)
-
Reducing ventilator-associated pneumonia in neonatal intensive care unit using “VAP prevention Bundle”: a cohort study
BMC Infectious Diseases (2015)
-
Work of breathing indices in infants with respiratory insufficiency receiving high-flow nasal cannula and nasal continuous positive airway pressure
Journal of Perinatology (2014)