Abstract
The 22q13 deletion syndrome is associated with global developmental delay, absent or delayed speech, and generalised hypotonia. In this study, the size and nature of 22q13 deletions (n=9) were studied in detail by high-resolution chromosome specific array-based comparative genomic hybridisation (array CGH). The deletion sizes varied considerably between the different patients, that is, the largest deletion spanning 8.4 Mb with the breakpoint mapping to 22q13.2 and the smallest deletion spanning 3.3 Mb with the breakpoint mapping to 22q13.31. In one case, a unique subtelomeric 3.9 Mb deletion associated with a 2.0 Mb duplication of 22q13 was observed, adding to a growing number of similar cases identified for other chromosome ends. Remarkably, this patient had signs suggestive of retinitis pigmentosa, which has never been reported before in the 22q13 deletion syndrome. The identification of two pairs of recurrent proximal breakpoints on 22q13 suggests that these specific regions may be prone to recombination, due to yet unknown genome architectural features. In addition to the copy number changes on 22q13, a duplication of ∼330 kb on 22q11.1 was observed and shown to be a genetic large-scale copy number variation without clinical consequences. The current study failed to reveal relationships between the clinical features and the deletion sizes. Global developmental delay and absent or severely delayed speech were observed in all patients, whereas hypotonia was present in 89% of the cases (8/9). This study underscores the utility of array CGH for characterising the size and nature of subtelomeric deletions, such as monosomy 22q13, and underlines the considerable variability in deletion size in the 22q13 deletion syndrome regardless of the clinical phenotype.
Similar content being viewed by others
Introduction
Subtelomeric deletions are a common cause of mental retardation.1, 2 In recent years, screening of subtelomeres for copy number changes in mentally retarded patients has resulted in the recognition of new distinct clinical entities, based on monosomy 1q, 2q, 9q, 14q, and 22q (reviewed in Vries et al1) The latter entity is also referred to as the 22q13 deletion syndrome, of which to date at least 100 cases have been reported.3, 4, 5, 6 Common features associated with this syndrome are mild-to-severe global developmental delay, absent or delayed speech, generalised hypotonia, and minor anomalies including dolichocephaly, ptosis, abnormal ears, relatively large hands, and dysplastic toenails.5
Here we describe a series of nine patients with monosomy 22q13 in which the size and the nature of the chromosome 22 deletions were studied in detail by high-resolution chromosome-specific array-based comparative genomic hybridisation (array CGH).7
Materials and methods
Patients and DNA samples
In total, nine patients with subtelomeric deletions of 22q13 were included in this study. Three cases were previously published (case 2,8 case 79 and case 910). DNA samples of the patients were derived from different clinical centres in France, Ireland, the United Kingdom, and the Netherlands (Nijmegen). Clinical information on the patients was obtained from the referring physician. DNA samples of all patients were analysed using array CGH. In one patient (case 3), the 22qter deletion was initially identified by routine chromosome analysis at a 550-band level and confirmed by fluorescence in situ hybridisation (FISH) [46, XY, del(22)(q13.2).ish del(22)(TUPLE+, ARSA-)]. Another deletion (case 4) resulted from a de novo translocation [46, XY, der(22)t(14;22)(q32.33;q13.31)pat. ish der(22)(N85A3-)], whereas the remaining cases were initially identified by FISH, using the following probes: N85A3 (cases 1–2, 5), ARSA (cases 6–8), D22S163 (case 8), or STS WI-941 and D22S39 (case 9).
Array-based comparative genomic hybridisation
High-resolution chromosome 22 array CGH was performed. The microarray consisted of 350 positionally selected chromosome 22 BAC clones (BACPAC Resources), together with 1532 control clones located on other chromosomes. The chromosome 22-specific clones covered the long arm of chromosome 22 (35.1 Mb) with an average spacing of one clone per 100 kb. However, the actual resolution may be less in repeat dense regions. The average clone-insert size was 168 kb, resulting in a 1.7-fold coverage of the long arm of chromosome 22. DOP-PCR products of the BAC clones were spotted in six-fold onto CMT-GAPS-coated glass slides (Ultragaps, Corning) using an OmniGrid 100 arrayer (Genomic Solutions). All steps in the labelling, hybridisation, and data-analysis procedure were performed as described previously.11 In brief, equal amounts of patient and reference genomic DNAs were labelled by random priming with Cy3-dUTP or Cy5-dUTP (Amersham Biosciences). Labelled test- and reference DNAs were mixed with Cot-1 DNA (Roche), coprecipitated and resuspended in a hybridisation solution. After denaturation of probe and target DNA, hybridisation and posthybridisation washing procedures were performed using a GeneTac Hybridisation Station (Genomic Solutions), according to the instructions of the manufacturer. Fluorescence intensity images were acquired using an Affymetrix 428 scanner (Affymetrix), and analysed by Genepix Pro 5.1 (Axon Instruments).
Statistical data analysis
Data normalisation was performed by applying Lowess curve fitting with a smoothing factor of 0.3 as described by Vissers et al11 Copy number alterations were identified by using a Hidden Markov Model algorithm. Three hidden states represent normal, loss, and gain conditions. The probability to observe a log ratio given its hidden state is modelled by a Gaussian with SD 0.25 and mean 0, −0.4 and 0.4, respectively. The hidden state of adjacent clones is correlated with respect to their distance. The thresholded marginal probability of a clone's hidden state determines if it is normal, a loss or gain. In order to discriminate between causative aberrations and large-scale copy number variations (LCV) we used a data set of 72 normal individuals. The control population was tested by a genome-wide 32.477 clone BAC array which included the same clones as used for the chromosome 22 array.
Results
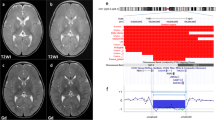
Seven patients with a submicroscopic 22qter deletion, one patient with an unbalanced translocation and one patient with a microscopically visible 22qter deletion were studied. In Table 1, the main characteristics of the patients are summarised. In addition, minor facial dysmorphisms were noted (Figure 1). High-resolution chromosome 22-specific array CGH confirmed the known copy number changes in all cases and delineated the specific aberrations in detail. Figure 2 shows two examples of chromosome 22 array CGH profiles. All deletions analysed included the most telomeric clones. Interstitial deletions in the subtelomeric region of the long arm of chromosome 22 were not observed. The deletion sizes identified in this study varied considerably between the different patients, that is, the largest deletion spanning 8.4 Mb with breakpoint mapping to 22q13.2qter (68 clones, case 1) and the smallest deletion spanning 3.3 Mb with breakpoints mapping to 22q13.31qter (27 clones, case 9) (Figure 3). Identical proximal breakpoints were localised in cases 2 and 3 (between RP11-786O06 and RP11-236I15) and cases 5 and 6 (between RP11-766K21 and RP11-49A20), resulting in deletion sizes of 7.7 and 5.9 Mb, respectively. In case 3, a del(22)(q13.2qter) was originally identified by routine chromosome analysis. Array CGH analysis confirmed the karyotypic analysis and established the deletion size to 7.7 Mb. Case 4 carried a translocation between chromosomes 14 and 22 [46, XY, der(22)t(14;22)(q32.33;q13.31)]. Array CGH analysis revealed a 6.6 Mb deletion at 22q13.31qter. In case 7, a deletion of 5.0 Mb was identified, whereas in case 8 the deletion spanned 3.9 Mb. The latter 22q13 deletion was associated with a duplication of 2.0 Mb, including 13 clones adjacent to the deleted region (Figure 2b). In addition to these subtelomeric copy number alterations, a duplication of ∼330 kb on 22q11.1 was detected in the same patient. Duplications in the same region next to the centromere were identified in two other cases in this series (cases 4 and 7). In the control panel of 72 normal individuals tested by a tiling resolution genome-wide BAC array, copy number gain of the same region was observed in five individuals, whereas loss of the chromosomal segment was seen in 21 controls (de Vries, submitted).
Examples of chromosome- 22 profiles obtained by array CGH. Arrays contained 350 cloned chromosome- 22 genomic DNA targets (indicated by small circles representing the mean log2-transformed and Lowess-normalised T/R intensity ratios), ordered from q11.1 to qter on the basis of physical mapping positions obtained from the May 2004 freeze of the UCSC Genome Browser. The centromere is indicated by a hatched area. A, case 1: del(22)(q13.2); B, case 8: del(22)(q13.31). Note the duplication of 2.0 Mb on 22q13.31 and the duplication on 22q11.1.
Overview of the array CGH results for the nine patients with monosomy 22qter. Arrays contained 350 chromosome- 22 DNA BAC clones, ordered from q11.1 to qter on the basis of physical mapping positions obtained from the May 2004 freeze of the UCSC Genome Browser. The distal 9 Mb of the long arm of chromosome 22 is depicted in the figure. Copy number alterations were identified, using a Hidden Markov Model algorithm. Three hidden states represent normal (empty), loss (LOSS) and gain (GAIN) conditions. Individual clones that did not pass quality control criteria were excluded (EXCL).
Discussion
For detailed analyses of patients with known 22q13 deletions, a tiling resolution array was constructed with a 1.7-fold coverage of the long arm of chromosome 22. Buckley et al12 demonstrated the utility of such a comprehensive chromosome 22 array by profiling acral melanoma, dermatofibrosarcoma, DiGeorge syndrome, and neurofibromatosis 2. The chromosome 22 tiling resolution array had an average clone spacing of 100 kb, resulting in a resolution that is 30 times higher than high-resolution karyotyping. The array did not cover the most telomeric 635 kb of the chromosome, which includes the gene SHANK3/ProSAP2. Haploinsufficiency of this gene has been proposed to be responsible for the major neurological features of the 22q13 deletion syndrome.6, 13, 14 However, FISH analysis using subtelomeric clones, confirmed the extension of all deletions found till the subtelomeric region.
In the present study, a considerable difference in deletion sizes was noted, which is in accordance with the results of Luciani et al3 which showed an extremely variable 22qter deletion size, extending from 160 kb to 9 Mb. Interestingly, a complex chromosome 22 rearrangement was observed in case 8, with a unique combination of a deletion and a duplication of 22q13. The detection of the deletion-duplication in this patient adds to a growing number of similar cases identified for other chromosomes, including deletion-duplications in 1p, 2q, 4p, and 8p.15, 16, 17, 18 Giglio et al19 demonstrated that the formation of the inverted duplications of 8p associated with a terminal deletion is caused by nonallelic homologous recombination (NAHR) between two olfactory receptor-gene clusters. In addition, Ballif et al described two terminal deletions of 1p36 associated with cryptic interrupted inverted duplications. This type of chromosome rearrangement may be more common than previously thought. The detection of cryptic duplication associated with terminal deletions is greatly improved by high-resolution copy number screening using array CGH. Further studies are needed to determine the mechanisms underlying these rearrangements. Ballif et al18 proposed a premeiotic model in which a terminally deleted chromosome is generated in the germ line and passes through at least one breakage–fusion–bridge cycle in which uncapped sister chromatids are fused by nonhomologous end joining (NHEJ), resulting in gametes with terminal deletions associated with cryptic interrupted inverted duplications. The identification of recurrent proximal breakpoints in cases 2 and 3 (between RP11-786O06 and RP11-236I15) and cases 5 and 6 (between RP11-564B15 and RP11-673D06), suggests that these regions may be prone to recombination, due to the presence of yet unknown genome architectural features. Segmental duplications were present at or close to the recurrent breakpoints and also to the other, nonrecurrent breakpoints in our series. To a large extent, chromosome rearrangement breakpoints are located in intervals containing complex genomic architecture, such as AT-rich palindromes or low-copy repearts (LCRs).20 Through the process of NAHR, LCRs can lead to translocations, inversions, duplications and interstitial deletions.21 However, the mechanisms for generating and/or stabilising terminally deleted chromosomes are poorly understood. NEHJ, possibly stimulated by LCRs or other repetitive sequences, may be one of the causative mechanisms for the terminal 22q13 deletions in our series.
In addition to the known 22qter deletions, a submicroscopic duplication on 22q11.1 next to the centromere was identified in three cases (cases 4, 7 and 8). In the control population of 72 normal individuals, copy number gains in the same region were identified in five individuals, whereas losses were observed in 21 controls (de Vries; submitted), indicating that this anomaly represents a LCV. This LCV at 22q11.1 was previously reported by Sebat et al22 (http://projects.tcag.ca/variation/) and stresses the variation of the human genome and the importance of parental and control analysis in case a submicroscopic alteration is identified.
In the current study, no relation between clinical features and deletion size could be observed. The clinical features observed were consistent with the common clinical phenotype associated with the 22q13 deletion syndrome,5 although dolichocephaly and ptosis were not found in the current study. Global developmental delay and absent or severely delayed speech were observed in all patients. Hypotonia was present in 89% of the cases (8/9). A pointed chin was present in cases 1 and 4–7. Wilson et al6 previously suggested a candidate gene for this feature in the proximal region of 22q13, however this could not be confirmed in our series. In addition, in case 8, ophthalmic assessment showed myopia and salt-and-pepper retinal changes suggestive of retinitis pigmentosa. These eye anomalies, which have not been reported in the 22q13 deletion syndrome before, are possibly attributable to the 2 Mb 22q13.31 duplication in this patient. Relationship between the deletion size and clinical features could not be observed. However, case 9 with the smallest 22q13 deletion (3.3 Mb), did not show any of the dysmorphic features commonly described in the 22q13 deletion syndrome. Facial dysmorphic features in this patient included upslanting palpebral fissures, a moderate hypertrophic nasal root, and thick lips.10 These findings underline the study of Wilson et al, in which no significant correlation with the size of the deletion could be demonstrated for most clinical features and support the idea that a gene in the 3.3 Mb minimal deleted region (notably SHANK3/ProSAP2) may be the major candidate gene in the 22q13 deletion syndrome.3, 4, 5, 6
In conclusion, this study underscores the utility of array CGH for further characterisation of the size and nature of subtelomeric deletions. In addition, these results confirm the considerable differences in deletion size observed in patients with the 22q13 deletion syndrome, regardless of the clinical phenotype.
References
De Vries BB, Winter R, Schinzel A, Ravenswaaij-Arts C : Telomeres: a diagnosis at the end of the chromosomes. J Med Genet 2003; 40: 385–398.
Knight SJ, Flint J : Perfect endings: a review of subtelomeric probes and their use in clinical diagnosis. J Med Genet 2000; 37: 401–409.
Luciani JJ, de Mas P, Depetris D et al: Telomeric 22q13 deletions resulting from rings, simple deletions, and translocations: cytogenetic, molecular, and clinical analyses of 32 new observations. J Med Genet 2003; 40: 690–696.
Manning MA, Cassidy SB, Clericuzio C et al: Terminal 22q deletion syndrome: a newly recognized cause of speech and language disability in the autism spectrum. Pediatrics 2004; 114: 451–457.
Phelan MC, Rogers RC, Saul RA et al: 22q13 deletion syndrome. Am J Med Genet 2001; 101: 91–99.
Wilson HL, Wong AC, Shaw SR et al: Molecular characterisation of the 22q13 deletion syndrome supports the role of haploinsufficiency of SHANK3/PROSAP2 in the major neurological symptoms. J Med Genet 2003; 40: 575–584.
Veltman JA, Yntema HG, Lugtenberg D et al: High resolution profiling of X chromosomal aberrations by array comparative genomic hybridisation. J Med Genet 2004; 41: 425–432.
De Vries BB, Bitner-Glindzicz M, Knight SJ et al: A boy with a submicroscopic 22qter deletion, general overgrowth and features suggestive of FG syndrome. Clin Genet 2000; 58: 483–487.
Koolen DA, Nillesen WM, Versteeg MH et al: Screening for subtelomeric rearrangements in 210 patients with unexplained mental retardation using multiplex ligation dependent probe amplification (MLPA). J Med Genet 2004; 41: 892–899.
Goizet C, Excoffier E, Taine L et al: Case with autistic syndrome and chromosome 22q13.3 deletion detected by FISH. Am J Med Genet 2000; 96: 839–844.
Vissers LE, De Vries BB, Osoegawa K et al: Array-based comparative genomic hybridization for the genomewide detection of submicroscopic chromosomal abnormalities. Am J Hum Genet 2003; 73: 1261–1270.
Buckley PG, Mantripragada KK, Benetkiewicz M et al: A full-coverage, high-resolution human chromosome 22 genomic microarray for clinical and research applications. Hum Mol Genet 2002; 11: 3221–3229.
Anderlid BM, Schoumans J, Anneren G et al: FISH-mapping of a 100-kb terminal 22q13 deletion. Hum Genet 2002; 110: 439–443.
Bonaglia MC, Giorda R, Borgatti R et al: Disruption of the ProSAP2 gene in a t(12;22)(q24.1;q13.3) is associated with the 22q13.3 deletion syndrome. Am J Hum Genet 2001; 69: 261–268.
Cotter PD, Kaffe S, Li L, Gershin IF, Hirschhorn K : Loss of subtelomeric sequence associated with a terminal inversion duplication of the short arm of chromosome 4. Am J Med Genet 2001; 102: 76–80.
Floridia G, Piantanida M, Minelli A et al: The same molecular mechanism at the maternal meiosis I produces mono- and dicentric 8p duplications. Am J Hum Genet 1996; 58: 785–796.
Bonaglia MC, Giorda R, Poggi G et al: Inverted duplications are recurrent rearrangements always associated with a distal deletion: description of a new case involving 2q. Eur J Hum Genet 2000; 8: 597–603.
Ballif BC, Yu W, Shaw CA, Kashork CD, Shaffer LG : Monosomy 1p36 breakpoint junctions suggest pre-meiotic breakage-fusion-bridge cycles are involved in generating terminal deletions. Hum Mol Genet 2003; 12: 2153–2165.
Giglio S, Broman KW, Matsumoto N et al: Olfactory receptor-gene clusters, genomic-inversion polymorphisms, and common chromosome rearrangements. Am J Hum Genet 2001; 68: 874–883.
Shaw CJ, Lupski JR : Implications of human genome architecture for rearrangement-based disorders: the genomic basis of disease. Hum Mol Genet 2004; 13 (Spec No 1): R57–R64.
Stankiewicz P, Lupski JR : Molecular-evolutionary mechanisms for genomic disorders. Curr Opin Genet Dev 2002; 12: 312–319.
Sebat J, Lakshmi B, Troge J et al: Large-scale copy number polymorphism in the human genome. Science 2004; 305: 525–528.
Acknowledgements
We thank the patients and their parents for their cooperation. David A Koolen, Joris A Veltman and Bert BA de Vries were supported by a grant from The Netherlands Organisation for Health Research and Development.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Koolen, D., Reardon, W., Rosser, E. et al. Molecular characterisation of patients with subtelomeric 22q abnormalities using chromosome specific array-based comparative genomic hybridisation. Eur J Hum Genet 13, 1019–1024 (2005). https://doi.org/10.1038/sj.ejhg.5201456
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejhg.5201456
Keywords
This article is cited by
-
Speech and language phenotype in Phelan-McDermid (22q13.3) syndrome
European Journal of Human Genetics (2021)
-
Phelan–McDermid Syndrome and SHANK3: Implications for Treatment
Neurotherapeutics (2015)
-
Phelan-McDermid syndrome: a review of the literature and practice parameters for medical assessment and monitoring
Journal of Neurodevelopmental Disorders (2014)
-
A pilot controlled trial of insulin-like growth factor-1 in children with Phelan-McDermid syndrome
Molecular Autism (2014)
-
Prospective investigation of autism and genotype-phenotype correlations in 22q13 deletion syndrome and SHANK3 deficiency
Molecular Autism (2013)