Key Points
-
Previous published data have suggested that medically compromised children receiving dental treatment under GA have had more extractions and less restorations than the ASA I and II children undergoing similar procedures. This study demonstrates that this is not the case.
Abstract
Objective To compare the level of dental disease and the pattern of dental treatment under controlled airway general anaesthesia for ASA I and II children and ASA III and IV children in two hospitals.
Design Prospective analysis.
Setting Hospital and postgraduate dental teaching institution, UK 1996 – 2000.
Subjects and methods During a four-year period (1996–2000), data were collected on children aged 1 to 16 years who were admitted for treatment of dental caries under general anaesthesia.
Outcome measures Levels of dental disease (dmft/DMFT), treatment provided.
Results A total of 515 ASA I and II and 430 ASA III and IV children were treated. The dmft and DMFT values of the ASA I and II children were significantly higher than those of the ASA III and IV children (p = 0.03). A significantly greater number of restorations and fissure sealants were carried out for permanent teeth in ASA III and IV children (p < 0.001). The number of extractions for both primary and permanent teeth was significantly greater in the ASA I and II group (p < 0.05).
Conclusions The ASA III and IV children had significantly lower levels of dental caries than the ASA I and II children and received a higher level of preventive and restorative care.
Similar content being viewed by others
Introduction
Earlier diagnosis and new treatment methods have resulted in an increased number of children surviving chronic childhood diseases.1 These children are at a greater risk of life threatening consequences from an oral focus of infection.
Like healthy children, chronically sick children may suffer from dental anxiety or phobia and may be unable to tolerate treatment under local anaesthesia alone or together with inhalation sedation.2 For these patients it may be necessary to resort to general anaesthesia (GA). General anaesthesia may also need to be prescribed in very young patients where extensive treatment is required and where there is an inability to cooperate.
The use of general anaesthesia is declining, with a higher percentage of GAs administered to children who are medically compromised.3 There is data indicating that the treatment is modified for chronically sick children,4 with significantly greater numbers of extractions and fewer restorations carried out in this group. The possibility that these children have different levels of disease cannot be excluded. The aim of this study was to compare the level of dental disease and pattern of dental treatment for a group of ASA (American Society of Anesthesiologists Physical Status Classification5) I and II and a group of ASA III and IV children receiving comprehensive dental treatment under GA.
Patients and Methods
Data for this prospective analysis were collected from children as they attended either the Eastman Dental Hospital and Institute (EDH) or Great Ormond Street Hospital for Children (GOS), over a four-year period (January 1996 – January 2000). EDH is a postgraduate dental teaching hospital and GOS is a major tertiary referral centre for paediatric specialties.
The source of patients at both hospitals was from general dental practitioners (GDPs) and community dental officers (CDOs) directly to the dental department, referral from other paediatric specialties within the hospital or self referrals (EDH only). The children were treated under GA because of an inability to accept treatment under local anaesthesia, or local anaesthesia with inhalation sedation.
All children were seen for a preoperative assessment. At this appointment, administrative and clinical details relating to the patient were recorded. Patients treated at EDH had been classified as ASA I and II patients and were treated as day stay cases. Patients treated at GOS were classified as ASA III and IV patients with the majority being admitted for overnight stay for extensive pre-anaesthetic preparations. These patients were usually discharged on the day of operation, or the next day.
The teeth were examined visually, using a mouth mirror and operating light, for dental caries, using the WHO criteria.6 Each surface was charted for caries and the indices were recorded as dmfs/dmft and DMFS/DMFT. Clinical data were completed with findings from a radiological examination using a dental panoramic tomography or bimolar radiographs. This examination was carried out either at the pre-anaesthetic appointment or if the child was uncooperative when they were anaesthetised.
Once treatment was completed the procedures carried out were recorded. This comprised the number of restorations, type of restorative material used, number of fissure sealants, number of pulp treatments and the number of primary and/or permanent teeth extracted. In addition the grade of operator was recorded.
At the end of the treatment session a senior house officer transferred the data recorded on the clinical data sheets on to matched electronic database forms. All numerical and categorical data were entered into a Microsoft Access database. Reports generated in Microsoft Excel format were exported for checking and subsequently imported to Statistical Package for Social Sciences program (SPSS) for Windows for cross tabulation and summarisation of the data.
Ethical approval for the study was granted by the Great Ormond Street Hospital for Sick Children NHS Trust.
Results
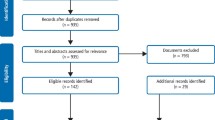
There were a total of 1,389 records in the database. Those patients who were over 16 years old, whose records were incomplete or who had been treated for reasons other than caries, for example orthodontic extractions, were excluded from the study. The final number of patients was 945. There were 515 ASA I and II children at EDH and 430 ASA III and IV children at GOS. All data were subjected to the Shapiro Wilk test for normality. The data were not normally distributed so the Mann-Whitney U test for independent groups was used for statistical comparison. Summary data are presented as median values and the 95% reference range (2.5 percentile to 97.5 percentile).
Patient characteristics
The age distribution of both groups of children was very similar with an age range of 1 year 2 months to 16 years at EDH and of 1 year 7 months to 16 years at GOS. There was no significant difference between the 2 groups (p = 0.51). The average age at operation was 7 years 6 months at EDH and 7 years 7 months at GOS. There were 530 males and 415 females, with gender distribution being similar.
At EDH two consultants treated the majority (42%) of the patients, whilst 38% were treated by the specialist registrars and the remaining 19% by the senior house officers. At GOS the majority (58%) of the patients were also treated by one consultant, 29% by the senior house officers and 13% by the specialist registrar. All treatment was supervised by a consultant.
Distribution of medical conditions
The ASA II, III and IV children were classified into nine main groups according to their medical diagnosis: cardiac, neurology, craniofacial, dermatology, immunology and viral infections, bleeding, renal/hepatic, respiratory and other (primary multiple system disorders, metabolic and endocrine disorders). The percentage of patients within the groups were compared between the two hospitals. Seventy per cent of the patients at EDH were healthy (ASA I, n=359). The next largest group had respiratory disorders (ASA II, n=71, 14%) mainly suffering from well-controlled asthma. Very few medically compromised patients were treated at EDH and these were all ASA II. At GOS the largest group was those with cardiac disorders (n=108, 25%), 78 of whom had congenital heart disease (all children at GOS were ASA III and IV).
Level of dental caries
The children were divided into two age groups: those aged 1–11 years (primary dentition) and those aged 6–16 years (permanent dentition). Analysis of the 1–11-year-olds age group resulted in a significantly higher (p < 0.001) dmft at EDH (median = 8) when compared with GOS (median = 6) (Table 1). There was also a significantly higher DMFS (median = 3) and DMFT (median = 2) in children aged 6-16 years old treated at EDH compared with the DMFS (median = 1) and DMFT (median = 1) at GOS (Table 2).
Pattern of dental treatment (Table 3)
Restorations
This included the sum of preventive resin restorations, tooth coloured restorations, amalgam restorations and stainless steel crown restorations. Overall, there was a significantly greater number of restorations (p = 0.03) per child at GOS compared with EDH (median = 2 at GOS and EDH). For the primary dentition alone, the figures were not statistically significantly different (p = 0.56).
Pulpal Treatment
Very few primary teeth were pulpally treated. Fifteen vital pulpotomies were carried out at GOS, 13 vital pulpotomies at EDH and one non-vital pulpotomy at EDH.
Primary tooth extractions
There was no significant difference (p = 0.07) in the number of primary teeth extracted between both groups (median number of teeth extracted was 4 at EDH and GOS).
Permanent tooth extractions
There was a significantly greater number of permanent extractions (p < 0.001) at EDH (median = 0 at EDH and GOS).
Preventive treatment
Preventive treatment was limited to fissure sealants with significantly more (p < 0.001) being carried out at GOS (median = 0 at EDH and GOS).
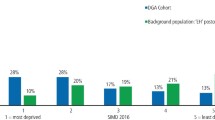
Data were further analysed by medical condition. The median number of total teeth extracted per healthy patient was 5 and was higher or equal to most of the chronically sick groups, with only the immunological/viral group having a higher median value (6). The median number of restorations placed per patient was highest for the endocrine group (3) and lowest for the bleeding group (1) (Fig. 1). Figure 2 shows the relative proportions of restorations and extractions and there is an overall predominance of extractions over restorations in all the groups with a restoration:extraction ratio of approximately 1:2.
Discussion
Study design
This study was a prospective analysis on the prevalence of dental disease and the pattern of dental treatment carried out under GA in two hospitals. At GOS, one consultant carried out most of the treatment. The remaining treatment was carried out by specialist registrars or senior house officers under direct supervision. At EDH the treatment was carried out or supervised by two consultants. It could be argued that the difference in treatment between the two hospitals was caused by differences in operator technique, materials available etc. Although it is not possible to discount this possibility, it is of note that the consultant carrying out treatment at the GOS also carried out some of the treatment at the Eastman. In addition facilities available were similar in both locations.
Sample (Table 4)
The number of medical conditions subgrouped, demonstrates that there is extensive dental disease across the spectrum of chronically sick children. The results obtained were a product of many factors, and cannot be taken to represent the prevalence of dental disease for a specific medical condition. A child may have more than one medical condition and it was the dental clinician's judgement as to which was the more relevant medical condition. This condition was then noted on the clinical data sheet which only accepted one entry in the table for medical diagnosis. The cardiac group represented 25% of all sick children which may be either a reflection of the awareness of paediatric cardiologists of the potential hazard of oral sepsis or that there is a large number of children with cardiac problems at GOS.
Dental caries
This study reports a lower level of caries in children at GOS (ASA III and IV) receiving dental treatment under GA. The potential of the existence of an oral focus for systemic sepsis can be life threatening in children with certain medical disorders. This encouraged early referral and prompt admission for dental treatment under GA at a lower level of caries. As a result of the medical care, chronically sick children may be less able to cooperate or they may be mentally or physically disabled and thus need GA, whereas with healthier children, acclimatisation to dental treatment may be more successful. Another possible reason may be that efficient targeting of the chronically sick child at an early age and combined appointments at GOS with dental advice given has resulted in increased parental awareness.
Interestingly the difference in dmfs in the 1 – 11 year age group between the two hospitals was not statistically significant (p = 0.227), yet dmft was (p < 0.001). This might represent the greater error incorporated when measuring dmfs.
Pattern of dental treatment
In the primary dentition more teeth were extracted than restored in both groups. Previous studies have recorded averages of 3.3 and 3.87,8 teeth extracted per child. If mean values are calculated for the data from this study the value is 5.5. This may indicate not only extensive treatment needs in patients referred to both hospitals, but also a radical approach to treatment provision in order to avoid the need for further GA.
In the permanent dentition, there were more teeth restored than extracted in chronically sick children, but less teeth restored than extracted in the case of the healthy children. This may have been due to:
-
Operator variance
-
Less advanced caries in the sick children.
The previous report on dental care provided in the two hospitals had less extractions in both dentitions in the ASA I and II group compared with the ASA III and IV group with a restoration:extraction ratio of 1:3 for the ASA I and II group and 1:2 for the ASA III and IV group.4
The predominance of extractions over restorations in sick children, as shown in Figure 2, was in agreement with the previous report from the two hospitals where the treatment philosophy was regarded as the reason for the predominance of extractions. Extraction is often the treatment of choice when taking into account the underlying medical condition and that treatment under GA should be more radical.
For the pooled data, the overall restoration to extraction ratio in this study was approximately 1:2. This is similar to that of previous investigators9,10 who concluded that in order to reduce the risk of a repeat general anaesthetic for dental treatment, a radical approach was used. The ratio is in contrast to that reported from other centres with an overall predominance of restorations over extractions.3,11
It is not possible to reliably identify why there was a higher level of preventive and restorative care at GOS compared with EDH. Possible reasons are:
-
Patients referred for treatment of dental caries under GA at EDH are usually referred following several attempts at acclimatisation when simple procedures such as fissure sealants may have been carried out as part of the attempt at acclimatisation to treatment.
-
At GOS it may be possible that the children were referred at an earlier stage, with lower levels of dental disease, as soon as carious lesions are noted. This may be because these children are under constant medical care and have greater ease of access to the specialist dental care available at GOS. It was therefore possible to restore more carious lesions and also to use the opportunity provided by the GA to carry out the preventive care such as fissure sealants.
-
The difference in treatment may have been related to treatment philosophy and policy at the centres at least as much as to differences in the groups served.
Conclusions
All children admitted for treatment of dental caries under controlled airway general anaesthesia had high levels of decayed, missing and filled teeth in both dentitions. The children at GOS (ASA III and IV) had significantly lower levels of dental caries in both dentitions than the children at EDH (ASA I and II). They received a significantly higher level of preventive and restorative care and the mean number of teeth extracted per patient was significantly lower. There was an overall predominance of extractions over restorations in both groups of children which may be attributed to the higher level of disease and the treatment under general anaesthesia being more radical.
References
Gortmaker SL, Sappenfield W . Chronic childhood disorders: prevalence and impact. Pediatr Clin North Am 1984; 31: 3–18.
Tyrer GL . Referrals for dental general anaesthesia - how many really need GA? Br Dent J 1999; 187: 440–443.
Wong FS, Fearne JM, Brook AH . Planning future general anaesthetic services in paediatric dentistry on the basis of evidence: an analysis of children treated in the Day Stay Centre at the Royal Hospitals NHS Trust, London, between 1985–95. Int Dent J 1997; 47: 285–292.
Harrison MG, Roberts GJ . Comprehensive dental treatment of healthy and chronically sick children under intubation general anaesthesia during a 5-year period. Br Dent J 1998; 184: 503–506.
American Society of Anesthesiologists. http://www.asahq.org/clinical/physicalstatus.htm
Oral Health Surveys. Basic Methods, 3rd Ed. Geneva. World Health Organisation, 1987.
Rule DC, Winter GB, Goldman V, Brookes RC . Restorative treatment for children under general anaesthesia. The treatment of apprehensive and handicapped children as clinic out- patients. Br Dent J 1967; 123: 480–484.
Mason C, Holt RD, Rule DC . The changing pattern of day-care treatment for children in a London dental teaching hospital. Br Dent J 1995; 179: 136–140.
Smallridge JA, Al Ghanim N, Holt RD . The use of general anaesthesia for tooth extraction for child out- patients at a London dental hospital. Br Dent J 1990; 168: 438–440.
O'Sullivan EA, Curzon ME . The efficacy of comprehensive dental care for children under general anesthesia. Br Dent J 1991; 171: 56–58.
Tarjan I, Mikecz G, Denes J . General anaesthesia of out-patients in pedodontics. J Int Ass Dent Child 1990, 20: 59–61.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed paper
Rights and permissions
About this article
Cite this article
Camilleri, A., Roberts, G., Ashley, P. et al. Analysis of paediatric dental care provided under general anaesthesia and levels of dental disease in two hospitals. Br Dent J 196, 219–223 (2004). https://doi.org/10.1038/sj.bdj.4810988
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.4810988
This article is cited by
-
Do paediatric patient-related factors affect the need for a dental general anaesthetic?
British Dental Journal (2022)
-
A rapid review of variation in the use of dental general anaesthetics in children
British Dental Journal (2020)
-
Dental characteristics and according treatments of children under GA in Germany
European Archives of Paediatric Dentistry (2019)
-
Neighbourhood incidence rate of paediatric dental extractions under general anaesthetic in South West England
British Dental Journal (2018)
-
Treatment outcomes of using inhalation sedation for comprehensive dental care
European Archives of Paediatric Dentistry (2018)