Key Points
The stages of fitting and cementation of crowns are considered including:
-
The clinical stages of try-in and adjustment of restorations prior to cementation
-
Conventional and adhesive cements
-
A rationale for the use of different cements based on their various physical and chemical properties
-
Crown cementation with conventional cements
Key Points
Crowns and extra-coronal restorations:
-
1
Changing patterns and the need for quality
-
2
Materials considerations
-
3
Pre-operative assessment
-
4
Endodontic considerations
-
5
Jaw registration and articulator selection
-
6
Aesthetic control
-
7
Cores for teeth with vital pulps
-
8
Preparations for full veneer crowns
-
9
Provisional restorations
-
10
Impression materials and technique
-
11
Try-in and cementation of crowns
-
12
Porcelain veneers
-
13
Resin bonded metal restorations
Abstract
Having successfully negotiated the planning, preparation, impression and prescription of your crown, the cementation stage represents the culmination of all your efforts. This stage is not difficult, but a successful outcome needs as much care as the preceding stages. Once a restoration is cemented there is no scope for modification or repeat. You have to get it right first time. Decemented crowns often have thick layers of residual cement suggesting problems with either initial seating or cement handling. When the fate of restorations costing hundreds of pounds depends on correct proportioning of cements and the quality of the mix, the value of a well-trained and experienced dental nurse is easy to see. Both dentist and nurse need a working knowledge of the materials they are handling.
Similar content being viewed by others
Main
Crown seating relies on a satisfactory try-in and this subject will be covered first. We will then consider the topics of cements, their selection and usage.
Try-in procedure for crowns
This involves three stages: firstly pre-operative evaluation of crown on its die, secondly seating on the tooth and finally evaluation of the seated crown.
Checking the crown on the die
It is always worth checking the fit of the crown on the cast before trying it in the patient. In this way problems involving marginal fit, aesthetics and articulation can be anticipated prior to try in. Always check the fit surface of the crown for defects and the die for damage, preferably with a good light and under magnification (Table 1). Detecting these problems before try-in will allow you either to address the problem yourself or to negotiate with your laboratory from a position of strength. It is surprising how often clear ledges or deficiencies can be detected at this stage. Subsequent stages then rely on the crown being checked in the mouth and then often back on the die again when there is a problem with the fit.
Seating the crown
Having checked the crown on the cast, any temporary restoration is removed and the preparation is carefully cleaned of all residues of temporary cement, especially in retention grooves. The try-in procedure can normally (though not always) be accomplished without the need for local anaesthetic. This is advantageous in that the patient's tactile sense is not impaired which is valuable in assessing the occlusion and tightness of proximal contacts.
The crown should be tried in without forcing it onto its preparation; if it fails to seat there are a range of reasons why this may have happened. It pays to use a systematic approach to localise problems:
-
1
First, ensure there is no retained temporary cement or trapped gingival tissue
-
2
Then check and adjust tight proximal contacts (see following section) as these often prevent seating. Also check the original cast for damage to the stone in these contact areas
-
3
Then re-check the crown for the most obvious laboratory errors, including casting blebs, damaged or chipped dies or grossly overextended margins. Casting blebs can be removed with a bur. Over-extended margins should be adjusted from the axial surface, not from underneath (Soflex discs are useful for this purpose – see Fig. 1). To avoid the abrasive dragging metal over the margin, run the disc so that the abrasive travels in the direction of the occlusal surface, not towards the margin
-
4
Where the crown still does not seat burnish marks on the internal walls of a sandblasted metal crown may indicate where it is binding. The identification of these points may be aided by the use of disclosing wax or aerosol sprays. Any imperfections may be lightly ground with a bur or stone before retrying the crown.
With modern day addition silicones, impression distortion is an unusual cause of ill-fitting restorations but may be responsible where no apparent fault can be detected on restoration or die. Problems can occur where an impression is removed too soon or where unset impression material results from glove contamination (look out for the tell tale smear of unset impression material on the surface of the cast). If you cannot get the crown to seat easily and can find no obvious reason, you may rightly suspect that there is an impression distortion. In that case, save time and just take a new one.
Finally, it is important to distinguish between a crown that rocks on its preparation because of binding somewhere on the fit surface and one that just has a loose fit resulting from the use of die spacer. In fact, tightly fitting crowns confer no additional retention after cementation1 and may interfere with seating.
Assessment of the seated crown
There is no point in making a detailed assessment of proximal contacts, marginal fit, aesthetics and occlusion until the crown is seated fully. Once you have got to this stage, providing you and the laboratory have taken care with preceding clinical and technical stages, minimal or no adjustment should be necessary. Again it is important to adopt a systematic approach.
Proximal contacts
The tightness of proximal contacts can be tested with dental floss and should offer some resistance but not make its passage too difficult. If these are too tight they can be ground a little at a time and polished. This requires the greatest care as it is easy to open the contact accidentally, and it is very problematic trying to rebuild it at this stage. Prior to adjustment it may be helpful to mark the proximal contact by sandwiching a small piece of articulating paper between crown and tooth either on the cast or in the mouth.
Open contact points occur less frequently and can only be modified by returning the crown to the laboratory for addition of porcelain or gold solder.
Assessment of marginal fit
Crowns really must have an accurate marginal fit if you intend them to survive in the long term. There is a full spectrum of fit, from perfection (which is probably rarely achieved) to open margins around the entire crown. It is up to you, your own clinical standards and perhaps your patient at what point on that spectrum you decide that the marginal fit becomes unacceptable. A combination of clinical experience and empirical data suggest a marginal opening of 100 mm2 is at the borderline of acceptability, especially where the margin can only be probed.3 Maintaining the highest possible clinical standards at this stage has long-term benefits; ill-fitting margins will render the tooth more susceptible to cement dissolution, plaque retention and recurrent caries. Defective subgingival margins compromise gingival health by an alteration in local bacteria.4
Poor fit can present as a gap or an overhanging margin (positive ledge) or deficient margin (negative ledge). Overextended margins and positive ledges may be corrected by adjusting the crown from its axial surface until it is possible to pass a probe from tooth to crown without it catching. A larger problem, necessitating that the crown be remade if it is unacceptable, occurs when a margin remains deficient or has a negative ledge.
Gold restorations should have their accessible margins burnished before cementation. The set cement is likely to be cracked if the margin is burnished afterwards. There is no evidence that burnishing improves longevity but it can insure that a discerning patient does not catch a fingernail at the margin! The procedure involves dragging the gold from restoration to tooth using a rotary instrument such as a green stone or steel finishing bur. Where only minimal burnishing is needed a sharp hand instrument such as a proprietary gold knife or half Hollenback instrument is useful. Once burnished the restoration must be re-polished taking care to avoid the fine edge of marginal gold.
Aesthetics
For porcelain crowns, some adjustment of shape and shade is possible at this stage but it is best to ensure minimal adjustment by following the advice given in Part 6 of the series.
Grinding with diamond burs can alter crown contours and porcelain additions can be made to metal ceramic crowns if necessary. Shades that are slightly too light may be darkened by the addition of stain and re-firing while all ceramic crowns with no cores may have their shade modified slightly by the luting composite in the same way as veneers. If you anticipate the need for substantial adjustments, a try-in at biscuit bake can be specified so that the crown can be glazed when you are happy with the final appearance. Obviously the patient will need to see the restoration and comment on it prior to cementation. If the shape and shade are clearly unacceptable it is better to acknowledge this rather than risk a dissatisfied patient with the possibility of having to cut off the restoration and repeat all the preceding stages.
Assessment of the occlusion
Assessment of the occlusion It is important you have a clear idea of the pattern of occlusal contact you are trying to achieve
The occlusion is the last assessment to make, but there is no point thinking about making any adjustment to the occlusal surface until the crown is finally seated. It is then best to remove it and identify a pair of adjacent occluding teeth, termed index teeth, which, after re-seating, can be used to assess visually, and with shim stock, how much adjustment is needed.
Visually checking the occlusion gives only a gross indication of the amount of adjustment needed; articulating foils and shim stock are needed too. Figure 2 shows shim stock, which is a 10 μm thick Mylar film, held in mosquito forceps and used as a feeler gauge between occluding teeth. Shim stock can be bought from dental suppliers or can be made, very inexpensively, in the dental surgery by passing a 'space blanket' (the sort of thing marathon runners wrap around themselves after a race, available at camping shops) through an office shredder and then cutting it into 2 cm lengths.
Miller's forceps, used to support articulating foils so that they do not crumple during intra-oral placement, are also an advantage (again look at Fig. 2). Some articulating papers resemble blotting paper in consistency and thickness. They are prone to leave false marks and may alter the patient's position of closure. These papers can be as thick as 200 μm, which is over ten times as thick as the best thin foils such as GHM (GHM Occlusion Prüf Folie, Germany),5 which are infinitely preferable. Despite their slightly higher cost, the accuracy and precision with which they will mark a restoration can save a great deal of time and effort provided the teeth are dry.
With posterior teeth, both restoration and adjacent teeth should hold shim stock firmly in the intercuspal position (ICP). With anteriors, if the other incisors hold shim stock lightly the restoration should be made to do so too. Failure to do so can result in the crowned tooth being overloaded, which in turn can cause pain, mobility, fracture or displacement. As well as using shim stock and articulating foils, it is also worth listening to the occlusion with and without the crown in place as small occlusal discrepancies can readily be heard with the teeth being tapped together.
Dentists will often have a favourite bur for occlusal adjustment. We prefer a large flame shaped diamond in an air rotor or speed increasing handpiece. Occasionally, it may be necessary to adjust the tooth opposing a restoration to avoid crown perforation or exposure of rough opaque porcelain. Such adjustments should be planned with the patient's consent and not sprung on them part way through the procedure. A thickness gauge (eg Svensen Gauge) is invaluable for predicting areas vulnerable to perforation.
Once ICP has been re-established the excursions can be checked, preferably with a different coloured foil (eg red). ICP contacts are then re-marked with the original colour (eg black) allowing the excursive contact to be differentiated and refined. The decision about whether the restoration is to be involved in guiding jaw movement (which it often is with anterior teeth) or whether there should be disclusion (as often occurs posteriorly) should have been made well before this stage and it is important you have a clear idea of the pattern of occlusal contact you are trying to achieve. Finally, it is worth guiding back the mandible into the retruded path of closure to ensure the restoration is not introducing a new deflective contact.
Occasionally, a restoration will be short of occlusion. This is used as a deliberate ploy in some laboratories to eliminate the clinical need for occlusal adjustment. A thin card spacer placed over the cast of the opposing tooth creates clearance. This may seem an innocuous, perhaps even a desirable practice, but can result in serious immediate problems presenting where multiple restorations are fitted. The lack of contacts can affect occlusal stability whilst destructive interferences may occur as teeth erupt back into occlusion. It may often be acceptable to monitor infra-occluding restorations and adjust interferences as necessary. In more critical cases occlusal additions of porcelain or solder may be indicated or the restoration remade. The point is that it should not be necessary to do this at all because all of these problems can be avoided by taking care at the preceding stages, especially with impressions (including opposing impressions), jaw registration and temporary restorations.
Finishing and polishing
The final stage prior to cementation is polishing. A rough surface, especially in porcelain, will rapidly wear the opposing tooth6 and so it is very important to use a sequence of abrasives designed for the material in question to achieve a smooth surface. Details of the materials we use are shown at the end of the article. Metal surfaces can be finished with finishing burs followed by rubber abrasive points (Kenda: blue, brown and green). Abrasive discs (eg Soflex) are useful for flat areas such as proximal contact points and can be used on either metal or porcelain. Porcelain can be also be finished with composite finishing diamonds (Premier: yellow and white stripe), but a light touch and water spray is needed to avoid stripping off the diamond coating. Further finishing is achieved with rubber abrasive points (Kenda: white) followed by a felt wheel or rubber cup charged with diamond polishing paste (Super Diglaze). Alternatively, a metal ceramic crown can be reglazed.
Cements
When the fit of the crown is considered satisfactory and all adjustments have been made, the crown can be cemented using one of the materials described in this section.
Cements may be classified as soft or hard. Soft cements can be used for provisional cementation of definitive crowns when a trial assessment period is needed, for example if the occlusion or aesthetics is being significantly altered. Hard cements are used for definitive cementation. This article deals principally with hard cements.
Hard cements
Many types of hard cement have been developed and continue to be available. This diversity of choice suggests no one cement meets all of the requirements of an 'ideal cement' however some are more suitable than others for certain applications.
There are essentially three types of hard cement: conventional, resin or a hybrid of the two. Conventional cements (eg zinc phosphate, zinc polycarboxylate and glass ionomer) rely on an acid-base reaction resulting in the formation of an insoluble salt (the cement) and water. Resin cements set by polymerisation.
The mechanisms by which cements secure restoration to prepared tooth include non-adhesive luting, micro-mechanical bonding and molecular adhesion. The mechanisms of non-adhesive luting and micro-mechanical retention are the main methods of action of conventional cements. Molecular adhesion on the other hand is more significant in the case of resin cements and hybrid cements. Although some conventional cements have adhesive properties, such as zinc polycarboxylate and GIC, these are limited by the cement's tensile strength. Furthermore, adhesion to noble metals is negligible but can be improved in the case of GICs by the use of tin-plating. Texturing the fitting surface of the crown, as after sandblasting, increases the resistance of the cement to dynamic lateral loading.7
We will now go on to discuss the advantages and disadvantages of each of the major groups of cements and make recommendations for their use.
Zinc phosphate cement
Advantages
-
Long track record
-
Good compressive strength (if correctly proportioned)
-
Good film thickness
-
Reasonable working time
-
Resistant to water dissolution
-
No adverse effect on pulp although initially acidic
Disadvantages
-
Low tensile strength
-
No chemical bonding
-
Not resistant to acid dissolution
Recommendations
-
Good default cement for conventional crowns and posts with retentive preparations
-
Working time can be extended for cementation of multiple restorations by incremental mixing and cooled slab
Zinc phosphate has the longest track record and has remained popular for luting purposes due mainly to its high compressive strength, relatively long working time and ability to form a low film thickness between crown and tooth. Look at Table 2 for the relative physical properties of cements and it is clear that in common with the other conventional cements, zinc phosphate possesses high compressive strength but low tensile strength. It is this low tensile strength, which dictates the importance of preparation geometry in reducing the development of disruptive tensile stresses within the cement lute resulting in loss of retention of the restoration.
The retaining action of zinc phosphate cement is one of micromechanical interlocking between surface irregularities of the crown and tooth. It does not bond to tooth substance or crown material.
It is normally supplied as a powder (essentially zinc oxide) and liquid (phosphoric acid buffered with zinc and aluminium ions), which are mixed together by hand. The proportions of powder and liquid are not normally measured and therefore care must be taken to produce a 'mix', which provides a cement of low initial viscosity to form a thin film, but with sufficient powder incorporated to give adequate strength once set.8 The powder should be incorporated in increments to prevent the cement setting too quickly as a result of the exothermic reaction. A slab cooled in the refrigerator can further extend working time. The consistency of zinc phosphate may be checked by lifting the cement on the spatula and holding it over the slab. It should string out slightly between the spatula and slab before running back onto the slab. If it requires to be pushed off the spatulait is too thick and conversely, if it runs off too quickly it is not thick enough. Given how critical this is, it is worth making sure that you and your chair side assistant both understand fully what is required, and are prepared to stop and mix again if a problem arises.
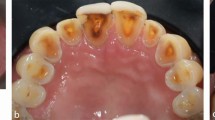
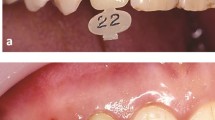
All cements are to some extent soluble. Zinc phosphate has a low solubility in water but erosion leading to loss of the cement lute and failure of the restoration is not normally associated with this cement, crowns tending to be lost more because of a poor retentive design of the preparation. However, cement erosion is seen in patients with acid regurgitation (Fig. 3).
Historically, zinc phosphate cements have been identified as having a potential irritant effect on the pulp.9 This has been attributed to the low pH of the cement at the time of cementation, but preparation trauma, temporisation and bacterial contamination may also have been responsible. Although zinc phosphate is acidic on mixing (pH 2–3.5 depending on brand) this acidity reduces over the first 24 hours and stabilises at a near neutral pH of 6.5. Despite this acidity Brannstrom and Nyborg10,11 found no irritating effect on the pulp per se and, in practice, this potential irritant effect does not seem to be significant.
At one time cavity varnish was advocated to coat a preparation prior to cementation to protect it from cement but this adversely affected retention.12,13 Nowadays a dentine-bonding agent could be used and, anecdotally, this has helped with some teeth, which have been sensitive after preparation, but controlled studies are needed to assess the long-term consequences. If the dentine is to be etched it is essential that the primer seals all the open tubules or sensitivity may worsen and bacterial invasion may jeopardise the pulp.
Zinc oxide eugenol cements
Cements based on zinc oxide and eugenol are classical soft cements. Attempts have been made to create a more permanent cement by adding o-ethoxy-benzoic acid (EBA) to zinc oxide-eugenol and by reinforcing it with aluminium oxide and polymethylmethacrylate. Based on in vitro tests, this type of cement was reported to have good strength and be less soluble than zinc phosphate cement.14,15 Unfortunately, its performance was much poorer in vivo and studies have shown that it deteriorates much more rapidly in the mouth than other cements.16,17It cannot be recommended as a definitive lute for restorations.
Polycarboxylate cements
Advantages
-
Reasonable track record
-
Good compressive strength (if correctly proportioned)
-
Adequate working time
-
Bonds to enamel and dentine
-
Adequate resistance to water dissolution (but less good than zinc phosphate)
-
No adverse effect on pulp and less acidic than zinc phosphate on mixing
Disadvantages
-
Low tensile strength
-
Can deform under loading
-
Can be difficult to obtain low film thickness
-
Not resistant to acid dissolution
Recommendations
-
Traditionally used for vital or sensitive teeth, but no evidence to support efficacy (dentine bonding agents used to seal preparation prior to cementation may be a better option)
-
Occasionally useful to retain an unretentive provisional crown
Zinc polycarboxylate (or zinc polyacrylate) has a relatively long history as a luting cement. Unlike zinc phosphate, polycarboxylate cement does bond to tooth tissue, its bond strength to enamel being greater than that to dentine. It also bonds to stainless steel so dental instruments must be cleaned before the material sets to prevent a tenacious bond forming.
The tensile strength of polycarboxylate compares favourably to that of zinc phosphate although its compressive strength tends to be lower and it is difficult to achieve an equally low film thickness.
Zinc polycarboxylate cement is not as acidic on mixing (approx. 4.8) as zinc phosphate. There appears to be little irritation to the pulp18 possibly because there is little penetration of the large polyacrylic acid molecules into the dentine tubules. The liquid for the cement is either a viscous solution of polyacrylic acid or water. If water is used the acid is contained in its anhydrous state within the zinc oxide powder. More recently developed polycarboxylate cements contain fluoride salts, which may aid caries prevention.
Correctly mixed polycarboxylate cement has a consistency similar to that of honey and the cement may appear too viscous to allow proper seating. However, this is normal and should not be of concern since the cement undergoes 'sheer thinning' which reduces the apparent viscosity during the seating of the crown.19
Glass ionomer cements
Glass ionomer cements A randomised, double blind trial of GIC versus zinc phosphate showed no significant difference in sensitivity
Advantages
-
As for polycarboxylate cement but cement has similar acidity to zinc phosphate on mixing
-
Fluoride release
Disadvantages
-
Sensitive to early moisture contamination
-
Low tensile strength
-
Not resistant to acid dissolution
-
Has been accused of causing post-operative sensitivity but a controlled trial reports it is no worse than zinc phosphate
Recommendations
-
Used empirically for conventional crowns where patient has had a previously high caries rate
-
May be used as an alternative 'default cement' to zinc phosphate
Conventional glass ionomer cements were first introduced into dentistry as a filling material in 1972.20 Like polycarboxylates, glass ionomers may be supplied as a powder and aqueous acid (polyalkenoic) or powder and water. The aluminosilicate glass powder of GIC luting cements has smaller particles than GIC filling materials to reduce film thickness, which may be similar to or lower than that of zinc phosphate cements.
For luting purposes, mixing is generally carried out by hand and where provided the manufacturer's powder and liquid dispensers should be used. Encapsulated glass ionomer luting cements are also available and have the advantage of providing the correct powder-liquid ratio.
GIC compares favourably with zinc phosphate with regard to compressive and tensile strength (Table 2). GIC has a significant advantage to zinc phosphate in that it forms a considerable bond to tooth tissue by reaction with the calcium salts in the tooth structure and releases fluoride ions.
The higher solubility in water of GIC in comparison with zinc phosphate and zinc polycarboxylate cements has been identified as a problem when the cement is used for luting purposes. This solubility is adversely affected by early moisture contamination and the cement lute margins should be protected with a varnish following cementation, although this may be difficult when the crown margin is subgingival. Solubility is not a great problem clinically once the cement is set. Another disadvantage of GIC is that its pH during setting is even lower than that of zinc phosphate and some concern has been expressed regarding post-cementation hypersensitivity.21 However, a randomised, double blind trial of GIC versus zinc phosphate showed no significant difference in sensitivity,22 but it should be noted that cementation procedures were carefully controlled, including the use of encapsulated mixing. Dentine desiccation may on occasion be responsible for sensitivity; some authorities are convinced that dentinal fluid is drawn into the setting cement, which may cause problems if the preparation is over-dried with an air syringe.
Resin modified glass ionomer cements and compomers
Resin modified glass ionomer cements Reports of high strength porcelain crowns fracturing following cementation with RMGIs, possibly as a result of expansion of the cement
Advantages
-
Good compressive and tensile strengths (if correctly proportioned)
-
Reasonable working time
-
Resistant to water dissolution
-
Fluoride release
Disadvantages
-
Short track record
-
May expand and crack overlying porcelain because of water absorption
Recommendations
-
Worth trying for metal or metal ceramic crowns especially where preparation retention is borderline
-
Currently unclear which RMGI cements can be used safely with ceramic crowns
Resin modified glass ionomer (RMGI) cements are a hybrid of traditional glass ionomer cement with small additions of light curing resin23 and generally have the advantages of both in that they are purported to combine the strength and insolubility of resin with the fluoride release of GIC. They were introduced with the aim of overcoming the moisture sensitivity and the low strength of conventional glass ionomers. Examples include Vitremer and Fuji Plus. Compomers are also composed of resin and glass ionomer but are more closely related to composites with the glass ionomer setting reaction occuring slowly as moisture is absorbed into the set resin matrix. Examples include Dyract Cem and Dyract Cem Plus.
The use of RMGIs for luting purposes is becoming more popular because of their relatively high bond strength to dentine, and their ability to form a very thin film layer. RMGIs leach fluoride, but it is unclear how useful this is in preventing secondary caries formation. Several RMGIs are available but whilst they may seem promising clinical studies are still in their infancy. There have also been anecdotal reports of high strength porcelain crowns fracturing following cementation with RMGIs, possibly as a result of expansion of the cement from water sorption.24 These have been supported by an in-vitro study showing that ceramic crowns crack between 3 and 12 months after cementation with both RMGIs and compomers.25 RMGIs contain the resin HEMA and absorb significantly more water than composites. In view of these concerns it is best to restrict the use of RMGIs and compomers to metal restorations. Furthermore, when cementing porcelain or composite restorations a better aesthetic result can be achieved with composite resin cements.
Resin cements
Resin cements The tensile strength of resin cements is about ten times that of zinc phosphate
Resin cements The Richwil crown remover is not unlike a sticky sweet
Advantages
-
Good compressive and tensile strengths
-
High tensile strength (relative to conventional cements)
-
Resistant to water dissolution
-
Relatively resistant to acid dissolution
-
Can enhance strength of ceramic restoration if bond obtained
Disadvantages
-
Film thickness varies substantially between materials
-
Excess material extruded at margin may be difficult to remove especially proximally
Recommendations
-
Must be used with or incorporate an effective dentine bonding agent
-
Material of choice for porcelain veneers, ceramic onlays and resin bonded ceramic crowns
-
May be used to improve retention where preparation geometry sub-optimal, but clinical studies needed to determine long-term success
Resin cements are composites composed of a resin matrix, eg bis-GMA or urethane dimethacrylate, and a filler of fine inorganic particles. They have been available as direct filling materials since the early 1950s26 but it was not until the early 1970s that a composite resin was introduced for crown and bridge cementation.27 Resin luting cements differ from restorative composites primarily in their lower filler content and lower viscosity. Following on from their successful use in the cementation of resin bonded bridges and veneers, their popularity has been increasing in recent years for crown cementation because of their use in conjunction with dentine bonding agents (DBA). However even when DBAs are used, resin cements are not without problems (see later).
Composite resin cements are available as self cured, light cured and dual cured materials. The self cured materials are typically used as luting cements because of the inability, or at best difficulty, of light to pass through porcelain and metal restorations. Examples include Panavia,21 All Bond 2 luting cement and Superbond.
Mechanical and physical properties of resin cements compare favourably with the other cements discussed above (Table 2). In particular, tensile strength is about ten times that of zinc phosphate, which in combination with the high bond strength explains why preparation geometry is of less importance to retention than with conventional cements. This makes resin cements useful for bonding restorations on tooth preparations that would not be retentive enough to succeed with conventional cements. Moreover, a well-bonded composite lute will confer much greater strength to an overlying porcelain restoration than a weaker conventional cement. This feature has been demonstrated in vitro with porcelain veneers28 and in vivo with porcelain inlays29 which were almost five times more likely to fracture when cemented with conventional glass ionomer. It should be noted that effective resin bonding to some high strength porcelain cores (eg In-Ceram) could not be achieved by the usual etching with hydrofluoric acid because of the lack of pores in the material.30
Problems with the use of resin cements for luting full crowns include excessive film thickness with some materials,31,32 marginal leakage because of setting shrinkage, and severe pulpal reactions when applied to cut vital dentine. However, this latter problem may be related more to bacterial infiltration than to any chemical toxicity. The use of DBA under resin cement is critical to its success unless the preparation has been cut only into enamel. Pulpal response is reduced by the use of DBAs, presumably by sealing dentine tubules and reducing microleakage.33Adhesive resin cement was found to produce a better marginal seal than zinc phosphate cement.34 However, even if the problems of microleakage and film thickness could be solved, the problem of adequately removing hardened excess resin from inaccessible margins may preclude the use of resin cement for crowns with subgingival margins. Indeed, proximal extrusions of resin cement are often radiolucent and may remain undetected.35
Crown cementation
When a crown has been successfully tried-in and the cement chosen, cementation may then take place. This section will consider conventional cementation. Cementation with resin cements is covered more fully in Parts 12 and 13 of this series on porcelain veneers and resin bonded metal restorations respectively.
Trial cementation
Most dentists are in the habit of fitting crowns and then cementing them with hard cement. Whilst this approach is usually satisfactory there are times where it is difficult to predict a patient's response to changes in aesthetics or occlusion. If such a patient returns unhappy the offending crowns must be cut off – a distressing experience for all concerned. In cases of doubt it is useful to have a period of trial cementation using soft cement, but you must ensure that the definitive restoration can be removed without damage to it or the underlying preparation. To make removal easier the cement should be applied in a ring around the inner aspect of the crown margin. It is important that the manufacturer's modifier is added to the cement. Equal lengths of base and catalyst with a third of a length of modifier will soften cements such as Temp Bond. Alternatively, a 'non-setting' zinc oxide eugenol material (eg Optow Trial Cement) can be used for short periods of soft cementation where preparations are retentive. This material has the advantage that it is easily pealed out of the crown like a membrane, but it cannot be relied upon for more than a few days retention.
Restorations can be removed either by finger pressure or by the application of a matrix band. In cases of difficult removal a Richwil crown remover can be helpful. This crown remover is simply a material, not unlike a sticky sweet, which is softened in hot water, positioned over the crown and the patient asked to bite. Once the material has hardened the crown is removed by asking the patient to snap open. Another way of applying a dislodging force to a soft-cemented crown is to use an impact mallet. The problem with this technique is finding a point of application on the crown. One solution to this problem is to incorporate small lugs resembling mushrooms on the lingual aspect of the crown's metal work.36 The lugs are removed, of course, prior to hard cementation.
Controlling cement film thickness
The interposition of a cement lute inevitably affects crown seating. Consequently, the art of cementation is to choose a cement with an inherently low film thickness and use techniques which allow it to escape whilst the crown is being seated.
Cement flow can be hindered by preparation features, which cause a build up of hydrostatic pressure.37Thus, retentive preparations, which are long, near parallel and have a large surface area, are most at risk of not seating fully. This problem can be overcome by die spacing and controlled cement application or by venting the crown. These techniques need to be used for all crowns not just apparently retentive ones.
Die spacing is the most common method of achieving space for the cement lute.38 It involves painting several layers of die relief agent over the whole of the die but avoiding the finish line. The increased cement space results in more rapid seating with decreased deformation of the restoration.39,40,41 Die spacing results in a slightly loose fit of a crown on its preparation, but its effect on retention is unclear with some studies reporting an increase in retention37 while others report a decrease or no effect. A recent study concluded that decreasing the width of the cement layer increases the resistance to dynamic lateral loading.7 This variability may occur because of differences in cement film thickness. A very thin cement lute may have higher stress concentrations than a slightly thicker one.42 However, too thick a cement lute is also undesirable as it is liable to fracture.
Another factor which influences the vertical seating of crowns and hence marginal adaptation is the amount of cement loaded into the crown prior to cementation. A study on the effect of volume of zinc phosphate cement, reported that lesser amounts of cement placed within a crown resulted in smaller marginal discrepancy and better occlusal accuracy.43Indeed, a crown treated in such a way seated almost 70% better than an identical crown completely filled with cement. However, care must be taken in applying cement in this way not to exceed the working time or the cement may be too viscous at the time of seating.
Venting is an effective8 but less popular method of reducing cement film thickness. External venting involves creating a perforation in the occlusal surface of the crown, which is sealed with a separate restoration after cementation. With internal venting an escape channel is created either in the axial wall of the preparation or the fit surface of the crown to help cement escape.
The amount of force required to allow maximum seating of cast crowns has been shown to be cement specific.44 Seating forces are discussed next in relation to cementation technique.
Technique
Technique Force must be adequate to ensure complete seating, but sudden excessive force may result in elastic rebound and the crown being partly dislodged
Isolate the preparation and ensure good moisture control. If the gingivae have overgrown the finish line use either retraction cord with haemostatic agent or if more severe use electro-surgery. A breakdown in technique at any of the following stages will predispose to failure:
-
Clean the preparation and crown with water spray
-
Air dry but do not desiccate preparation
-
Mix cement according to manufacturer's instructions
-
Coat the fit surface with cement – do not overfill
-
Only apply cement to preparation if cementing a post
The crown should be seated quickly with firm finger pressure until all excess cement has been expressed from the margins. Seating force must be adequate to ensure complete seating of the crown onto the preparation, but sudden excessive force may result in elastic strain of the dentine, creating a rebound effect, which results in the crown being partly dislodged when the force is removed.34 Karpidis and Pearson (1988)45 revealed that crowns seated on preparations in bovine dentine with a force of 300 N/cm2 could be removed more easily than those cemented with half the force.
Depending on the angulation of the tooth, pressure may then continue to be exerted onto the crown by the dentist or by the patient biting onto a cotton roll. Some operators prefer a wooden orange stick or similar implement for cementing posterior restorations as this can reduce film thickness. However care must be taken as these are rigid and may only contact part of the occlusal surface of the crown resulting in tipping. Pressure should be maintained for about one minute. Maintaining pressure beyond this time has no appreciable additional effect.46 It is worth checking the accuracy of the fit at this stage using a sharp probe on the margin and if necessary fine gold margins can be burnished before the cement sets.
Adequate moisture control should be maintained until the cement has set to prevent moisture contamination of the unset material at the crown margin. In the case of conventional cements, excess cement should be left until after the cement sets. For resin-based cements, removal of excess before setting is recommended as it can be very difficult to remove following setting but may still remain despite our best efforts.47 Some operators apply a smear of petroleum jelly to the outside of the crown which also helps with removal of set cement, but if you do this take great care to prevent contamination of the fit surface. A common failing is for excess cement to be left, especially interproximally. Your nurse can help by having a piece of floss ready. This can be made more effective by tying a knot in the middle of the floss and passing it through the interdental space. Following clean up, a final evaluation of the cemented crown can be made including rechecking the occlusion.

References
Kaufman EG The retention of crowns before and after cementation. NY Univ J Dent 1967; 25: 6–7.
McClean JW, von Fraunhoffer JA The estimation of cement film thickness by an in vivo technique. Br Dent J 1971; 131: 107–111.
Christensen GJ Marginal fit of gold inlay castings. J Prosthet Dent 1966; 16: 297–305.
Lang NP, Kiel RA, Anderhalden K Clinical and microbiological effects of subgingival restorations with overhanging or clinically perfect margins. J Clin Perio 1983; 10: 563–578.
Kelleher MGD, Setchell DJ An investigation of marking materials used in occlusal adjustment. Br Dent J 1984; 156: 96–102.
Monasky GE, Taylor DF Studies on the wear of porcelain, enamel and gold. J Prosthet Dent 1971; 25: 299–306.
Wiskott HW, Belser UC, Scherrer SS The effect of film thickness and surface texture on the resistance of cemented extracoronal restorations to lateral fatigue. Int J Prosthodont 1999; 12: 255–262.
Kaufman EG, Colin LC, Schlagel E, Coelho DH Factors influencing the retention of cemented gold castings: the cementing medium. J Prosthet Dent 1966; 16: 731–739.
Langeland K, Langeland LK Pulp reactions to crown preparation, impression, temporary crown fixation and permanent cementation. J Prosthet Dent 1965; 15: 129–143.
Brännström M, Nyborg H Bacterial growth and pulpal changes under inlays cemented with zinc phosphate cement and Epoxylite CBA 9080. J Prosthet Dent 1974; 31: 556–565.
Brännström M, Nyborg H Pulpal reaction to polycarboxylate and zinc phosphate cement used with inlays in deep cavity preparations. J Am Dent Assoc 1977; 94: 308–310.
Smith DC, Ruse ND Acidity of glass ionomer cements during setting and its relation to pulp sensitivity. J Am Dent Assoc 1986; 112: 654–657.
Chan KC, Svare CW, Horton DJ The effect of varnish on dentinal bonding strength of five dental cements. J Prosthet Dent 1976; 35: 403–406.
Brauer GM, McLaughlin R, Huget EF Aluminium oxide as a reinforcing agent for zinc oxide-eugenol-o-ethoxy-benzoic acid cements. J Rest Dent 1968; 47: 622–628.
Phillips RW, Swartz ML, Norman RD, Schnell RJ, Niblack BF Zinc oxide and eugenol cements for permanent cementation. J Prosthet Dent 1968; 19: 144–150.
Osbourne JW, Swartz ML, Goodacre CJ, Phillips RW, Gale EN A method for assessing the clinical solubility and disintegration of luting cements. J Prosthet Dent 1978; 40: 413–417.
Mesu FP, Reedijk T Degradation of luting cements measured in vitro and in vivo. J Rest Dent 1983; 62: 1236–1240.
Going RE, Mitchem JC Cements for permanent luting: a summarising review. J Am Dent Assoc 1975; 91: 129–137.
Lorton L, Moore ML, Swartz ML, Phillips RW Rheology of luting cements. J Rest Dent 1980; 59: 1486–1492.
Wilson AD, Kent BE A new translucent cement for dentistry. Br Dent J 1972; 132: 133–135.
Smith DC, Ruse NC Acidity of glass ionomer cements during setting and its relation to pulp sensitivity. J Am Dent Assoc 1986; 112: 654–657.
Kern M, Kleimeier B, Schaller HG, Strub JR Clinical comparison of postoperative sensitivity for a glass ionomer and a zinc phosphate luting cement. J Prosthet Dent 1996; 75: 159–62.
Sidhu SK, Watson TF Resin-modified glass ionomer materials. A status report for the American Journal of Dentistry. Am J Dent 1995; 8: 59–67.
Kanchanavista W, Arnstice HM, Pearson GJ Water sorption characteristics of resin-modified glass-ionomer cements. Biomater 1997; 18: 343–349.
Leevailoj C, Platt JA, Cochran MA, Moore BK In vitro study of fracture incidence and compressive fracture load of all-ceramic crowns cemented with resin-modified glass ionomer and other luting agents. J Prosthet Dent 1998; 80: 699–707.
Schouboe PJ, Paffenbarger GC, Sweeney WJ Resin cements and posterior type direct filling resins. J Am Dent Assoc 1956; 52: 584.
Lee H, Swartz ML Evaluation of a composite resin crown and bridge luting agent. J Rest Dent 1976; 51: 756.
Brandson SJ, King PA The compact fracture resistance of restored endodontically treated anterior teeth. J Rest Dent 1992; 72: 1141.
Åberg CH, van Dijken JWV, Olofsson A-L Three-year comparison of fired ceramic inlays cemented with composite resin or glass-ionomer cement. Acta Odontol Scand 1994; 52: 140–149.
Awliya W, Oden A, Yaman P, Dennison JB, Razzoog ME Shear bond strength of a resin cement to densely sintered high-purity alumina with various surface conditions. Acta Odontol Scand 1998; 56: 9–13.
White SN, Yu Z, Kipnis V Effect of seating force on film thickness of new adhesive luting agents. J Prosthet Dent 1992; 68: 476–481.
White SN, Kipnis V Effect of adhesive luting agents on the marginal seating of cast restorations. J Prosthet Dent 1993; 69: 28–31.
Qvist V, Stolze K, Qvist J Human pulp reactions to resin restorations performed with different acid-etch restorative procedures. Acta Odontologica Scandinavia 1989; 47: 253–263.
Tjan AHL, Dunn JR, Brant BE Marginal leakage of cast gold crowns luted with an adhesive resin cement. J Prosthet Dent 1992; 67: 11–15.
O'Rourke B, Walls AW, Wassell RW Radiographic detection of overhangs formed by resin composite luting agents. J Dent 1995; 23: 353–357.
Pameijer JHN Periodontal and occlusal factors in crown and bridge procedures. pp394 Amsterdam: Centre for Post graduate Courses 1985.
Carter SM, Wilson PR The effect of die-spacing on crown retention. Int J Prosthodont 1996; 9: 21–29.
Grajower R, Zuberi Y, Lewinstein I Improving the fit of crowns with die spacers. J Prosthet Dent 1989; 61: 555–563.
Wilson PR, Goodkind RJ, Sakaguchi R Deformation of crowns during cementation. J Prosthet Dent 1990; 64: 601–609.
Wilson PR The effect of die spacing on crown deformation and seating time. Int J Prosthodont 1993; 6: 397–401.
Wilson PR Effect of increasing cement space on cementation of artificial crowns. J Prosthet Dent 1994; 71: 560–564.
Kamposiora P, Papavasilious G, Bayne SC, Felton DA Finite element analysis estimates of cement microfracture under complete veneer crowns. J Prosthet Dent 1994; 71: 435–441.
Tan K, Ibbetson R The effect of cement volume on crown seating. Int J Prosthodont 1996; 9: 445–451.
Wilson PR Low force cementation. J Dent 1996; 24: 269–273.
Karipidis A, Pearson GJ The effect of seating pressure and powder/liquid ratio of zinc phosphate cement on the retention of crowns. J Oral Rehabil 1988; 15: 333–337.
Jorgensen KD Structure of the film thickness of zinc phosphate cements. Factors affecting the film thickness of zinc phosphate. Acta Odontol Scand 1960; 18: 479–501.
Mitchell CA, Pintado MR, Geary L, Douglas WH Retention of adhesive cement on the tooth surface after crown cementation. J Prosthet Dent 1999; 81: 668–677.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed paper
Rights and permissions
About this article
Cite this article
Wassell, R., Barker, D. & Steele, J. Crowns and other extra-coronal restorations: Try-in and cementation of crowns. Br Dent J 193, 17–28 (2002). https://doi.org/10.1038/sj.bdj.4801473
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.4801473
This article is cited by
-
Clinical applications of polytetrafluoroethylene (PTFE) tape in restorative dentistry
British Dental Journal (2017)