Abstract
We have previously demonstrated that a slight increase in intracellular superoxide (O2•−) anion confers resistance to death stimuli. Using pharmacological and molecular approaches to manipulate intracellular O2•−, here we report that an increase in intracellular O2•− anion induces Na+/H+ exchanger 1 (NHE-1) gene promoter activity resulting in increased NHE-1 protein expression, which strongly correlates with the resistance of cells to death stimuli. In contrast, exposure to exogenous hydrogen peroxide suppressed NHE-1 promoter activity and gene expression, and increased cell sensitivity to death triggers. Furthermore, the increase in cell sensitivity to death upon downregulation of NHE-1 gene expression correlates with reduced capacity of cells to recover from an acid load, while survival upon overexpression of NHE-1 appears independent of its pump activity. These findings indicate that NHE-1 is a redox-regulated gene, and provide a novel intracellular target for the redox control of cell death sensitivity.
Similar content being viewed by others
Introduction
The involvement of reactive oxygen species (ROS) in biological systems over the years has been restricted to damaging reactions; however, there is mounting evidence to the contrary implicating ROS as important signaling molecules in a variety of physiological processes. In this regard, the regulation of tumor cell sensitivity to death stimuli was shown to be a function of the balance between intracellular levels of superoxide (O2•−) and hydrogen peroxide (H2O2).1, 2, 3, 4 Indeed, an increase in intracellular O2•− concentration, achieved by either its direct overproduction,5 drug induction,6, 7 activation of the small GTPase Rac18 or as a result of an inhibition of the O2•− scavenger Cu/Zn superoxide dismutase (Cu/Zn SOD),6 inhibits tumor cell apoptosis triggered by either the ligation of the CD95 receptor or anticancer drugs. In contrast, H2O2 is a widely accepted trigger of cell death9 and nontoxic levels of H2O2 sensitize cells to death stimuli.10
Earlier reports have highlighted the regulatory role of intracellular redox status on death signaling by demonstrating an effect on caspase family protease, the central executioners of apoptotic signals.11, 12 However, a complete understanding of redox regulation of cell survival pathways is still lacking. Interestingly, recent data from our group suggested that redox regulation of cell survival in tumor cells could be associated with regulation of intracellular pH (pHi).2 Regulation of pHi is accomplished via active extrusion of H+ by the Na+/H+ exchanger (NHE), a membrane antiporter expressed in a variety of cell types. In mammalian cells, the NHE family consists of nine isoforms, Na+/H+ exchanger 1 (NHE-1) to NHE-9. NHE-1, the first isoform cloned, is ubiquitous in its distribution, while other isoforms have more restricted or specialized functions.13, 14, 15, 16 Interestingly, in addition to its role as a principal regulator of pHi and cell volume, NHE-1 has been implicated in cell proliferation, survival and transformation. Growth factors such as serum, epidermal growth factor (EGF) and phorbol ester myristyl acetate (PMA), have all been shown to activate NHE-1 promoter activity.17 Not only is it intriguing that a slight pro-oxidant intracellular environment also shares the prosurvival and proliferative properties of NHE-1, but more interestingly the link between intracellular ROS and NHE-1 is further supported by the observations that the aforementioned inducers of NHE-1 gene expression have also been implicated in intracellular ROS production.
Intrigued by these findings, we set out to investigate if the prosurvival activity of O2•− and NHE-1 was a matter of serendipity, or the result of a true cause and effect relationship. Therefore, we first asked if regulation of NHE-1 gene expression affected cell sensitivity to apoptosis and whether O2•−-induced survival could be mediated trough redox regulation of NHE-1 gene expression. Here, we report that an increase in NHE-1 protein inhibited death execution, while silencing NHE-1 with specific NHE-1 siRNA increased cell sensitivity to death stimuli. Furthermore, using three different murine cell lines (L6 muscle cells, MCT renal fibroblasts and NIH3T3 fibroblasts), the human glioma cells (U87), and a human melanoma cell line (M14), we present evidence that intracellular O2•− is a signal for the activation of the NHE-1 gene promoter that leads to an increase in NHE-1 protein expression. In contrast, exogenous addition of H2O2 inhibited NHE-1 promoter activity, decreased NHE-1 protein level, and sensitized cells to death triggers.
Results
Regulation of NHE-1 gene expression affects cells sensitivity to death triggers
Recent evidence suggests that in addition to regulating pHi, NHE-1 could be a critical regulator of cell sensitivity to death stimuli.18 In agreement with this recent finding, transfection of NIH3T3 cells with increasing concentrations of the pECE-NHE-1 vector resulted in a dose-dependent increase in NHE-1 protein expression that correlated with inhibition of staurosporine-induced cell death (Figure 1a and b). Interestingly, increase in NHE-1 expression and survival did not correlate with a significant increase in pHi and acid-loading recovery capacity of the cells (Figure 1c and d). To the contrary, silencing of NHE-1 expression with a specific NHE-1 siRNA led to a significant sensitization of NIH3T3 cells to the same trigger (Figure 2a and b). Moreover, silencing of NHE-1 led to a maximum of 0.16 U decrease in pHi in cells transfected with 100 nM NHE-1 siRNA (Figure 2c) and a concentration-dependent decreased acid-loading recovery capacity compared to control-transfected cells (Figure 2d). Similar results were obtained with etoposide-induced death (data not shown). It should be noted that in both experiments, cell death was assessed by the βgalactosidase protein (βgal) assay as described in Materials and Methods and reported previously.8 We used this method because it allows for the measurement of cell death in transfected cells only. This approach is particularly important when overexpressing NHE-1 keeping in view the transfection efficiency of ∼30% usually obtained in these experiments. Hence, measurement of cell death in βgal-transfected cells is a better index of the effect of NHE-1 overexpression on cells' response to death triggers. On the contrary, transfection of cells with the specific NHE-1 siRNA routinely affects 90% of the cells. However, in order to compare results obtained by overexpression or downregulation of NHE-1 protein the βgal assay was also used when assessing NIH3T3 cells response to staurosporine-induced cell death upon silencing of the NHE-1 gene expression. Hence, taken together results from Figures 1b and 2b show that staurosporine can either induce from 15 to 48% death in NIH3T3 cells depending on the level of NHE-1 expression. Moreover, in order to assess if cells died by apoptosis, caspase activity using the Ac-DEVD-AFC substrate was measured. Similar to the result obtained with cell death, caspase activity was increased upon silencing of NHE-1 while overexpression of NHE-1 decreased caspase activity (Figure 2e).
Overexpression of NHE-1 inhibits cells' sensitivity to staurosporine-induced cell death but does not increase cells capacity to recover from an acid load. (a) NIH3T3 cells were cotransfected with increasing concentrations of the pECE vector encoding for the human NHE-1 cDNA (pECE-NHE-1) and 0.5 μg of a pCMVβ as described in Materials and Methods. At 48 h post-transfection level of NHE-1 expression was assessed by Western blot analysis. Band intensity of NHE-1/β actin±S.E. from three different transfections has been averaged as % of pECE-transfected cells (% control). (b) Cells death of NHE-1-transfected cells upon incubation with 0.5 μM staurosporine for 18 h was assessed using the βgal assay and expressed as described in Materials and Methods. (c) and (d) NIH3T3 cells were transfected with increasing concentrations of pECE-NHE-1. At 48 h post-transfection (c) expression of NHE-1 and pHi and (d) acid-loading recovery capacity (ΔpH/Δt) in transfected cells were measured as described in Materials and Methods. Gel represents one transfection out of a minimum of three. Results are shown as mean of three experiments±S.E. *P<0.02
Silencing of NHE-1 increases cells sensitivity to staurosporine-induced cell death and inhibits cells' capacity to recover from an acid load. (a) NHE-1 protein expression was silenced using increasing concentrations of a specific NHE-1 siRNA (NHE-1siRNA) or a control siRNA (CosiRNA) as described in Materials and Methods. Gel represents one transfection out of three. (b) At 48 h postsilencing, cell death was triggered for 18 h with 0.5 μM staurosporine before being assessed using the βgal assay as described in Materials and Methods. (c) pHi and (d) acid-loading recovery capacity were measured as described in Materials and Methods. (e) At 48 h post-transfection, NIH3T3 cells mock transfected, transfected with 6 μg pECE-NHE-1 or 100 nM NHE-1siRNA, were incubated with 0.5 μM staurosporine for 12 h before caspase activity was measured as described in Materials and Methods. Mock represents cells transfected without siRNA. *P<0.02
Silencing of NHE-1 prevents O2•−-mediated survival in NIH3T3 cells
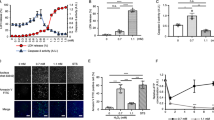
We have previously shown that, similar to the upregulation of NHE-1, an increase in intracellular O2•− achieved by either its overproduction or due to inhibition of the O2•−scavenger Cu/Zn SOD with diethyldithiocarbamate (DDC) inhibited cell death.1, 5 These observations and the results presented above suggest that NHE-1 gene transcription could be one of the targets responsible for O2•−-mediated inhibition of cell death. Hence, to test if an increase in NHE-1 expression could be the mechanism involved in O2•−-mediated survival, we tested the effect of NHE-1 gene silencing with a specific NHE-1 siRNA on the ability of DDC to increase intracellular O2•− and inhibit cell death induced by exposure to 0.5 μM staurosporine for 18 h. As shown in Figure 3a, silencing of NHE-1 gene expression (Figure 3b) did not prevent DDC-induced increase in intracellular level of O2•− in NIH3T3 cells; however, NHE-1siRNA prevented DDC-mediated inhibition of staurosporine-induced cell death (Figure 3c). In these experiments, cell death was assessed using the crystal violet assay, as the transfection efficiency obtained with NHE-1siRNA was routinely around 90% (data not shown). As such, the difference in the assay used to assess cell death might account for variance in the actual percentage of cell death in Figure 3 as opposed to Figure 1, in control- and siRNA-transfected cells in the absence of DDC. Nonetheless, these data demonstrate that DDC-mediated inhibition of staurosporine-induced cell death in NIH3T3 cells is dependent on NHE-1. Moreover, activation of the apoptotic pathway upon incubation of NIH3T3 cells with staurosporine was ascertained by measuring caspase activity. Similar to cell death, incubation with DDC inhibited caspase activity in cells transfected with the vector control while cells in which NHE-1 expression had been silenced did not show a significant difference in caspase activity induced by staurosporine in the presence or absence of DDC (Figure 3d). Furthermore, incubation of NIH3T3 cells with DDC resulted in an increase in NHE-1 expression (Figure 3b), thereby providing additional evidence that O2•− could be a signal for NHE-1 gene expression.
DDC-mediated inhibition of cell death is dependent on NHE-1. NHE-1 gene expression was silenced using a specific NHE-1siRNA as described in Materials and Methods. At 24 h post-transfection, NIH3T3 cells were serum deprived (0.5% serum) for 24 h prior incubation with or without 1 mM DDC for (a) 2 h before measurement of intracellular O2•−, (b) 10 h before NHE-1 expression level was assessed by Western blot and (c) cell death with 0.5 μM staurosporine was assessed using the crystal violet assay. (d) caspase activity was assessed 8 h following induction of cell death. Superoxide level, cell death and caspase activity were assessed and are expressed as described in Materials and Methods. Western blot analysis of NHE-1 expression is a representative experiment out of three. Other results are shown as a mean of three experiments±S.E.*P<0.02
Intracellular superoxide activates NHE-1 promoter activity
A well-documented activator of NHE-1 gene expression is the presence of serum in the cell culture medium.17 Indeed, mouse fibroblast NIH3T3 cells, stably transfected with the 1.1-kb proximal fragment of the mouse NHE1 promoter/enhancer inserted 5′ to the luciferase gene (NIH3T31A8)17 and grown in 10% serum, showed higher NHE-1 promoter activity compared to the same cells grown in 0.5% serum for 18 h (Figure 4a). Moreover, serum-dependent increase in NHE-1 promoter activity correlated with a higher level of NHE-1 protein compared to serum-starved cells (Figure 4b). Incidentally, in addition to an increase in NHE-1 promoter activity, the presence of serum was also a stimulus for the intracellular generation of O2•− that could be partially inhibited by the widely used oxidase inhibitor diphenyleneiodonium (DPI) (Figure 4c). Interestingly, incubation of NIH3T31A8 cells with DPI not only inhibited NHE-1 promoter activity (Figure 4a), but also decreased NHE-1 protein expression to the level of cells grown in 0.5% serum (Figure 4b). These results suggest that ROS such as O2•−could be involved in the increase in NHE-1 expression by serum. The effect of O2•− on NHE-1 gene expression was further supported by the ability of tiron, a specific O2•− scavenger, to revert DDC-induced increases in intracellular O2•−, NHE-1 promoter activity and NHE-1 protein expression in NIH3T3 cells (Figure 5a, b and c). Intracellular O2•− level was measured after 2 h incubation with DDC because we hypothesized that production of O2•− is upstream of NHE-1 promoter activation. Moreover, supporting further the role of O2•− as the ROS involved in induction of NHE-1 gene expression, measurement of H2O2 level using the DCF-DA probe showed that inhibition of O2•− dismutation into H2O2 with DDC or prevention of ROS production with DPI induced a lower level of H2O2 compared to control cells. Moreover, contrary to tiron presence of catalase, neither prevented DDC-mediated increase in intracellular O2•− level nor the activation of NHE-1 promoter activity (data not shown). Taken together these results demonstrate that NHE-1 gene expression is a target for O2•−-mediated inhibition of cell sensitivity to death triggers.
Serum-induced activation of NHE-1 is dependent upon intracellular production of O2•−. NIH3T3 1A8 cells were grown in MEM medium containing 0.5% (0.5% serum), 10% serum (10% serum) or 10% serum and 6 μM DPI (10% serum +DPI) for 2 h before (a) level of O2•−, or for 18 h before (b) NHE-1 promoter activity or (c) NHE-1 protein level, was measured as described in Materials and Methods. NHE-1 promoter activity and intracellular O2•− are expressed as % of cells left in 0.5% serum (% control). For (c) the result shown is a representative experiment out of two. For (a) and (b) results are shown as mean of at least three experiments performed in duplicate±S.E. *P<0.02
O2•− is a signaling molecule for NHE-1 promoter activity. NIH3T3 A8 cells were incubated with MEM medium containing 0.5% FBS for 18 h before 10% serum, 1 mM DDC (0.5% serum/DDC), 1 mM tiron (0.5% serum/tiron) or 1mMDDC plus 1 mM tiron (0.5% serum/DDC+tiron) were added and (a) O2•− level, (b) NHE-1 promoter activity and (c) NHE-1 protein level were assessed after 4, 8 and 18 h, respectively, as described in Materials and Methods. Gel is a representative experiment out of three. Band intensity of NHE-1/β actin from three different experiments has been averaged±S.E. Results are shown as mean of at least three experiments performed in duplicate±S.E. *P<0.02
A pro-oxidant state or increase in intracellular level of ROS such as O2•− is a characteristic of tumor cells,19 and we have previously linked tumor cells' resistance to death triggers to an increase in intracellular O2•− level. Consistent with this, decreasing intracellular level of O2•− restored tumor cell sensitivity to cell death triggers.1, 2, 3 Therefore, we set out to test our findings obtained in NIH3T3 cell in the human glioma cell line U87. Indeed, similar to the results obtained in NIH3T3 cells, DPI-induced decrease in intracellular level of O2•− (Figure 6a) resulted in a significant downregulation of NHE-1 protein expression to the levels obtained with direct silencing of the gene with NHE-1siRNA in U87 cells (Figure 6b). In addition, DPI-mediated downregulation of NHE-1 expression correlated with an increase in sensitivity of U87 cells to etoposide-induced cell death in a manner similar to that obtained upon silencing NHE-1 expression with NHE-1siRNA (Figure 6c). Moreover, activation of the apoptotic pathway upon incubation of U87 cells with etoposide was ascertained by measuring caspase activity. Similar to cell death, caspase activity was higher in the presence of either DPI or upon silencing of NHE-1 compared to control cells. These data suggest that the pro-oxidant milieu of tumor cells (increase in constitutive levels of intracellular O2•−) maintains a level of NHE-1 gene expression that accounts for the resistance of cells to death stimuli.
DPI induces inhibition of NHE-1 expression in U87 cells. NHE-1 gene expression in U87 cells was silenced by either incubation with 6 μM DPI for 18 h or transfection with NHE-1siRNA. (a) Intracellular level of O2•− was measured as described in Materials and Methods. (b) Expression of NHE-1 protein was assessed by Western blot as described in Materials and Methods. Gel represents one experiment out of two. (c) Following NHE-1 silencing with either DPI or NHE-1siRNA cell death was induced by 10 μM etoposide for 18 h and assesses by the crystal violet assay as described in Materials and Methods and (d) caspase activity was measured after 8 h incubation with etoposide as described in Materials and Methods. Results shown are mean of three experiments performed in duplicate±S.E. CosiRNA represents cells transfected with the control siRNA and NHE-1siRNA cells transfected with the specific NHE-1siRNA. *P<0.005
Rac1-mediated survival is dependent upon NHE-1 protein expression
In nonphagocytic cells, production of O2•− has long been attributed to mitochondrial respiration. However, during the 1990s it became increasingly evident that nonphagocytic cells could also produce low levels of O2•− through mechanisms similar to those in phagocytes. In particular, Sudaresan et al.20 showed the production of O2•− upon growth factor-mediated activation of the small GTPase Rac1 in fibroblasts that could be inhibited by the expression of RacN17, the dominant-negative allele of Rac1. Moreover, Irani et al.21, 22 clearly demonstrated the role for Rac1-mediated O2•− production in cell cycle regulation in tumor cells. Coincidently, using Rac1 loss-of-function mutants, we previously demonstrated that resistance to staurosporine- and etoposide-induced cell death in NIH3T3 and in the human melanoma cells M14 correlated with the ability of Rac1 to produce intracellular O2•−.8 Collectively, these data suggest that O2•−-dependent NHE-1 transcription could function as the effector between activation of Rac1 and inhibition of cell death. Indeed, in addition to the decrease in etoposide-induced death in M14 RacV12 cells compared to cells expressing the pIRES vector control, expression of a constitutively active form of Rac1 (RacV12) induced an increase in NHE-1 expression (Figure 7a). However, upon silencing NHE-1 protein (Figure 7a), cells' sensitivity to etoposide in M14RacV12 cells was brought to the level of M14pIRES cells transfected with the control siRNA (Figure 7b). Interestingly, downregulation of NHE-1 expression in M14pIRES cells further increased M14 cells' sensitivity to etoposide-mediated death. These results are in agreement with the results obtained with overexpression or silencing of NHE-1 in NIH3T3 cells and support that increased NHE-1 protein level is involved in Rac1/O2•−-mediated cell survival. Interestingly, contrary to what we found in NIH3T3 cells', increase in NHE-1 protein expression in M14RacV12 cells also led to a higher intracellular pHi compared to M14pIRES that could be decreased upon silencing of NHE-1 (M14RacV12 pHi: 7.74±0.1, M14RacV12/NHE-1siRNA pHi: 7.53±0.06, M14pIRES pHi: 7.48±0.05 and M14pIREs/NHE-1siRNA pHi: 7.22±0.04). However, in agreement with the results obtained in NIH3T3 cells higher level of NHE-1 protein did not lead to an increased acid-loading recovery capacity in M14RacV12 compared to M14pIRES, while NHE-1 silencing decreased the acid-loading recovery capacity in both cells (Figure 7c).
Rac-induced survival is dependent on NHE-1 expression. M14 cells constitutively expressing an active form of Rac1 (M14RacV12) and its vector -expressing counterpart (M14pIRES) were cotransfected with an NHE-1 specific siRNA (NHE-1siRNA) or a control siRNA (cosiRNA) and 0.5 μg pCMVβgal as described in Materials and Methods. At 48 h post-transfection, (a) level of NHE-1 protein, (b) cell death was induced with 40 μM etoposide for 18 h and (c) acid-loading recovery capacity was assessed. Band intensity of NHE-1/β actin from three different experiments has been averaged±S.E. Acid-loading recovery capacity was assessed as described in Materials and Methods. Cell death was determined by the βgal assay as described in Materials and Methods. Results represent an average of three experiments performed in duplicate±S.E. *P<0.002
To support further a role for Rac1 activation in the induction of NHE-1 promoter activity, we used mouse muscle L6 cells (L6 1.1 Kb),23 mouse renal fibroblast MCT cells (MCT 1.1 kb) and NIH3T31A8 cells stably transfected with the 1.1-kb proximal fragment of the mouse NHE1 promoter/enhancer inserted 5′ to a luciferase gene. These cells were transiently transfected with a constitutively active form of Rac1, RacV12 or an empty pIRES vector. A significant increase in NHE-1 promoter activity was observed upon RacV12 transfection compared to the same cells transfected with the pIRES control vector in all three cell types (Figure 8a). Similar results were obtained in NIH3T3 cells stably transfected with the 1.1-kb proximal fragment of the mouse NHE1 promoter/enhancer inserted 5′ to a chloremphenicol acetyl transferase gene (CAT), NIH3T3CatC2 and NIH3T3CatB3 cells (Figure 8b). Hence, data obtained with two different reporter genes in five different cell lines confirm that activation of Rac1 stimulates NHE-1 promoter activity.
Expression of RacV12 induces NHE-1 promoter activity. (a) MCT 1.1 kb, L6 1.1 kb and NIH3T3 1A8 and (b) NIH3T3CatB3 and NIH3T3CatC2 were transiently transfected with pIRESRacV12 or the empty pIRES vector control as described in Materials and Methods. At 48 h post-transfection cells were serum deprived (0.5%serum) for 18 h before (a) luciferase activity or (b) CAT expression was measured as described in Materials and Methods. Results are shown as mean of three independent transfections performed in duplicate±S.E. **P<0.05; *P<0.02
In addition to triggering intracellular production of O2•−, activation of Rac1 has also been shown to regulate actin polymerization and Jun kinase (JNK) activation.24 In order to support that Rac1-mediated induction of NHE-1 gene promoter activity was indeed a function of an increase in intracellular O2•−, NIH3T31A8 cells were transfected with partial myc-tagged loss-of-function mutants of Rac1 containing specific amino-acid substitutions in the activated RacV12 background.8 The RacV12L37 mutant activates JNK but is defective in inducing actin polymerization, whereas the RacV12H40 mutant induces actin polymerization but is defective in JNK activation. However, both of these mutations still retain the ability to generate intracellular O2•−.25 In contrast, the critical role of histidine 103 (H103) and lysine 166 (K166) of Rac1 protein in O2•− production has been established.26 Note that these mutants are the same as those we used to demonstrate that O2•− production was involved in Rac1-mediated survival.8 NIH3T31A8 cells were cotransfected with the pCMVβgal plasmid, which encodes for the βgal and either the pIRES control vector or pIRESRacV12, pIRESRacV12L37, pIRESRacV12H40, pIRESRacV12H103A or pIRESRacV12K166E. At 48 h post-transfection, cells were serum starved (0.5% serum) for 18 h before assessing NHE-1 promoter activity. Cells were serum starved in order to prevent serum-induced activation of the promoter and background activity of the endogenous Rac. Cotransfection with the pCMVβgal plasmid was used to standardize transfection efficiency within the different constructs. It should be pointed out that the βgal activity for each transfection and the level of expression of Rac mutants 48 h post-transfection in NIH3T31A8 cells were not significantly different (data not shown). Hence, the differences in the ability of different plasmids to induce NHE-1 promoter activity could not be attributed to differences in protein expression. In addition, we confirmed that transient transfection of NIH3T3 1A8 cells with pIRESRacV12, pIRESRacV12L37and pIRESRacV12H40 induced a significant increase in intracellular O2•− compared to vector control-transfected cells, while a minimum induction was observed with pIRESRacV12H103A or pIRESRacV12K166E (Figure 9a). Rac1-mediated production of intracellular O2•− always correlated with the ability of Rac1 to increase NHE-1 promoter activity (Figure 9b) but was not linked to JNK activation or actin polymerization. These findings, together with the results obtained with DDC, strongly support that activation of NHE-1 gene promoter is a critical target for O2•−-mediated survival.
NADPH oxidase interaction domain of Rac1 is necessary to Rac1-induced NHE-1 promoter activity. NIH3T3 1A8 cells were transiently transfected with myc-tagged loss-of-function mutants of Rac1. At 48 h post-transfection (a) cells were serum starved for 18 h before production of O2•− was measured as described in Materials and Methods. Results are expressed as % of O2•− increased above cells transfected with the pIRES vector control (% of control) and (b) cells were serum starved for 18 h before NHE-1 promoter activity was measured as described in Materials and Methods. Results are shown as % of cells transfected with the pIRES vector control (% control). Results are shown as mean of at least three independent transfections performed in duplicate±S.E. *P<0.05
H2O2 inhibits NHE-1 gene promoter activity
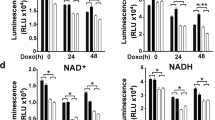
The intracellular concentration of O2•− in eukaryotic cells is tightly regulated by the activity of the enzyme Cu/Zn SOD, which catalyzes the dismutation of O2•− to H2O2 and O2. We therefore asked whether the increase in NHE-1 promoter activity was a direct effect of O2•− on NHE-1 gene transcription or a result of H2O2 production and H2O2-dependent transcription of the NHE-1 gene. To test these possibilities NIH3T3 1A8, NIH3T3CatC2 and NIH3T3CatB3 cells were incubated with increasing concentrations of H2O2 for 18 h before the activity of NHE-1 promoter was assessed. The concentration of H2O2 used throughout this study was ≤150 μM because higher concentrations elicited toxicity (data not shown). Interestingly, in contrast to the stimulatory effect of O2•−, results clearly showed a concentration-dependent inhibition of NHE-1 promoter activity by H2O2 in the three cell types tested (Figure 10a and b). These results were corroborated by Western blot analysis of NHE-1 protein in lysates obtained from NIH3T3 1A8 cells treated for 18 h with H2O2 (Figure 10c). Similar results were obtained with NIH3T3CatC2 and NIH3T3CatB3 (data not shown). Moreover, similar to the result obtained by silencing NHE-1, preincubation of NIH3T3 cells with 50 μM H2O2 for 18 h sensitized NIH3T3 cells to etoposide-induced cell death (Figure 10d). On the contrary, transfection with the pECE-NHE-1 cDNA prevented the decrease in NHE-1 expression and sensitization of NIH3T3 cells to etoposide-induced death as shown by the measurement of caspase activity and NHE-1 protein expression in Figure 10e. Taken together, these data provided strong evidence to support that the expression of NHE-1 is redox regulated, with opposing effects of O2•− and H2O2 on its promoter activity and protein expression. Moreover, the use of two different reporter gene systems rules out the possibility that the observed inhibitory effect on NHE-1 promoter activity could have been attributed to the inhibitory effect of H2O2 on the reporter gene (luciferase or CAT) itself.
H2O2 inhibits NHE-1 promoter activity in NIH3T3 cells. (a) NIH3T31A8, (b) NIH3T3CatB3 and NIH3T3CatC2 cells were incubated with increasing concentrations of H2O2 for 18 h before the NHE-1 promoter activity was measured by either (a) the luciferase assay or (b) detection of the CAT protein and (c) NHE-1 protein level was assessed in NIH3T31A8 as described in Materials and Methods and shown as one representative experiment out of three. (d) NIH3T3 cells were incubated for 18 h with 50 or 100 μM H2O2 before cell death was triggered with 20 (eto 20 μM) or 40 μM etoposide (eto 40 μM). Viability was assessed using the crystal violet assay and the result is shown as OD at 595 nm. (e) NIH3T3 were either mock transfected (mock) or transfected with 6 μg of pECE-NHE-1 (pECE-NHE-1 6 μg). At 48 h post-transfection cells were incubated with 50 μM H2O2 for 18 h before NHE-1 expression level was assessed or cell death was induced with 40 μM etoposide (eto 40 μM) and measured by caspase activity as described in Materials and Methods after 12 h incubation with etoposide. Results are shown as mean of at least two experiments performed in duplicate±S.E. *P<0.02
Discussion
The predominant cellular function of the ubiquitously expressed Na+/H+ exchanger isoform 1, NHE-1, is the regulation of intracellular pH (pHi). The expression of NHE-1 is induced by a variety of external stimuli, such as serum, acidosis, PKC and cell proliferation (for review see16); however, the signals involved in NHE-1 gene transcription remain largely unknown. Recent evidence strongly suggests that, in addition to regulating pHi, NHE-1 could be a critical regulator of cell sensitivity to death stimuli.18 In agreement with these recent findings we show that level of NHE-1 gene expression regulates the sensitivity of mouse fibroblast NIH3T3 cells, the human U87 glioma cells and the human melanoma M14 cells to etoposide- or staurosporine-induced cell death. In addition, we provide evidence that NHE-1 is a redox-regulated gene with a clear divergent effect of O2•− and H2O2; NHE-1 is induced by intracellular O2•− and repressed by H2O2. The effect of O2•− on NHE-1 gene transcription was demonstrated (a) by inhibiting O2•− production using DPI, a widely used inhibitor of O2•−-producing oxidase, (b) by increasing the level of intracellular O2•− using DDC, an inhibitor of the intracytosolic Cu/Zn SOD and (c) by showing that activation of NHE-1 promoter activity by the small GTPase Rac1, a widely accepted essential component for oxidase-mediated production of intracellular O2•−, was indeed due to production of intracellular O2•−.
Over the years data from our laboratory have demonstrated that whereas increased intracellular level of O2•− inhibited cell death, increased intracellular H2O2 sensitized cells to death triggers.1 However, apart from the possible oxidation-mediated inhibition of key enzymes involved in tumor cells' death,11, 12, 27 the exact mechanism involved in O2•−-mediated cell survival is not yet well understood. Data presented here support that NHE-1 could be one such target. Indeed, in absence of NHE-1 gene expression DDC was unable to inhibit staurosporine-induced cell death in NIH3T3 cells despite inducing an increase in intracellular level of O2•−. In addition, using a protocol similar to the one used in the present manuscript, we previously demonstrated that resistance to apoptosis correlated with the ability of Rac1 to produce intracellular O2•−.8 Hence, it was tempting to speculate that O2•−-mediated activation of the NHE-1 promoter activity could couple NHE-1 protein expression with cell survival induced by activation of the small GTPase Rac1. Indeed, our results show that RacV12 induces NHE-1 promoter activity in an O2•−-dependent fashion. Moreover, expression of RacV12 in M14 cells increased NHE-1 expression compared to that in the mock-transfected cells and correlated with a lower sensitivity to etoposide-induced cell death, which could be reverted by silencing NHE-1.
Owing to the fact that redox-regulated transcription factors, such as NFκB and AP-1, have been shown to be activated by H2O2,28, 29 we asked whether the increase in NHE-1 promoter activity in our system was indeed due to O2•− or a function of its dismutated product, H2O2. We provide evidence that nontoxic concentration of H2O2 does not activate the NHE-1 promoter. Instead, incubation of NIH3T31A8 cells with increasing concentration of H2O2 resulted in inhibition of NHE-1 promoter activity. In addition, results showing that inhibition of Cu/Zn SOD with DDC resulted in a significant activation of the promoter also favor O2•− rather than H2O2 in the activation of the NHE-1 gene transcription. Interestingly, we have previously shown that exposure of cells to H2O2 results in a significant decrease in intracellular O2•− through activation of the nuclear protein poly (ADP)-ribose polymerase.10 In light of that, inhibition of NHE-1 promoter activity by H2O2 could be a consequence of a decrease in intracellular O2•− concentration. This hypothesis is supported by data showing that DDC-induced increase in intracellular O2•− can prevent H2O2-mediated inhibition of NHE-1 promoter activity (Kumar A and Clement MV, unpublished data). It should be pointed out that in a previous study using rat cardiomyocytes NHE-1 gene transcription was shown to be induced by H2O2.30 Although, the paradoxical effect of H2O2 in these two systems is not clearly understood, it is plausible that a different set of redox-regulated transcription factors are involved in myocytes compared to cells used in the present study. Notwithstanding the differences, our results provide strong evidence to implicate intracellular redox status in the regulation of NHE-1 promoter activity and gene expression.
These results could have important relevance in tumor cells. Indeed, there is evidence to suggest that transformation and proliferation are favored during intracellular redox imbalance leading to a pro-oxidant intracellular milieu.19 To that effect, mitogenic signal triggered by the oncogene Ras in a fibroblast cell line was attributed to Rac-dependent intracellular production of O2•−, thereby lending support to the hypothesis that O2•−acts as an important proliferative signal during tumorigenesis.22 Along similar lines, Reshkin et al.31 have recently demonstrated that just as efficient Ras-mediated transformation requires activation of Rac, NHE-1 protein expression was equally implicated in malignant transformation and the development of the transformed phenotype.32 Taken together, these findings suggest that, in addition to activation of the exchanger leading to alkaline pHi, redox regulation of NHE-1 gene expression could be critical in tumor cell formation. In particular, resistance of tumor cells to death triggers due to a slight increase in intracellular O2•−could be linked to the regulation of NHE-1 protein expression.
NHE-1-mediated inhibition of cell death has mostly been attributed to its ability to extrude H+ upon death triggers, and thereby create an intracellular environment nonpermissive for death execution. However, overexpression of NHE-1 protein in NIH3T3 cells did not significantly affect pHi. This is not surprising because at physiological pHi, NHE-1 is mostly in a quiescent state. Hence, overexpression of a quiescent H+ pump is not expected to significantly alter pHi. On the contrary, expression of an activated form of Rac1 in M14 tumor cells seems to be responsible for the increase in NHE-1 protein level leading to a significant alkanization of the cytosol, while silencing NHE-1 expression had the opposite effect (acidification). The reason for these effects, as opposed to those noted in NIH3T3 cells, could be due to a higher metabolism of M14 tumor cells, in comparison to NIH3T3 cells, or a greater relative dependence upon the Na+/H+ exchanger for pH regulation. In cells with a low metabolism and low acid production, the Na+/H+ exchanger may be mostly quiescent. In contrast, in cells with a higher steady-state production of acid, varying NHE1 activity or expression may alter intracellular pH more markedly. For example, heart cells have a high rate of metabolism,33 and it has been demonstrated that the Na+/H+ exchanger has a role in steady-state pH regulation. Small though detectable, steady-state rates of Na+/H+ exchange also occur in neuroblastoma cells34 and necturus gallbladder,35 but steady-state pH regulation by the Na+/H+ exchanger is not detectable in cultured skeletal muscle cells36 and thymic lymphocytes.37 In the present study, it appears as though M14 tumor cells fall into the former category, cells with either a high metabolism that requires Na+/H+ exchanger activity, or cells in which other pH regulatory mechanisms are of lesser importance. More interestingly, both NIH3T3 cells expressing an increased level of NHE-1 compared to the NHE-1 steady-state level in cells grown in 10% serum containing medium and M14RacV12 compared to M14pIRES did not show an increase in their acid-loading recovery capacity. To the contrary, silencing NHE-1 in the same cells led to a decrease in pHi and a lower capacity to recover from an acid load. Taken together these results strongly suggest that two mechanisms could be involved in NHE-1-mediated regulation of cells' response to death trigger. The mechanism involved in the increased cell sensitivity upon decrease in NHE-1 expression may be linked to a lower capacity to recover from an acid load. To the contrary, resistance to death trigger due to overexpression of NHE-1 could be linked to a mechanism that may be independent of an increase in NHE-1 capacity to extrude H+. Interestingly, two recent reports have demonstrated that activation of NHE-1 induced prosurvival kinase PKB/AKT in human renal proximal tubule epithelial cells38 and ERK activity in rat aortic vascular smooth muscle cells.39 In the light of these findings and our data presented here, we propose that redox regulation of NHE-1 expression could indirectly influence activation of two well-known survival pathways, that is, the PI3K/AKT and ERK. If this association is proven to be true, the present report could have tremendous implications in our understanding of redox-regulated sensitivity of cells to death triggers and may uncover the molecular mechanism involved in redox-mediated survival in normal and tumor cells.
In summary, this report demonstrates that NHE-1 is a redox-regulated gene and activation of the small GTPase Rac1 activates NHE-1 transcription through intracellular O2•− production. Moreover, we show that level of NHE-1 protein expression can influence cell sensitivity to death triggers. These findings could provide a mechanism for the regulation of cell survival by ROS, particularly in tumor cells, and may be important in enhancing our understanding of the relationship between cell redox status and tumorigenesis.
Materials and Methods
Chemicals
Staurosporine, DPI, lucigenin, DDC, tiron (4,5-dihydro-1,3 benzene disulfonic acid), anti-β actin antibodies, lucigenin and crystal were purchased from Sigma-Aldrich (LO, USA). Etoposide was purchased from Clonetech Laboratories (CA, USA). DPI, Etoposide and staurosporine stock solutions were prepared in dimethyl sulfoxide (DMSO) at 25, 250 and 1 mM, respectively. Dilutions for the experiments were performed in medium. DDC and tiron were directly diluted in culture medium.
Cell lines
Wild-type NIH3T3 cells (ATCC) were maintained in RPMI medium supplemented with 10% fetal bovine serum (Hyclone, Irvine, CA), 1% glutamineand 0.5% gentamicin (Gibco-BRL, Gaithersburg, MD, USA). NIH3T3 cells stably transfected with a 1.1-kb proximal fragment of the mouse NHE1 promoter/enhancer inserted 5′ to a luciferase (NIH3T31A8)17 or a CAT (NIH3T3CatC2 and NIH3T3CatB3),17 MCT cells stably transfected with a 1.1-kb proximal fragment of the mouse NHE1 promoter/enhancer inserted 5′ to a luciferase gene (MCT 1.1 kb) and L6 cells stably transfected with a 1.1-kb proximal fragment of the mouse NHE1 promoter/enhancer inserted 5′ to a luciferase gene (L6 1.1 kb) (34) were maintained in minimum essential medium (MEM), RPMI and DME, respectively, supplemented with 10% fetal bovine serum, 1% glutamine, 0.5% gentamicin (Gibco-BRL, Gaithersburg, MD, USA) and 0.25 mg/ml G418 (Roche Diagnostics Corporation, In, USA). M14 cells stably transfected with a constitutively activated form of Rac (M14RacV12) or the vector control (M14pIRES)8 were maintained in DMEM supplemented with 5% fetal bovine serum, 1% glutamine, 0.5% gentamicin and 0.25 mg/ml hygromycine (Roche Diagnostics Corporation, IN, USA). The U87 human glioma cells (gift from Dr Tang BL, Department of Biochmistry, National University of Singapore) were maintained in RPMI medium supplemented with 10% fetal bovine serum, 1% glutamine and 0.5% gentamicin.
Plasmids used
The partial myc-tagged loss-of-function mutants of Rac1 containing specific amino-acid substitutions in the activated RacV12 background used in this study were all cloned in the pIRES vector as described previously.8 pECE plasmid encoding for the human NHE-1 was a generous gift from Dr Pouyssegur, University of Nice, France. pCMV plasmid encoding for the βgalactosidase protein (pCMVβ) was from Clonetech Laboratories Inc., Palo Alto, CA.
DNA transfection and reporter assays
All cells were transfected using CalPhos™ Mammalian transfection kit (Clonetech Laboratories Inc., Palo Alto, CA). In brief, 0.3 × 106cells/well were plated in 6-well plates 24 h prior to transfection. At 2 h before transfection, the cell culture medium was changed with DMEM supplemented with 5% FBS. To prepare the transfection mixture, 6 μg of DNA, was diluted in sterile dH2O in a microfuge tube, followed by the addition of 12.4 μl of 2.5 M CaCl2 in a total amount of 100 μl/well. The DNA-CaCl2 solution was then mixed dropwise with DNA precipitation buffer (100 μl) while gently vortexing, and the mixture was added to the medium of each well, that is, 200 μl per well. After 16 h incubation, the transfection medium was removed and 2 ml/well of 15% glycerol in phosphate-buffered saline (PBS) was added onto the cells for 90 s (glycerol shock). Cells were then washed twice with PBS and normal tissue culture media added for another 24 h. Cotransfection with the βgal plasmid (Clonetech Laboratories Inc., Palo Alto, CA) was used to assess transfection efficiency in reporter assays and used to assess % of cell death when cotransfected with pECE-NHE-1 or the specific NHE-1 siRNA as described previously in Pervaiz et al.8 βGal activity was measured using the Galacto-Star mammalian reporter Kit (TROPIX, Bedford, MA). Percentage of cell death was measured as 100-((βgal activity μg of protein of transfected cells incubated with the cell death trigger)/(βgal activity μg of protein of transfected cells incubated without the cell death trigger) × 100).
siRNA transfection
21-nucleotide RNAs were chemically synthesized (Xeragon Inc., Germantown MD, USA). 5′-GAUAGGUUUCCAUGUGAUC sequence was used to silence NHE-1 gene transcription (NHE-1siRNA) and 5′-AGCUUCAUAAGGCGCAUGCTT (luciferase gene sequence inverted) sequence was used as a control (CosiRNA). Transfection of siRNAs was carried out using oligofectamine (InVitrogen, Life technologies) and 100 nM of siRNAs per well in a six-well plate. Gene silencing was assayed 48 h post-tranfection by Western blot analysis.
Luciferase reporter gene assay
NHE-1 promoter activity in NIH3T3 1A8, MCT 1.1 kb and L61.1 kb was assessed using the luciferase reporter assay system according to the manufacturer's instructions (Promega, Madison, WI, USA). In brief, cell lysates were prepared using 200 μl/well of lysis buffer provided by the manufacturer. Cell lysate (20 μl) was mixed with 100 μl of luciferase substrate. Luminescence was measured for 10 s in a TD-20/20 Luminometer (Turner Designs, Sunnyvale, CA).
CAT reporter gene assay
In addition to the luciferase reporter gene assay, NHE-1 promoter was assessed using an enzyme immunoassay to determine the expression of the CAT. The Elisa assay was performed according to the manufacturer's instructions (Roche Diagnostics Corporation Inc., USA). Amount of CAT detected is expressed in pg/ml.
Western blot analysis of the NHE-1 protein
Cell lysates were prepared using 300 μl/well of six-well plates of RIPA/NP-40 lysis buffer (5 mM Tris pH7.4, 30 mM NaCl, 1 mM PMSF, 1 μg/ml aprotinin and 0.5% NP-40). A 100 μg of total protein per sample was then subjected to 15% PAGE, transferred to nitrocellulose membrane and blocked for 1 h with 5% fat-free milk in Tris-buffered saline/0.1% Tween 20 (TBST). After three washes with TBST, the membranes were exposed to a 1 : 1000 dilution of a mouse antiporcine NHE1 antibody (Chemicon International Inc., Temecula, CA, USA) at 4°C overnight. The anti-NHE-1 antibody used here crossreacts with all vertebrate NHE-1 proteins including human. Following three washes with TBST, the membrane was exposed to a 1 : 15 000 dilution of goat anti-mouse IgG-HRP conjugate (PIERCE, Rockford, IL, USA) for 1 h and washed repeatedly with TBST. Chemiluminescence was detected using the SuperSignal Substrate (PIERCE, Rockford, IL, USA). Loading control was assessed by the detection of β actine. NHE-1 and β actine protein intensity were measured using the Analytical Imaging Station software version 2.
Intracellular measurement of superoxide
A lucigenin-based chemiluminescence assay was used for the detection of intracellular O2•− as described in Pervaiz and Clement.40 Briefly, cells were washed once with PBS, trypsinized, and centrifuged at 2000 g at room temperature for 1 min. Cell pellets were resuspended and permeabilized in 400 μl of 1 × somatic cell ATP-releasing reagent (Sigma-Aldrich Pte Singapore). Lucigenin solution (100 μl of 850 μM) was injected automatically before the reading. Chemiluminescence was monitored for 60 s in a TD-20/20 Luminometer (Turner Designs, Sunnyvale, CA).
Crystal violet assay
Crystal violet assay was performed to assess NIH3T3 and U87 cells viability following induction of cell death with either staurosporine or etoposide. Crystal violet assay was performed in six- wells following induction of cell death in control cells or cells where NHE-1 expression had been silenced using either 6 μM DPI or NHE-1 siRNA. After 18 h incubation time with the death trigger, the medium was aspirated and replaced for 10 min by 2 ml of 0.75% crystal violet in 50% ethanol, 0.25% NaCl and 1.75% formadehyde solution. Cells were then washed with water, air dried and the dye eluted with PBS/1%SDS. Viability was assessed by dye absorbance determined by optical density (OD) measurement at 595 nm on a Spectrafluorplus plate reader (TECAN). Percentage of cell death was assessed as 1−(OD from cells incubated with the death trigger/OD from control cells) × 100.
Caspase activity assay
Cells were harvested after drug treatment and lysed using 1 × cell lysis buffer (BD Biosciences Pharmingen, San Diego, CA). Cell lysate was added to 2 × reaction buffer (10 mM HEPES, pH7.4, 2 mM EDTA, 6 mM DTT, 10 mM KCl and 1.5 mM MgCl2) supplemented with protease inhibitors and caspase substrate (50 μM) (caspase 3 substrate: Ac-DEVD-AFC) (A.G. Scientific, San Diego, CA) in a 96-well plate. Samples were incubated at 37°C for 1 h and AFC fluorescence was measured using SpectrafluorPlus spectrofluorometer. Caspase activity was normalized with protein amount and expressed as relative fluorescence unit/μg of protein (RFU/μg of protein).
Measurement of intracellular pH and NHE-1 activity
Cells were washed and incubated with 5 μM of BCECF-AM in HCO3−-free HEPES buffer (135 mM NaCl, 5 mM KCl, 1.8 mM CaCl2, 1 mM MgSO4, 5.5 mM glucose, 10 mM HEPES and pH7.4) for 30 min at 37°C. The cells were washed and fluorescence of BCECF was measured (excitation at 485 and 430 nm; emission at 535 nm). pHi was derived by determining the ratio of dual excitation measurement (485 : 430 nm) from a pHi standard curve. To calibrate the relationship between the excitation ratio (485 : 430 nm) and pH, cells loaded with 5 μM BCECF-AM were incubated with 10 μM nigericin for 3 min in high K+ buffer of pH 6.4–8.0, obtained by mixing pH 4 buffer (140 mM KH2PO4 and 20 mM NaCl) and pH 9 buffer (70 mM K2HPO4 and 20 mM NaCl), and fluorescence measurement was taken. After measurement of pHi, the cells were acid loaded with HCO3−-free HEPES buffer containing 30 mM NH4Cl, pH7.4 for 8 min. The cells were then exposed to Na+-free and HCO3−-free HEPES buffer (135 mM N-methyl glucamine, 5 mM KCl, 1.8 mM CaCl2, 1 mM MgSO4, 5.5 mM glucose, 10 mM HEPES and pH7.4) for 30 s and subsequently washed with HEPES buffer. The pH recovery from acid load was monitored every minute for 15 min and NHE-1 activity was determined by the rate of pHi recovery within the first 2 min and is expressed as ΔpH/Δtime (ΔpH/Δt).
Statistical analysis
Statistical analysis was performed using the paired Student's t-test with P<0.05 considered significant.
Abbreviations
- NHE-1:
-
Na+/H+ exchanger 1
- O2•−:
-
superoxide
- H2O2:
-
hydrogen peroxide
- pHi:
-
Intracellular pH
- βgal:
-
βgalactosidase protein
- CAT:
-
chloramphenicol acetyl transferase gene
- DPI:
-
diphenyleneiodonium
References
Pervaiz S and Clement MV (2004) Tumor intracellular redox status and drug resistance—serendipity or a causal relationship? Curr. Pharm. Des. 10: 1969–1977
Pervaiz S and Clement MV (2002) A permissive apoptotic environment: function of a decrease in intracellular superoxide anion and cytosolic acidification. Biochem. Biophys. Res. Commun. 290: 1145–1150
Clement MV and Pervaiz S (1999) Reactive oxygen intermediates regulate cellular response to apoptotic stimuli: an hypothesis. Free Radic. Res. 30: 247–252
Clement MV and Pervaiz S (2001) Intracellular superoxide and hydrogen peroxide concentrations: a critical balance that determines survival or death. Redox. Rep. 6: 211–214
Clement MV and Stamenkovic I (1996) Superoxide anion is a natural inhibitor of FAS-mediated cell death. EMBO J. 15: 216–225
Pervaiz S, Ramalingam JK, Hirpara JL and Clement MV (1999) Superoxide anion inhibits drug-induced tumor cell death. FEBS Lett. 459: 343–348
Ahmad KA, Clement MV, Hanif IM and Pervaiz S (2004) Resveratrol inhibits drug-induced apoptosis in human leukemia cells by creating an intracellular milieu nonpermissive for death execution. Cancer Res. 64: 1452–1459
Pervaiz S, Cao J, Chao OS, Chin YY and Clement MV (2001) Activation of the RacGTPase inhibits apoptosis in human tumor cells. Oncogene 20: 6263–6268
Hirpara JL, Clement MV and Pervaiz S (2001) Intracellular acidification triggered by mitochondrial-derived hydrogen peroxide is an effector mechanism for drug-induced apoptosis in tumor cells. J. Biol. Chem. 276: 514–521
Clement MV, Ponton A and Pervaiz S (1998) Apoptosis induced by hydrogen peroxide is mediated by decreased superoxide anion concentration and reduction of intracellular milieu. FEBS Lett. 440: 13–18
Hampton M and Orrenius S (1998) Redox regulation of apoptotic cell death. Biofactors 8: 1–5
Chandra J, Samali A and Orrenius S (2000) Triggering and modulation of apoptosis by oxidative stress. Free Radic. Biol. Med. 29: 323–333
Brett CL, Wei Y, Donowitz M and Rao R (2002) Human Na(+)/H(+) exchanger isoform 6 is found in recycling endosomes of cells, not in mitochondria. Am. J. Physiol. Cell Physiol. 282: C1031–C1041
Goyal S, Vanden Heuvel G and Aronson PS (2003) Renal expression of novel Na+/H+ exchanger isoform NHE8. Am. J. Physiol. Renal Physiol. 284: F467–F473
Numata M and Orlowski J (2001) Molecular cloning and characterization of a novel (Na+,K+)/H+ exchanger localized to the trans-Golgi network. J. Biol. Chem. 276: 17387–17394
Putney LK, Denker SP and Barber DL (2002) The changing face of the Na+/H+ exchanger, NHE1: structure, regulation, and cellular actions. Annu. Rev. Pharmacol. Toxicol. 42: 527–552
Besson P, Fernandez-Rachubinski F, Yang W and Fliegel L (1998) Regulation of Na+/H+ exchanger gene expression: mitogenic stimulation increases NHE1 promoter activity. Am. J. Physiol. 274: C831–C839
Wu KL, Khan S, Lakhe-Reddy S, Wang L, Jarad G, Miller RT, Konieczkowski M, Brown AM, Sedor JR and Schelling JR (2003) Renal tubular epithelial cell apoptosis is associated with caspase cleavage of the NHE1 Na+/H+ exchanger. Am. J. Physiol. Renal. Physiol. 284: F829–F839
Cerutti PA (1985) Prooxidant states and tumor promotion. Science 227: 375–381
Sundaresan M, Yu Z-X, Ferrans VJ, Sulciner DJ, Gutkind JS, Iranis K, Goldschmidt-Clermont PJ and Finkel T (1996) Regulation of reactive-oxygen-species generation in fibroblasts by Rac1. Biochem. J. 318: 379–382
Irani K and Goldschmidt-Clermont PJ (1998) Ras, superoxide and signal transduction. Biochem. Pharmacol. 55: 1339–1346
Irani K, Xia Y, Zweier JL, Sollott SJ, Der CJ, Fearon ER, Sundaresan M, Finkel T and Goldschmidt-Clermont PJ (1997) Mitogenic signaling mediated by oxidants in Ras-transformed fibroblasts. Science 275: 1649–1652
Yang W, Dyck JR and Fliegel L (1996) Regulation of NHE1 expression in L6 muscle cells. Biochim. Biophys. Acta. 1306: 107–113
Campbell SL, Khosravi-Far R, Rossman KL, Clark GJ and Der CJ (1998) Increasing complexity of Ras signaling. Oncogene 17: 1395–1413
Joneson T and Bar-Sagi D (1998) A Rac1 effector site controlling mitogenesis through superoxide production. J. Biol. Chem. 273: 17991–17994
Toporik A, Gorzalczany Y, Hirshberg M, Pick E and Lotan O (1998) Mutational analysis of novel effector domains in Rac1 involved in the activation of nicotinamide adenine dinucleotide phosphate (reduced) oxidase. Biochemistry 37: 7147–7156
Hampton MB, Fadeel B and Orrenius S (1998) Redox regulation of the caspases during apoptosis. Ann. NY Acad. Sci. 854: 328–335
Baeuerle PA and Baltimore D (1996) NF-kappa B: ten years after. Cell 87: 13–20
Bowie A and O'Neill LA (2000) Oxidative stress and nuclear factor-kappaB activation: a reassessment of the evidence in the light of recent discoveries. Biochem. Pharmacol. 59: 13–23
Gan XT, Chakrabarti S and Karmazyn M (1999) Modulation of Na+/H+ exchange isoform 1 mRNA expression in isolated rat hearts. Am. J. Physiol. 277: H993–H998
Qiu RG, Chen J, Kirn D, McCormick F and Symons M (1995) An essential role for Rac in Ras transformation. Nature 374: 457–459
Reshkin SJ, Bellizzi A, Caldeira S, Albarani V, Malanchi I, Poignee M, Alunni-Fabbroni M, Casavola V and Tommasino M (2000) Na+/H+ exchanger-dependent intracellular alkalinization is an early event in malignant transformation and plays an essential role in the development of subsequent transformation-associated phenotypes. FASEB J. 14: 2185–2197
Piwnica-Worms D, Jacob R, Horres CR and Lieberman M (1985) Na/H exchange in cultured chick heart cells. pHi regulation. J. Gen. Physiol. 85: 43–64
Moolenaar WH, Boonstra J, van der Saag PT and de Laat SW (1981) Sodium/proton exchange in mouse neuroblastoma cells. J. Biol. Chem. 256: 12883–12887
Weinman SA and Reuss L (1982) Na+–H+ exchange at the apical membrane of Necturus gallbladder* Extracellular and intracellular pH studies. J. Gen. Physiol. 80: 299–321
Vigne P, Frelin C and Lazdunski M (1982) The amiloride-sensitive Na+/H+ exchange system in skeletal muscle cells in culture. J. Biol. Chem. 257: 9394–9400
Grinstein S, Cohen S and Rothstein A (1984) Cytoplasmic pH regulation in thymic lymphocytes by an amiloride-sensitive Na+/H+ antiport. J. Gen. Physiol. 83: 341–369
Wu KL, Khan S, Lakhe-Reddy S, Jarad G, Mukherjee A and Obejero-Paz CA et al. (2004) The NHE1 Na+/H+ exchanger recruits ezrin/radixin/moesin proteins to regulate Akt-dependent cell survival. J. Biol. Chem. 279: 26280–26286
Mukhin YV, Garnovskaya MN, Ullian ME and Raymond JR (2004) ERK is regulated by sodium-proton exchanger in rat aortic vascular smooth muscle cells. J. Biol. Chem. 279: 1845–1852
Pervaiz S and Clement MV (2002) Hydrogen peroxide-induced apoptosis: oxidative or reductive stress? Methods Enzymol. 352: 150–159
Acknowledgements
This work was supported by Grant R-183-000-084-213 from The National Medical Research Council of Singapore to MVC, R-185-000-072-305 from the Biomedical Research Council of Singapore to MVC and SP and the Canadian Institute of Health Research to LF.
Author information
Authors and Affiliations
Corresponding author
Additional information
Edited by A Finazzi-Agrò
Rights and permissions
About this article
Cite this article
Akram, S., Teong, H., Fliegel, L. et al. Reactive oxygen species-mediated regulation of the Na+–H+ exchanger 1 gene expression connects intracellular redox status with cells' sensitivity to death triggers. Cell Death Differ 13, 628–641 (2006). https://doi.org/10.1038/sj.cdd.4401775
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cdd.4401775
Keywords
This article is cited by
-
JAK2V617F mediates resistance to DNA damage-induced apoptosis by modulating FOXO3A localization and Bcl-xL deamidation
Oncogene (2016)
-
Endothelial Na+/H+ exchanger NHE1 participates in redox-sensitive leukocyte recruitment triggered by methylglyoxal
Cardiovascular Diabetology (2014)
-
NHE1 gene associated with avian leukosis virus subgroup J infection in chicken
Molecular Biology Reports (2014)
-
Myocardial Na+/H+ exchanger-1 (NHE1) content is decreased by exercise training
Journal of Physiology and Biochemistry (2013)
-
Vasculoprotective effect of cilostazol in aldosterone-induced hypertensive rats
Hypertension Research (2010)