Abstract
In a meta-analysis of testicular cancer in twins, twins had a 30% increased risk (estimate 1.31, 95% CI 1.1–1.6), providing indirect support for the hypothesis that in utero hormone variations influence risk of testicular cancer. The summary-estimate for dizygotic twins was 1.3 (1.0–1.7) and for monozygotic or same sex twins 1.4 (1.2–1.8).
Similar content being viewed by others
Main
Testicular germ-cell cancer is either the most common or second most common cancer in men aged 15–45, depending on country, and rates have been increasing substantially in developed countries over the past few decades (Huyghe et al, 2007). Despite attempts to identify risk factors, the aetiology remains unclear. Cryptorchidism, age (Garner et al, 2005), contra-lateral disease, and family history (Hemminki and Chen, 2006) are the only established risk factors. Both low and high birth weight may also be associated (Michos et al, 2007). Evidence from animal models (Newbold et al, 1987), and indirectly from human studies (reviewed in Grotmol et al, 2006), indicates that the susceptibility for testicular cancer is probably established in utero. The relative importance of environmental factors and genetic factors are not clear, but it is likely that both play an aetiological role (Oosterhuis and Looijenga, 2003). Although the mechanism is uncertain, it is thought that foetal exposure to unusually high oestrogen levels, or an imbalance of oestrogen and androgen levels, might contribute to an increased risk. Examining features of pregnancy, which can affect the levels of these hormones, may help to elucidate the aetiology of this cancer. Twinning is of interest, as twin pregnancies, perhaps particularly with dizygotic twins, result in higher maternal levels of serum oestrogens than with singleton pregnancies.
Several studies have suggested an association between being a twin and testicular cancer, but as both testicular cancer and twinning are rare events, inferences have been limited by a lack of precision in most studies. We therefore aimed to improve the precision of the estimate of testicular cancer risk among twins by carrying out a meta-analysis of previously published studies.
Materials and methods
Studies published in English between 1961 and 2006 were identified through systematic searches of computerised bibliographic databases (Medline and Embase) using combinations of individual search terms and subject headings. We inspected the reference lists of studies retrieved from these initial searches for previously unidentified studies, which were then located on Medline to identify their subject headings. Further searches were then undertaken using these derived subject headings.
We included all studies that had reported the risk of testicular cancer in twins compared with the general population or a specific single birth control group. Some studies did not provide a risk estimate for all male twins, instead reporting monozygotic and dizygotic twin risks separately (Braun et al, 1995; Swerdlow et al, 1997; Verkasalo et al, 1999), but if a total estimate could be calculated from the data provided, these studies were included.
Analyses were conducted using the meta command in Stata (StataCorp LP, College Station, TX, USA), which tests that the true pooled effect is zero. Tests for heterogeneity were based on the Q statistic. Due to the small number of studies, we report on the random effect estimates and include the overall fixed effect estimate for completeness. Sensitivity analyses were conducted by assessing the impact of dropping specific studies on the overall estimated pooled effect. While acknowledging their limited power, we used Begg's test and Egger's test to assess whether there was any evidence of publication bias.
Results
We identified seven studies, which met our inclusion criteria (Table 1; Braun et al, 1995; Westergaard et al, 1998; Verkasalo et al, 1999; Dieckmann et al, 2001; Iversen et al, 2001; Hemminki and Chen, 2005; Neale et al, 2005). Six were cohort or retrospective cohort studies providing relative risks (RRs) or standardised incidence ratios (SIRs), and one (Dieckmann et al, 2001) was a case–control study providing an odds ratio (OR). The number of testicular cancer cases ranged from 4 to 112. Two of these studies were from Sweden and it is likely that the later study has some overlap of study subjects with those in the earlier study.
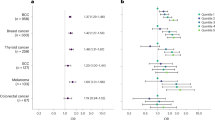
Six of the seven studies reported an increased risk of testicular cancer among twins (Figure 1), with two estimates being significant (Dieckmann et al, 2001; Hemminki and Chen, 2005). The smallest study found a non-significant decrease in risk. There was no significant heterogeneity between studies (Q=6.18, df=5, P=0.289). The pooled estimate of risk was 1.31 (1.1–1.6) assuming random effects and 1.34 (95% CI 1.2–1.5) assuming fixed effects. Excluding the earlier Swedish study resulted in an estimate of 1.3 (1.0–1.7) (P=0.068). When we additionally excluded the study with only four cases, we found a risk of testicular cancer among twins of 1.4 (1.2–1.6). We conducted a further analysis excluding the largest and smallest studies, generating a risk estimate of 1.4 (1.1–1.7). Removing the only case–control study did not materially alter the summary estimate. There was no evidence of publication bias (Begg: z=−0.45, P=0.652; Egger: t=−0.63, P=0.555).
Five studies either reported the dizygotic twin risk or the risks for male twins that came from an opposite sex twin pair. Pooling these risks resulted in a similar estimate of risks as for all twins (OR 1.3, 95% CI 1.0–1.7). The summary estimate for monozygotic or same sex twins was 1.4 (1.2–1.8).
Discussion
Only two studies have previously found a significant positive association between twinning and the development of testicular cancer, with four others generating suggestive but non-significant results and one finding a non-significant protective effect. These analyses indicate that these are unlikely to be chance findings, that the result is not sensitive to the inclusion/exclusion of eligible studies, and that there is a real increase in testicular cancer among twins.
Case–control studies have previously suggested a role for maternal and pregnancy-related factors for the development of testicular cancer, with speculation that high in utero oestrogen exposure may be the underlying cause (Wanderas et al, 1998; Richiardi et al, 2002). Twin pregnancies are associated with higher levels of placental hormones than singleton pregnancies, and thus this finding of a significant 30% increase in risk of testicular cancer among twins provides indirect evidence for the in utero hormone hypothesis.
Dizygotic mothers have a different menstrual, although not necessarily gestational, hormonal profile than mothers of monozygotic twins. A small proportion of twins will have resulted from ovulation induction in subfertile women who may have distinctly different cyclical hormone patterns, although their pregnancy levels are not likely to be unusual. Some studies included here and others not included report higher testicular cancer risks among dizygotic than monozygotic twins (Braun et al, 1995; Swerdlow et al, 1997), although this finding is not consistent (Verkasalo et al, 1999). Our summary estimates did not support the hypothesis of a higher risk in dizygotic twins than monozygotic or like sex twins, with the estimate for the latter being marginally and not significantly higher. However about half of the like-sex twins would be dizygotic, which could have obscured a real difference.
Apart from the circulating oestrogen hypothesis, there are many other aspects of twin pregnancies (in particular dizygotic pregnancies) that may alter risk of testicular cancer. These include different levels of many other hormones and characteristics of the mother including age, parity, and height (Blondel and Kaminski, 2002). Twins on average weigh about 1000 g less than singleton births and low birth weight may be a risk factor for testicular cancer (Michos et al, 2007).
There is emerging evidence that being a twin is protective for childhood cancer, possibly due to the lower birth weight of twins, earlier limitation of their growth velocity, or the selection effects of higher intrauterine death rates (Murphy et al, 2001; Neale et al, 2005; Milne et al, 2007). It is not yet known how far this extends into young adulthood, although it seems likely that there is no long-term difference in the overall risk of cancer in twins compared with singletons (Hemminki and Chen, 2005). Hence any isolated finding in young adulthood, such as that reported here, is salient. These results highlight the importance of exploring maternal factors that influence oestrogen levels, such as obesity, that may be responsible for the rapid increase in testicular cancer incidence that has been seen in many countries over the past several decades.
Change history
16 November 2011
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Blondel B, Kaminski M (2002) Trends in the occurrence, determinants, and consequences of multiple births. Semin Perinatol 26: 239–249
Braun MM, Ahlbom A, Floderus B, Brinton LA, Hoover RN (1995) Effect of twinship on incidence of cancer of the testis, breast, and other sites (Sweden). Cancer Causes Control 6: 519–524
Dieckmann KP, Endsin G, Pichlmeier U (2001) How valid is the prenatal estrogen excess hypothesis of testicular germ cell cancer? A case control study on hormone-related factors. Eur Urol 40: 677–683, discussion 684
Garner MJ, Turner MC, Ghadirian P, Krewski D (2005) Epidemiology of testicular cancer: an overview. Int J Cancer 116: 331–339
Grotmol T, Weiderpass E, Tretli S (2006) Conditions in utero and cancer risk. Eur J Epidemiol 21: 561–570
Hemminki K, Chen B (2005) Are twins at risk of cancer: results from the Swedish family-cancer database. Twin Res Hum Genet 8: 509–514
Hemminki K, Chen B (2006) Familial risks in testicular cancer as aetiological clues. Int J Androl 29: 205–210
Huyghe E, Plante P, Thonneau PF (2007) Testicular cancer variations in time and space in Europe. Eur Urol 51: 621–628
Iversen T, Tretli S, Kringlen E (2001) An epidemiological study of cancer in adult twins born in Norway 1905–1945. Br J Cancer 84: 1463–1465
Michos A, Xue F, Michels KB (2007) Birth weight and the risk of testicular cancer: a meta-analysis. Int J Cancer 121: 1123–1131
Milne E, Laurvick CL, Blair E, Bower C, de Klerk N (2007) Fetal growth and acute childhood leukemia: looking beyond birth weight. Am J Epidemiol 166: 151–159
Murphy MF, Whiteman D, Hey K, Griffith M, Gill L, Goldacre MJ, Vincent TJ, Bunch K (2001) Childhood cancer incidence in a cohort of twin babies. Br J Cancer 84: 1460–1462
Neale RE, Mineau G, Whiteman DC, Brownbill P, Murphy MF (2005) Childhood and adult cancer in twins: evidence from the Utah genealogy. Cancer Epidemiol Biomarkers Prev 14: 1236–1240
Newbold RR, Bullock BC, McLachlan JA (1987) Testicular tumors in mice exposed in utero to diethylstilbestrol. J Urol 138: 1446–1450
Oosterhuis JW, Looijenga LH (2003) Current views on the pathogenesis of testicular germ cell tumours and perspectives for future research: highlights of the 5th Copenhagen Workshop on Carcinoma in situ and Cancer of the Testis. APMIS 111: 280–289
Richiardi L, Akre O, Bellocco R, Ekbom A (2002) Perinatal determinants of germ-cell testicular cancer in relation to histological subtypes. Br J Cancer 87: 545–550
Swerdlow AJ, De Stavola BL, Swanwick MA, Maconochie NE (1997) Risks of breast and testicular cancers in young adult twins in England and Wales: evidence on prenatal and genetic aetiology. Lancet 350: 1723–1728
Verkasalo PK, Kaprio J, Koskenvuo M, Pukkala E (1999) Genetic predisposition, environment and cancer incidence: a nationwide twin study in Finland, 1976–1995. Int J Cancer 83: 743–749
Wanderas EH, Grotmol T, Fossa SD, Tretli S (1998) Maternal health and pre- and perinatal characteristics in the etiology of testicular cancer: a prospective population- and register-based study on Norwegian males born between 1967 and 1995. Cancer Causes Control 9: 475–486
Westergaard T, Andersen PK, Pedersen JB, Frisch M, Olsen JH, Melbye M (1998) Testicular cancer risk and maternal parity: a population-based cohort study. Br J Cancer 77: 1180–1185
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Neale, R., Carrière, P., Murphy, M. et al. Testicular cancer in twins: a meta-analysis. Br J Cancer 98, 171–173 (2008). https://doi.org/10.1038/sj.bjc.6604136
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bjc.6604136
Keywords
This article is cited by
-
Testicular germ cell tumor: a comprehensive review
Cellular and Molecular Life Sciences (2019)
-
Genomic screening of testicular germ cell tumors from monozygotic twins
Orphanet Journal of Rare Diseases (2014)
-
Contrasting effects of Deadend1 (Dnd1) gain and loss of function mutations on allelic inheritance, testicular cancer, and intestinal polyposis
BMC Genetics (2013)
-
Meta-analysis identifies four new loci associated with testicular germ cell tumor
Nature Genetics (2013)
-
Perinatal markers of estrogen exposure and risk of testicular cancer: follow-up of 1,333,873 Danish males born between 1950 and 2002
Cancer Causes & Control (2009)