Key Points
-
Dental practitioners are becoming aware that the problem of dental erosion, particularly in children, is an increasing one. Is this just a subjective impression or is there scientific evidence for this?
-
The causes are multi-factorial, but there is increasing evidence that acidic dietary components such as soft drinks, are directly related to dental erosion.
-
The prevalence of anorexia and bulimia nervosa is also increasing and, along with gastro-oesophageal reflux from other sources, is an aetiological factor that must be considered. Control of dental erosion is dependent on accurate diagnosis of its causes.
-
The aetiological factors need to be addressed first before proceeding with complex restorative techniques.
Abstract
There has been a clinical impression among dental practitioners, particularly those working with children, that the problem of dental erosion is increasing. Is this really the case or are we more aware of the problem? What is causing this increase, if it really exists? Perhaps more importantly, what can we do about it? This article looks at the prevalence, and aetiology of dental erosion, particularly in children, and makes some practical suggestions for possible control.
Similar content being viewed by others
Main
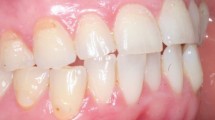
Tooth wear has long been a recognised phenomenon in adults and ascribed to the triumvirate of attrition, abrasion and erosion. Pathological tooth wear has been seen in antiquity but the problems are becoming even more evident in society now, with an ageing population who are retaining their natural teeth for significantly longer. There has been a gradual realisation in recent years that our younger population may also be increasingly affected. This is with increasing dental erosion, rather than attrition and abrasion, although these factors also contribute.
Erosion has been defined as the irreversible loss of dental hard tissue by a chemical process not involving bacteria;1 this differentiates it from caries. The question must be asked as to whether it really is on the increase and if so, then why?
Is it increasing?
If we are going to answer this question then we must have a baseline figure from which to measure and we must have an accurate scale of measurement. This has been a major stumbling block. There have been many scales and indices suggested; their very diversity suggests that not one of them is ideal or else we should all be using the same one. There have been some accurate and reproducible scales devised which have worked well in anaesthetised animals, taken 45 minutes per charting and required a scanning electron microscope. However, their use is plainly limited in an active 4-year-old hopping around the dental surgery! In adults the Tooth Wear Index of Smith and Knight2 has achieved the greatest clinical acceptance but this does not differentiate between attrition, abrasion and erosion.
It is this index, though, with some modifications that has been generally used in children. Until a simple, reproducible diagnostic index has been established which is accepted worldwide it will be difficult to say what the true prevalence of erosion is in children or whether it is increasing significantly.
The studies that have been published in children have largely been undertaken in the UK. From the 1950s onward a series of case reports have been published linking loss of tooth tissue to varying aetiological factors.3,4,5,6 The prevalence surveys often suffer from deficiencies of sample selection as well as poor reproducibility of the diagnostic index used. The largest study undertaken was that of the UK Child Dental Health Survey of 1993,7 which showed that 52% of 5-year-olds had significant erosion. Other surveys are given in Table 1. They all show high figures for tooth wear, particularly in the primary dentition which is more susceptible because of higher acid solubility and reduced thickness of the enamel.
What causes it?
Without doubt the aetiology of dental erosion is multi-factorial. A diagram rather like that produced for caries can be constructed — see figure 1. Plainly, time and a susceptible tooth are required but there are many factors influencing the host which significantly affect susceptibility. The mineralisation of the dental hard tissues and the presence of fluorapatite rather than hydroxyapatite affects the acid solubility. The actual anatomy of the mouth and salivary flow rates and buffering capacity at different sites also influence erosion. Where there is abundant saliva such as in the lower incisor region, there tends to be little erosion.
Some of the evidence directly relating erosion to low salivary buffering capacity is conflicting,11,12 and this is certainly an area where further research is required. All acids, whether from intrinsic or extrinsic sources, are capable of demineralising tooth tissue and therefore of causing erosion.
Intrinsic sources of acid
Essentially these are from the gastric contents and enter the mouth from gastric reflux or vomiting. Very occasional case reports of rumination in children have been published.13 Gastro-oesophageal reflux is much more common in the developed world than was thought and it has been stated from recent research that it affects 7% of the adult population on a daily basis and more than 30% every few days.14 Most of this is asymptomatic but there is a wide spectrum of disease and severity of reflux into the mouth. Sometimes erosion of the dental tissues may be the first sign that reflux is occurring. Symptoms associated with reflux are heartburn, retrosternal discomfort and dysphagia. Children with neurological impairments such as cerebral palsy have significantly higher levels of gastro-oesophageal reflux than 'normal' children. There are many potential causes of reflux, some of them uncommon in childhood; the main ones are shown in Table 2. There are other causes such as excessive alcohol consumption which are more common in adults.
Vomiting, either spontaneous or self-induced, may be associated with a variety of medical problems, but if this continues over a lengthy period in a susceptible individual then again extensive dental erosion may occur. Current research suggests that the prevalence of bulimia and anorexia nervosa is increasing. Table 3 lists the principal causes of vomiting.
Extrinsic sources of acid
There has been recent media publicity as well as scientific research to suggest that dietary practices and habits are changing. No longer do we have the 'three meals a day' routine but rather the habits of 'grazing' and 'snacking'. This is particularly the case with soft drink consumption: there has been an enormous increase in the total amount drunk and a considerable change in the age distribution of drinkers. At one time most soft drinks were confined to children but there is now good evidence to show that this is being carried forward to adult life, rather than 'graduating' onto tea and coffee drinking. Erosion may be particularly harmful to infants if drinks are taken from a feeder bottle used as a comforter.15 There have been significant associations shown between soft drink consumption and dental erosion, particularly the bed-time consumption of fruit-based drinks.16
There are other sources of dietary acid besides soft drinks: teenagers and adults should be aware that many alcoholic beverages such as wine and particularly sparkling wine, are erosive. However, it is not just the pH that is important but rather the titratable acidity. Table 4 gives the pH and titratable acidity of some commonly consumed drinks both in children and adults, with an indication of their erosive potential. (The titratable acidity is the amount of alkali needed to be added to an acid to bring it up to a neutral pH. It therefore represents the amount of available acid and is an indication of strength and thus of erosive potential.)
There are also acidic foods that may be implicated in the development of erosion eg fruit, pickles. yoghourt and sauces.
Lifestyle
An increased emphasis on a 'healthy' diet in recent years has been just part of the overall emphasis on a healthy life-style. Encouragement to take regular exercise may also lead to increased consumption of acidic drinks and some of the sports drinks which are now heavily advertised are also acidic. Competitive swimmers and cyclists have been re-ported as having higher levels of dental erosion.
Conversely there are unhealthy lifestyles that may be implicated in dental erosion. The use of the drug 'ecstasy' (3,4 methylenedioxy-methamphetamine) reduces salivary flow. The dry mouth combined with dehydration from vigorous exercise and excessive consumption of low pH drinks has also been linked to dental erosion.17
Oral hygiene products and medication
Some mouthwashes and saliva substitutes have been shown to be acidic18 and if used to excess have caused problems. Now that this problem has been recognised they have largely been reformulated. Dental erosion is frequently associated with people who have very high standards of oral hygiene. If enamel or dentine has been demineralised by some acidic attack from whatever source and then is brushed there will be much more dental tissue removed. Loss of tooth structure is accelerated until the demineralised layers are removed. The effect is probably very important in the development of erosion and may explain the significant increase of erosion in those children consuming a fruit-based drink last thing at night — presumably before brushing their teeth.
There are a number of common medications, particularly vitamin C tablets and iron preparations, which are very acidic, particularly if consumed in chewable form.
How can we control it?
First of all we must make a diagnosis. Obviously dental erosion is not a problem for everyone but if signs are detected at an early stage and appropriate steps taken then it may be possible to halt the progression to pain and destruction. Restorative treatment of extensive tooth wear is very expensive and time-consuming.
Once suspicion has been raised then it is essential to record accurately the severity and extent. This will establish the clinical baseline so that any progression can be observed and the effects of preventive measures assured.
Record the clinical situation
For children in the permanent dentition and adults take impressions and make good quality stone study casts. Clinical photographs are also helpful. The most useful diagnostic index is the Tooth Wear Index2 but this is probably not sufficiently sensitive to detect small changes. A silicone index can be prepared.
Try to find the aetiological factors
This is reliant on taking an in-depth history to include a detailed dietary history, medical history, dental hygiene habits and sensitive investigation about lifestyle factors.
A 3-day diet history to include everything that passes the patient's lips is important. The periodicity of eating and toothbrushing is also important. Such habits as continuous sipping or 'frothing' of drinks should be noted. (Frothing is the habit of holding carbonated drinks in the mouth and sucking them in and out of the teeth to make a froth. This tends to add the 'ultrasonic' effect of the bursting bubbles to the erosive effects of the acid.)
Dietary counselling
This can only be given after a thorough analysis of the diet and influencing factors. It must be tailored to the individual bearing in mind the constraints that are operating on them. It needs to be given in a positive, individualised way to maximise compliance.
It will include:
-
Limit acid foods and drinks to mealtimes
-
Reduce frequency
-
Avoid acidic substances last thing at night
-
Finish meals with something alkaline such as a small piece of cheese or milk
-
Avoid toothbrushing after acidic substances
-
Check any medication, mouthwashes, and so on
-
Chewing gum has been shown to stimulate salivary flow and increase buffering capacity, but may also cause increased gastric secretion. It should not be recommended for children, probably below the age of 7 years, and is not suggested for those with a history of gastric reflux.
Are there any possible intrinsic acid sources?
If there is any evidence or suspicion then referral to the general medical practitioner and onward to a gastro-enterologist or psychiatrist may be required. Medication may be useful but this obviously needs medical supervision.
If reflux or vomiting are occurring then rinsing the mouth with water and sodium bicarbonate helps to neutralise the oral environment. People who have vomited often rush off to clean their teeth. This is quite the wrong thing to do and should be advised against. If reflux is occurring during sleep then an occlusal guard containing sodium bicarbonate can be used in adults or teenagers.
Prevention and treatment of sensitivity
The following will not only to keep the patient comfortable but also to aid remineralisation:
-
Fluoride mouthrinses and varnish
-
High fluoride level toothpaste
-
Low abrasive toothpaste
-
Use of dentine bonding agents
-
Sugar free chewing gum (but with some reservations).
Monitor
When the patient returns for review, their compliance with all the advice given should be checked. Perhaps more importantly, the clinical situation must be examined very carefully. A localised silicone index should be taken of the original study casts in the area of most concern. This can be cut through with a sharp scalpel over the area (often the palatal aspect of the upper incisors). It is then transferred to be fit on to the patient. If there is any gap between the silicone index and the surface of the tooth then there has been further tooth surface loss. However, this would indicate fairly extensive surface loss. General comparison with the study casts and the clinical photographs is also necessary. These records have a number of errors inherent in their methods but can be useful in showing and educating patients about their erosion problems. There are more accurate methods such as replica techniques examined under the scanning electron microscope but these have very limited use in general dental practice.
Restorative treatment?
If there has been early diagnosis and control of the situation then restorative treatment, hopefully, will be unnecessary. However, we all have patients who are not as compliant as we might like. If the situation is not under control then covering eroded teeth may merely disguise the problem. Certainly, the aetiological factors need to be addressed first before proceeding with complex restorative techniques.
Adhesive restorations in composite or compomers may be useful as an interim treatment with adhesive metal castings and porcelain veneers later if necessary.
Preventive programmes must remain the cornerstone in the management of dental erosion.
References
Pindborg J J . Pathology of the dental hard tissues. Copenhagen: Munksgaard. 1970; 312–321.
Smith B G N, Knight J K . An index for measuring the wear of teeth. Br Dent J 1984; 156: 435–438.
Holloway P J, Mellany M, Steward R J C . Fruit drinks and tooth erosion. Br Dent J 1958; 104: 305–309.
Eccles J D, Jenkins W G . Dental erosion and diet. J Dent 1974; 2: 153–159.
Giunta J L . Dental erosion resulting from chewable vitamin C tablets. J Am Dent Assoc 1983; 107: 253–256.
Linkosalo E, Markkanen H . Dental erosion in relation to lactovegetarian diet. Scand J Dent Res 1985; 93: 436–441.
O'Brien M . Children's Dental Health in the United Kingdom 1993. Office of Population Censuses and Surveys. London: HMSO, 1994.
Milosevic A, Young P J, Lennon M A . The prevalence of tooth-wear in 14-year-old school children in Liverpool. Community Dent Health 1994; 11: 83–86.
Millward A, Shaw L, Smith A . Dental erosion in four year old children from differing socioeconomic backgrounds. J Dent Child 1994; 61: 263–266.
Hinds K, Gregory J R . National diet and nutrition survey: children 1Þ to 4Þ years. Volume 2: Report of the Dental Survey Office of Population Censuses and Surveys. London: HMSO, 1994.
Bartlett D W, Coward P Y, Nikkah C, Wilson P F . The prevalence of tooth wear in a cluster sample of adolescent schoolchildren and its relationships with potential explanatory factors. Br Dent J 1998; 184: 125–129.
Gudmundson K, Kristleifsson G, Theodors A, Holbrook W P . Tooth erosion, gastrooesophageal reflux and salivary buffer capacity. Oral Surg, Oral Med, Oral Path 1995; 79: 185–189.
Reis S . Rumination in two developmental normal children. J Fam Pract 1994; 38: 521–523.
Colin-Jones D G . Gastro-oesophageal reflux disease. Prescribers J 1996; 36: 66–72.
Smith A J, Shaw L . Baby fruit juice and tooth erosion. Br Dent J 1987; 162: 65–67.
Millward A, Shaw L, Smith A J, Rippin J W, Harrington E . The distribution and severity of tooth wear and the relationship between erosion and dietary constituents in a group of children. Int J Paediatric Dentistry 1994; 4: 151–157.
Duxbury A J . Ecstasy — dental implications. Br Dent J 1993; 175: 38.
Bhatti S A, Walsh T F, Douglas C W I . Ethanol and pH levels of proprietary mouthrinses. Community Dent Health 1994; 11: 71–74.
Author information
Authors and Affiliations
Additional information
Refereed Paper
Rights and permissions
About this article
Cite this article
Shaw, L., Smith, A. Dental erosion — the problem and some practical solutions. Br Dent J 186, 115–118 (1999). https://doi.org/10.1038/sj.bdj.4800037
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.4800037