Abstract
MUC1 mucin is aberrantly glycosylated and overexpressed in a number of epithelial malignancies and is therefore a promising tumour-associated antigen for target-directed immunotherapy of a panel of malignant diseases. In MUC1-positive tumours, MHC class I expession is frequently downregulated and MUC1-specific cytotoxic T cells (CTLs) are either not available or in a state of anergy allowing tumour growth without limitation by CTL control. To activate lymphocytes and natural killer (NK) cells, we here generated an anti-MUC1-scFv-IL2 fusion protein (C595scFv-Fc-IL2) that contains the C595 single-chain antibody for MUC1 binding, the human IgG1 CH2CH3 domain for protein dimerisation, and interleukin-2 (IL2) for activation of immunological effector cells. The fusion protein binds to MUC1-derived peptides and to MUC1-positive tumour cells with the same specificity as does the C595 monoclonal antibody. Bound to MUC1, the C595scFv-Fc-IL2 fusion protein stimulates proliferation of human activated lymphocytes in vitro. Upon binding to MUC1-positive MCF7 breast carcinoma cells, moreover, the fusion protein activates resting NK cells to tumour cell lysis. These properties make the C595scFv-Fc-IL2 fusion protein a suitable candidate for the immunotherapy of MUC1-positive tumours.
Similar content being viewed by others
Main
MUC1 is a high molecular weight, type 1 transmembrane mucin with >50% carbohydrates O-linked to the protein core through serine and threonine. The unique extracellular mucin domain consists of variable numbers of tandemly repeated peptides (VNTR domain), each of them made up of 20 amino-acid sequences. The VNTR domain varies in length from 20 to over 100 repeats depending on the different alleles, exhibits a sequence polymorphism, and is characterised by differentiation-dependent profiles of complex glycans that control antigenicity and immunogenicity of the mucin (Hanisch and Müller, 2000). MUC1 is expressed on the luminal surfaces of glandular epithelial cells of respiratory, gastrointestinal and genitourinary tracts as well as of pancreatic and mammary ducts. Adenocarcinomas from these organs frequently overexpress and aberrantly glycosylate MUC1 leading to the suggestion that loss of MUC1 topological restriction and increased cellular expression in cancer cells may contribute to the malignant phenotype (Hilkens et al, 1992). As MUC1 is secreted by tumour cells, determination of the levels of MUC1 antigen in the blood has been exploited as a measure of tumour burden and changing levels as a reflection of the response to therapy (Berruti et al, 1994; Martoni et al, 1995).
Patients with MUC1-positive tumours develop both humoral and cellular immune responses against determinants on the MUC1 antigen from malignant cells as measured by in vitro parameters (Jerome et al, 1991; Rughetti et al, 1993; Kotera et al, 1994; Domenech et al, 1995; Hamanaka et al, 2003). Breast and pancreatic cancer patients may spontaneously develop a specific, MHC-independent cytotoxic T-cell response against epitopes in the protein core of tumour-associated MUC1 (Jerome et al, 1991); however, MHC class I and class II restricted cellular immune reactions against MUC1 protein were observed as well (Apostolopoulos et al, 1997; Hiltbold et al, 1998; Reddish et al, 1998; Brossart et al, 1999; Pietersz et al, 2000; Heukamp et al, 2001). Although anti-MUC1 responses are frequently detected in patients with advanced and progressing adenocarcinomas (Nakamura et al, 1998), activation of immunological effector cells is obviously not sufficient to protect against tumour progression in vivo. Natural B-cell responses to lactation- or tumour-associated glycoforms of the mucin, as detected in women after pregnancy or in some cancer patients, improve survival rates, but usually do not eliminate the MUC1+ tumour cells in vivo. Accordingly, enhancement of endogenous immune responses to MUC1 by active specific immunisation based on designed MUC1 vaccines is predicted to improve long-term survival of patients with MUC1+ adenocarcinomas. Recent evidence suggests that the induction of a strong anti-MUC1 response in cancer patients may require the activation of specific T helper cells via MHC class II presented peptide and glycopeptide epitopes, a process that is controlled by site-specific O-glycosylation (Vlad et al, 2002). CD4-mediated responses generated against MUC1 apparently do not fit the type 1 or 2 model (VanLith et al, 2002), and the involvement of natural killer cells (NK cells) in MUC1-based immunity has been demonstrated. The search for immunological strategies that allow an MUC1-specific and locally restricted activation of effector cells in the vicinity of the tumour could lead to alternative therapeutical tools.
We here made use of an immunocytokine to modulate specifically and locally the immune response. The concept of immunocytokines is based on fusion proteins composed of a cytokine for the activation of immune cells and of an antibody-derived binding domain for specific targeting of the cytokine (Lode et al, 1998). Strategies based on antifolate receptor scFv or anticarcinoembryonic antigen scFv were successfully evaluated in transgenic mouse models (Melani et al, 1998; Xu et al, 2000) proving the principal of the approach as promising. A panel of antibodies were raised against the tumour-associated form of the MUC1 antigen, particularly against the protein core motif (Price et al, 1997). The anti-MUC1 monoclonal antibody (mAb) C595 reacts with the peptide motif RPAP in the repeat sequence of the protein core (Price et al, 1990). C595 mAb has been used in immunoassays for the measurement of soluble MUC1 in breast cancer patients (Price et al, 1992; Dixon et al, 1993) and for in vivo immunoscintigraphy (Symonds et al, 1992; Perkins et al, 1993). The C595 mAb has been converted into a single-chain fragment of variable regions (scFv) with retained binding specificities (Denton et al, 1997). Utilising the C595 scFv, we generated an anti-MUC1-scFv-Fc-IL2 fusion protein that after binding to MUC1-positive tumour cells induces proliferation of peripheral blood T cells and mediates activation of resting NK cells to lysis of MUC1-positive tumour cells. Results presented here suggest the C595scFv-Fc-IL2 fusion protein as suitable immunocytokine for the specific immune modulation in the vicinity of MUC1-positive tumours.
Materials and methods
Cell lines
The human mammary carcinoma cell line T-47D (HTB-133, ATCC, Rockville, MD, USA) was cultured in RPMI 1640 medium supplemented with 2 mM L-glutamine (Sigma, Deisenhofen, Germany), 0.2 U ml−1 insulin (Novo Nordisk, Mainz, Germany) and 10% (v v−1) fetal calf serum (FCS, Biochrome KG, Berlin, Germany). The human mammary carcinoma cell line MCF7 (HTB-22, ATCC) and the human renal carcinoma line 293 T expressing the SV40 large T antigen (Pear et al, 1993) were maintained in DME medium with 10% (v/v) FCS. The Hodgkin's lymphoma-derived cell line L540 (Diehl et al, 1983) was cultured in RPMI 1640 medium, 2 mM L-glutamine, 10% (v /v) FCS.
MUC1 glycoforms
Native MUC1 glycoforms were isolated from human milk fat globule membranes as described previously (Müller et al, 1997). A partially deglycosylated derivative of the lactation-associated glycoform was generated by treatment with trifluoromethane sulfonic acid for 30 min at 0°C (Müller et al, 1997).
Chemical synthesis and purification of MUC1 peptides and glycopeptides
Glycopeptides A13, A9 and H4 corresponding to MUC1 tandem repeat peptides based on the AHG21 sequences AHGVTSAPDTRPAPGSTAPPA (A13, A9) and AHGVTSAPESR PAPGSTAPAA (H4) and carrying GalNAc at Thr/Ser10 (A13, H4) or at multiple sites (refer to Table 1) were chemically synthesised according to previously published protocols (Paulsen et al, 1995) and isolated successively on preparative and analytical reversed-phase columns on an HPLC workstation (System Gold, Beckman, München, Germany). The peptides TAP25 and AHG21-AES were chemically synthesised by a local facility at the Center of Biochemistry (Medical Faculty of the University of Cologne) and isolated on a preparative C18 reversed-phase column AQ20S11153OR (150 × 30 mm, YMC Europe GmbH). TR3 (60-mer) with repetitive PAP20 sequence was a kind gift of Dr Jo Hilgers (previously at Academisch Ziekenhuis, Amsterdam, The Netherlands) and TR5 (100-mer) with repetitive GVT20 was kindly provided by Dr. Olivera Finn (Department of Immunology, University of Pittsburgh, Pittsburgh, PA, USA).
Monoclonal antibodies
C595 is a monoclonal antibody (IgG3, kappa light chain) with specificity for MUC1 urinary mucin (Price et al, 1990). The recombinant antibody fragment C595scFv was derived from the C595 antibody and is composed of the VH and VL variable regions joined via a (Gly4Ser)3 linker peptide (Denton et al, 1997).
Construction and expression of the MUC1-specific fusion proteins C595scFv-Fc and C595scFv-Fc-IL2
The cDNA encoding the human IgG1 CH2/CH3 domain (Shu et al, 1993) as well as the IL2 cDNA, derived from Jurkat cells (TIB-152, ATCC), were terminally equipped by polymerase chain reaction PCR with BamHI and XhoI restriction sites, respectively, using the following oligonucleotide primers:
hIgG-5′[5′-CTGAAGGATCCCGCCGAGCCCAAATCTCCTGACAAAACT-3′],
hIgG-Stop-3′[5′-GGCCTCGAGCTAGATCTTACCCGGAGACAGGGA-3′],
5′-hIL2,[5′-GATCAGGATCCGGTGATCAAAGCACCTACTTCAAGTTCTACA-3′],
3′-hIL2, [5′-TCAACTCGAGTCGACTCAAGTCAGTGTTGAGATGAT-3′] (restriction sites are underlined). The PCR products were ligated into the corresponding sites of the expression vector pRSV-HRS3scFv-γ that encodes a CD30-specific recombinant immunoreceptor (Hombach et al, 1998). Thereby, the FcɛRIγ signalling domain is replaced by the cDNA coding for the human IgG1 constant domain and the IL2 cDNA, respectively. The DNA encoding the single-chain antibody fragment C595scFv was flanked by PCR with nucleotide sequences containing XbaI and BamHI restriction sites (underlined), respectively, utilising the primer oligonucleotides VH5′, 5′-[GCGGCCCAGTCTAGAATGGCCCAG]-3′ and C595VL3′, 5′-[CGCACCTGGATCCGCCCGTTTCAGCTGCAG]-3′. The amplified C595 scFv DNA was subsequently inserted into the corresponding sites of pRSV-HRS3scFv-Fc DNA herewith replacing the HRS3 scFv domain. To construct the C595scFv-Fc-IL2 expression cassette, the C595scFv-Fc DNA was amplified by PCR and flanked with SnaBI and BglII restriction sites (underlined) utilising the plasmid DNA pRSV-C595scFv-Fc as template and the oligonucleotide primers Lkappa-5′ [5′-CTACGTACCATGGATTTTCAGGTGCAGATTTTC-3′] and hIgG1-3′(BglII) [5′-CCCACCCAGATCTTTTTTACCCGGAGACAGGGAGAGGCTCTTCTG-3′]. The PCR product was ligated into the vector construct pRSV-HRS3scFvIL2 replacing the HRS3scFv binding domain. For expression of the recombinant anti-MUC1 fusion proteins, 293 T cells were transfected by calcium phosphate techniques with 10–20 μg of the plasmid DNA pRSV-C595scFv-Fc and pRSV-C595scFvFc-IL2, respectively. After 48–72 h the cell culture supernatants were harvested and analysed for the presence of the fusion proteins.
ELISA to detect the anti-MUC1 fusion proteins
Serial dilutions of the cell culture supernatant of transfected 293 T cells were incubated in microtitre plates coated with an anti-human IgG antibody (1 μg ml−1, Southern Biotechnology, Birmingham, AL, USA). Bound fusion proteins were detected by a biotinylated anti-human IgG antibody (0.125 μg ml−1, Southern Biotechnology) or, alternatively, by a biotin-labelled anti-human IL2 antibody (0.5 μg ml−1, BD Biosciences/PharMingen). The assays were developed by means of a streptavidin-coupled peroxidase and ABTS substrate (both Roche Diagnostics, Mahnheim, Germany).
Sodium dodecyl sulphate–polyacrylamide gel electrophoresis and Western blot analysis
The cell culture supernatant of transfected 293 T cells was electrophoretically separated by sodium dodecylsulphate polyacrylamide gel electrophoresis (SDS–PAGE) and blotted onto nitrocellulose membrane. The membrane was blocked with Roti®-Block (Roth GmbH, Karlsruhe, Germany) containing 5% milk powder and subsequently incubated with a horseradish peroxidase (HRP)-conjugated rabbit anti-human IgG antibody (1 : 20 000, Dako, Hamburg, Germany) or with a mouse anti-human IL2 antibody (1 : 250, Serotec, Düsseldorf, Germany), followed by incubation with a rabbit anti-mouse IgG-HRP conjugate (1 : 20 000, Dako), respectively. The blots were developed by means of the ECL™ detection reagent (Amersham Pharmacia Biotech, Freiburg, Germany).
Antigen-binding assays
Binding of the C595scFv-Fc and C595scFv-Fc-IL2 fusion proteins was monitored by ELISA using partially deglycosylated MUC1 from human milk fat membranes (Müller et al, 1997) as well as a set of synthetic peptides and glycopeptides (Table 1).
Microtitre plates (maxi-sorp, Nunc, Roskilde, Denmark) were coated with the peptide antigens (10 μg ml−1), partially deglycosylated MUC1 from human milk (100 μg ml−1), BSM (100 μg ml−1) and for control reason with an anti-human IgG antibody and an anti-mouse IgG1 antibody, respectively (both 1 μg ml−1, Southern Biotechnology). After blocking the microtitre plates were incubated with cell culture supernatants containing the fusion proteins C595scFvFc and C595scFv-Fc-IL2, respectively, with the monoclonal antibody C595 (250 ng ml−1), and for control with a murine IgG1 monoclonal antibody (250 ng ml−1, Sigma). Bound fusion proteins and antibodies were detected with biotin-labelled anti-isotypic goat anti-human IgG and goat anti-mouse IgG antibody (both 125 ng ml−1, Southern Biotechnology). The assays were developed by means of a streptavidin-coupled peroxidase and ABTS substrate (both Roche Diagnostics).
To compare the antigen-binding capacity of the fusion proteins C595scFv-Fc and C595scFv-Fc-IL2, respectively, with that of the parental mAb C595, microtitre plates (maxi-sorp, Nunc) were coated with the peptide antigen TR5 (2.5 μg ml−1), blocked and subsequently incubated with serial dilutions of cell culture supernatants containing the fusion proteins C595scFv-Fc and C595scFv-Fc-IL2, respectively, and dilutions of the parental mAb C595. The fusion proteins and the mAb bound to the microtitre plates were detected by biotin-labelled secondary antibodies as described above. Dilutions of supernatants and antibody resulting in half-maximal absorbance at 405 nm were applied to plates with immobilised TR5 antigen (2.5 μg ml−1). Binding was assayed in the presence of increasing concentrations of soluble TR5 antigen (up to 20 μg ml−1). The percentage of binding inhibition was calculated as follows:

Immunofluorescence and flow cytometry
Immunofluorescence assays were performed by incubation of T-47D cells (MUC1+/CD25−), 293 T cells (MUC1−/CD25−) and L540 cells (MUC1−/CD25+) with cell culture supernatant of transfected 293 T cells containing the fusion protein C595scFv-Fc and C595scFv-Fc-IL2, respectively, and as control with supernatant of mock-transfected 293 T cells. Alternatively, fusion proteins were incubated with resting peripheral blood lymphocytes (PBL) or lymphocytes activated with IL2 (400 U ml−1) and anti-CD3 antibody OKT3 (100 ng ml−1). Bound fusion proteins were detected by an FITC-labelled F(ab′)2 anti-human IgG antibody (2 μg ml−1, Southern Biotechnology). The IL2 receptor (α-chain) was detected by incubation of PBL with an FITC-conjugated anti-CD25 antibody (clone B1.49.9, Coulter-Immunotech Diagnostics, Hamburg, Germany). Immunofluorescence assays were analysed utilising a FACScan™ cytofluorometer equipped with the Cellquest™ analysis software (Becton Dickinson, Mountain View, CA, USA).
Proliferation assays
Peripheral blood lymphocytes from healthy donors were isolated from peripheral blood by density centrifugation and cultured for 24 to 48 h in RPMI 1640 medium supplemented with 10% (v /v) FCS, IL2 (400 U ml−1), and anti-CD3 mAb OKT3 (100 ng ml−1). Activated lymphocytes were washed twice and cultured for additional 48 h in RPMI 1640 medium containing 10% (v /v) FCS, IL2 (400 U ml−1). Peripheral blood lymphocytes were washed twice and cultured for 3 h in the absence of IL2. Subsequently 2.5 × 105 PBL per well were cultured in the presence of serial dilutions of cell culture supernatant containing the fusion proteins C595scFv-Fc-IL2 or C595scFv-Fc and for control IL2 (2000 U ml−1), respectively. After 72 h, lymphocyte proliferation was quantified by means of the ‘XTT cell proliferation kit’ (Roche Diagnostics) according to the manufacturer's recommendations.
Alternatively, activated PBL were cultured in the presence of fusion protein bound to immobilised antigen. Microtitre plates (maxi-sorp, Nunc) were coated with increasing amounts of MUC1 antigen, TR5 glycopeptide, and asialo-BSM, respectively (up to 100 μg ml−1). After blocking, the coated wells were incubated with cell culture supernatants containing the fusion proteins C595scFv-Fc and C595scFv-Fc-IL2. The plates were washed three times with PBS and lymphocytes (2.5 × 105 per well) were added. After culture for 72 h, proliferation was monitored utilising ‘XTT cell proliferation kit’ (Roche Diagnostics).
Alternatively, polystyrene-coated ferric oxide beads M-280 (tosylated, Dynal, Hamburg, Germany) were covalently coated with TR5 peptide antigen and for control reason with human serum albumin (following the manufacturer's recommendations). The beads were incubated with cell culture supernatants of transfected 293 T cells containing the fusion proteins C595scFv-Fc and C595scFv-Fc-IL2, respectively, and supernatant of untransfected 293 T cells. Specific binding of the fusion proteins to TR5-coated beads was monitored by flow cytometry utilising a FITC-labelled F(ab')2 anti-human IgG antibody (2 μg ml−1, Southern Biotechnology). After three times of washing, serial dilutions of coated beads were seeded onto 96-well microtiter plates (15±105–0.6±105 beads/well) and activated lymphocytes (2 × 105 cells–well) were added. After 72 h, proliferation was determined as described.
Cytotoxicity assay
Tumour cell viability was monitored by an XTT-based colorimetric assay according to Jost et al. (1992). Briefly, PBL from healthy donors were isolated by density centrifugation and NK cells were negatively enriched by magnetic activated cell sorting (MACS) utilising the ‘NK Cell Isolation Kit’ (Miltenyi Biotec, Bergisch Gladbach, Germany). MUC-1-positive MCF7 cells or T47D cells were incubated with cell culture supernatants containing C595scFv-Fc and C595scFv-Fc-IL2 fusion protein, respectively, and for control with medium with and without IL2 (400 U ml−1). After four times of washing, coated target cells were seeded onto round-bottomed microtiter plates (5 × 104 cells per well) together with resting NK cells (1 × 105 per well). In a second set of experiments, untreated tumour cells (5 × 104 per well) were cocultured with NK cells (1 × 105 per well) in the presence of the soluble fusion protein C595scFv-Fc-IL2 and IL2 (400 U ml−1), respectively. After 48 h, the XTT reagent (1 mg ml−1, ‘Cell Proliferation Kit II’, Roche Diagnostics) was added to the cells and incubated for 60–90 min at 37°C. Metabolisation of XTT to a formazan was monitored colorimetrically at an adsorbance wavelength of 450 nm and a reference wavelength of 650 nm. Maximal reduction of XTT was determined as the mean of three wells containing tumor cells only, and background was determined as the mean of three wells containing RPMI 1640 medium, 10% (v v−1) FCS. The formation of formazan due to the effector cells was determined from triplicate wells containing NK cells only. The percentage of viable tumour cells was calculated as follows:

Results
Expression of the recombinant fusion proteins C595scFv-Fc and C595scFv-Fc-IL2
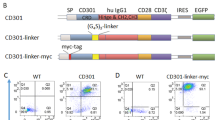
We generated the expression constructs pRSV-C595scFv-Fc and pRSV-C595scFv-Fc-IL2 that code for fusion proteins consisting of the anti-MUC1 scFv C595 and the human IgG1 CH2CH3 domain (Fc domain) with or without linked IL2, respectively (Figure 1). After transient transfection, 293 T cells secrete the fusion proteins into the cell culture medium as monitored by ELISA (Figure 2). Whereas both proteins are captured by the anti-human IgG antibody directed against the Fc domain of the fusion proteins, only the C595scFv-Fc-IL2 immunocytokine is detected by the anti-human IL2 antibody. Western blot analysis revealed that the C595scFv-Fc fusion protein migrates at about 120 kDa and the C595scFv-Fc-IL2 fusion protein at about 150 kDa under nonreducing conditions (Figure 3A) corresponding to the homodimeric forms of the respective fusion proteins. Western blot analysis moreover confirmed the IL2 cytokine as part of the C595scFv-Fc-IL2 fusion protein (Figure 3B).
Expression cassettes coding for the recombinant anti-MUC1 fusion proteins C595scFv-Fc and C595scFv-Fc-IL2. The expression cassettes were generated as described in Materials and Methods. Lk: leader sequence of the Ig κ chain; C595scFv: anti-MUC1 scFv; Fc: IgG1 CH2CH3. The expression cassettes are driven by the RSV LTR.
Detection of the fusion proteins C595scFv-Fc and C595scFv-Fc-IL2 in the supernatants of transfected 293 T cells. Serial dilutions of culture supernatants from 293 T cells transfected with pRSV-C595scFv-Fc (▪), pRSV-C595scFv-Fc-IL2 (•) and, as control, from mock-transfected cells (*), respectively, were incubated in microtitre plates coated with an anti-human IgG antibody. Bound fusion proteins were detected by a biotin-labelled anti-human IgG (A) or anti-human IL2 (B) antibody.
The fusion proteins C595scFv-Fc and C595scFv-Fc-IL2 are expressed as homodimers. Cell culture supernatants from 293 T cells transfected with pRSV-C595scFv-Fc DNA (lane 1) or with pRSV-C595scFv-Fc-IL2 DNA (lane 2) as well as recombinant human IL2 (1000 U, lane 3) were electrophoretically separated under nonreducing conditions, blotted onto nitrocellulose membrane and probed with an anti-human IgG antibody (A) and an anti-human IL2 antibody (B). The calculated molecular weight of the monomeric form of the fusion protein C595scFv-Fc is 60 kDa, of the C595scFv-Fc-IL2 protein is 75 kDa.
Fusion proteins bind specifically to MUC1
The fusion proteins C595scFv-Fc and C595scFv-Fc-IL2 and the mAb C595 were tested by ELISA for binding to partially deglycosylated MUC1 antigen from human milk fat membranes as well as to a set of MUC1 glycopeptides corresponding to parts of the repeat domain and containing the RPAP motif (Table 1). As shown in Figure 4, the binding patterns of the fusion proteins to the panel of MUC1-derived antigens are similar to that of the monoclonal antibody C595 indicating that the C595 scFv domain in the fusion proteins conserved the antigen-binding profile of the parental C595 mAb. The profile is characterised by (i) binding to DTRPAP-containing repeat peptides (Table 1), (ii) no cross-reactivity to ESRPAP-containing repeat peptides (AHG21-AES, H4), which represent a known sequence polymorphism in the tandem repeat domain of the mucin (Hanisch and Müller, 2000; Engelmann et al, 2001, iii) stronger binding to oligorepeats (TR3 and TR5) and native MUC1 (MUC1deglyco) than to monorepeats (TAP25), and (iv) inhibition of antibody binding due to O-glycosylation of the peptides (A13, A11, A9).
Antigen binding profile of the recombinant fusion proteins C595scFv-Fc and C595scFv-Fc-IL2. Microtitre plates were coated with a set of MUC1-related (glyco-) peptides (10 μg ml−1) corresponding to mono- and oligorepeats and containing the RPAP motif (see Table 1), partially deglycosylated MUC1 antigen (100 μg ml−1), and, as control, BSM (100 μg ml−1), an anti-human IgG antibody (1 μg ml−1) and an anti-mouse IgG antibody (1 μg ml−1), respectively. The coated wells were incubated with cell culture supernatants containing the fusion proteins C595scFv-Fc (A) and C595scFv-Fc-IL2 (B), respectively, and as control with the mAb C595 (C) and a mouse IgG1 control antibody (D) (both 0.25 μg ml−1). Bound fusion proteins and antibodies were detected by a biotin-labelled anti-human IgG mAb (A and B) or a biotin labelled anti-mouse IgG mAb (C and D). The assay was performed in triplicate; data are presented as the mean±s.e.m.
We furthermore compared the binding properties of the recombinant proteins C595scFv-Fc and C595scFv-Fc-IL2, respectively, to that of the mAb C595 by competition assays utilising dilutions of the fusion proteins and of mAb C595, respectively, that lead to half-maximal binding. Binding to immobilised TR5 peptide was assayed in the presence of increasing amounts of soluble TR5 peptide. As summarised in Figure 5, binding of both fusion proteins C595scFv-Fc and C595scFv-Fc-IL2 is titrated out by increasing concentrations of soluble TR5 peptide. The apparent antigen-binding affinities of the recombinant fusion proteins, however, are reduced by a factor of 2–3 compared to that of the mAb C595 in this assay.
Binding-inhibition assay. Microtitre plates coated with the peptide antigen TR5 (2.5 μg ml−1) were incubated with dilutions of C595scFv-Fc (•), C595scFv-Fc-IL2 (▪), and C595 mAb (▴), respectively, that result in half-maximal binding. The binding to immobilized TR5 antigen was specifically competed by addition of increasing amounts of soluble TR5 antigen. Bound fusion proteins were detected by the biotin-labelled anti-human IgG antibody; bound C595 mAb was detected by the biotinylated anti-mouse IgG antibody. The percentage of inhibition was determined as described in ‘Material and Methods’.
The fusion proteins were furthermore assayed by flow cytometry for binding to MUC1-expressing tumour cells. As demonstrated in Figure 6A, both fusion proteins C595scFv-Fc and C595scFv-Fc-IL2 bind to cells of the MUC1-positive line T-47D but not to cells of the MUC1-negative 293 T line. The fusion proteins bind to polystyrene ferric oxide beads coated with TR5 peptide, but do not bind to beads coated with human serum albumin as control. C595scFv-Fc-IL2 protein, moreover, binds to the IL2 receptor (CD25) constitutively expressed on the surface of MUC1-negative L540 cells. Binding of C595scFv-Fc-IL2 to the IL2 receptor is specific because (i) the C595scFv-Fc fusion protein that lacks the IL2 domain does not bind to MUC1− CD25+ L540 cells (Figure 6A), and (ii) C595scFv-Fc-IL2 binds to activated lymphocytes with increased CD25 expression after stimulation with the anti-CD3 antibody OKT3 plus IL2, but does not bind to resting lymphocytes that do not express the IL2 receptor (Figure 6B). As control, the C595scFv-Fc protein without IL2 domain does not bind to resting lymphocytes, but binds weakly via the C595 scFv domain to activated T cells that express Muc1 (Agrawal et al, 1998). Taken together, the fusion proteins C595scFv-Fc and C595scFv-Fc-IL2 specifically bind to MUC1-positive tumour cells via the anti-MUC1 scFv domain, the C595scFv-Fc-IL2 protein binds in addition via IL2 to CD25+, activated lymphocytes in vitro.
Fusion proteins C595scFv-Fc and C595scFv-Fc-IL2 bind specifically to MUC1 positive tumour cells and TR5 peptide-coated beads. Cell culture supernatants from transfected 293 T cells containing the C595scFv-Fc and C595scFv-Fc-IL2 fusion protein (thick lines), respectively, and, as control, supernatant from 293 T cells transfected with an irrelevant DNA (thin lines), were incubated (A) with T-47D cells (MUC1+/CD25−), 293 T cells (MUC1−/CD25−), L540 cells (MUC1−/CD25+), TR5 peptide-coated beads or, as control, with human serum albumin-coated beads, and (B) with quiescent lymphocytes from the peripheral blood (PBL) or with PBL activated by preincubation with the anti-CD3 mAb OKT3 plus IL2. Bound fusion proteins were detected by an FITC-labelled anti-human IgG antibody. Expression of the IL2 receptor CD25 was monitored by incubation with a FITC-conjugated anti-CD25 mAb (anti-CD25).
C595scFv-Fc-IL2 fusion protein induces proliferation of activated lymphocytes
We assessed the IL2 bioactivity of the C595scFv-Fc-IL2 fusion protein by monitoring the induction of proliferation of activated lymphocytes. As shown in Figure 7 the C595scFv-Fc-IL2 protein stimulates proliferation of activated lymphocytes in a dose-dependent manner, whereas the C595scFv-Fc protein that lacks the IL2 domain does not. Incubation of activated lymphocytes with IL2 served as control. Resting T cells, in contrast, are not activated to proliferate in the presence of the C595scFv-Fc-IL2 fusion protein (data not shown).
Activated lymphocytes proliferate in the presence of soluble C595scFv-Fc-IL2 fusion protein. Lymphocytes from the peripheral blood (2.5 × 105 cells per well) were activated by incubation with the anti-CD3 mAb OKT3 plus IL2 and cultured in the presence of cell culture supernatants containing the fusion proteins C595scFv-Fc-IL2 (•), C595scFv-Fc (▪), and as control IL2 (▴) (2 000 U ml−1), respectively. After 72 h, lymphocyte proliferation was quantified by means of the ‘XTT cell proliferation kit’ (Roche Diagnostics). The assays were performed in triplicate; data are presented as mean±s.e.m.
To assay whether the C595scFv-Fc-IL2 fusion protein retains its IL2 bioactivity after binding to MUC1 antigen, we incubated C595scFv-Fc-IL2 protein, and C595scFv-Fc protein as control, on plastic surfaces coated with MUC1 or TR5 peptide, respectively. Bound to MUC1 and TR5 antigen, respectively, the C595scFv-Fc-IL2 protein stimulates proliferation of activated lymphocytes in a dose-dependent manner, whereas no lymphocyte proliferation was detected in the presence of the bound C595scFv-Fc fusion protein (Figure 8A, B). As control, plates coated with asialo-BSM and incubated with the C595scFv-Fc-IL2 fusion protein did not induce proliferation of activated lymphocytes (Figure 8C).
C595scFv-Fc-IL2 fusion protein bound to MUC1 antigen stimulates proliferation of activated lymphocytes. Micotitre immunoplates were coated with increasing amounts of deglycosylated MUC1 (A), TR5 peptide (B), and asialo-BSM (C), respectively, and subsequently incubated with cell culture supernatants containing the fusion proteins C595scFv-Fc (▪) and C595scFv-Fc-IL2 (•), respectively. After extensive washing, activated lymphocytes (2.5 × 105 per well) were incubated in coated plates for 72 h. In a second set of experiments, beads coated with TR5 peptide antigen (D) and, as control, coated with human serum albumin (E) were incubated with culture supernatant containing the fusion protein C595scFv-Fc or C595scFv-Fc-IL2, respectively, washed extensively and incubated in serial dilutions (15 × 105–0.6 × 105 beads per well) with activated lymphocytes (2.5 × 105 per well). After 72 h, lymphocyte proliferation was quantified by means of the ‘XTT cell proliferation kit’. The assays were performed in triplicate; data are presented as the mean±s.e.m.
In a second assay, tosylated ferric oxide beads were coated with TR5 peptide, or with human serum albumin as a control, and subsequently incubated with the fusion proteins C595scFv-Fc-IL2 and C595scFv-Fc, respectively. Binding of the fusion proteins on TR5-coated beads was confirmed by FACS analysis (Figure 6A). As summarised in Figure 8D, C595scFv-Fc-IL2 fusion protein bound to TR5-coated beads stimulates proliferation of activated lymphocytes in a dose-dependent manner, whereas C595scFv-Fc control protein does not. As control, beads coated with human serum albumin and incubated with the fusion proteins did not induce proliferation of activated lymphocytes (Figure 8E).
C595scFv-Fc-IL2 fusion protein induces resting NK cells to lysis of MUC1-positive tumour cells
We assayed the bioactivitiy of the C595scFv-Fc-IL2 fusion protein bound to MUC1-positive target cells by monitoring the activation of resting NK cells to lyse target cells. MUC1-positive MCF7 tumour cells were incubated with C595scFv-Fc-IL2 fusion protein and IL2, respectively, and cocultured with resting NK cells. Tumour cell viability was monitored by an XTT-based colorimetric assay. As shown in Figure 9A, C595scFv-Fc-IL2 protein induced resting NK cells to lysis of MCF7 cells as does IL2 indicating that the fusion protein is capable to activate resting NK cells.
The fusion protein C595scFv-Fc-IL2 activates resting NK cells to tumour cell lysis (A). MCF7 cells (MUC1+) (5 × 104 cells per well) were cocultured with resting NK cells (1x105 cells per well) in the presence of C595scFv-Fc-IL2 fusion protein or IL2 (400 U ml−1). As control, MCF7 cells were cocultured with NK cells in cell culture medium without additives. (B) MCF7 and T-47D tumour cells (MUC1+) were preincubated with cell culture supernatants containing C595scFv-Fc, C595scFv-Fc-IL2, or IL2 (400 U ml−1), respectively. After four rounds of washings, cells were seeded into round-bottom microtiter plates (5 × 104 cells per well) and cocultured with resting NK cells (1 × 105 cells per well). The viability of MCF7 and T-47D cells was determined by an XTT-based viability assay as described in Material and Methods. The assays were performed in triplicate; data are presented as the mean±s.e.m. Statistical significance was determined utilising Student's t-test.
In a second assay, MCF7 cells were preincubated with C595scFv-Fc-IL2, C595scFv-Fc, and IL2 as control, respectively, washed intensively, and subsequently coincubated with resting NK cells. As shown in Figure 9B, MCF7 cells coated with C595scFv-Fc-IL2 protein were significantly lysed by NK cells compared to preincubation with C595scFv-Fc protein without the IL2 domain. Soluble IL2 not bound to MCF7 cells and washed out did not induce NK-cell-mediated cytolysis indicating that soluble IL2 is substantially eliminated by repeated washings prior to coincubation with NK cells. Essentially, the same results were obtained when using Muc1+ T-47D cells in the assay (Figure 9B). This set of experiments demonstrates that the C595scFv-Fc-IL2 fusion protein bound to MUC1-positive tumour cells activates resting NK cells to tumour cell lysis.
Discussion
The purpose of this study was to engineer a novel immunotherapeutic reagent that is directed to MUC1-positive tumour cells and activates effector responses of NK cells. Activation of resting NK cells in particular is expected to be of significance considering recent evidences that NK cells may contribute to MUC1 immunity and that the MUC1 directed immune response does not fit the type 1 or type 2 model (VanLith et al, 2002). In the light of these findings the insufficient outcomes of multiple efforts to stimulate an MUC1-specific CD4+ or CD8+ T-cell response may find an explanation.
The anti-MUC1 scFv-Fc-IL2 fusion protein harbours the C595 scFv domain for targeting IL2 to MUC1-positive tumours. C595 scFv represents, to our best knowledge, the only example of a successful attempt to generate high-affinity anti-DTR MUC1-specific scFv from phage libraries or from established hybridoma clones. This antibody defines a peptide motif more upstream of the DTR sequence (RPAP). We here demonstrate that the conservative replacement of Asp-Thr within the sequence PDTRPAP by Glu-Ser has a severe negative impact on the binding of both, the parental antibody C595 and the scFv-Fc-IL2 fusion protein, which indicates a contribution of these two residues to the epitope structure of the C595 antibody. The replacement of DT by ES represents a sequence polymorphism found with a high incidence in all repeat domains of human MUC1, which were analysed on the level of genomic DNA (Engelmann et al, 2001). The C595 scFv binds to a panel of mammary and bladder carcinoma biopsies but not to benign tissues like breast ducts (Denton et al, 1997) making the scFv suitable for specific tumour cell binding.
The C595scFv-Fc-IL2 fusion protein is expressed as homodimer (cf. Figure 3) that is likely to be formed by disulphide bonds between the IgG1 Fc domains incorporated into the fusion protein between the scFv and IL2 moiety. Utilising a panel of MUC1 mucins and peptides, we here demonstrate that the C595scFv-Fc-IL2 fusion protein exhibits the same binding specificity as the C595 mAb (Figure 4), however, with slightly reduced avidity compared to that of the mAb C595 (Figure 5). The C595scFv-Fc-IL2 fusion protein binds specifically to the IL2 receptor on activated lymphocytes, but not to resting lymphocytes that do not express the IL2 receptor (Figure 6B). C595scFv-Fc weakly binds to activated lymphocytes, most likely via the C595scFv domain to Muc1 expressed on activated T cells (Agrawal et al, 1998). Although C595scFv-Fc-IL2 binds much stronger to activated lymphocytes via CD25, binding to activated T cells and dendritic cells via Muc1 cannot be excluded. Noteworthy, binding to resting T cells was not observed (cf. Figure 6B).
C595scFv-Fc-IL2 fusion protein stimulates proliferation of activated lymphocytes from the peripheral blood in a dose-dependent manner, whereas the C595scFv-Fc protein that lacks the IL2 domain does not. The IL2 activity of the fusion protein to induce proliferation of activated T cells is still conserved after binding to MUC1 mucin (cf. Figure 8). Resting T cells that do not express the IL2 receptor (CD25) are not activated by the fusion protein. Resting NK cells, in contrast, are activated by the C595scFv-Fc-IL2 fusion protein to tumour cell lysis (cf. Figure 9). These results are of major significance because (i) the fusion protein is designed to act locally in the near vicinity of the tumour after binding to MUC1-positive tumour cells and (ii) the fusion protein activates resting NK cells and preactivated T cells thereby recruiting both compartments of the cellular immune response. Noteworthy, resting T cells are not activated thereby avoiding an immune response of T cells that are not activated in the tumour environment and may be of nontumour-related specificities (not shown).
Strategies during the last years to improve the cellular immune responses against MUC1 protein include: (i) conjugation of MUC1 peptides with KLH or mannan (Karanikas et al, 1997; Gilewski et al, 2000, ii) coexpression of MUC1 with CD80 (B7.1) in tumour cells to provide costimulatory signals to the immune system (Smith et al, 1999, iii) fusing MUC1-positive tumour cells with antigen-presenting cells or pulsing dendritic cells with MUC1-derived peptides (Brossart et al, 2000; Gong et al, 2000, iv) application of MUC1 together with Th1 cytokines (Acres et al, 2000; Carr-Brendel et al, 2000; Lees et al, 2000; Mukherjee et al, 2003), and (v) use of a BCG-MUC1-IL2 fusion protein (He et al, 2002). The latter fusion protein consists of the BCG antigen signal sequence, the MUC1 VNTR core peptide, and IL2. Immunisation of SCID/hu-PBL mice with the fusion protein resulted in increased MUC1-specific cellular immunity suggesting that combined application of MUC1 peptide and IL2 may mediate an effective immunity against MUC1-positive cancer. As far as clinical studies were performed on the basis of the above-cited approaches, the outcomes were insufficient in terms of the strength and longevity of the cellular immune responses. On the other hand, passive transfer of MUC1-specific antibodies did not affect the growth of MUC1 expressing, experimentally transplanted melanomas in a mouse model (Tempero et al, 1999). In this model, CD4+ T cells were critical for rejection of MUC1-positive tumours (Tempero et al, 1998; VanLith et al, 2002), whereas other studies suggest that CD8+ T cells are required for MUC1-specific immunity against MUC1-positive pancreatic carcinoma (Morikane et al, 2001).
Although in vitro detection of cytolytic activity does not always correlate with in vivo tumour rejection, the potential of the C595scFv-Fc-IL2 fusion protein to activate immunocompetent resting NK and preactivated T cells after binding to MUC1-positive tumour cells is clearly demonstrated. Suppressive effects of the tumour environment, including locally accumulated suppressive cytokines, and other stromal elements may additionally modulate the efficacy of the fusion protein in vivo. The fusion protein, however, provides a specific tool to increase stimulatory signals to both activated T and resting NK cells in the vicinity of MUC1-positive tumour cells in order to improve the antitumour immune response.
Change history
16 November 2011
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Acres B, Apostolopoulos V, Balloul JM, Wreschner D, Xing PX, Ali-Hadji D, Bizouarne N, Kieny MP, McKenzie IF (2000) MUC1-specific immune responses in human MUC1 transgenic mice immunized with various human MUC1 vaccines. Cancer Immunol Immunother 48: 588–594
Agrawal B, Krantz MJ, Parker J, Longenecker BM (1998) Expression of Muc1 mucin on activated human T cells: implications for a role of muc1 in normal immune regulation. Cancer Res 58: 4079–4081
Apostolopoulos V, Karanikas V, Haurum JS, McKenzie IF (1997) Induction of HLA-A2-restricted CTLs to the mucin 1 human breast cancer antigen. J Immunol 159: 5211–5218
Berruti A, Tampellini M, Torta M, Buniva T, Gorzegno G, Dogliotti L (1994) Prognostic value in predicting overall survival of two mucinous markers: CA 15-3 and CA 125 in breast cancer patients at first relapse of disease. Eur J Cancer 30A: 2082–2084
Brossart P, Heinrich KS, Stuhler G, Behnke L, Reichardt VL, Stevanovic S, Muhm A, Rammensee HG, Kanz L, Brugger W (1999) Identification of HLA-A2-restricted T-cell epitopes derived from the MUC1 tumor antigen for broadly applicable vaccine therapies. Blood 93: 4309–4317
Brossart P, Wirths S, Stuhler G, Reichardt VL, Kanz L, Brugger W (2000) Induction of cytotoxic T-lymphocyte responses in vivo after vaccinations with peptide-pulsed dendritic cells. Blood 96: 3102–3108
Carr-Brendel V, Markovic D, Ferrer K, Smith M, Taylor-Papadimitriou J, Cohen EP (2000) Immunity to murine breast cancer cells modified to express MUC-1, a human breast cancer antigen, in transgenic mice tolerant to human MUC-1. Cancer Res 60: 2435–2443
Denton G, Sekowski M, Spencer DI, Hughes OD, Murray A, Denley H, Tendler SJ, Price MR (1997) Production and characterization of a recombinant anti-MUC1 scFv reactive with human carcinomas. Br J Cancer 76: 614–621
Diehl V, Burrichter H, Schaadt M, Kirchner HH, Fonatsch C, Stein H, Gerdes J, Heit W, Ziegler A (1983) Hodgkin's cell lines: characteristics and possible pathogenetic implications. Hematol Oncol 1: 139–147
Dixon AR, Price MR, Hand CW, Sibley PE, Selby C, Blamey RW (1993) Epithelial mucin core antigen (EMCA) in assessing therapeutic response in advanced breast cancer – a comparison with CA15.3. Br J Cancer 68: 947–949
Domenech N, Henderson RA, Finn OJ (1995) Identification of an HLA-A11-restricted epitope from the tandem repeat domain of the epithelial tumor antigen mucin. J Immunol 155: 4766–4774
Engelmann K, Baldus SE, Hanisch F-G (2001) Identification and topology of variant sequences within individual repeat domains of the human epithelial tumor mucin MUC1. J Biol Chem 276: 27764–27769
Gilewski T, Adluri S, Ragupathi G, Zhang S, Yao TJ, Panageas K, Moynahan M, Houghton A, Norton L, Livingston PO (2000) Vaccination of high-risk breast cancer patients with mucin-1 (MUC1) keyhole limpet hemocyanin conjugate plus QS-21. Clin Cancer Res 6: 1693–1701
Gong J, Avigan D, Chen D, Wu Z, Koido S, Kashiwaba M, Kufe D (2000) Activation of antitumor cytotoxic T lymphocytes by fusions of human dendritic cells and breast carcinoma cells. Proc Natl Acad Sci USA 97: 2715–2718
Hamanaka Y, Suehiro Y, Fukui M, Shikichi K, Imai K, Hinoda Y (2003) Circulating anti-MUC1 IgG antibodies as a favorable prognostic factor for pancreatic cancer. Int J Cancer 103: 97–100
Hanisch FG, Muller S (2000) MUC1: the polymorphic appearance of a human mucin. Glycobiology 10: 439–449
He J, Shen D, O'Donnell MA, Chang HR (2002) Induction of MUC1-specific cellular immunity by a recombinant BCG expressing human MUC1 and secreting IL2. Int J Oncol 20: 1305–1311
Heukamp LC, van der Burg SH, Drijfhout JW, Melief CJ, Taylor-Papadimitriou J, Offringa R (2001) Identification of three non-VNTR MUC1-derived HLA-A*0201-restricted T-cell epitopes that induce protective anti-tumor immunity in HLA-A2/K(b)-transgenic mice. Int J Cancer 91: 385–392
Hilkens J, Ligtenberg MJ, Vos HL, Litvinov SV (1992) Cell membrane-associated mucins and their adhesion-modulating property. Trends Biochem Sci 17: 359–363
Hiltbold EM, Ciborowski P, Finn OJ (1998) Naturally processed class II epitope from the tumor antigen MUC1 primes human CD4+ T cells. Cancer Res 58: 5066–5070
Hombach A, Heuser C, Sircar R, Tillmann T, Diehl V, Pohl C, Abken H (1998) An anti-CD30 chimeric receptor that mediates CD3-zeta-independent T-cell activation against Hodgkin's lymphoma cells in the presence of soluble CD30. Cancer Res 58: 1116–1119
Jerome KR, Barnd DL, Bendt KM, Boyer CM, Taylor-Papadimitriou J, McKenzie IF, Bast Jr RC, Finn OJ (1991) Cytotoxic T-lymphocytes derived from patients with breast adenocarcinoma recognize an epitope present on the protein core of a mucin molecule preferentially expressed by malignant cells. Cancer Res 51: 2908–2916
Jost LM, Kirkwood JM, Whiteside TL (1992) Improved short- and long-term XTT-based colorimetric cellular cytotoxicity assay for melanoma and other tumor cells. J Immunol Methods 147: 153–165
Karanikas V, Hwang LA, Pearson J, Ong CS, Apostolopoulos V, Vaughan H, Xing PX, Jamieson G, Pietersz G, Tait B, Broadbent R, Thynne G, McKenzie IF (1997) Antibody and T cell responses of patients with adenocarcinoma immunized with mannan–MUC1 fusion protein. J Clin Invest 100: 2783–2792
Kotera Y, Fontenot JD, Pecher G, Metzgar RS, Finn OJ (1994) Humoral immunity against a tandem repeat epitope of human mucin MUC-1 in sera from breast, pancreatic, and colon cancer patients. Cancer Res 54: 2856–2860
Lees CJ, Apostolopoulos V, Acres B, Ramshaw I, Ramsay A, Ong CS, McKenzie IF (2000) Immunotherapy with mannan-MUC1 and IL-12 in MUC1 transgenic mice. Vaccine 19: 158–162
Lode HN, Xiang R, Becker JC, Gillies SD, Reisfeld RA (1998) Immunocytokines: a promising approach to cancer immunotherapy. Pharmacol Ther 80: 277–292
Martoni A, Zamagni C, Bellanova B, Zanichelli L, Vecchi F, Cacciari N, Strocchi E, Pannuti F (1995) CEA, MCA, CA 15.3 and CA 549 and their combinations in expressing and monitoring metastatic breast cancer: a prospective comparative study. Eur J Cancer 31A: 1615–1621
Melani C, Figini M, Nicosia D, Luison E, Ramakrishna V, Casorati G, Parmiani G, Eshhar Z, Canevari S, Colombo MP (1998) Targeting of interleukin 2 to human ovarian carcinoma by fusion with a single-chain Fv of antifolate receptor antibody. Cancer Res 58: 4146–4154
Morikane K, Tempero R, Sivinski CL, Kitajima S, Gendler SJ, Hollingsworth MA (2001) Influence of organ site and tumor cell type on MUC1-specific tumor immunity. Int Immunol 13: 233–240
Mukherjee P, Madsen CS, Ginardi AR, Tinder TL, Jacobs F, Parker J, Agrawal B, Longenecker BM, Gendler SJ (2003) Mucin 1-specific immunotherapy in a mouse model of spontaneous breast cancer. J Immunother 26: 47–62
Muller S, Goletz S, Packer N, Gooley A, Lawson AM, Hanisch FG (1997) Localization of O-glycosylation sites on glycopeptide fragments from lactation-associated MUC1. All putative sites within the tandem repeat are glycosylation targets in vivo. J Biol Chem 272: 24780–24793
Nakamura H, Hinoda Y, Nakagawa N, Makiguchi Y, Itoh F, Endo T, Imai K (1998) Detection of circulating anti-MUC1 mucin core protein antibodies in patients with colorectal cancer. J Gastroenterol 33: 354–356
Paulsen H, Peters S, Bielfeldt T, Meldal M, Bock K (1995) Synthesis of the glycosyl amino acid N alpha-Fmoc-Ser[Ac4-beta-D-Galp-(1–>3)-Ac2-alpha-D-GalN3p]-OPfp and N alpha-Fmoc-Thr[Ac4-beta-D-Galp-(1–>3)-Ac2-alpha-D-GalN3p]-OPfp and the application in the solid-phase peptide synthesis of multiply glycosylated mucin peptides with Tn and T antigenic structures. Carbohydr Res 268: 17–34
Pear WS, Nolan GP, Scott ML, Baltimore D (1993) Production of high-titer helper-free retroviruses by transient transfection. Proc Natl Acad Sci USA 90: 8392–8396
Perkins AC, Symonds IM, Pimm MV, Price MR, Wastie ML, Symonds EM (1993) Immunoscintigraphy of ovarian carcinoma using a monoclonal antibody (111In-NCRC48) defining a polymorphic epithelial mucin (PEM) epitope. Nucl Med Commun 14: 578–586
Pietersz GA, Li W, Osinski C, Apostolopoulos V, McKenzie IF (2000) Definition of MHC-restricted CTL epitopes from non-variable number of tandem repeat sequence of MUC1. Vaccine 18: 2059–2071
Price MR, Briggs S, Scanlon MJ, Tendler SJB, Sibley PEC, Hand CW (1992) The mucin antigens – what are we measuring? Dis Markers 9: 205–212
Price MR, Hudecz F, O'Sullivan C, Baldwin RW, Edwards PM, Tendler SJ (1990) Immunological and structural features of the protein core of human polymorphic epithelial mucin. Mol Immunol 27: 795–802
Price MR, and 59 coathors (1997) Summary report on the ISOBM TD-4 Workshop: analysis of 56 monoclonal antibodies against the MUC1 mucin. Tumour Biol 19 (Suppl): 1–20
Reddish M, MacLean GD, Koganty RR, Kan-Mitchell J, Jones V, Mitchell MS, Longenecker BM (1998) Anti-MUC1 class I restricted CTLs in metastatic breast cancer patients immunized with a synthetic MUC1 peptide. Int J Cancer 76: 817–823
Rughetti A, Turchi V, Ghetti CA, Scambia G, Panici PB, Roncucci G, Mancuso S, Frati L, Nuti M (1993) Human B-cell immune response to the polymorphic epithelial mucin. Cancer Res 53: 2457–2459
Shu L, Qi CF, Schlom J, Kashmiri SV (1993) Secretion of a single-gene-encoded immunoglobulin from myeloma cells. Proc Natl Acad Sci USA 90: 7995–7999
Smith M, Burchel JM, Grahman R, Cohen EP, Taylor-Papadimitriou J (1999) Expression of B7.1 in an MUC1-expressing mouse mammary epithelial tumour cell line inhibits tumorigenicity but does not induce autoimmunity in MUC1 transgenic mice. Immunology 97: 648–655
Symonds IM, Price MR, Pimm MV, Perkins AC, Wastie ML, Baldwin RW, Symonds EM (1992) Preliminary report of tumour localisaton and imaging of ovarian neoplasia with a new monoclonal antibody raised against urinary mucin. In Tumour Associated Antigens. Oncogenes, Receptors, Cytokines in Tumour Diagnosis and Therapy at the Beginning of the Ninties, Klapdor R (ed) pp 572–577. Munich: W Zuckscherdt.
Tempero RM, Rowse GJ, Gendler SJ, Hollingsworth MA (1999) Passively transferred anti-MUC1 antibodies cause neither autoimmune disorders nor immunity against transplanted tumors in MUC1 transgenic mice. Int J Cancer 80: 595–599
Tempero RM, VanLith ML, Morikane K, Rowse GJ, Gendler SJ, Hollingsworth MA (1998) CD4+ lymphocytes provide MUC1-specific tumor immunity in vivo that is undetectable in vitro and is absent in MUC1 transgenic mice. J Immunol 161: 5500–5506
VanLith ML, Kohlgraf KG, Sivinski CL, Tempero RM, Hollingsworth MA (2002) MUC1-specific anti-tumor responses: molecular requirements for CD4-mediated responses. Int Immunol 14: 873–882
Vlad AM, Muller S, Cudic M, Paulsen H, Otvos L Jr, Hanisch FG, Finn OJ (2002) Complex carbohydrates are not removed during processing of glycoproteins by dendritic cells: processing of tumor antigen MUC1 glycopeptides for presentation to major histocompatibility complex class II-restricted T cells. J Exp Med 196: 1435–1446.
Xu X, Clarke P, Szalai G, Shively JE, Williams LE, Shyr Y, Shi E, Primus FJ (2000) Targeting and therapy of carcinoembryonic antigen-expressing tumors in transgenic mice with an antibody–interleukin 2 fusion protein. Cancer Res 60: 4475–4484
Acknowledgements
This project was supported by the Deutsche Forschungsgemeinschaft (grant Ab58/5-1 to HA and F-GH), the Deutsche Krebshilfe, Bonn (Grant 10-1559-Ho2 to AH), the National Institute of Health (Grant 1R01 CA84106 to F-GH), the Köln Fortune Program of the Medical Faculty and the Center for Molecular Medicine Cologne.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Heuser, C., Ganser, M., Hombach, A. et al. An anti-MUC1-antibody–interleukin-2 fusion protein that activates resting NK cells to lysis of MUC1-positive tumour cells. Br J Cancer 89, 1130–1139 (2003). https://doi.org/10.1038/sj.bjc.6601267
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bjc.6601267
Keywords
This article is cited by
-
The role of tumor hypoxia in MUC1-positive breast carcinomas
Virchows Archiv (2011)
-
Therapeutic efficacy of tumor-targeted IL2 in LTα−/− mice depends on conditioned T cells
Cancer Immunology, Immunotherapy (2006)