Abstract
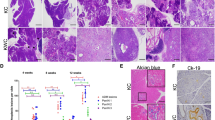
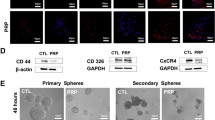
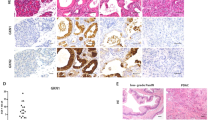
PTEN is a candidate tumour suppressor gene and frequently mutated in multiple cancers, however, not in pancreatic cancer. Recently, it has been demonstrated that PTEN expression is regulated by TGF-β1. Using TGF-β1 transgenic mice (n=7) and wildtype littermates (n=6), as well as pancreatic tissues obtained from organ donors (n=10) and patients with pancreatic cancer (n=10), we assessed the expression of PTEN by means of immunohistochemistry and semiquantitative PCR analysis. In addition, PANC-1 cells were treated with TGF-β1 in vitro and the levels of PTEN mRNA were determined in these cells. In human pancreatic cancers PTEN mRNA levels were significantly decreased (P<0.05). In addition, in the pancreas of TGF-β1 transgenic mice the expression of PTEN was significantly reduced (P<0.01), as compared to wildtype littermates and incubation of PANC-1 cells with TGF-β1 decreased PTEN mRNA levels after 24 h. Inasmuch as TGF-β1 decreases PTEN expression in human pancreatic cancer cells and human pancreatic cancers overexpress TGF-β1, the reduced expression of PTEN in pancreatic cancer may be mediated by TGF-β1 overexpression. Thus, although PTEN is not mutated in pancreatic cancers, the reduction of its expression may give pancreatic cancer cells an additional growth advantage.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Davies MA, Koul D, Dhesi H, Berman R, McDonnell TJ, McConkey D, Yung K, Steck PA (1999) Regulation of Akt/PKB activity, cellular growth, and apoptosis in prostate carcinoma cells by MMAC/PTEN. Cancer Res 59: 2551–2556
Ebert M, Hoffmann J, Haeckel C, Rutkowski K, Schmid RM, Wagner M, Adler G, Schulz HU, Roessner A, Hoffmann W, Malfertheiner P (1999) Induction of TFF1 gene expression in pancreas overexpressing transforming growth factor-α. Gut 45: 105–111
Ebert M, Yokoyama M, Kobrin MS, Friess H, Lopez ME, Büchler MW, Korc M (1994) Induction and expression of amphiregulin in human pancreatic cancer. Cancer Res 54: 3959–3962
Ebert M, Yokoyama M, Kobrin MS, Friess H, Büchler MW, Korc M (1995) Induction of platelet-derived growth factors and overexpression of their receptors in pancreatic cancers. Int J Cancer 62: 529–535
Friess H, Yamanaka Y, Büchler MW, Ebert M, Beger HG, Gold LI, Korc M (1993) Enhanced expression of transforming growth factor β isoforms in pancreatic cancer correlates with decreased survival. Gastroenterology 105: 1846–1856
Fujimoto K, Hosotani R, Wada M, Lee JU, Koshiba T, Miyamoto Y, Tsuji S, Nakajima S, Doi R, Imamura M (1998) Expression of two angiogenic factors, vascular endothelial growth factor and platelet-derived growth factor in human pancreatic cancer, and its relationship to angiogenesis. Eur J Cancer 34: 1439–1447
Geng M, Ellenrieder V, Wallrapp C, Müller-Pillasch F, Sommer G, Adler G (1999) Identification of TGF-β1 target genes in pancreatic cancer cells by cDNA representational difference analysis. Genes Chromosomes Cancer 26: 70–79
Hahn SA, Schmiegel WH (1998) Recent discoveries in cancer genetics of exocrine pancreatic neoplasia. Digestion 59: 493–501
Korc M, Chandrasekar B, Yamanaka Y, Friess H, Büchler M, Beger HG (1992) Overexpression of the epidermal growth factor receptor in human pancreatic cancer is associated with concomitant increase in the levels of epidermal growth factor and transforming growth factor-alpha. J Clin Invest 90: 1352–1360
Korc M (1998) Role of growth factors in pancreatic cancer. Surg Oncol Clin North Am 7: 25–41
Kornmann M, Ishiwata T, Beger HG, Korc M (1997) Fibroblast growth factor-5 stimulates mitogenic signaling and is overexpressed in human pancreatic cancer: evidence for autocrine and paracrine actions. Oncogene 15: 1417–1424
Kornmann M, Tangvoranuntakul P, Korc M (1999) TGF-beta-1 up-regulates cyclin D1 expression in COLO-357 cells, whereas suppression of cyclin D1 levels is associated with down-regulation of the type I TGF-beta receptor. Int J Cancer 83: 247–254
Li DM, Sun H (1997a) TEP1, encoded by a candidate tumor suppressor locus, is a novel protein tyrosine phosphatase regulated by transforming growth factor beta. Cancer Res 57: 2124–2129
Li J, Yen C, Liaw D, Podsypanina K, Bose S, Wang SI, Puc J, Miliaresis C, Rodgers L, McCombie R, Bigner SH, Giovanella BC, Ittmann M, Tycko B, Hibshoosh H, Wigler MH, Parsons R (1997b) PTEN, a putative protein tyrosine phosphatase gene mutated in human brain, breast, and prostate cancer. Science 275: 1943–1947
Löhr M, Schmidt C, Ringel J, Kluth M, Muller P, Nizze H, Jesnowski R (2001) Transforming growth factor beta1 induces desmoplasia in an experimental model of human pancreatic carcinoma. Cancer Res 61: 550–555
Liaw D, Marsh DJ, Li J, Dahia PL, Wang SI, Zheng Z, Bose S, Call KM, Tsou HC, Peacocke M, Eng C, Parsons R (1997) Germline mutations of the PTEN gene in Cowden disease, an inherited breast and thyroid cancer syndrome. Nat Genet 16: 64–74
Lynch ED, Ostermyer EA, Lee MK, Arena JF, Ji H, Dann J, Swisshelm K, Suchard D, MacLeod PM, Kvinnsland S, Gjertsen BT, Heimdal K, Lubs H, Moller P, King MC (1997) Inherited mutation in PTEN that are associated with breast cancer, Cowden's disease, and juvenile polyposis. Am J Genet 61: 1254–1260
Maehama T, Dixon JE (1998) The tumour suppressor, PTEN/MMAC1, dephosphorylates the lipid second messenger phosphatidylinositol 3,4,5-triphosphate. J Biol Chem 273: 13375–13378
Marsh DJ, Dahia PL, Zheng Z, Liaw D, Parsons R, Gorlin RJ, Eng C (1997) Germline mutations in PTEN are present in Bannayan-Zonana syndrome. Nat Genet 16: 333–334
Massagué J (1996) TGF-beta signaling: Receptors, transducers, and Mad proteins. Cell 85: 947–950
McMenamin ME, Soung P, Perera S, Kaplan I, Loda M, Selers WR (1999) Loss of PTEN expression in paraffin-embedded primary prostate cancer correlates with high Gleason score and advanced stage. Cancer Res 59: 4291–4296
Mutter GL, Lin MC, Fitzgerald JT, Kum JB, Baak JP, Lees JA, Wenig LP, Eng C (2000) Altered PTEN expression as a diagnostic marker for the earliest endometrial precancers. J Natl Cancer Inst 92: 924–930
Myers MP, Stolarov JP, Eng C, Li J, Wang SI, Wigler MH, Persons R, Tonks NK (1997) P-TEN, the tumor suppressor from human chromosome 10q23, is a dual specificity phosphatase. Proc Natl Acad Sci USA 94: 9052–9057
Nelen MR, van Staveren WC, Peeters EA, Hassel MB, Gorlin RJ, Hamm H, Lindboe CF, Fryns JP, Sijmons RH, Woods DG, Mariman EC, Padberg GW, Kremer H (1997) Germline mutations in the PTEN/MMAC1 gene in patients with Cowden disease. Hum Mol Genet 6: 1383–1387
Okami K, Wu L, Riggins G, Cairns P, Goggins M, Evron E, Halachmi N, Ahrendt SA, Reed AL, Hilgers W, Kern SE, Koch WM, Sidransky D, Jen J (1998) Analysis of PTEN/MMAC1 alterations in aerodigestive tract tumors. Cancer Res 58: 509–511
Perren A, Komminoth P, Saremaslani P, Matter C, Feurer S, Lees JA, Heitz PU, Eng C (2000) Mutation and expression analyses reveal differential subcellular compartmentalization of PTEN in endocrine pancreatic tumors compared to normal islet cells. Am J Pathol 157: 1097–1103
Perren A, Wenig LP, Boag AH, Ziebold U, Thakore K, Dahia PL, Komminoth P, Lees JA, Mulligan LM, Mutter GL, Eng C (1999) Immunohistochemical evidence of loss of PTEN expression in primary ductal adenocarcinomas of the breast. Am J Pathol 155: 1253–1260
Sakurada A, Suzuki A, Sato M, Yamakawa H, Orikasa K, Uyeno S, Ono T, Ohuchi N, Fujimura S, Horii A (1997) Infrequent genetic alterations of the PTEN/MMAC1 gene in Japanese patients with primary cancers of the breast, lung, pancreas, kidney, and ovary. Jpn J Cancer Res 88: 1025–1028
Sano T, Lin H, Chen X, Langford LA, Koul D, Bondy ML, Hess KR, Myers JN, Hong YK, Yung WK, Steck PA (1999) Differential expression of MMAC/PTEN in glioblastoma multiforme: relationship to localization and prognosis. Cancer Res 59: 1820–1824
Sanvito F, Nichols A, Herrera PL, Huarte J, Wohlwend A, Vassalli JD, Orci L (1995) TGF-β1 overexpression in murine pancreas induces chronic pancreatitis and, together with TNF-α, triggers insulin-dependent diabetes. Biochem Biophys Res Commun 217: 1279–1286
Satoh K, Shimosegawa T, Hirota M, Koizumi M, Toyota T (1998) Expression of transforming growth factor beta1 (TGFbeta1) and its receptors in pancreatic duct cell carcinoma and in chronic pancreatitis. Pancreas 16: 468–474
Siegel S (1956) Nonparametric statistics for behavioral sciences. New York: McGraw-Hill
Simpkins SB, Peiffer-Schneider S, Mutch DG, Gersell D, Goodfellow PJ (1998) PTEN mutations in endometrial cancers with 10q LOH: additional evidence for the involvement of multiple tumor suppressors. Gynecol Oncol 71: 391–395
Stambolic V, Suzuki A, de la Pompa JL, Brothers GM, Mirtsos C, Sasaki T, Ruland J, Penninger JM, Siderovski DP, Mak TW (1998) Negative regulation of PKB/Akt-dependent cell survival by the tumor suppressor PTEN. Cell 95: 29–39
Steck PA, Pershouse MA, Jasser SA, Yung WK, Lin H, Ligon AH, Langford LA, Baumgard ML, Hattier T, Davis T, Frye C, Hu R, Swedlund B, Teng DH, Tavtigian SV (1997) Identification of a candidate tumour suppressor gene, MMAC1, at chromosome 10q23.3 that is mutated in multiple advanced cancers. Nat Genet 15: 356–362
Warshaw AL, Fernandez-Del Castillo C (1992) Pancreatic carcinoma. N Engl J Med 326: 455–465
Whang YE, Wu X, Suzuki H, Reiter RE, Tran C, Vessella RL, Said JW, Isaacs WB, Sawyers CL (1998) Inactivation of the tumor suppressor PTEN/MMAC1 in advanced human prostate cancer through loss of expression. Proc Natl Acad Sci USA 95: 5246–5250
Acknowledgements
This study was supported by grants from the Matthias-Lackas-Stiftung and the Land Sachsen-Anhalt awarded to MPA Ebert. L Schandl was supported by the DAAD.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ebert, M., Fei, G., Schandl, L. et al. Reduced PTEN expression in the pancreas overexpressing transforming growth factor-beta 1. Br J Cancer 86, 257–262 (2002). https://doi.org/10.1038/sj.bjc.6600031
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bjc.6600031