Abstract
Lipoxygenases are a family of enzymes which dioxygenate unsaturated fatty acids, thus initiating lipoperoxidation of membranes and the synthesis of signaling molecules. Consequently, they induce structural and metabolic changes in the cell in a number of pathophysiological conditions. Recently, a pro-apoptotic effect of lipoxygenase, and of the hydroperoxides produced thereof, has been reported in different cells and tissues, leading to cell death. Anti-apoptotic effects of lipoxygenases have also been reported; however, this has often been based on the use of enzyme inhibitors. Here we review the characteristics of the lipoxygenase family and its involvement in the initiation of oxidative stress-induced apoptosis. Finally, we discuss the role of lipoxygenase activation in apoptosis of animal and plant cells, suggesting a common signal transduction pathway in cell death conserved through evolution of both kingdoms. Cell Death and Differentiation (2001) 8, 776–784
Similar content being viewed by others
The lipoxygenase family
Lipoxygenases (linoleate:oxygen oxidoreductase, EC 1.13.11.12; LOXs) are a family of monomeric non-heme, non-sulfur iron dioxygenases, which catalyze the conversion of polyunsaturated fatty acids into conjugated hydroperoxides. The unsaturated fatty acids, which are essential in humans, are absent in most bacteria and thus LOXs are also absent in typical prokaryotes. LOXs are widely expressed in animal and plant cells, sometimes at high level, and their activity may initiate the synthesis of a signaling molecule or may induce structural or metabolic changes in the cell. Mammalian lipoxygenases have been implicated in the pathogenesis of several inflammatory conditions such as arthritis, psoriasis and bronchial asthma.1 They are also thought to have a role in atherosclerosis, brain aging, HIV infection, kidney disease and terminal differentiation of keratinocytes. In plants, lipoxygenases favor germination, participate in the synthesis of traumatin and jasmonic acid and in the response to abiotic stress.2
The phylogenetic tree shows that plant and animal LOXs are separate branches, each forming several subgroups.3 When arachidonic (eicosatetraenoic, C20:4; ETE) acid is the substrate, different LOX isozymes can add a hydroperoxy group at carbons 5, 12 or 15, and therefore they are designated 5-, 12- or 15-lipoxygenases. Linoleic (octadecadienoic, C18:2; OD) acid and linolenic (octadecatrienoic, C18:3; OT) acid are also substrates of LOXs. Soybean (Glycine max) lipoxygenase-1 (LOX-1) is a 15-lipoxygenase widely used as a prototype for studying the homologous family of lipoxygenases from tissues of different species, both in structural4 and kinetic5 investigations.
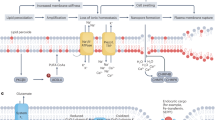
The primary sequence and three dimensional structure of LOX-1 have been determined, showing that it is an ellipsoid of 90 by 65 by 60 Å, with 839 amino acid residues and a molecular mass of 93840 Da.3 LOX-1 is made of two domains: a 146-residue β-barrel at the N-terminal (domain I) and a 693-residue helical bundle at the C-terminal (domain II). The iron-containing active site is in the center of domain II, liganded to four conserved histidines and to the carboxyl group of the C-terminal conserved isoleucine. It can be reached through the two cavities (I and II), as shown in Figure 1. Cavity I presents an ideal path for the access of molecular oxygen to iron, whereas cavity II can accommodate arachidonic acid or even slightly larger fatty acids. Mammalian lipoxygenases lack the N-terminal domain present in LOX-1 and related plant lipoxygenases, thus showing smaller molecular mass (75–80 kDa compared to 94–104 kDa in plants). The N-terminal domain in LOX-1 makes only a loose contact with the C-terminal domain; this may be dispensable for plant lipoxygenases, because all the amino acid side chains responsible for catalysis are located in the C-terminal domain. However, limited proteolysis experiments indicated that the two domains are instead tightly associated, and that domain–domain interactions play a role in the reversible unfolding of LOX-1, through ionic interactions. LOX-1 is usually in the inactive Fe2+ form and oxidation to the active Fe3+ enzyme is required for catalysis. Substrate dioxygenation by LOX-1 can be explained by two different mechanisms, indicated as ‘free-radical’ and ‘organoiron’ respectively, both compatible with the iron coordination in the active site (Figure 2A). They explain in different ways the C-H bond cleavage of the substrate, which is the rate-limiting step of the overall dioxygenation reaction.3 The free radical mechanism assumes an involvement of Fe in the (stereospecific) hydrogen abstraction from the methylene group in the pentadiene system of the substrate, yielding a free radical intermediate. The hydrogen removal implies the reduction of Fe3+ to Fe2+ (Figure 2B). The organoiron hypothesis involves concerted deprotonation, catalyzed by a basic group (B) in the active site and electrophilic attack of Fe on the substrate, without any formal change in the iron oxidation state (Figure 2C).
Schematic diagram of the three-dimensional structure of soybean (Glycine max) lipoxygenase-1, showing the small N-terminal domain I and the large C-terminal domain II. The iron-containing active site is located in domain II, and can be reached by molecular oxygen through cavity I and by arachidonic acid through cavity II. The β-sandwiches are represented in yellow, the α-helices in blue, the random coils in gray and the iron in red. The three-dimensional structure was modeled through the MOLSCRIPT program, using the lipoxygenase-1 sequence (PDB accession number: 2SBL)
(A) Current views of the iron coordination in the active site of soybean (Glycine max) lipoxygenase-1: coordination by four ligands, forming a highly distorted octahedron with two unoccupied positions (I); coordination by six ligands, forming a slightly distorted octahedron (II). The free-radical model (B) and the organoiron model (C) of lipoxygenase catalysis are compatible with both views of iron coordination. See text for details
In mammals, most work has been done on 5-lipoxygenase (arachidonate:oxygen 5-oxidoreductase, EC 1.13.11.34; 5-LOX), which is found primarily in polymorphonuclear leukocytes, macrophages and mast cells, where it plays a central role in cellular leukotriene synthesis. The interaction of human 5-LOX with cellular proteins has been recently investigated through the two-hybrid approach,6 showing that this enzyme binds to proteins as different as a coactosin-like protein (an element of the cytoskeleton), a transforming growth factor (TGF) type β receptor-I-associated protein 1 (involved in TGF signaling), and a hypothetical helicase (a DNA metabolizing enzyme). Complex protein-protein interactions have been demonstrated in nuclear membrane translocation, activation and substrate binding by 5-LOX in intact cells.3 In fact, cell activation by different stimuli results in translocation of 5-LOX to the nuclear membrane, where it associates with a ‘5-LOX activating protein’ (FLAP), an 18 kDa integral membrane protein which acts as an arachidonic acid transfer protein and is essential for full leukotriene biosynthesis. FLAP shows homology with leukotriene C4 synthase and other microsomal glutathione transferases, but no enzymatic activity itself. Initially, FLAP was believed to be localized at the outer cell membrane, but later it became clear that it is associated with the nuclear envelope. Thus, arachidonic acid released from the nuclear membrane of leukocytes, and presented to 5-LOX by FLAP, may be the substrate for leukotriene synthesis.3 Recently, growing evidence has accumulated suggesting that FLAP can have effects independent of 5-LOX.7 Also regulatory, nonenzymatic activities of 5-LOX have been reported, made possible by an Src homology 3 (SH3) binding motif, which enables the interaction with growth factor receptor-bound protein 2 (Grb2) and cytoskeletal proteins.6 In this line, a possible interaction of 5-LOX with the nuclear factor-κB (NF-κB) complex seems to indicate that 5-LOX protein might also indirectly influence gene transcription.6 The ability of 5-LOX to enter the nucleus supports its regulatory role on the transcription process, though possible nonenzymatic functions of 5-LOX protein wait to be investigated.
Lipoxygenase involvement in apoptotic pathways
LOX products have been shown to induce PCD in human T cells,8 neutrophils,9 PC12h cells10 and Jurkat cells.11 Therefore, it is not surprising that activation of lipoxygenases has been associated to programmed death of different cells and tissues, induced by different, unrelated stimuli (Table 1 and references therein). Several studies have shown the pro-apoptotic activity of 5-LOX,15,23 of leukocyte type 12-LOX,21,26 and of 15-LOX,24,28 and have indicated molecular targets for lipoxygenase interaction able to contribute to the induction of apoptosis (Table 2 and references therein). However, also anti-apoptotic effects of LOXs have been reported, mainly based on the observation that LOX inhibitors, most often nordihydroguaiaretic acid (NDGA) and MK886, had pro-apoptotic activity.30,35,37,38 Interestingly, in other cellular types NDGA or MK886 protected against apoptosis,12,13,14,15,21,28,36 or induced PCD in cell types completely devoid of LOX activity.7,32,39 In this context, it should be recalled that most of the LOX inhibitors used in PCD studies, including NDGA, act by reducing the active Fe3+ enzyme to the inactive Fe2+ form (Figure 3). NDGA also blocks voltage-activated calcium currents, inhibits P450 monooxygenase activity and acts as a general radical scavenger.12 On the other hand, MK886, which inhibits 5-LOX by blocking FLAP, can also induce PCD via a caspase-3-dependent pathway which is related to bcl-xL but unrelated to 5-LOX.7 Recently, MK886 has been found to be effective as PCD inducer at doses 100-fold higher than those required for 5-LOX inhibition, in a human cell line which lacks FLAP and its mRNA.7 Resveratrol, an alleged natural cancer preventive agent present in red wine,40 has been shown to inhibit PCD induced by unrelated stimuli in human erythroleukemia K562 cells, through competitive inhibition of 5-LOX and 15-LOX activity.41 However, resveratrol is a general antioxidant which also inhibits nonenzymatic lipoperoxidation and cyclooxygenase activity41 and acts as an agonist for the estrogen receptor.42 Finally caffeic acid, which prevents apoptosis linked to 5-LOX activation,15 is a LOX inhibitor with general antioxidant properties,43 much like the 5-LOX inhibitor α-tocopherol.44 In a recent investigation, we sought to overcome the problem of the specificity of LOX inhibitors, by treating human cells with physiological concentrations of the hydroperoxide products generated by the main mammalian lipoxygenase isozymes: 5-, 12- and 15-hydroperoxyeicosatetraenoic acids (5-, 12- and 15-HPETE), 13-hydroperoxyoctadecadienoic acid (13-HPOD) and 13-hydroperoxy-octadecatrienoic acid (13-HPOT). The structure of these hydroperoxides is shown in Figure 4. We demonstrated that all these hydroperoxy fatty acids are fully capable of eliciting apoptotic bodies formation, both in human erythroleukemia and neuroblastoma cells.13 The most active compound is that generated by 5-lipoxygenase from arachidonate (5-HPETE), followed by 13-HPOT, 15-HPETE, 9-HPOT, 9-HPOD, 13-HPOD and 12-HPETE. In this context, it should be recalled that mammalian cells can reduce the lipid hydroperoxides (LOOH) to the purportedly less toxic hydroxides (LOH), in a reaction requiring glutathione (GSH) and catalyzed by glutathione peroxidase:45
Hydroperoxides generated by different lipoxygenases (LOXs) with arachidonic, linoleic or linolenic acids as substrates. The hydroperoxides can be reduced to the corresponding hydroxides by cellular glutathione peroxidases, which concomitantly convert reduced glutathione (GSH) to its oxidized form (GSSG). Asterisks mark the hydro(pero)xide position in 9-H(P)OD and 9-H(P)OT

Therefore, depletion of intracellular GSH might enhance hydroperoxide-induced PCD, by analogy with other apoptotic pathways such as that induced by Fas. However, we found that apoptosis induced by LOX products was independent of intracellular GSH, and that the hydroxides derived by reduction of the LOX hydroperoxy products were as effective in inducing PCD as the corresponding peroxides. These findings are at variance with previous reports that some lipoxygenase products (namely, 12- and 15-HETEs, but not their metabolic precursors 12- and 15-HPETEs) may protect cells, whereas others (namely, 5-HETE) are toxic.30,38 Unlike the hydro(pero)xides, the terminal products of the LOX pathway (leukotrienes) are not cytotoxic.33 Moreover, neither RNA nor protein synthesis appear to have a role in lipid hydro(pero)xide-induced PCD, which instead is paralleled by an increase (within seconds) in intracellular calcium,33 extending previous observations on unrelated models of PCD.21,35,46 The mechanism of the hydroperoxide-induced calcium increase is not due to an increase in permeability of the plasma membrane, since calcium was absent in the extracellular medium. Most probably, the hydro(pero)xides may stimulate the release of calcium from mitochondrial and endoplasmic stores.8 This hypothesis is in agreement with the observation that they are also able to uncouple mitochondria within hours.33 It is noteworthy that 15-LOX activity can dioxygenate mitochondrial membranes, leading to formation of pore-like structures observable by electron microscopy also in membranes of endoplasmic reticulum, thus initiating programmed organelle disruption.47 On the other hand, the role of mitochondria as key players in death programmes is well established,48 yet the mechanisms responsible for the release of mitochondrial components which affect apoptosis remain obscure.49
Here, we sought to assess whether lipoxygenase activity might cause mitochondrial damage associated to apoptosis. We isolated mitochondria from human erythroleukemia K562 cells, and studied the effect induced by LOXs on: (i) the oxidative index of membranes, a marker of lipoperoxidation; (ii) the dissipation of mitochondrial membrane potential; and (iii) the release of cytochrome c, using specific anti-cytochrome c monoclonal antibodies in the enzyme-linked immunosorbent assays.50 Mitochondria were treated with pure soybean lipoxygenase-1, which is a 15-LOX widely used as a prototype for studying the structural and kinetic properties of mammalian lipoxygenases.3,4,5
We found that treatment of mitochondrial suspensions with amounts of soybean 15-LOX within the physiological range,47 dose-dependently increased the oxidative index (up to threefold over the control) and the uncoupling of mitochondria (up to eightfold over the control), both indicative of the disruption of membrane integrity (Figure 5A). Remarkably, incubation of mitochondria with 15-LOX caused also a dose-dependent release of cytochrome c (up to fivefold over the control), a critical trigger of apoptosis induced by several unrelated stimuli.51 The lipoxygenase inhibitors eicosatetraynoic acid (ETYA) and n-propyl gallate (nPG) fully prevented these effects of 15-LOX (Figure 5A), corroborating the previous observation that they block 15-LOX-dependent formation of pore-like structures in endoplasmic reticulum membranes.47 On the other hand, cyclosporin A, a mitochondrial permeability transition pore inhibitor,49 was ineffective (Figure 5A), suggesting that opening of this type of pores did not contribute to mitochondrial membrane disruption by 15-LOX. We extended the study to the other available LOX isozymes, incubating mitochondrial suspensions under the same experimental conditions as those used with soybean 15-LOX. We found that rabbit reticulocyte 15-LOX was more effective than the soybean enzyme, whereas barley (Hordeum vulgare) 5-LOX was as effective and human platelet 12-LOX was less effective than soybean 15-LOX (Figure 5B).
(A) Dose-dependence of different mitochondrial parameters on the amount of soybean 15-lipoxygenase (15-LOX). Suspensions of mitochondria (200 μl/test) were incubated for 3 h at 25°C, and controls were treated with incubation buffer alone (140 mM NaCl, 5 mM KCl, 1 mM MgCl2, 1.8 mM CaCl2, 10 mM glucose, 0.1% bovine serum albumin, 15 mM HEPES, pH 7.4). Lipoxygenase inhibitors eicosatetraynoic acid (EYTA, 10 μM) and n-propyl gallate (nPG, 100 μM), and permeability transition pore inhibitor cyclosporin A (CycA, 10 μM), were added to the mitochondrial suspensions at the same time as 15-LOX. All increases induced by 15-LOX were significant vs controls: P<0.05 for oxidative index and cytochrome c release at 25 units/test, P<0.01 in all other cases. *P<0.01, **P>0.05 vs samples treated with 15-LOX (100 units/test). (B) Effect of different LOX isozymes on the same mitochondrial parameters as those shown in A. *P<0.05 vs controls; in all other cases, P values vs controls were <0.01. Results are shown as mean±S.D. of four independent experiments, each performed in duplicate
Taken together, the present results suggest that lipoxygenases, in the order 15-LOX>5-LOX>12-LOX, are able to disrupt mitochondrial integrity and to trigger cytochrome c release, thus giving a biochemical ground to the observation that activation of these enzymes is critical in different models of apoptosis (Table 1). It can be suggested that LOXs, by introducing molecular oxygen into the fatty acid moieties of (phospho)lipids and thus increasing membrane lipoperoxidation (Figure 5), can alter fluidity and permeability of biomembranes. These modifications might be the basis for the formation of pore-like structures in membranes,47 which cause dissipation of the mitochondrial potential and favor cytochrome c release (Figure 5). Remarkably, this LOX-mediated disruption of mitochondrial integrity represents a controlled mechanism, which might allow the ‘delicate’ (i.e., without severe damage of structure and function) release of cytochrome c observed in various models of apoptosis.51 In conclusion, we suggest that activation of LOXs might be a means to disrupt the integrity of mitochondria and to allow the release of pro-apoptotic proteins from these organelles. Further work should be aimed at ascertaining whether the effects of LOX on mitochondria can be inhibited by Bcl-2 family members.52 This information would be of great value for understanding more general aspects of the release of apoptotic factors from mitochondria and, for example, the relationship with the permeability transition. In this line, it may be worth reminding that lipoxygenase activation has been shown to affect also cytoskeleton organization and protein phosphorylation,6 which can be instrumental in promoting PCD. In fact, we have previously shown that LOX activation is an early event along different apoptotic pathways, and occurs several hours before any typical sign of apoptosis at nuclear level.15,53 Furthermore, early LOX activation was not observed in necrotic cells,53 thus representing the first biochemical difference between the initiation of apoptosis and that of necrosis so far described.
Overall, physical (UV-light) or chemical (drugs, oxidative stress, serum starvation) induction of PCD, as well as apoptotic pathways mediated by receptors such as CD28, interleukin receptor or Fas, have been shown to involve LOX activation, which in turn is accompanied by modifications of: (i) membrane properties (lipoperoxidation, exposure of phosphatidylserine, increased levels of cholesterol and consequent altered Ras expression, generation of free hydroperoxides); (ii) cytoskeleton (at the level of coactosin-like protein, lamins, Gas 2 and α-fodrin), and (iii) gene transcription (through NF-κB, poly(ADP-ribose) polymerase and reactive oxygen species). We could therefore hypothesize a model of ‘Redox Stress Sensor’, depicted in Figure 6. LOX activity generates toxic intermediates (such as hydroperoxides and superoxide anions), which lead to apoptosis by increasing membrane fluidity and permeability, intracellular calcium concentration, mitochondrial uncoupling and cytochrome c release. The intracellular level of glutathione, regulated by N-acetylcysteine, counteracts the effect of LOX activity, also by possibly promoting detoxification of its intermediates. The equilibrium between LOX and glutathione might interfere with the intracellular level of reactive oxygen species. Collectively, the balance between these elements, and the status of the membranes, will finely tune the sensitivity of the cell to resist to redox stresses or to die.
The ‘Redox Stress Sensor’ model, whereby lipoxygenase (LOX) activity generates toxic intermediates (TI), which lead to apoptosis by (i) increasing membrane fluidity (F) and permeability (P), (ii) elevating intracellular calcium concentration ([Ca]i), (iii) decreasing mitochondrial membrane potential (ΔΨm), and (iv) increasing cytochrome c (Cyt c) release. The intracellular level of glutathione (GSH), regulated by N-acetylcysteine (NAC), counteracts the effect of LOX activity, also by possibly promoting detoxification of TI to non-toxic species. The equilibrium between LOX and GSH might interfere with the intracellular level of reactive oxygen species (ROS). This picture is further complicated by the ability of LOX to induce directly the events triggered by the toxic intermediates
Plant lipoxygenases and apoptosis
In plants, PCD has been associated to various phases of development and senescence, germination, and response to cold or salt stress.54 A type of PCD of particular interest has been observed during the plant response to pathogen attack, that was termed ‘hypersensitive response (HR)’.17,54 Signal transduction pathways are activated during HR, leading to biosynthesis or release of potential antimicrobial effector molecules, which are thought to contribute to both host and pathogen cell death.54 Among other signals, rapid generation of reactive oxygen species has been implicated in HR of plants against pathogens.17 In particular, hydrogen peroxide has been shown to be a crucial component of the HR control circuit, since a short pulse of exogenous H2O2 is sufficient to activate the hypersensitive cell death program in soybean cells.17 A similar HR has been observed also in bean,16 pepper18 and tobacco19 leaves, infected with different pathogens. Interestingly, LOX activation has been associated to HR,18,19 and H2O2 oxidative stress has been shown to induce animal cell apoptosis, through activation of 5-LOX.15
Recently, we have used oxidative stress by exogenous H2O2 to investigate whether LOX activation was a cause rather than an effect of plant cell apoptosis. Lentil (Lens culinaris) lipoxygenase has been characterized, cloned and expressed in Escherichia coli,55 therefore lentil root protoplasts (LRP) were chosen as a model. It was shown that the early phase of hydrogen peroxide-induced apoptosis is characterized by enhancement of lipoxygenase activity, attributable to up-regulation of gene expression at both transcriptional and translational level. The increase of lipoxygenase was paralleled by an enhancement of ultraweak luminescence, a marker of LOX-related membrane lipid peroxidation.20 These findings suggest that lipoxygenase activation might contribute to membrane peroxidation during hydrogen peroxide-induced CPD, resembling previous observations on animal cells.15 NDGA protected LRP against H2O2-induced DNA fragmentation and ultraweak luminescence. However, in view of the lack of specificity of this LOX inhibitor, we also used inhibitory anti-LOX monoclonal antibodies, able to block LOX activity in LRP without affecting the redox state of the cell.20 These antibodies, too, protected LRP against H2O2-induced PCD, whilst the specific products of LRP lipoxygenase, 9-HPOD and 13-HPOD, were able per se to induce DNA fragmentation.20 Also 9-HOD and 13-HOD, the reduced forms of the LRP LOX products, were able to induce cell death and DNA fragmentation to almost the same extent as the corresponding HPODs, again matching previous observations on human cells.20 Since similar findings were reported in H2O2-induced PCD of human cells, these observations suggest that animals and plants share a common signal transduction pathway triggering apoptosis after oxidative stress.
Conclusions
Activation of different LOX isozymes has been shown to be associated to an early phase of apoptosis, triggered by several, unrelated stimuli. Consistently, LOXs and the hydro(pero)xides generated by their activity have been shown to induce programmed cell death in different cellular models, through a series of events including an immediate and sustained rise in cytosolic calcium (within seconds), followed by mitochondrial uncoupling and cytochrome c release (within hours). Animal and plant cells share a similar signal transduction pathway able to trigger apoptosis after oxidative stress, based on lipoxygenase activation.
Abbreviations
- CycA:
-
cyclosporin A
- ERK:
-
extracellular regulated kinase
- ETE:
-
eicosatetraenoic (arachidonic) acid
- ETYA:
-
eicosatetraynoic acid
- FLAP:
-
5-lipoxygenase activating protein
- GSH:
-
reduced glutathione
- H(P):
-
hydro(pero)xide
- HR:
-
hypersensitive response
- IL-R:
-
interleukin receptor
- LO(O)H:
-
lipid hydro(pero)xide
- LOX:
-
lipoxygenase
- LRP:
-
lentil root protoplast
- MAPK:
-
mitogen-activated protein kinase
- NAC:
-
N-acetylcysteine
- NDGA:
-
nordihydroguaiaretic acid
- NF-kB:
-
nuclear factor-kB
- NSAID:
-
nonsteroidal anti-inflammatory drug
- OD:
-
octadecadienoic (linoleic) acid
- OT:
-
octadecatrienoic (linolenic) acid
- PCD:
-
programmed cell death
- nPG:
-
n-propyl gallate
- ROS:
-
reactive oxygen species
- TGF:
-
transforming growth factor
- TI:
-
toxic intermediates
- TNF:
-
tumor necrosis factor
References
Kühn H, Borngraber S . 1999 Mammalian 15-lipoxygenases. Enzymatic properties and biological implications Adv. Exp. Med. Biol. 447: 5–28
Grechkin A . 1998 Recent developments in biochemistry of the plant lipoxygenase pathway Prog. Lipid. Res. 37: 317–352
Brash AR . 1999 Lipoxygenases: occurrence, functions, catalysis, and acquisition of substrate J. Biol. Chem. 274: 23679–23682
Sudharshan E, Appu Rao AG . 1999 Involvement of cysteine residues and domain interactions in the reversible unfolding of lipoxygenase-1 J. Biol. Chem. 274: 35351–35358
Clapp CH, McKown J, Xu H, Grandizio AM, Yang G, Fayer J . 2000 The action of soybean lipoxygenase-1 on 12-iodo-cis-9-octadecenoic acid: the importance of C11-H bond breaking Biochemistry 39: 2603–2611
Provost P, Samuelsson B, Radmark O . 1999 Interaction of 5-lipoxygenase with cellular proteins Proc. Natl. Acad. Sci. USA 96: 1881–1885
Datta K, Biswal SS, Kehrer JP . 1999 The 5-lipoxygenase-activating protein (FLAP) inhibitor, MK886, induces apoptosis independently of FLAP Biochem. J. 340: 371–375
Sandstrom PA, Pardi D, Tebbey PW, Dudek RW, Terrian DM, Folks TM, Buttke TM . 1995 Lipid hydroperoxide-induced apoptosis: lack of inhibition by Bcl-2 over-expression FEBS Lett. 365: 66–70
Hébert M-J, Takano T, Holthöfer H, Brady HR . 1996 Sequential morphologic events during apoptosis of human neutrophils. Modulation by lipoxygenase-derived eicosanoids J. Immunol. 157: 3105–3115
Aoshima H, Satoh T, Sakai N, Yamada M, Enokido Y, Ikeuchi T, Hatanaka H . 1997 Generation of free radicals during lipid hydroperoxide-triggered apoptosis in PC12h cells Biochim. Biophys. Acta 1345: 35–42
Liberles SD, Schreiber SL . 2000 Apoptosis-inducing natural products found in utero during murine pregnancy Chem. Biol. 7: 365–372
O'Donnell VB, Spycher S, Azzi A . 1995 Involvement of oxidants and oxidant-generating enzyme(s) in tumour-necrosis-factor-α-mediated apoptosis: role for lipoxygenase pathway but not mitochondrial respiratory chain Biochem. J. 310: 133–141
Maccarrone M, Nieuwenhuizen WF, Dullens HFJ, Catani MV, Melino G, Veldink GA, Vliegenthart JFG, Finazzi-Agrò A . 1996 Membrane modifications in human erythroleukemia K562 cells during induction of programmed cell death by transforming growth factor β1 or cisplatin Eur. J. Biochem. 241: 297–302
Wagenknecht B, Schulz JB, Gulbins E, Weller M . 1998 Crm-A, bcl-2 and NDGA inhibit CD95L-induced apoptosis of malignant glioma cells at the level of caspase 8 processing Cell Death Differ. 5: 894–900
Maccarrone M, Catani MV, Finazzi-Agrò A, Melino G . 1997 Involvement of 5-lipoxygenase in programmed cell death of cancer cells Cell Death Differ. 4: 396–402
Croft KPC, Voisey CR, Slusarenko AJ . 1990 Mechanism of hypersensitive cell collapse: correlation of increased lipoxygenase with membrane damage in leaves of Phaseolus vulgaris (L.) cv. Red Mexican inoculated with avirulent race 1 of Pseudomonas syringae pv. phaseolicola. Physiol Mol. Plant Pathol. 36: 49–62
Levine A, Tenhaken R, Dixon R, Lamb C . 1994 H2O2 from the oxidative burst orchestrates the plant hypersensitive disease resistance response Cell 79: 583–593
Buonaurio R, Servili M . 1999 Involvement of lipoxygenase, lipoxygenase pathway volatiles, and lipid peroxidation during the hypersensitive reaction of pepper leaves to Xanthomonas campestris pv. vesicatoria Physiol. Mol. Plant Pathol. 54: 155–169
Rusterucci C, Montillet JL, Agnel JP, Battesti C, Alonso B, Knoll A, Bessoule JJ, Etienne P, Suty L, Blein JP, Triantaphylides C . 1999 Involvement of lipoxygenase-dependent production of fatty acid hydroperoxides in the development of the hypersensitive cell death induced by cryptogein on tobacco leaves J. Biol. Chem. 274: 36446–36455
Maccarrone M, Van Zadelhoff G, Veldink GA, Vliegenthart JFG, Finazzi-Agrò A . 2000 Early activation of lipoxygenase in lentil (Lens culinaris) root protoplasts by oxidative stress induces programmed cell death Eur. J. Biochem. 267: 5078–5084
Zhou YP, Teng D, Dralyuk F, Ostrega D, Roe MW, Philipson L, Polonsky KS . 1998 Apoptosis in insulin-secreting cells. Evidence for the role of intracellular Ca2+ stores and arachidonic acid metabolism J. Clin. Invest. 101: 1623–1632
Vernole P, Tedeschi B, Caporossi D, Maccarrone M, Melino G, Annicchiarico-Petruzzelli M . 1998 Induction of apoptosis by bleomycin in resting and cycling human lymphocytes Mutagenesis 13: 209–215
Maccarrone M, Fantini C, Ranalli M, Melino G, Finazzi-Agrò A . 1998 Activation of nitric oxide synthase is involved in tamoxifen-induced apoptosis of human erythroleukemia K562 cells FEBS Lett. 434: 421–424
Kamitani H, Geller M, Eling T . 1998 Expression of 15-lipoxygenase by human colorectal carcinoma Caco-2 cells during apoptosis and cell differentiation J. Biol. Chem. 273: 21569–21577
Ikawa H, Kamitani H, Calvo BF, Foley JF, Eling TE . 1999 Expression of 15-lipoxygenase-1 in human colorectal cancer Cancer Res. 59: 360–366
Kamitani H, Ikawa H, Hsi LC, Watanabe T, DuBois RN, Eling TE . 1999 Regulation of 12-lipoxygenase in rat intestinal epithelial cells during differentiation and apoptosis induced by sodium butyrate Arch. Biochem. Biophys. 368: 45–55
Matyshevskaia OP, Pastukh VN, Solodushko VA . 1999 Inhibition of lipoxygenase activity reduces radiation-induced DNA fragmentation in lymphocytes Radiat. Biol. Radioecol. 39: 282–286
Shureiqi I, Chen D, Lee JJ, Yang P, Newman RA, Brenner DE, Lotan R, Fischer SM, Lippman SM . 2000 15-LOX-1: a novel molecular target of nonsteroidal anti-inflammatory drug-induced apoptosis in colorectal cancer cells J. Natl. Cancer Inst. 92: 1136–1142
Surette ME, Fonteh AN, Bernatchez C, Chilton FH . 1999 Perturbations in the control of cellular arachidonic acid levels block cell growth and induce apoptosis in HL-60 cells Carcinogenesis 20: 757–763
Tang DG, Guan K-L, Li L, Honn KV, Chen YQ, Rice RL, Taylor JD, Porter AT . 1997 Suppression of W256 carcinosarcoma cell apoptosis by arachidonic acid and other polyunsaturated fatty acids Int. J. Cancer 72: 1078–1087
Szekeres CK, Tang K, Trikha M, Honn KV . 2000 Eicosanoid activation of extracellular signal-regulated kinase 1/2 in human epidermoid carcinoma cells J. Biol. Chem. 275: 38831–38841
Biswal SS, Datta K, Shaw SD, Feng X, Robertson JD, Kehrer JP . 2000 Glutathione oxidation and mitochondrial depolarization as mechanisms of nordihydroguaiaretic acid-induced apoptosis in lipoxygenase-deficient FL5.12 cells Toxicol. Sci. 53: 77–83
Maccarrone M, Ranalli M, Bellincampi L, Salucci ML, Sabatini S, Melino G, Finazzi-Agrò A . 2000 Activation of different lipoxygenase isozymes induces apoptosis in human erythroleukemia and neuroblastoma cells Biochem. Biophys. Res. Commun. 272: 345–350
Metzler B, Hu Y, Sturm G, Wick G, Xu Q . 1998 Induction of mitogen-activated protein kinase phosphatase-1 by arachidonic acid in vascular smooth muscle cells J. Biol. Chem. 273: 33320–33326
Buyn T, Dudeja P, Harris JE, Ou D, Seed T, Sawlani D, Meng J, Bonomi P, Anderson KM . 1997 A 5-lipoxygenase inhibitor at micromolar concentration raises intracellular calcium in U937 cells prior to their physiologic cell death Prostaglandins Leukot. Essent. Fatty Acids 56: 67–77
Aoshiba K, Yasui S, Nishimura K, Nagai A . 1999 Thiol depletion induces apoptosis in cultured lung fibroblasts Am. J. Respir. Cell. Mol. Biol. 21: 54–64
Ghosh J, Myers CE . 1998 Inhibition of arachidonate 5-lipoxygenase triggers massive apoptosis in human prostate cancer cells Proc. Natl. Acad. Sci. USA 95: 13182–13187
Tang K, Nie D, Honn KV . 1999 Role of autocrine motility factor in a 12-lipoxygenase dependent anti-apoptotic pathway Adv. Exp. Med. Biol. 469: 583–590
Vanags DM, Larsson P, Feltenmark S, Jakobsson P-J, Orrenius S, Claesson H-E, Aguilar-Santelises M . 1997 Inhibitors of arachidonic acid metabolism reduce DNA and nuclear fragmentation induced by TNF plus cycloheximide in U937 cells Cell Death Differ. 4: 479–486
Jang M, Cai L, Udeani GO, Slowing KV, Thomas CF, Beecher CWW, Fong HHS, Farnsworth NR, Kinghorn AD, Metha RG, Moon RC, Pezzuto JM . 1997 Cancer chemopreventive activity of resveratrol, a natural product derived from grapes Science 275: 218–220
Maccarrone M, Lorenzon T, Guerrieri P, Finazzi-Agrò A . 1999 Resveratrol prevents apoptosis in K562 cells by inhibiting lipoxygenase and cyclooxygenase activity Eur. J. Biochem. 265: 27–34
Gehm BD, McAndrews JM, Chien PY, Jameson JL . 1997 Resveratrol, a polyphenolic compound found in grapes and wine, is an agonist for the estrogen receptor Proc. Natl. Acad. Sci. USA 94: 14138–14143
Sud'ina GF, Mirzoeva OK, Pushkareva MA, Korshunova GA, Sumbatyan NV, Varfolomeev SD . 1993 Caffeic acid phenethyl ester as a lipoxygenase inhibitor with antioxidant properties FEBS Lett. 329: 21–24
Maccarrone M, Taccone-Gallucci M, Meloni C, Cococcetta N, Manca di Villahermosa S, Casciani U, Finazzi-Agrò A . 1999 Activation of 5-lipoxygenase and related cell membrane lipoperoxidation in hemodialysis patients J. Am. Soc. Nephrol. 10: 1991–1996
Schnurr K, Belkner J, Ursini F, Schewe T, Kuhn H . 1996 The selenoenzyme phospholipid hydroperoxide glutathione peroxidase controls the activity of the 15-lipoxygenase with complex substrates and preserves the specificity of the oxygenation products J. Biol. Chem. 271: 4653–4658
Fadok VA, Xue D, Henson P . 2001 If phosphatidylserine is the death knell, a new phosphatidylserine-specific receptor is the bellringer Cell Death Differ. 8: 582–587
Van Leyen K, Duvoisin RM, Engelhardt H, Wiedmann M . 1998 A function for lipoxygenase in programmed organelle degradation Nature 395: 392–395
Vieira HLA, Haouzi D, El Hamel EI, Jacotot E, Belzacq A-S, Brenner C, Kroemer G . 2000 Permeabilization of the mitochondrial inner membrane during apoptosis: impact of the adenine nucleotide translocator Cell Death Differ. 7: 1146–1154
Bernardi P, Petronilli V, Di Lisa F, Forte M . 2001 A mitochondrial perspective on cell death Trends Biochem. Sci. 26: 112–117
Maccarrone M, Lorenzon T, Bari M, Melino G, Finazzi-Agrò A . 2000 Anandamide induces apoptosis in human cells via vanilloid receptors. Evidence for a protective role of cannabinoid receptors J. Biol. Chem. 275: 31938–31945
Von Ahsen O, Waterhouse NJ, Kuwana T, Newmeyer DD, Green DR . 2000 The ‘harmless’ release of cytochrome c Cell Death Differ. 7: 1192–1199
Roucou X, Martinou J-C . 2001 Conformational change of Bax: a question of life or death Cell Death Differ. 8: in press
Maccarrone M, Salucci ML, Melino G, Rosato N, Finazzi-Agrò A . 1999 The early phase of apoptosis in human neuroblastoma CHP100 cells is characterized by lipoxygenase-dependent ultraweak light emission Biochem. Biophys. Res. Commun. 265: 758–762
Morel J-B, Dangl JL . 1997 The hypersensitive response and the induction of cell death in plants Cell Death Differ. 4: 671–683
Hilbers MP, Finazzi-Agrò A, Veldink GA, Vliegenthart JFG . 1996 Purification and characterization of a lentil seedling lipoxygenase expressed in E. coli Int. J. Biochem. Cell Biol. 28: 751–760
Acknowledgements
We thank Dr. Mattia Falconi for the molecular model of LOX-1 and Mr. Graziano Bonelli for the excellent production of the artwork. All colleagues at University of Rome Tor Vergata and at Utrecht University who took part over the years in the study of the role of lipoxygenases in programmed cell death are gratefully acknowledged as well. This work was supported by Istituto Superiore di Sanità, Rome, through a III Aids Project grant (to A Finazzi-Agrò), and by EU grant QL661-1999-00739, Telethon E872, AIRC and MURST-Cofin (to G Melino).
Author information
Authors and Affiliations
Corresponding author
Additional information
Edited by H Ichijo
Rights and permissions
About this article
Cite this article
Maccarrone, M., Melino, G. & Finazzi-Agro, A. Lipoxygenases and their involvement in programmed cell death. Cell Death Differ 8, 776–784 (2001). https://doi.org/10.1038/sj.cdd.4400908
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cdd.4400908
Keywords
This article is cited by
-
Function and molecular mechanism analysis of CaLasSDE460 effector involved in the pathogenesis of “Candidatus Liberibacter asiaticus” in citrus
Molecular Horticulture (2023)
-
GABA and Potassium Modulates Defence Systems, Assimilation of Nitrogen and Carbon, and Yield Traits Under Salt Stress in Wheat
Journal of Plant Growth Regulation (2023)
-
Dynamic formation and transcriptional regulation mediated by phytohormones during chalkiness formation in rice
BMC Plant Biology (2021)
-
Investigating the effects of two novel 4-MMPB analogs as potent lipoxygenase inhibitors for prostate cancer treatment
Journal of Biological Research-Thessaloniki (2021)
-
Molecular regulation of potato tuber dormancy and sprouting: a mini-review
Plant Biotechnology Reports (2021)