Abstract
Nail-patella syndrome (NPS) is characterized by developmental defects of dorsal limb structures, nephropathy, and glaucoma and is caused by heterozygous mutations in the LIM homeodomain transcription factor LMX1B. In order to identify possible genotype–phenotype correlations, we performed LMX1B mutation analysis and comprehensive investigations of limb, renal, ocular, and audiological characteristics in 106 subjects from 32 NPS families. Remarkable phenotypic variability at the individual, intrafamilial, and interfamilial level was observed for different NPS manifestations. Quantitative urinanalysis revealed proteinuria in 21.3% of individuals. Microalbuminuria was detected in 21.7% of subjects without overt proteinuria. Interestingly, nephropathy appeared significantly more frequent in females. A significant association was established between the presence of clinically relevant renal involvement in an NPS patient and a positive family history of nephropathy. We identified normal-tension glaucoma (NTG) and sensorineural hearing impairment as new symptoms associated with NPS. Sequencing of LMX1B revealed 18 different mutations, including six novel variants, in 28 families. Individuals with an LMX1B mutation located in the homeodomain showed significantly more frequent and higher values of proteinuria compared to subjects carrying mutations in the LIM domains. No clear genotype–phenotype association was apparent for extrarenal manifestations. This is the first study indicating that family history of nephropathy and mutation location might be important in precipitating individual risks for developing NPS renal disease. We suggest that the NPS phenotype is broader than previously described and that NTG and hearing impairment are part of NPS. Further studies on modifier factors are needed to understand the mechanisms underlying phenotypic heterogeneity.
Similar content being viewed by others
Introduction
Nail-patella syndrome (NPS; MIM 161200) is an autosomal dominant disorder characterised by developmental defects of dorsal limb structures, the kidney, and the eye, manifested by nail dysplasia, patellar abnormalities, elbow dysplasia, iliac horns, nephropathy, and glaucoma, respectively. NPS is caused by heterozygous mutations in the gene encoding the LIM-homeodomain transcription factor LMX1B.1, 2 Studies in Lmx1b−/− mice have shown that Lmx1b plays a crucial role in dorso-ventral patterning of the limb, patterning of the skull, morphogenesis and function of the podocytes and the glomerular basement membrane (GBM), and development of the anterior segment of the eye.3, 4, 5, 6, 7, 8 In the central nervous system, Lmx1b is involved in developing dopaminergic and serotonergic neurons of the hindbrain and the midbrain, and dorsal interneurons of the spinal cord.9, 10, 11, 12
Nephropathy and glaucoma are the most relevant clinical manifestations in human NPS.13, 14 NPS nephropathy is a disease of both the podocytes and the GBM, with irregular thickening and electron lucent areas as consistent ultrastructural hallmarks of the GBM.7, 15, 16 Interestingly, abnormal collagen expression has been observed in human NPS renal biopsy specimens15 and in Lmx1b−/− murine kidneys5 and corneal stroma.6 The molecular mechanisms underlying the phenotypic aspects of this disorder, however, are as yet unclear. Recent studies, including an excellent review by Sweeney et al,17 have shown remarkable phenotypic heterogeneity of NPS, but no statistical analysis of the LMX1B genotype with respect to detailed multidisciplinary clinical studies has been performed.
Here, we performed comprehensive clinical investigations and LMX1B mutation analysis in a large cohort of NPS patients. The aim of the study was three-fold: (a) to define the complete phenotype of NPS based on the knowledge of the Lmx1b expression and function (Figure 1); (b) to compare the presence and severity of renal and extrarenal manifestations at the individual, intrafamilial, and interfamilial level; and (c) to evaluate the NPS characteristics in the view of the LMX1B genotype in order to identify possible genotype–phenotype associations.
Schematic presentation of putative pathogenic pathways underlying the phenotype of nail-patella syndrome. The hypothesised molecular bases underlying ocular anomalies and hearing impairment and clinical findings of possible hearing impairment and psychological symptoms are indicated by dotted arrows. GBM, glomerular basement membrane.
Patients and methods
Patients
The study population comprised 106 subjects with NPS, 50 males and 56 females. The total of 32 families included 96 individuals from 22 unrelated families and 10 sporadic subjects. In total, 21 families were recruited from Human Genetics Departments, five from Orthopaedic Surgery Departments, one from a Paediatric Department, and two from patient contact groups. Three families contacted us through the media. The series of families included one of the first NPS families (family 1) in which linkage of NPS to the ABO blood group was shown in 195718 and a five generation family (family 26) with high prevalence of nephropathy originally described in 1988.19 The study was approved by the local medical ethics committee and written informed consent was obtained from all participants or their parents. All patients were examined at the Radboud University Nijmegen Medical Centre.
Examination of limbs and pelvis
Radiographic series of both knees of individuals aged >6 years, included an antero-posterior view, a true lateral view, and an axial view. For assessment of patellar aplasia or hypoplasia in subjects aged ≤6 years, ultrasonography of both knees was performed. A lateral view of the elbows and an antero-posterior view of the pelvis were taken in all subjects. To quantify the nail, patellar and elbow anomalies, iliac horns, and additional major and minor orthopaedic manifestations of NPS, the clinical scoring system developed by Farley et al20 was used. However, for objective determination of patellar anomalies and iliac horns, the radiographic findings were included instead of palpation. Major orthopaedic diagnoses included club feet and/or hip dysplasia.20 Minor orthopaedic findings comprised tendon contractures in hand and feet and/or foot deformities.20 The severity score was categorised as mild, moderate, or severe according to Farley et al.20
Nephrological examination
Nephrological investigations could be performed in 81 patients from 27 families, 35 males and 46 females with a mean age of 38.6 years (range 0.5–81.8 years) at the time of examination. Blood pressures (BP) were measured in supine position by Dynamap (Criticon, Tampa, FL, USA). The determination of protein and albumin excretion and microscopic examination of urine sediment were performed in a random and a first morning urine specimen. Serum creatinine, albumin, and cholesterol were measured by standard chemical procedures. Proteinuria was defined as total urinary protein >0.1 g/l accompanied by a protein–creatinine ratio >0.2 g per 10 mM of creatinine. Microalbuminuria was defined as an albumin–creatinine ratio (ACR; mg of albumin per 10 mM of creatinine) between 20 and 300 in males and between 30 and 300 in females and macroalbuminuria as an ACR >300. Hypertension was defined as systolic BP ≥140 mmHg and/or diastolic BP ≥90 mmHg for adults and age-related BP reference values were used for children.21 Individuals using antihypertensive therapy were also considered as being hypertensive. Glomerular filtration rate (GFR) was estimated by endogenous creatinine clearance (CrC), calculated by Cockcroft–Gault formula and adjusted for body surface area.22, 23 To investigate possible characteristics related to the renal phenotype, individuals were subdivided according to the presence or absence of nephropathy. For comparing urine and serum analysis and blood pressure between proteinuric and nonproteinuric subjects, the female patient with end-stage renal disease (ESRD) was excluded. For identifying possible renal–extrarenal phenotype associations, the patient with ESRD was included in the group of individuals with nephropathy.
Ophthalmologic investigation
Ophthalmologic investigation could be performed in 51 subjects from 16 families, 21 males and 30 females with a mean age of 39.7 years (range 6–74 years) at the time of evaluation. Ocular examination included visual acuity assessment, intra-ocular pressure (IOP) measurement with Goldmann applanation tonometry, slit-lamp biomicroscopy, gonioscopy, ophthalmoscopy, and visual field investigation by Humphrey visual field analysis (central 30-2) and glaucoma hemifield testing. Subjects using intraocular hypotensive medication interrupted medical therapy 4 days before examination until completion of ocular examination. Ocular hypertension was defined by an IOP >21 mmHg on two separate occasions. Glaucomatous optic disk alteration was defined by a cup–disk ratio of ≥0.7 or a difference in the cup–disk ratios of at least 0.2 between both eyes accompanied by notching of the rim and/or peripapillary haemorrhages of the optic rim.24 Primary open-angle glaucoma (POAG) was defined by glaucomatous cupping of the optic disk, glaucomatous visual field defects, an IOP >21 mmHg on two separate occasions, and open anterior chamber angle. Normal-tension glaucoma (NTG) was defined as POAG with the exception of an IOP≤21 mmHg at the first ocular examination and confirmed by diurnal phasing 6–12 months later.
Audiometric evaluation
Based on the remarkable similarities between nephropathy in NPS and Alport syndrome, a type IV collagen kidney disease associated with sensorineural hearing loss, we questioned whether hearing loss may accompany NPS (Figure 1). Otoscopy and pure tone audiometry were performed in 28 subjects from six families, nine males and 19 females with a mean age of 46.2 years (range 11–75 years) at the time of examination. Individual binaural mean pure tone thresholds (dB hearing loss, air conduction level) at 0.25, 0.5, 1, 2, 4, and 8 kHz were compared with the International Organization for Standardization (ISO) standard 7029 presbyacusis thresholds.25 For genotype–phenotype studies, an individual severity score for threshold progression beyond the 95th percentile (P95) presbyacusis was assessed. Hearing impairment was designated significant when ≥2 out of 6 thresholds at the frequencies 0.25–8 kHz were >P95 presbyacusis matched by age and gender for each ear separately, bilaterally tested with P<0.05 and unilaterally with P<0.095.25 Additionally, individual monaural thresholds were compared with different percentiles (P70–P95) of presbyacusis to find the best-fitting percentile of the ISO 7029 threshold distribution. Four patients were excluded for audiometric analysis, one individual due to noise trauma and three patients aged >70 years since no age-related reference values are available beyond 70 years.
Psychological and health state measures
To investigate psychological symptoms and health status, individuals aged ≥16 years were asked to complete the Dutch version of standardised self-report questionnaires, including:
-
1
Psychopathology using the Symptom Checklist (SCL-90).26
-
2
Depression using the Beck Depression Inventory, diagnosed from a score of 16.27
-
3
State and trait anxiety using the Spielberger Trait Anxiety Inventory.28
-
4
Five personality dimensions using the Revised NEO Five-Factor Inventory.29
To compute an overall ‘health-related quality of life’ figure, five health state dimensions were assessed using the EuroQol-5D inventory.30 Additionally, valuation of health status using a visual analogue scale (VAS) with a score from 0 to 100, representing the lowest to the highest possible health status was requested.
Mutational and FISH analysis
Direct sequencing of the eight coding exons and flanking introns of LMX1B was performed on DNA extracted from peripheral blood lymphocytes as described already.31 In subjects in which no LMX1B mutation could be identified, fluorescence in situ hybridisation (FISH) studies were carried out on metaphases derived from peripheral blood lymphocytes. For FISH analysis, biotin labelled PAC clones 830-M14 and 1195-M2 located in the LMX1B region were used according to standard procedures.32
Statistics
Clinical and molecular findings were analysed using linear and logistic regression models. Since age and gender are known covariates in developing renal, ocular, audiological, and psychological anomalies, multivariate analysis of these symptoms was adjusted for age and gender. For the comparison between clinical and molecular data within and between families, analysis of covariance was performed. For all statistics, P-values are two-tailed and present unadjusted values concerning multiplicity. Significance was set at the 5% probability level.
Results
Limb and pelvic malformations
The results of examination of the limbs and pelvis are summarised in Table 1. Fingernail anomalies were observed in all subjects (Table 1, Figure 2a). On physical examination, an abnormal volume distribution of the proximal musculature of the upper limb was recognised in some NPS patients, with a lower muscle volume of the dorsal muscle groups (triceps brachii) compared to the ventral counterparts (biceps brachii) (Figure 2b). In the lower limb, such evident differences between dorsal (quadriceps femoris) and ventral (hamstrings) proximal musculature volume were not observed. The severity of nail and orthopaedic features, scored according to Farley et al20 was mild in 13.4% (11/82) of individuals, moderate in 52.4% (43/82), and severe in 34.2% (28/82) and was highly variable both within and between families (Figure 3). The complete tetralogy of nail, patellar, elbow, and pelvic anomalies classified according to Farley et al20 was found in 50.6% (41/81) of individuals.
(a) Triangular lunula pathognomonic for nail-patella syndrome, longitudinal ridging of the nail, and absent skin creases on the dorsal aspect of the distal interphalangeal joints of the index finger. (b) Lower muscle volume of the dorsal muscle groups (triceps brachi) compared to the ventral counterparts (biceps brachi). (c) Audiogram of a female nail-patella syndrome patient, aged 59 years, from family 26, showing significant bilateral hearing impairment. The circles and solid line indicate the pure tone thresholds of the right ear; the crosses and broken line of the left ear; the solid bold line denotes the P95 of presbyacusis, the dotted line the P78.
Pedigrees of families 5 and 26 showing clinical variability of nephropathy, glaucoma, hearing impairment, and nail and orthopaedic findings within and between families and high prevalence of nephropathy in family 26. MILD, MOD, SEV denote mild, moderate, and severe nail and orthopaedic scores according to Farley et al,20 respectively. Asterisks indicate individuals excluded for audiometry due noise trauma or age >70 years since no age-related reference values are available beyond 70 years.
Nephropathy
The results of nephrological investigations are summarised in Table 2. Proteinuria was identified in 13 individuals from six unrelated families and in four sporadic cases by quantitative urinanalysis of a random urine specimen (17/80) (Table 2, Figure 3). Isolated proteinuria was detected in 14.5% (11/76) of individuals, both proteinuria and hematuria in 6.6% (5/76), and isolated microscopic hematuria in 11.8% (9/76). ESRD was found in only one subject of NPS patients overall (1/106). The mean age of individuals with proteinuria (48.1 years, range 8.7–76.2 years) was significantly higher compared to nonproteinuric individuals (36.0 years, range 0.5–81.8 years). Protein–creatinine ratio was 1.6±2.1 g/10 mM (range 0.3–7.5g/10 mM) in proteinuric subjects. GFR was below 60 ml/min/1.73 m2 in 5.3% (4/76) of subjects overall and between 60 and 90 ml/min/1.73 m2 in 34.2% (26/76). Proteinuric patients had a significantly lower GFR compared to nonproteinuric patients (Table 2). Patients with isolated microscopic hematuria had normal GFR (Table 2). Serum creatinine, albumin and cholesterol, and mean arterial blood pressure did not differ between proteinuric and nonproteinuric subjects. Urinanalysis of first morning specimens demonstrated microalbuminuria in 27.5% (14/51) of an unselected series of NPS patients and macroalbuminuria in 3.6% (2/51) (data not shown). In the series of nonproteinuric subjects, 21.7% (10/46) had microalbuminuria detected in the same morning urine specimen. In microalbuminuric subjects, ACR was 85.3±58.3 g/10 mM. Proteinuria was found significantly more frequent in females (33.3%; 15/45) than in males (5.7%; 2/35), adjusted for age (Table 2). The same was true for microalbuminuria, 29.6% (8/27) of females versus 16.7% (4/24) of males, although statistically not significant (P=0.28). We performed a follow-up study of family 26, which has been extensively reported with high prevalence (43.4%; 10/23) of nephropathy 16 years ago.19, 31 Previous investigations demonstrated proteinuria in 33.3% (5/15) of subjects, with a mean age of 48 years (range 33–61 years) of proteinuric subjects at the time of examination. Present studies of the same subjects revealed proteinuria in 40.0% (6/15) with a mean age of 62 years (49–77 years) of proteinuric individuals at the time of examination and progression of proteinuria compared to earlier studies in three out of five subjects (Figure 3). One patient from this family had undergone kidney transplantation at the age of 24 years. Previous ultrastructural studies of renal biopsy specimens of the latter patient demonstrated typical GBM anomalies characteristic for NPS.33 None of the unaffected relatives of NPS family 26 were reported to have nephropathy.
Ophthalmologic involvement
Glaucoma, isolated glaucomatous alteration of the optic disk, and ocular hypertension were found in 35.3% (17/51) of individuals from five out of 16 families (Table 3). Glaucoma was diagnosed in 11.8% (6/51) of subjects: POAG in 3.9% (2/51) or NTG in 7.8% (4/51) (Table 3). Isolated glaucomatous alteration of the optic disk was found in 23.3% (10/43) of subjects with normal IOP not using IOP lowering treatment (data not shown). Ocular hypertension was shown in 3.9% (2/51) of cases. The mean age at which glaucoma or ocular hypertension had been detected was 63.4 years (range 55–72 years). Under the age of 40 years, one case (1/23) showed glaucomatous optic disk excavation and one subject had ocular hypertension. Between 40 and 50 years, 30.8% (4/13) had glaucomatous alteration of the optic disk. Over 50 years, 13.3% (2/15) had POAG, 26.7% (4/15) NTG, 33.3% (5/15) glaucomatous optic disk alterations, and 6.7% (1/15) ocular hypertension. Mean IOP was 15.5 mmHg (range 10–30 mmHg), respectively. No association between excavation of optic disk and IOP could be demonstrated, suggesting that pathological cupping of the optic disk in NPS can occur without elevated IOP. Cataract was found in 7.8% (4/51) of subjects, including congenital cataract in two siblings (family 32). Additional anomalies of the anterior segment included corneal abnormalities, iris pigmentation, and pigment dispersion syndrome. The frequency of ocular findings did not differ significantly between males (6/21) and females (12/30).
Hearing impairment
Otoscopy revealed no pathological findings. Sensorineural hearing impairment was observed in 45.8% (11/24) of NPS subjects from four out of six families examined (Table 3). It was diagnosed bilaterally in 36.4% (4/11) of individuals and unilaterally in 63.6% (7/11) and equally distributed across the various frequencies (0.25–8 kHz). The mean age at the time of detection was 46.7 years (range 17.5–69.2 years). Unaffected family members had normal hearing.
In family 26 with high prevalence of nephropathy, bilateral hearing impairment was demonstrated in a statistical significant proportion of individuals with NPS (P<0.02), whereas in the group of randomly selected NPS patients unilateral hearing impairment was detected significantly frequent (P≤0.02) (Table 3, Figure 3). However, detailed evaluation of the audiograms of individuals diagnosed with unilateral hearing impairment showed fairly symmetrical thresholds suggesting bilateral involvement, although significant scores for both ears were lacking. No significant differences were found in the frequency of hearing impairment in females (7/16) compared to that in males (4/9).
The NPS individual pure tone threshold data were comparable to the 78th percentile of presbyacusis (Figure 2c).25 In total, 52% of the individual thresholds were >P78 at all frequencies. Whether the audiometric results can be interpreted as mildly accentuated presbyacusis or, alternatively, as the development of a normal degree of presbyacusis at an earlier age than is normal cannot be elucidated as yet.
Psychological and health state findings
Response rate of self-report questionnaires on psychological symptoms was 88.2% (75/85). Signs of psychopathology, depression, anxiety, and personality dimensions were comparable to those of the general population. Depression was diagnosed in four subjects (5.3%; 4/75) from four unrelated families. Two out of four individuals with depressive symptoms used antidepressive medication. In total, six subjects used antidepressive medication and one patient used anxiolytics at the time of investigation. The response rate of the health state inventory was 96.4% (81/84). Findings of health status valuations, including mobility, self-care, usual activities, pain/discomfort, and anxiety/depression were also similar to those of the general population.34
LMX1B mutations and FISH results
By mutational screening, 18 different heterozygous LMX1B mutations were identified in 28 unrelated families, including six novel variants (Table 3). In four families in which no LMX1B mutation could be detected, FISH analysis revealed no deletions of the entire LMX1B gene. All four families showed the cardinal findings of NPS. Additionally, two siblings from one of these families (family 32) are known with mild mental retardation and congenital cataract. These families were too small for genetic linkage studies. DNA CGH-microarray analysis is presently being performed to identify possible microdeletions/duplications, including the region encompassing LMX1B.
Genotype–phenotype relationships
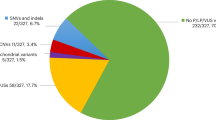
No statistical significant differences between 18 different LMX1B mutations could be established concerning the presence and severity of the diverse renal and extrarenal manifestations (data not shown). However, family 26 (with LMX1B mutation 672+1G>A) demonstrated a high prevalence (53.3%; 8/15) of nephropathy compared to family 4 ((C57S), 0%; 0/8), family 5 ((C63G), 7.6%; 1/13) and NPS patients overall (22.2%; 18/81) (Table 3, Figure 3). Comparison of phenotypic manifestations with LMX1B mutation locations (LIM-A and LIM-B domains versus homeodomain (HD)) demonstrated a significant higher frequency of nephropathy (15/40) and higher level of total urinary protein and albumin excretion in individuals with mutations in the HD than in those with mutations in the LIM domains (3/38), adjusted for age, gender, and family (P=0.046). Analysis of the different putative effects of identified LMX1B mutations (premature truncation of protein, disrupted Zn-finger, or DNA-binding) in relation to the phenotype observed in patients carrying these mutations revealed no statistically significant relationships concerning any of the NPS characteristics.
A significant association was identified between the presence of renal involvement in NPS patients and a positive family history of nephropathy. In total, 53% of the variance in proteinuria measured in a random urine sample could be attributed to the family to which an individual is belonging, while the LMX1B genotype explained only 30% of the variance.
The presence and severity of different NPS manifestations showed high variability at the individual, intrafamilial, and interfamilial level (data not shown). Comparison of extrarenal NPS characteristics between individuals with and without nephropathy is summarised in Table 4 (Figure 3). A statistically significant association was identified between radial head hypoplasia and proteinuria (P<0.01). In contrast to earlier reports35, 36 but consistent with recent observations,17 no relation could be demonstrated between elbow pterygia (5%; 5/100) and nephropathy (data not shown). Although statistically not significant, glaucomatous anomalies or ocular hypertension were observed more frequently in individuals with renal symptoms (63.6%; 7/11) than subjects without nephropathy (35.7%; 10/28) (P=0.11). No significant differences were found with respect to hearing impairment, nail dysplasia, orthopaedic manifestations, and various skeletal anomalies between individuals with and without nephropathy (Table 4).
Discussion
In this study, new clinical and molecular aspects of NPS were identified, establishing that: (a) LMX1B mutations located in the homeodomain and female gender may be associated with a higher risk for developing nephropathy; (b) the family history of nephropathy is important in precipitating the individual risk for developing renal disease; and that (c) NTG and sensorineural hearing impairment expand the NPS phenotypic spectrum.
The prevalence of proteinuria (21.3%) detected by quantitative analysis of a random urine sample is comparable to the frequency (22.3%) demonstrated by dipstick analysis by Sweeney et al.17 The present finding of a female predominance for both proteinuria and microalbuminuria is in contrast with the findings in the general population, where the prevalence of microalbuminuria is about two-fold higher in males.37 The reason for this observation is unclear and needs to be determined. Nephropathy is known to occur during pregnancy only.17 However, none of the present 16 females with nephropathy was pregnant at the time of investigation and six of them had not been pregnant. Moreover, we have to keep in mind that half of the female patients with nephropathy belong to family 26 with a relatively high prevalence of nephropathy and that less males than females were available for investigation from this family. Microalbuminuria, as the earliest clinically measurable finding of changes in glomerular permeability may be an important diagnostic tool, since it represents an early phase in the spectrum of NPS renal disease. Additionally, microalbuminuria is known to play a role in the progression of kidney damage and cardiovascular disease.38 Since GFR was significantly lower in proteinuric individuals compared to nonproteinuric cases, we recommend annual screening of CrC for detecting changes in glomerular filtration in proteinuric patients. In addition to the NPS podocyte disease,7 the severely impaired development of the glomerular capillary network with less fenestrated glomerular endothelial cells as seen in Lmx1b−/− mice16 may contribute to a decreased GFR in NPS.
The prevalence of NTG (7.8%) in the present NPS patients is significantly higher than in the general population (0.6%).39 Based on the finding of POAG, NTG, and isolated glaucomatous optic disk alterations in NPS, we hypothesise that primary structural changes in the membranes of the lamina cribrosa and the trabecular meshwork40 may play a role in NPS glaucomatous optic nerve damage and may result from disrupted collagen expression and/or an irregular arrangement or deposition of collagen fibrils similar to glomerular changes in NPS.
Hearing impairment has previously been described in two out of six subjects from one NPS family, but no additional familial hearing impairment has been reported in NPS.41 We found sensorineural hearing impairment in almost half of the examined NPS individuals. Cosegregation of hearing impairment and NPS and absence of audiological anomalies in unaffected family members further suggest that hearing impairment is another aspect of the NPS phenotype.
Recently, it has been suggested that disrupted midbrain dopamine neuron development and function observed in Lmx1b−/− mice may result in psychological symptoms in human NPS.11, 42 Previous psychological evaluation of self-report questionnaires revealed depression in five out of 10 cases and anxiety symptoms in five out of eight subjects, respectively.42 In the present psychological assessment of 75 individuals, however, we found no evidence for psychological symptoms such as depression and mood symptoms associated with NPS.
Since nephropathy is important for prognosis and possibly indicative for the occurrence of associated NPS manifestations, we performed comprehensive nephrological examinations and compared extrarenal NPS manifestations between the subgroups of individuals with and without nephropathy. A statistically significant association was only identified between nephropathy and radial head hypoplasia, but no common pathogenic mechanism could be proposed for this finding. No association was found between the presence and severity of nail and patellar dysplasia and iliac horns at the individual and familial level, suggesting that NPS manifestations of disrupted dorso-ventral patterning are not necessarily associated. Different spatiotemporal effects of LMX1B mutations or modifier factors may be involved in the highly variable clinical expression of dorsal NPS features.
A significant association was identified between the presence of nephropathy in NPS patients and a positive family history of renal involvement. These findings indicate a higher degree of interfamilial than intrafamilial variability for nephropathy. Individuals within a specific family do not only share the same LMX1B genotype, but also possible environmental aspects and endogenous risk cofactors predisposing to nephropathy, such as blood pressure and modifier genes. However, no relationship could be established between mean arterial pressure and protein excretion (Table 4). The influence of other predisposing risk factors will be the subject of future studies.
Individuals with mutations located in the HD of LMXIB showed significant higher frequency of nephropathy and higher values of proteinuria than individuals with mutations located in the LIM domains. This is in contrast with a previous compilation of LMX1B mutations in NPS, which revealed no such relationship: nephropathy was reported in 55.2% (16/29) of individuals from 20 families with mutations identified in the HD of LMX1B and in 55.6% (5/9) of subjects from four families mutations located within LIM-A or LIM-B domains.43 However, in the latter study, phenotypic information was provided by anamnestic history and/or based on qualitative urinanalysis, and no definition of nephropathy was mentioned. Two other patients with the same mutation have been reported, both are without nephropathy.43 In two other familial cases with a similar LMX1B mutation (672+1G>T), one patient had nephropathy.43 In the current study, the high prevalence of nephropathy in patients with HD mutations is mainly attributable to the large family 26 with a mutation 672+1G>A (8/15 nephropathy). However, if we exclude family 26 from statistical analysis, the relationship between nephropathy and the location of the LMX1B mutation is still significant, emphasizing the presence of this association in additional NPS families (Tables 3 and 4).
Although haploinsufficiency has been hypothesised as the main molecular mechanism of NPS, dominant negative and/or gain-of-function effects cannot be excluded as yet. In fact, the clustering of mutations in the LIM and HD domains, including many that predict premature truncation codons (PTCs), provide strong genetic support for such dominant effects. More insight is needed in the molecular functions of LMX1B to resolve the effects of individual mutations and to elucidate the mechanism that underlies the distinct nephrological phenotypes.
The present inventory indicates that both LMX1B genotype and modifier factors shared among family members may contribute to the development of nephropathy. A possible role of modifier genes in NPS had already been put forward in 1956 by the assumption that the NPS phenotype is modulated by the wild-type LMX1B allele.44 Although haplotype analysis and quantification of the severity of orthopaedic anomalies have given some support to this hypothesis,20 recent single-nucleotide polymorphism (SNP) analyses across the LMX1B gene suggest a relationship between the haplotype of the mutant allele and the severity of nail anomalies.45 Previous studies on the candidate modifier gene CLIM2, encoding a transcriptional activator interacting with LMX1B, revealed no correlation between different CLIM2 polymorphisms and the renal phenotype in our family 26 (LMX1B mutation 672+1G>A) with high prevalence of nephropathy.46 A previous observation15, 47 of ESRD in one, and absence of renal symptoms in the other half of identical male twins with NPS emphasizes a role of external and/or endogenous cofactors in the development and progression of renal disease. In the present study, no association could be identified between the LMX1B genotype and severity scores of various extrarenal NPS characteristics, indicating that different modifier factors may also be involved in extrarenal NPS features.
Further studies on candidate modifier genes are necessary to understand the molecular mechanisms underlying inter- and intrafamilial phenotypic variation and to identify cofactors involved in the progression to glaucoma and terminal renal insufficiency in NPS. Pyrosequencing and whole-genome microarray techniques offer comprehensive genotyping solutions for detecting individual genetic variations, including SNPs, insertion/deletion polymorphisms, and mutations in genetic modifiers. Gene expression profiling of urinary podocytes from NPS patients with and without renal symptoms is presently being performed.
The first indication that hearing impairment and NTG are part of the NPS phenotype and the finding that LMX1B mutation location, family history, and female gender may be associated with the NPS renal phenotype requires confirmation in additional families before applying into counselling. Further investigation and follow-up of additional large LMX1B mutation and clinically well-characterised NPS pedigrees, will be of enormous value to finally elucidate the cofactors underlying the phenotypic variability and the complete phenotype of NPS.
In agreement with the recommendations for clinical management proposed by Sweeney et al,17 we stress the necessity of annual measurement of albumin/creatinine ratio in a first morning specimen starting from birth and additionally annual ophthalmologic screening, including investigation of glaucomatous optic disk alterations from late childhood. NPS patients carrying mutations in the HD of LMX1B, especially from families with a positive family history of nephropathy, require comprehensive renal studies.
Accession codes
References
Dreyer SD, Zhou G, Baldini A et al: Mutations in LMX1B cause abnormal skeletal patterning and renal dysplasia in nail patella syndrome. Nat Genet 1998; 19: 47–50.
Vollrath D, Jaramillo-Babb VL, Clough MV et al: Loss-of-function mutations in the LIM-homeodomain gene, LMX1B, in nail-patella syndrome. Hum Mol Genet 1998; 7: 1091–1098.
Chen H, Lun Y, Ovchinnikov D et al: Limb and kidney defects in Lmx1b mutant mice suggest an involvement of LMX1B in human nail patella syndrome. Nat Genet 1998; 19: 51–55.
Chen H, Ovchinnikov D, Pressman CL, Aulehla A, Lun Y, Johnson RL : Multiple calvarial defects in lmx1b mutant mice. Dev Genet 1998; 22: 314–320.
Morello R, Zhou G, Dreyer SD et al: Regulation of glomerular basement membrane collagen expression by LMX1B contributes to renal disease in nail patella syndrome. Nat Genet 2001; 27: 205–208.
Pressman CL, Chen H, Johnson RL : LMX1B, a LIM homeodomain class transcription factor, is necessary for normal development of multiple tissues in the anterior segment of the murine eye. Genesis 2000; 26: 15–25.
Miner JH, Morello R, Andrews KL et al: Transcriptional induction of slit diaphragm genes by Lmx1b is required in podocyte differentiation. J Clin Invest 2002; 109: 1065–1072.
Dreyer SD, Naruse T, Morello R et al: Lmx1b expression during joint and tendon formation: localization and evaluation of potential downstream targets. Gene Expression Patterns 2004; 4: 397–405.
Ding YQ, Marklund U, Yuan W et al: Lmx1b is essential for the development of serotonergic neurons. Nat Neurosci 2003; 6: 933–938.
Ding YQ, Yin J, Kania A, Zhao ZQ, Johnson RL, Chen ZF : Lmx1b controls the differentiation and migration of the superficial dorsal horn neurons of the spinal cord. Development 2004; 131: 3693–3703.
Smidt MP, Asbreuk CH, Cox JJ, Chen H, Johnson RL, Burbach JP : A second independent pathway for development of mesencephalic dopaminergic neurons requires Lmx1b. Nat Neurosci 2000; 3: 337–341.
Dunston JA, Reimschisel T, Ding YQ et al: A neurological phenotype in nail patella syndrome (NPS) patients illuminated by studies of murine Lmx1b expression. Eur J Hum Genet 2005; 13: 330–335.
Hawkins CF, SMITH OE : Renal dysplasia in a family with multiple hereditary abnormalities including iliac horns. Lancet 1950; 1: 803–808.
Lichter PR, Richards JE, Downs CA, Stringham HM, Boehnke M, Farley FA : Cosegregation of open-angle glaucoma and the nail-patella syndrome. Am J Ophthalmol 1997; 124: 506–515.
Heidet L, Bongers EMHF, Sich M et al: In vivo expression of putative LMX1B targets in nail-patella syndrome kidneys. Am J Pathol 2003; 163: 145–155.
Rohr C, Prestel J, Heidet L et al: The LIM-homeodomain transcription factor Lmx1b plays a crucial role in podocytes. J Clin Invest 2002; 109: 1073–1082.
Sweeney E, Fryer A, Mountford R, Green A, McIntosh I : Nail patella syndrome: a review of the phenotype aided by developmental biology. J Med Genet 2003; 40: 153–162.
Lawler SD, Renwick JH, Wilder-vanck LS : Further families showing linkage between the ABO and nail-patella loci, with no evidence of heterogeneity. Ann Hum Genet 1957; 21: 410–419.
Looij Jr BJ, te Slaa RL, Hogewind BL, van de Kamp JJ : Genetic counselling in hereditary osteo-onychodysplasia (HOOD, nail-patella syndrome) with nephropathy. J Med Genet 1988; 25: 682–686.
Farley FA, Lichter PR, Downs CA, McIntosh I, Vollrath D, Richards JE : An orthopaedic scoring system for nail-patella syndrome and application to a kindred with variable expressivity and glaucoma. J Pediatr Orthop 1999; 19: 624–631.
Chobanian AV, Bakris GL, Black HR et al: Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 2003; 42: 1206–1252.
Cockcroft DW, Gault MH : Prediction of creatinine clearance from serum creatinine. Nephron 1976; 16: 31–41.
National Kidney Foundation: K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Am J Kidney Dis 2002; 39: S1–266.
Carpel EF, Engstrom PF : The normal cup–disk ratio. Am J Ophthalmol 1981; 91: 588–597.
International Organization for Standardization: ISO 7029, 1984. Acoustics-threshold of hearing by air conduction as a function of age and sex for otologically normal persons. International Organization for Standardization. Geneva, Switzerland, 1984.
Derogatis LR, Lipman RS, Covi L : SCL-90: an outpatient psychiatric rating scale – preliminary report. Psychopharmacol Bull 1973; 9: 13–28.
Beck AT, Steer RA, Garbin MG : Psychometric properties of the Beck Depression Inventory. Twenty-five years of evaluation. Clin Psychol Rev 1988; 8: 77–100.
Spielberger CD : Assessment of state and trait anxiety: conceptual and methodological issues. South Psychol 1985; 2: 6–16.
Costa PT, McCreae RR : Revised NEO Personality Inventory (NEO-PI-R) and NEO Five Factor Personality Inventory (NEO-FFI) professional manual. Florida: Odess, 1992.
Brooks R : EuroQol: the current state of play. Health Policy 1996; 37: 53–72.
Knoers NVAM, Bongers EMHF, van Beersum SE, Lommen EJ, van Bokhoven H, Hol FA : Nail-patella syndrome: identification of mutations in the LMX1B gene in Dutch families. J Am Soc Nephrol 2000; 11: 1762–1766.
Silahtaroglu A, Hol FA, Jensen PK et al: Molecular cytogenetic detection of 9q34 breakpoints associated with nail patella syndrome. Eur J Hum Genet 1999; 7: 68–76.
Bongers EMHF, Gubler MC, Knoers NVAM : Nail-patella syndrome. Overview on clinical and molecular findings. Pediatr Nephrol 2002; 17: 703–712.
Kind P, Dolan P, Gudex C, Williams A : Variations in population health status: results from a United Kingdom national questionnaire survey. BMJ 1998; 316: 736–741.
Carbonara P, Alpert M : Hedereditary osteo-onycho-dysplasia (HOOD). Am J Med Sci 1964; 248: 139–151.
Rizzo R, Pavone L, Micali G, Hall JG : Familial bilateral antecubital pterygia with severe renal involvement in nail-patella syndrome. Clin Genet 1993; 44: 1–7.
Verhave JC, Hillege HL, Burgerhof JG, Navis G, de Zeeuw D, de Jong PE : Cardiovascular risk factors are differently associated with urinary albumin excretion in men and women. J Am Soc Nephrol 2003; 14: 1330–1335.
Gerstein HC, Mann JF, Yi Q et al: Albuminuria and risk of cardiovascular events, death, and heart failure in diabetic and nondiabetic individuals. JAMA 2001; 286: 421–426.
Bonomi L, Marchini G, Marraffa M, Morbio R : The relationship between intraocular pressure and glaucoma in a defined population. Data from the Egna-Neumarkt Glaucoma Study. Ophthalmologica 2001; 215: 34–38.
Rehnberg M, Ammitzboll T, Tengroth B : Collagen distribution in the lamina cribrosa and the trabecular meshwork of the human eye. Br J Ophthalmol 1987; 71: 886–892.
Hussain SS, Hope GA : Sensorineural hearing loss and nail patella syndrome. Arch Otolaryngol Head Neck Surg 1994; 120: 674–675.
McIntosh I, Tierney E, Bukelis I et al: Behavioral phenotype of nail-patella syndrome [Abstract]. Am J Hum Genet 2001; S69: 281.
McIntosh I, Dreyer SD, Clough MV et al: Mutation analysis of LMX1B gene in nail-patella syndrome patients. Am J Hum Genet 1998; 63: 1651–1658.
Renwick JH : Nail-patella syndrome: evidence for modification by alleles at the main locus. Ann Hum Genet 1956; 21: 159–169.
Dunston JA, Lin S, Park JW, Malbroux M, McIntosh I : Phenotype severity and genetic variation at the disease locus: an investigation of nail dysplasia in the nail patella syndrome. Ann Hum Genet 2005; 69: 1–8.
Marini M, Bongers EMHF, Cusano R et al: Confirmation of CLIM2/LMX1B interaction by yeast two-hybrid screening and analysis of its involvement in nail-patella syndrome. Int J Mol Med 2003; 12: 79–82.
Meyrier A, Rizzo R, Gubler MC : The nail-patella syndrome. A review. J Nephrol 1990; 2: 133–140.
Hamlington JD, Jones C, McIntosh I : Twenty-two novel LMX1B mutations identified in nail patella syndrome (NPS) patients. Hum Mutat 2001; 18: 458–460.
Clough MV, Hamlington JD, McIntosh I : Restricted distribution of loss-of-function mutations within the LMX1B genes of nail-patella syndrome patients. Hum Mutat 1999; 14: 459–465.
Dunston JA, Hamlington JD, Zaveri J et al: The human LMX1B gene: transcription unit, promoter, and pathogenic mutations. Genomics 2004; 84: 565–576.
Seri M, Melchionda S, Dreyer S et al: Identification of LMX1B gene point mutations in italian patients affected with Nail-Patella syndrome. Int J Mol Med 1999; 4: 285–290.
Acknowledgements
We are grateful to patients and their families for their participation in this study. We thank Sjoukje Nauta and the nephrologists from the Department of Internal Medicine, Radboud University Nijmegen Medical Centre for renal studies, Alfred Pinckers (†) for ocular studies, Mieke Verbrugge for assistance in audiometric examinations, Wim Lemmens for statistical assistance, and Frits Beemer, Ineke van der Burgt, Raoul Hennekam, Conny Schrander, Yvonne Arends, Cora Aalfs, Jeanette Hoogeboom, Marleen Simons, Gretel Oudesluijs, Cor van der Hart, Anton Burgers, and Marinus Kooijman for referring NPS patients. This work was supported by the Council for Medical and Health Research of the Netherlands Organization for Scientific Research (ZON-MW), through Grant 920-03-131.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bongers, E., Huysmans, F., Levtchenko, E. et al. Genotype–phenotype studies in nail-patella syndrome show that LMX1B mutation location is involved in the risk of developing nephropathy. Eur J Hum Genet 13, 935–946 (2005). https://doi.org/10.1038/sj.ejhg.5201446
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejhg.5201446
Keywords
This article is cited by
-
The first presentation of a case of nail-patella syndrome newly diagnosed at the onset of rheumatoid arthritis: a case report
BMC Musculoskeletal Disorders (2024)
-
Ocular manifestations of the genetic causes of focal and segmental glomerulosclerosis
Pediatric Nephrology (2024)
-
Reconstruction of isolated hypoplasia of the patella by a modified Galeazzi procedure: a case report
Journal of Medical Case Reports (2023)
-
The molecular genetics of human appendicular skeleton
Molecular Genetics and Genomics (2022)
-
Letter to the editor in reponse to Louboutin, Wascher, and Neyret in management of patellar problems in skeletally mature patients with nail–patella syndrome. KSSTA 2017 Oct;25(10):3012–3016. https://doi.org/10.1007/s00167-016-4044-y. Epub 2016 Feb 12
Knee Surgery, Sports Traumatology, Arthroscopy (2021)