Abstract
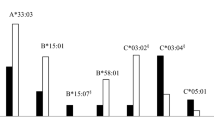
Toll-like receptor 6 (TLR6) is one of a series of highly conserved innate immune receptors. We resequenced TLR6 in DNA samples from 24 African Americans, 23 European Americans, and 24 Hispanic Americans, identifying 53 SNPs, 22 with an allele frequency >5%. Significant differences in SNP frequencies among the three populations were noted. In all, 11 SNPs caused amino-acid changes, including one with a frequency >5% in all three populations. Utilizing this SNP (Ser249Pro), we performed exploratory nested case–control disease-association studies, including one involving 56 African Americans with asthma and 93 African American controls. The minor allele of this SNP was associated with decreased risk for asthma (odds ratio 0.38, 95% CI 0.16–0.87, P=0.01), an effect consistent with the known biology of the toll-like receptors. Although replication of this finding in other, larger samples is needed, variation in TLR6 may have relevance to the pathogenesis of immunologically mediated diseases.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 digital issues and online access to articles
$119.00 per year
only $19.83 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Kadowaki N, Ho S, Antonenko S et al. Subsets of human dendritic cell precursors express different toll-like receptors and respond to different microbial antigens. J Exp Med 2001: 863–869.
Means TK, Golenbock DT, Fenton MJ . The biology of Toll-like receptors. Cytokine Growth Factor Rev 2000; 11: 219–232.
Hallman M, Ramet M, Ezekowitz RA . Toll-like receptors as sensors of pathogens. Pediatr Res 2001; 50: 315–321.
Takeuchi O, Kawai T, Sanjo H et al. TLR6: a novel member of an expanding toll-like receptor family. Gene 1999; 231: 59–65.
Guo SW, Thompson EA . Performing the exact test of Hardy–Weinberg proportion for multiple alleles. Biometrics 1992; 48: 361–372.
Cargill M, Altshuler D, Ireland J et al. Characterization of single-nucleotide polymorphisms in coding regions of human genes. Nat Genet 1999; 22: 231–238.
Halushka MK, Fan JB, Bentley K et al. Patterns of single-nucleotide polymorphisms in candidate genes for blood-pressure homeostasis. Nat Genet 1999; 22: 239–247.
Goddard KA, Hopkins PJ, Hall JM, Witte JS . Linkage disequilibrium and allele-frequency distributions for 114 single-nucleotide polymorphisms in five populations. Am J Hum Genet 2000; 66: 216–234.
Stampfer MJ, Willett WC, Colditz GA et al. A prospective study of postmenopausal estrogen therapy and coronary heart disease. N Engl J Med 1985; 313: 1044–1049.
Bell B, Rose CL, Damon H . The Normative Aging Study: an interdisciplinary and longitudinal study of health and aging. Aging Hum Dev 1972; 3: 5–17.
Manson JE, Grobbee DE, Stampfer MJ et al. Aspirin in the primary prevention of angina pectoris in a randomized trial of United States physicians. Am J Med 1990; 89: 772–776.
Strachan DP . Hay fever, hygiene, and household size. BMJ 1989; 299: 1259–1260.
Romagnani S . Human TH1 and TH2 subsets: regulation of differentiation and role in protection and immunopathology. Int Arch Allergy Immunol 1992; 98: 279–285.
Bach JF . Protective role of infections and vaccinations on autoimmune diseases. J Autoimmun 2001; 16: 347–353.
Mazzoni A, Young HA, Spitzer JH, Visintin A, Segal DM . Histamine regulates cytokine production in maturing dendritic cells, resulting in altered T cell polarization. J Clin Invest 2001; 108: 1865–1873.
Arbour NC, Lorenz E, Schutte BC et al. TLR4 mutations are associated with endotoxin hyporesponsiveness in humans. Nat Genet 2000; 25: 187–191.
Von Ehrenstein OS, Von Mutius E, Illi S et al. Reduced risk of hay fever and asthma among children of farmers. Clin Exp Allergy 2000; 30: 187–193.
Hume DA, Underhill DM, Sweet MJ et al. Macrophages exposed continuously to lipopolysaccharide and other agonists that act via toll-like receptors exhibit a sustained and additive activation state. BMC Immunol 2001; 2: 11.
McCurdy JD, Olynych TJ, Maher LH, Marshall JS . Cutting edge: distinct Toll-like receptor 2 activators selectively induce different classes of mediator production from human mast cells. J Immunol 2003; 170: 1625–1629.
Bradding P . The role of the mast cell in asthma: a reassessment. Curr Opin Allergy Clin Immunol 2003; 3: 45–50.
Busse WW, Lemanske Jr. RF . Asthma. N Engl J Med 2001; 344: 350–362.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by the Program for Genomic Applications, NIH R01: HL66795, Innate Immunity in Heart, Lung and Blood Disease, from the National Heart and Blood Institute, and by NIH 2T32: HL07427-21, The Clinical Epidemiology of Lung Diseases.
Supplementary Information accompanies the paper on Genes and Immunity's website (http://www.nature.com/gene).
Supplementary information
Web Table A
Flanking Sequences of Identified TLR6 SNPs
Rights and permissions
About this article
Cite this article
Tantisira, K., Klimecki, W., Lazarus, R. et al. Toll-like receptor 6 gene (TLR6): single-nucleotide polymorphism frequencies and preliminary association with the diagnosis of asthma. Genes Immun 5, 343–346 (2004). https://doi.org/10.1038/sj.gene.6364096
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.gene.6364096
Keywords
This article is cited by
-
Integrated genomics analysis highlights important SNPs and genes implicated in moderate-to-severe asthma based on GWAS and eQTL datasets
BMC Pulmonary Medicine (2020)
-
Genetic predisposition of variants in TLR2 and its co-receptors to severe malaria in Odisha, India
Immunologic Research (2016)
-
Toll-like receptors: promising therapeutic targets for inflammatory diseases
Archives of Pharmacal Research (2016)
-
Association of TLR1, TLR2, TLR4, TLR6, and TIRAP polymorphisms with disease susceptibility
Immunologic Research (2015)
-
Diversity in the Toll-like receptor genes of the Tasmanian devil (Sarcophilus harrisii)
Immunogenetics (2015)