Abstract
Local adenoviral gene transfer can be performed by means of isolated hepatic perfusion (IHP). This methodology is a very effective and safe way to deliver adenoviral vectors. We studied the immune response after IHP. A decreased neutralising antibody formation was observed, offering possibilities for further research in the field of gene therapy in isolated perfusion settings.
Similar content being viewed by others
Main
The main reason for failure of adenoviral gene delivery is insufficient transduction efficacy in vivo. A method, which improves in vivo efficacy, is locoregional administration. Previously, we and others demonstrated successful transduction and subsequent tumour response after isolated limb perfusion (ILP) and isolated hepatic perfusion (IHP) (de Roos et al, 1997, 2000; de Wilt et al, 2001; van Etten et al, 2002).
Adenoviral mediated gene transfer results in transient gene expression. Loss of the therapeutic gene requires readministration to achieve prolonged gene expression, which however is precluded by formation of neutralising antibodies (Yang et al, 1994; Kaplan et al, 1997). Since IHP is a technique with minimal systemic exposure and washout possibilities after the perfusion, immune response after adenoviral treatment may be impaired.
We performed IHP in rats with a recombinant adenoviral vector and investigated the production of neutralising antibodies and leukocytes compared to systemic intravenous (i.v.) treatment.
Materials and methods
Animals
Male inbred immunocompetent WAG/RIJ rats, weighing 250–300 g (Harlan-CPB, The Netherlands) were used. The rats were fed a standard laboratory diet and were housed under standard conditions of light and accommodation. The ethical committee for animal research of the Erasmus University Medical Center approved the protocol. The experimental protocols adhered to the rules outlined in the Dutch Animal Experimentation Act of 1977 and the published UKCCCR Guidelines for the Welfare of Animals in Experimental Neoplasia (Workman et al, 1998).
Recombinant adenovirus construct
The viral constructs were provided by Aventis-Pharma (Vitry-sur-Seine, France) and are described previously by us in detail (van Etten et al, 2002). AV1.0CMV is a recombinant replication-deficient adenovirus vector. AV1.0CMV.LacZ expresses the Escherichia coli derived β-galactosidase protein that can be detected by X-gal histochemistry.
Routes of administration
Isolated hepatic perfusion
We have described the rat isolated liver perfusion model in detail earlier (van IJken et al, 2000). Rats were perfused for 10 min with oxygenated and heated (38–39°C) colloid fluid (Haemaccel, Behring Pharma, Amsterdam, Netherlands) with 1.0 × 1011 virus particles (vp). This dose was previously determined as the maximum tolerated dose (MTD). Afterwards, a washout procedure was performed to remove all nonbound viruses by perfusing with 10 ml Haemaccel.
Intravenous injection
A volume of 200 μl of PBS containing 2.5 × 1011 vp (MTD) was slowly injected into the penile vein.
Blood and tissue sampling
Blood samples were taken via the tail vein at day 0, 3, 6, 9,16, 23, and 30 after treatment. Serum was collected after centrifugation (16 000 × g) and stored at −80°C until further analysis. At 24 h after treatment animals were killed. Liver was taken out and snap frozen in liquid nitrogen. Cryosections of tissue samples were stained according to the X-gal staining protocol (van Etten et al, 2002).
Measurement of neutralising antibodies
Adenovirus type 5 specific neutralising antibodies were measured by the virus neutralisation (VN) test as previously described (Schrader and Wigand, 1981; De Jong et al, 1999). The presence of cytopathic effects of Hep 2 cells caused by the virus was scored under the microscope. Neutralising antibody titres were expressed as the highest serum dilution showing no cytopathological effects.
Measurement of leukocyte count, liver and renal functions
Leukocyte numerations were determined with a microcell counter (Sysmex; Kyoto, Japan). Liver functions (alkaline phosphatase, alaline aminotransferase, aspartate aminotransferase, total bilirubin and γ-glutamyl transpeptidase) and renal functions (creatinin and urea) were measured by spectophotometric analysis (ELAN-analyzer; Eppendorf-Merck, Hamburg, Germany).
Statistical analysis
Results were evaluated for statistical significance with the Kruskal–Wallis and Mann–Whitney U tests with SPSSv10.0 for Windows 2000. A significance level of P<0.05 was used.
Results
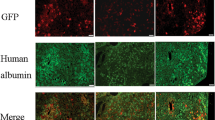
We observed augmented transfection of cells after isolated perfusion (n=3) (transduction efficacy of 80–90%) compared to systemic therapy (n=3) (transduction efficacy around 5%) (Figure 1).
Antibody titres after IHP (n=5) were significantly lower compared to i.v. (n=5) from day 3 up to day 23 (Figure 2). On day 6 after treatment a mean peak titre could be measured: 352 after i.v. injection vs 27 after IHP (P=0.03). During follow-up, performed up to 30 days after treatment the levels decreased and were equalised approximately as from day 23.
Neutralising antibody titre after i.v. (♦) or IHP (▴) with AV1.0CMV determined as described in Materials and methods section. Antibody titres after IHP were significantly lower compared to i.v. from day 3 up to day 23 (P⩽0.05). On day 6 after treatment a mean peak titre could be measured: 352 after i.v. injection vs. 27 after IHP (P=0.03). Mean values of five animals±s.d. are shown.
Leukocyte count was determined at day 6 after treatment. Numerations of leukocytes (mean values of three animals±s.d.) were significantly higher after i.v. (2.16 × 1010±0.19) compared to IHP (1.18 × 1010±0.45) or the untreated control group (1.15 × 1010±0.16), whereas leukocyte count after IHP was not increased compared to control values (i.v. vs IHP: P⩽0.05, i.v. vs control: P⩽0.05). The increased leukocyte count following i.v. administration correlates directly with the rise of titres measured after i.v. treatment.
No severe hepatic or renal toxicity could be detected in the i.v. or IHP group after treatment. Levels of toxicity parameters measured in sera varied in a range of + and −25% of the control values (data not shown). After i.v. injection, no weight loss was observed. Following IHP a maximum transient weight loss of 10% was observed, which could not be related to the viral vector as similar weight loss was observed upon sham IHP.
Discussion
Isolated hepatic perfusion is a more effective and safe method to deliver adenoviral vectors towards liver or tumour cells compared to i.v. injection (de Roos et al, 1997; van Etten et al, 2002). A transduction efficacy up to 45% of hepatocytes by means of IHP combined with a chelating agent has been described (de Roos et al, 1997). Here we demonstrate that this highly selective delivery method can result in even higher transduction rates and, importantly, is accompanied by an impaired neutralising antibody formation and leukocyte proliferation. Several studies have been conducted to influence immune response upon adenoviral gene therapy, including incorporation of immunosuppressive genes into the vector or manipulation of the immune system during administration (Qin et al, 1997; Nakagawa et al, 1998; Kuzmin et al, 2001). To our knowledge this is the first report demonstrating an impaired immune response using isolated perfusion methodology with a ‘regular’ adenoviral vector in an immunocompetent animal model.
The liver is known for its ability to induce immune tolerance (Calne, 2000). Both in patients and animal models host-to-graft tolerance was observed (Kamada et al, 1981; Mazariegos et al, 1997). Liver sinusoidal endothelial cells (LSECs), which clear the antigen from the blood can function as an antigen-presenting cell (Limmer et al, 2000). Naïve T cells, which are activated by the LSECs, do not differentiate into effector T cells thereby inducing antigen-specific T cell tolerance (Knolle and Limmer, 2001). This mechanism might play a role in the lesser immune response we observed.
It is known that the height of neutralising antibodies titres is correlated with the dose of virus administrated (Yang et al, 1996). Since most circulating viruses are washed away at the end the perfusion, only a relative low viral load is left behind in the liver. Worgall et al (1997) demonstrated that the acute innate immune mechanism eliminated 90% of the circulating adenoviral vectors within 24 h. So, if hardly any circulating viruses are left after IHP and the majority is cleared rapidly, only an extremely low amount of viruses can induce the humoral immune response, likely resulting in low neutralising antibody production.
Retrograde infusion of adenoviruses in the common bile duct of mice resulted in increased hepatic restricted gene transfer, combined with lower neutralising antibody titres (Peeters et al, 1996). It has been reported that the route of administration strongly determines the humoral immunity to the transgene in experiments with adeno-associated virus vectors in mice. Delivery via the hepatic artery resulted in higher transgene expression and an absent immune response to the transgene product (Nathwani et al, 2001). These results and our current findings suggest that loco-regional liver directed gene therapy offers advantages at gene transfer efficacy level as well as at immune response level. We recently performed pilot experiments with repeated administration. Primary adenovirus treatment by IHP followed by i.v. challenge 30 days later. These preliminary data showed no advantage with respect to transduction efficacy after the i.v. administration. Since repeated IHP in rats is not possible due to technical reasons we cannot provide data on this issue at this moment. In pigs we previously developed leakage free and potentially repeatable balloon catheter based IHP technique (van IJken et al, 1998), offering possibilities for future experiments with repeated IHP.
In conclusion, our findings are a strong argument for further research on delivery of viral vectors in isolated perfusion settings (limb, kidney, lung, liver).
Change history
16 November 2011
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Calne RY (2000) Immunological tolerance – the liver effect. Immunol Rev 174: 280–282
De Jong JC, Wermenbol AG, Verweij-Uijterwaal MW, Slaterus KW, Wertheim-Van DP, Van Doornum GJ, Khoo SH, Hierholzer JC (1999) Adenoviruses from human immunodeficiency virus-infected individuals, including two strains that represent new candidate serotypes Ad50 and Ad51 of species B1 and D, respectively. J Clin Microbiol JID – 7505564 37: 3940–3945
de Roos WK, de Wilt JH, van Der K, Manusama ER, de Vries MW, Bout A, ten Hagen TL, Valerio D, Eggermont AM (2000) Isolated limb perfusion for local gene delivery: efficient and targeted adenovirus-mediated gene transfer into soft tissue sarcomas. Ann Surg 232: 814–821
de Roos WK, Fallaux FJ, Marinelli AW, Lazaris-Karatzas A, von Geusau AB, van der Eb MM, Cramer SJ, Terpstra OT, Hoeben RC (1997) Isolated-organ perfusion for local gene delivery: efficient adenovirus-mediated gene transfer into the liver. Gene Ther 4: 55–62
de Wilt JH, Bout A, Eggermont AM, van Tiel ST, de Vries MW, ten Hagen TL, de Roos WK, Valerio D, van der Kaaden ME (2001) Adenovirus-mediated interleukin 3 beta gene transfer by isolated limb perfusion inhibits growth of limb sarcoma in rats. Hum Gene Ther 12: 489–502
Kamada N, Davies HS, Roser BJ (1981) Fully allogeneic liver grafting and the induction of donor-specific unreactivity. Transplant Proc 13: 837–841
Kaplan JM, Armentano D, Sparer TE, Wynn SG, Peterson PA, Wadsworth SC, Couture KK, Pennington SE, St George JA, Gooding LR, Smith AE (1997) Characterization of factors involved in modulating persistence of transgene expression from recombinant adenovirus in the mouse lung. Hum Gene Ther JID – 9008950 8: 45–56
Knolle PA, Limmer A (2001) Neighborhood politics: the immunoregulatory function of organ-resident liver endothelial cells. Trends Immunol JID – 100966032 2: 432–437
Kuzmin AI, Galenko O, Eisensmith RC (2001) An immunomodulatory procedure that stabilizes transgene expression and permits readministration of E1-deleted adenovirus vectors. Mol Ther JID – 100890581 3: 293–301
Limmer A, Ohl J, Kurts C, Ljunggren HG, Reiss Y, Groettrup M, Momburg F, Arnold B, Knolle PA (2000) Efficient presentation of exogenous antigen by liver endothelial cells to CD8+ T cells results in antigen-specific T-cell tolerance. Nat Med JID – 9502015 6: 1348–1354
Mazariegos GV, Reyes J, Marino I, Flynn B, Fung JJ, Starzl TE (1997) Risks and benefits of weaning immunosuppression in liver transplant recipients: long-term follow-up. Transplant Proc 29: 1174–1177
Nakagawa I, Murakami M, Ijima K, Chikuma S, Saito I, Kanegae Y, Ishikura H, Yoshiki T, Okamoto H, Kitabatake A, Uede T (1998) Persistent and secondary adenovirus-mediated hepatic gene expression using adenovirus vector containing CTLA4IgG. Hum Gene Ther JID – 9008950 9: 1739–1745
Nathwani AC, Davidoff A, Hanawa H, Zhou JF, Vanin EF, Nienhuis AW (2001) Factors influencing in vivo transduction by recombinant adeno-associated viral vectors expressing the human factor IX cDNA. Blood JID – 7603509 97: 1258–1265
Peeters MJ, Patijn GA, Lieber A, Meuse L, Kay MA (1996) Adenovirus-mediated hepatic gene transfer in mice: comparison of intravascular and biliary administration. Hum Gene Ther JID – 9008950 7: 1693–1699
Qin L, Ding Y, Pahud DR, Robson ND, Shaked A, Bromberg JS (1997) Adenovirus-mediated gene transfer of viral interleukin-10 inhibits the immune response to both alloantigen and adenoviral antigen. Hum Gene Ther JID – 9008950 8: 1365–1374
Schrader E, Wigand R (1981) Neutralization of adenovirus infectivity and cytotoxin in various cell cultures. J Virol Methods JID – 8005839 2: 321–330
van Etten B, ten Hagen TL, de Vries MR, Ambagtsheer G, Huet T, Eggermont AM (2002) Prerequisites for effective adenovirus mediated gene therapy of colorectal liver metastases in the rat using an intracellular neutralizing antibody fragment to p21-Ras. Br J Cancer JID – 0370635 86: 436–442
van IJken MG, de Bruijn EA, de Boeck G, ten Hagen TL, van der Sijp JR, Eggermont AM (1998) Isolated hypoxic hepatic perfusion with tumor necrosis factor-alpha, melphalan, and mitomycin C using balloon catheter techniques: a pharmacokinetic study in pigs. Ann Surg 228: 763–770
van IJken MG, van Etten B, de Wilt JH, van Tiel ST, ten Hagen TL, Eggermont AM (2000) Tumour necrosis factor-alpha augments tumour effects in isolated hepatic perfusion with melphalan in a rat sarcoma model. J Immunother JID – 9706083 23: 449–455
Worgall S, Wolff G, Falck-Pedersen E, Crystal RG (1997) Innate immune mechanisms dominate elimination of adenoviral vectors following in vivo administration. Hum Gene Ther JID – 9008950 8: 37–44
Workman P, Twentyman P, Balkwill F, Balmain A, Chaplin D, Double J, Embleton J, Newell D, Raymond R, Stables J, Stephens T, Wallace J (1998) United Kingdom Co-ordinating Committee on Cancer Research (UKCCCR) Guidelines for the Welfare of Animals in Experimental Neoplasia (Second Edition). Br J Cancer 77: 1–10
Yang Y, Jooss KU, Su Q, Ertl HC, Wilson JM (1996) Immune responses to viral antigens versus transgene product in the elimination of recombinant adenovirus-infected hepatocytes in vivo. Gene Ther 3: 137–144
Yang Y, Nunes FA, Berencsi K, Furth EE, Gonczol E, Wilson JM (1994) Cellular immunity to viral antigens limits E1-deleted adenoviruses for gene therapy. Proc Natl Acad Sci USA 91: 4407–4411
Acknowledgements
We thank Dr J Groen, PhD, from the Department of Virology of the Erasmus University Medical Centre, for his help in the virus neutralization test.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
van Etten, B., Eggermont, A., Ambagtsheer, G. et al. Impaired neutralising antibody formation and high transduction efficacy after isolated hepatic perfusion with adenoviral vectors. Br J Cancer 91, 1610–1613 (2004). https://doi.org/10.1038/sj.bjc.6602151
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bjc.6602151