Abstract
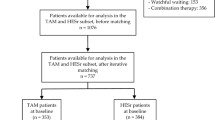
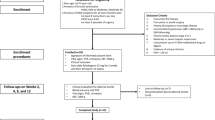
In this multicentre, double-blind study, patients with LUTS/BPH were randomised to 26 weeks with finasteride 5 mg once daily (n=204) or tamsulosin 0.4 mg once daily (n=199). Double-blind treatment was continued for another 26 weeks (total treatment duration: 1 y). The primary efficacy parameter was the difference in mean change in total Symptom Problem Index (SPI) from baseline to end point at week-26 in the intention-to-treat (ITT) and per protocol (PP) populations. Tamsulosin induced a greater improvement in total SPI (−5.2 points or −37%) compared to finasteride (−4.5 points or −31%) at week-26 (P=0.055 in ITT and P=0.032 in PP). Tamsulosin improved urinary symptoms (particularly the more bothersome storage symptoms) and flow more quickly than finasteride. The difference was statistically significant for the SPI from week-1 (reduction, respectively, −2.5 vs −1.8 points, P=0.043) to week-18 and for Qmax from week-1 (increase, respectively, 2.3 vs 0.7 ml/s, P=0.0007) to week-12. Both treatments were well tolerated with a comparable incidence of adverse events, including urinary retention.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Chapple CR . Selective α1-adrenoceptor antagonists in benign prostatic hyperplasia: rationale and clinical experience. Eur Urol 1996; 29: 129–144.
Peters TJ et al. The international continence society ‘benign prostatic hyperplasia’ study: the bothersomeness of urinary symptoms. The International Continence Society ‘Benign Prostatic Hyperplasia’ Study Group. J Urol 1997; 157: 885–889.
Sells H, Donovan J, Ewings P, MacDonagh RP . The development and validation of a quality-of-life measure to assess partner morbidity in benign prostatic enlargement. Br J Urol 2000; 85: 440–445.
Speakman MJ . Who should be treated and how? Evidence-based medicine in symptomatic BPH. Eur Urol 1999; 36 (Suppl 3): 40–51.
Boyle P, Gould AL, Roehrborn CG . Prostate volume predicts outcome of treatment of benign prostatic hyperplasia with finasteride: meta-analysis of randomized clinical trials. Urology 1996; 48: 398–405.
Djavan B, Marberger M . A meta-analysis on the efficacy and tolerability of α1-adrenoceptor antagonists in patients with lower urinary tract symptoms suggestive of benign prostatic obstruction. Eur Urol 1999; 36: 1–13.
Schulman CC et al. Long-term use of tamsulosin to treat lower urinary tract symptoms/benign prostatic hyperplasia. J Urol 2001; 166: 1358–1363.
Narayan P, Ranhosky A, Doyle CA . Long-term efficacy of tamsulosin: results of a 6-year experience. J Urol 2001; 165 (Suppl 5): 381 (abstract 1561).
Chapple CR . Introduction and concluding remarks. Eur Urol 1999; 36 (Suppl 3): 1–6.
Debruyne FMJ et al. Sustained-release alfuzosin, finasteride and the combination of both in the treatment of benign prostatic hyperplasia. European ALFIN Study Group. Eur Urol 1998; 34: 169–175.
Lepor H et al. The impact of medical therapy on bother due to symptoms, quality of life and global outcome, and factors predicting response. Veterans Affairs Cooperative Studies Benign Prostatic Hyperplasia Study Group. J Urol 1998; 160: 1358–1367.
Kirby R et al. Efficacy and tolerability of doxazosin and finasteride, alone or in combination, in treatment of symptomatic benign prostatic hyperplasia: the Prospective European Doxazosin and Combination Therapy (PREDICT) trial. Urology 2003; 61: 119–126.
Barry MJ et al. Measuring disease-specific health status in men with benign prostatic hyperplasia. Med Care 1995; 33 (Suppl 4): AS145–AS155.
Malloy BJ et al. α1-adrenergic receptor subtypes in human detrusor. J Urol 1998; 160: 937–943.
Hampel C et al. Changes in adrenergic control of obstructed bladder. J Urol 2001; 165 (Suppl 5): 41–42 (abstract 170).
Price D . Potential mechanisms of action of superselective α1-adrenoceptor antagonists. Eur Urol 2001; 40 (Suppl 4): 5–11.
McConnell JD et al. The effect of finasteride on the risk of acute urinary retention and the need for surgical treatment among men with benign prostatic hyperplasia. N Engl J Med 1998; 338: 557–563.
Peters DH, Sorkin EM . Finasteride: a review of its potential in the treatment of benign prostatic hyperplasia. Drugs 1993; 46: 177–208.
Denis L . Tamsulosin: effect on PSA levels in 3 month placebo-controlled studies and long-term follow-up of these studies. Eur Urol 1998; 33 (Suppl 1): 130 (abstract 517).
Höner K et al. Tamsulosin 0.4 mg once daily: effect on sexual function in patients with lower urinary tract symptoms suggestive of benign prostatic obstruction. Eur Urol 1999; 36: 335–341.
McConnell JD, for the MTOPS Steering Committee. The long term effects of medical therapy on the progression of BPH: results from the MTOPS trial. Presented during the 97th Annual Meeting of the American Urological Association, May 25–30, 2002. Orlando. J Urol 2002; 167 (Suppl 4): 265 (abstract 1042).
Foley CL, Kirby RS . 5 Alpha-reductase inhibitors: what's new? Curr Opin Urol 2003; 13: 31–37.
Acknowledgements
Boehringer Ingelheim Italy SpA sponsored the MICTUS study. We are grateful to the Ismar Healthcare NV for their support in editing of the manuscript.
Author information
Authors and Affiliations
Consortia
Corresponding author
Appendix 1
Rights and permissions
About this article
Cite this article
Rigatti, P., Brausi, M., Scarpa, R. et al. A comparison of the efficacy and tolerability of tamsulosin and finasteride in patients with lower urinary tract symptoms suggestive of benign prostatic hyperplasia. Prostate Cancer Prostatic Dis 6, 315–323 (2003). https://doi.org/10.1038/sj.pcan.4500680
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.pcan.4500680
Keywords
This article is cited by
-
Tadalafil versus tamsulosin as combination therapy with 5-alpha reductase inhibitors in benign prostatic hyperplasia, urinary and sexual outcomes
World Journal of Urology (2024)
-
In-vivo and in-silico studies revealed the molecular mechanisms of Colocasia esculenta phenolics as novel chemotherapy against benign prostatic hyperplasia via inhibition of 5α-reductase and α1-adrenoceptor
In Silico Pharmacology (2023)
-
Characterisation of the prostanoid receptor mediating inhibition of smooth muscle contractility in the rat prostate gland
Naunyn-Schmiedeberg's Archives of Pharmacology (2010)
-
The α1A‐adrenoceptor gene is required for the α1L‐adrenoceptor‐mediated response in isolated preparations of the mouse prostate
British Journal of Pharmacology (2008)