Key Points
-
Cutaneous tuberculosis is on the rise in immigrant population.
-
Difficulty in diagnosis is due to rarity of condition in developed nations.
-
Provides differential diagnosis of mid facial cutaneous lesions.
-
Provides a diagnostic approach for a dental practitioner in the case of lupus vulgaris.
Abstract
Cutaneous tuberculosis of the orofacial region is a rare condition and when it occurs, can cause confusion regarding the true nature of the lesion. This is compounded by the fact that neither mantoux test nor histopathology is confirmatory. In this report we discuss a case of lupus vulgaris with emphasis on the diagnostic approach to be followed by dental practitioners who come across a similar case.
Similar content being viewed by others
Main
Tuberculosis of the skin is a rare disease accounting for approximately 1% of all reported cases of tuberculosis.1,2 Cutaneous tuberculosis has various clinical manifestations such as plaque, ulcers or mutilating lesions. One progressive form of cutaneous tuberculosis that occurs as a post-primary infection in a person with moderate or high degree of immunity is known as lupus vulgaris.3 Lupus vulgaris (LV) is characterised by plaque with apple-jelly nodule that extends irregularly with scar formation and tissue destruction.3 The lesion typically appears on the head and neck, particularly around the nose.4 Lupus vorax is a variant of LV that affects the nasal cartilage causing ulceration and mutilation.3 We report a case of lupus vulgaris affecting the nose with emphasis on the diagnostic difficulties and treatment protocol.
Case report
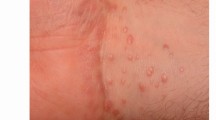
A nine-year-old boy presented with a three-year history of multiple nodules appearing on and around the nose. These increased in size and number despite treatment with topical and systemic antibiotics. These nodules later coalesced to form a plaque on the nose. The lesion was localised on the nose for two years and in the last six months it had extended to involve the right lower eyelid and upper lip, and had lead to the destruction of the nasal tip.
Examination of the patient (Fig. 1) revealed erythrematous scaly plaque with crusting around the nose extending on to the cheeks, inferiorly to the lower lip, angle of the mouth and superiorly to the right lower eye lid. There was destruction of ala nasi, nasal septum and columella. The right lower eyelid showed loss of eyelashes with ectropion of the eyelid. There was conjunctival congestion and epiphora. Swelling and crusting of upper lip and fissuring of the angle of mouth was evident. Mouth opening was limited as upper and lower lip appeared fibrosed and could not be everted.
Multiple bilateral submandibular lymph nodes were palpable, mobile and non tender. Routine haematological and biochemical investigations revealed no abnormalities. Serological test results for Leishmania, syphilis, and human immunodeficiency virus were negative. Para nasal sinus view and chest radiograph findings were normal. Fine needle aspiration cytology of lungs revealed no evidence of tuberculosis. A purified protein derivative test (Mantoux test) was strongly positive, 14 mm diameter after 48 hours. A biopsy of the nasal lesion (Fig. 2) revealed a delicate stroma, markedly amorphous, exhibiting areas of necrosis surrounded by many multinucleated giant cells of langhans type containing many small nuclei disposed to the periphery and a few ill defined epitheloid cells interspersed with mononuclear leukocytes. These features were suggestive of a chronic granulomatous inflammatory reaction. No typical tuberculous follicles or acid-fast bacilli could be identified. Culture was negative for fungi, bacteria and acid-fast bacilli. Mycobacterium tuberculosis DNA was identified from the tissue sample of the lesion subjected to polymerase chain reaction (PCR).
The patient was put on four drug anti tubercular therapy (ATT) consisting of Rifampicin 450 mg one-and-a-half tablets once daily, Isoniazid 300mg one-and-a-half tablets once daily, Pyrazinamide 750 mg half a tablet once daily and Ethambutol 200 mg 1 tablet once daily for a period of two months, following which Isoniazid and Rifampacin were continued for the next four months. For the right eye, moistening eye drops (0.7% hydroxypropyl methyl cellulose) and antibiotic eye ointment (0.3% W/W ciprofloxacin) were used for a period of two weeks.
A review after three months revealed healed lesions on the face (Fig. 3) and improved eye symptoms. ATT was continued for another three months then stopped. The patient is being reviewed every month for assessment of a possible relapse. Reconstructive surgery is planned for a later date.
Discussion
LV usually results from an infection of the skin in a person who has been infected elsewhere with mycobacterium tuberculosis.5 Usually the pathogenic mechanism is contiguous, lymphatic or haematogenous, spread from a tuberculous lesion. In rare situations it can appear at the site of primary inoculation or at the site of a BCG vaccination.6
The disease may have different forms of presentation including plaque, ulcer, mutilating lesions, vegetative, tumour like lesion, and papulonodular lesion. The ulcerative and the mutilating form have the highest tendency for scarring together with deep tissue involvement.3
LV is commonly seen on the face, ears and neck and may heal with scarring. Facial involvement may typically involve the nose and may result in destruction of the nasal and septal cartilage. This mutilating variant of lupus vulgaris is also known as lupus vorax.7,8
The nasal lesion of LV may spread either directly or through lymphatic vessels to the buccal mucosa, palate, gingiva, conjunctiva or oropharynx, giving rise to ulcers or vegetation in these areas.7,9 Further complications include secondary infection of the ulcerative lesion and scarring deformities such as ectropion and microstomia requiring plastic surgery.8,9
In our patient the typical nasal lesion was evident, along with scarring and involvement of upper lip and lower eyelid resulting in ectropion of the eyelid. The differential diagnosis (Fig. 4) should include lupus erythematosus, lymphocytoma, Spitz naevus, syphilis, psoriasis and Bowen's disease for an early nodule or early plaque type. For the more mutinodular or vegetative type the differential diagnosis will include leishmaniasis, leprosy, sarcoidosis, acne rosacea and Wegener's granulomatosus.3,8
Diagnosis of cutaneous tuberculosis is at times difficult because the clinical appearance of the lesion may not always be characteristic and will require multiple investigations (Fig. 5). At times culture for the bacilli may not yield positive results and demonstration of acid-fast bacilli may be difficult especially in patients with chronic lesions and with a high degree of immunity against the infection.6,7,10,11 In the present case acid fast bacilli could not be demonstrated in the biopsy specimen and culture for acid fast bacilli yielded negative results.
Tuberculosis infection is a granulomatous inflammatory reaction in which the granuloma shows central caseous necrosis which is diagnostic, but its absence may not rule out the diagnosis of tuberculosis.11,12,13 In this case there was no evidence of caseation necrosis in the biopsy specimen.
The Mantoux test is positive in most cases of LV6,11,13 as in our case. A negative reaction provides strong evidence against tuberculosis.14 The diagnostic value of a positive tuberculin test is blurred if the subject has a history of BCG vaccination in early life or previous mycobacterial infection. Thus confirmation is not always possible.
A therapeutic trial of anti tubercular drugs is justified if clinical suspicion is strong but cannot be confirmed with biopsy or the Mantoux test. Then diagnosis can be done based on the therapeutic response of the lesion to anti tubercular drugs.14
The absolute criteria for diagnosis of cutaneous tuberculosis are a positive culture of M.tuberculosis from the lesion or successful guinea-pig inoculation, or DNA identification by PCR. In PCR, specific fragments of mycobacterial DNA can be amplified and hence, can be detected even when present only in tiny amounts. It has sensitivity that is equal to or higher than culture, and a high specificity.3,11 Diagnosis in the present case was based on the positive PCR test that revealed presence of mycobacterial DNA.
Conclusion
Since facial lesions of LV occur particularly around the nose, the oral structures in close proximity are naturally involved. Lupus vulgaris must be considered in the differential diagnosis of ulcerative and mutilating lesions of the oro-nasal region.
References
Chen CH, Shih JF, Wang LS, Perng RP . Tuberculous subcutaneous abscess: analysis of seven cases. Tuber Lung Dis 1996; 77: 184–187.
Grosset JH . Present status of chemotherapy for tuberculosis. Rev Infect Dis 1989; II: 347–352.
Gawkrodger DJ . Mycobacterial infections. In: Rook A, Wilkinson DS, Ebling FJG (Eds). Textbook of Dermatology, 6th ed. Oxford; Boston: Blackwell Scientific, 1998; V.2, Chap. 28, p1194.
El-Gatit AL, EL-Deriny, Mahmoud AA and Ashi AS . Presumed periorbital lupus vulgaris with ocular extension. Ophthalmology 1999; 106: 1990–1993.
Sehgal VN, Jain MK and Srivastava G . Changing pattern of cutaneous tuberculosis — A prospective study. Int J Dermatol 1989; 28: 231–236.
Marcoval J, Servitje O, Moreno A, et al. Lupus vulgaris. Clinical, histopathologic, and bacteriologic study of 10 cases. J Am Acad Dermatol 1992; 26: 404–407.
Farina MC, Gegundez MI, Pique E, et al. Cutaneous tuberculosis. Clinical, histopathologic, and bacteriologic study of 10 cases. J Am Acad Dermatol 1995; 33: 433–440.
Freitag DS, Chin R . Facial granuloma with nasal destruction. Chest 1998; 92–3: 422–423.
Kounis NG, Constantinidis K . Lupus vulgaris: a rare dermal involvement. Practice of medicine 1980; 224: 1284–5.
Serfling U, Penneys NS, Leonardi CL . Identification of Mycobacterium tuberculosis DNA in case of lupus vulgaris. J Am Acad Dermatol 1993; 28: 318–22.
Sehgal VN, Jain MK and Srivastava G . Changing pattern of cutaneous tuberculosis — A prospective study. Int J Dermatol 1989; 28: 231–236.
Walter JB, Hamilton MC, Israel MS . Tuberculosis, Leprosy, Syphilis and Actinomycosis. In principles of pathology for dental students. 4th edition. Churchill living stone. pp213–223.
Kumar B, Rai R, Kaur I, et al. Childhood cutaneous tuberculosis: a study over 25 years from northern India. Int J Dermatology 2001; 40: 26–32.
Kakakhel K, Fritsch P . Cutaneous Tuberculosis. Int J Dermatol 1989; 28: 355–362.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed paper
Rights and permissions
About this article
Cite this article
Thomas, S., Suhas, S., Pai, K. et al. Lupus vulgaris — Report of a case with facial involvement. Br Dent J 198, 135–137 (2005). https://doi.org/10.1038/sj.bdj.4812038
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.4812038
This article is cited by
-
Lupus vulgaris mimicking hemangioma diagnosed 42 years after onset: a case report
Journal of Medical Case Reports (2015)
-
Lupus vulgaris als destruierender Nasen- und Gesichtstumor
HNO (2009)