Abstract
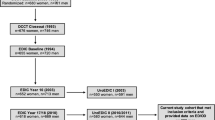
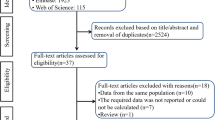
Although erectile dysfunction (ED) has been considered a complication of other medical conditions, clinicians and researchers suggest that ED may serve as a clinical marker of vascular health. This retrospective claims study examined the prevalence of predefined comorbid conditions in men with ED (N=301 994) in the 12 months before and the 6 months following ED diagnosis. Consistent with previous research, comorbid conditions were prevalent among men with ED. Comorbid conditions were most often diagnosed before an ED diagnosis, although new diagnoses in the 6 months following an ED diagnosis were common and occured more frequently than new diagnoses in a matched sample of men without ED during the same period. Differences by age, region and insurance coverage for ED medications were also examined. Findings support previous research that suggests ED may serve as a marker for previously undetected comorbid conditions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
NIH Consensus Development Panel on Impotence. Impotence. JAMA 1993; 270: 83–90.
Rosen RC, Fisher WA, Eardley I, Niederberger C, Nadel A, Sand M . The multinational Men's Attitudes to Life Events and Sexuality (MALES) study: prevalence of erectile dysfunction and related health concerns in the general population. Curr Med Res Opin 2004; 20: 607–617.
Feldman HA, Goldstein I, Hatzichristou DG, Krane RJ, McKinlay JB . Impotence and its medical and psychosocial correlates: results of the Massachusetts Male Aging Study. J Urol 1994; 151: 54–61.
Fung MM, Bettencourt R, Barrett-Connor E . Heart disease risk factors predict erectile dysfunction 25 years later. J Am Coll Cardiol 2004; 43: 1405–1411.
Seftel AD, Sun P, Swindle R . The prevalence of hypertension, hyperlipidemia, diabetes mellitus and depression in men with erectile dysfunction. J Urol 2004; 171: 2341–2345.
Sun P, Swindle R . Are men with erectile dysfunction more likfely to have hypertension than men without erectile dysfunction? A naturalistic national cohort study. J Urol 2005; 174: 244–248.
Baum N . Erectile dysfunction and cardiovascular disease. Clin Geriatr 2004; 12: 21–24.
Blumenthals WA, Gomez-Caminero A, Joo S, Vannappagari V . Should erectile dysfunction be considered a marker for acute myocardial infarction? Results from a retrospective cohort study. Int J Impot Res 2004; 16: 350–353.
Levine LA, Kloner RA . Importance of asking questions about erectile dysfunction. Am J Cardiol 2000; 86: 1210–1213.
Billups KL, Bank AJ, Padma-Nathan H, Katz S, Williams R . Erectile dysfunction is a marker for cardiovascular disease: results of the minority health institute expert advisory panel. J Sex Med 2005; 2: 40–52.
Ganz P . Erectile dysfunction: pathophysiologic mechanisms pointing to underlying cardiovascular disease. Am J Cardiol 2005 (in press).
Fisher WA, Rosen RC, Eardley I, Niederberger C, Nadel A, Kaufman J et al. The Multinational Men's Attitudes to Life Events and Sexuality (MALES) Study Phase II: understanding PDE5 inhibitor treatment seeking patterns, among men with erectile dysfunction. J Sex Med 2004; 1: 150–160.
Druss BG, Marcus SC, Olfson M, Tanielian T, Elinson L, Pincus HA . Comparing the national economic burden of five chronic conditions. Health Aff 2005; 20: 233–241.
Kearney PM, Whelton M, Reynolds K, Muntner P, Whelton PK, He J . Global burden of hypertension: analysis of worldwide data. Lancet 2005; 365: 217–223.
Hodgson TA, Liming C . Medical care expenditures for hypertension, its complications, and its comorbidities. Med Care 2001; 39: 599–615.
Sadovsky R, Mulhall JP . The potential value of erectile dysfunction inquiry and management. Int J Clin Pract 2003; 57: 601–608.
Sadovsky R . Integrating erectile dysfunction treatment into primary care practice. Am J Med 2000; 109: 22S–28S.
Frankel SJ, Donovan JL, Peters TI, Abrams P, Dabhoiwala NF, Osawa D et al. Sexual dysfunction in men with lower urinary tract symptoms. J Clin Epidemiol 1998; 51: 677–685.
Rosen RC, Altwein J, Boyle P, Kirby RS, Lukacs B, Meuleman E et al. Lower urinary tract symptoms and male sexual dysfunction: The Multinational Survey of the Aging Male (MSAM-7). Eur Urol 2003; 44: 637–649.
Braun MH, Sommer F, Haupt G, Mathers MJ, Reifenrath B, Engelmann UH . Lower urinary tract symptoms and erectile dysfunction: co-morbidity of typical ‘aging male’ symptoms? Results of the ‘Cologne Male Survey. Eur Urol 2003; 44: 588–594.
Kubin M, Wagner G, Fugl-Meyer AR . Epidemiology of erectile dysfunction. Int J Impot Res 2003; 15: 63–71.
Shabsigh R, Perelman MA, Laumann EO, Lockhart DC . Drivers and barriers to seeking treatment for erectile dysfunction: a comparison of six countries. BJU Int 2004; 94: 1055–1065.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cameron, A., Sun, P. & Lage, M. Comorbid conditions in men with ED before and after ED diagnosis: a retrospective database study. Int J Impot Res 18, 375–381 (2006). https://doi.org/10.1038/sj.ijir.3901439
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijir.3901439
Keywords
This article is cited by
-
Can written information material help to increase treatment motivation in patients with erectile dysfunction? A survey of 1188 men
International Journal of Impotence Research (2007)
-
Psychological features in men with erectile dysfunction with or without preclinical atherosclerosis
International Journal of Impotence Research (2007)