Abstract
The products of the blood clotting reaction, eg, thrombin and fibrinopeptides, have various proinflammatory activities and are suggested to modulate inflammation. The macrophage expression of tissue factor (TF), the clotting initiator, has been shown to cause clotting in the site of the delayed-type hypersensitivity reaction, a cellular immune response. However, the mechanism of the clotting induction in humoral immune response has been insufficiently studied. Therefore, the Arthus reaction, a model of immune-complex diseases, was produced in monkey skin that was examined for TF expression and fibrin deposition. TF antigen was positive on most of polymorphonuclear leukocytes, which were the main leukocytes in the lesions and were identified as neutrophils with an anti-neutrophil-elastase mAb. TF mRNA was detected in neutrophils by in situ hybridization using TF RNA probes, indicating de novo TF synthesis by the leukocytes. Specific binding of activated factor VII onto TF-positive neutrophils suggested the activity of neutrophil TF to trigger the cascade reaction of clotting. The number of TF-positive neutrophils were correlated in time with the intensity and extent of fibrin deposition that was visualized with an mAb specific for fibrin and peaked in 24 hours. Interestingly, the fibrin deposit was partially positive for an mAb specific for neutrophil elastase-digested fibrin. These results show in vivo evidence of a close relationship between neutrophils and both clotting and fibrinolysis in the Arthus reaction and may suggest that these neutrophil functions contribute to the pathogenesis of this hypersensitivity inflammation.
Similar content being viewed by others
Introduction
Accumulated evidence indicates that clotting is a defensive host response and combines with inflammation against infection and tissue injury (Cicala and Cirino, 1998). Induction of tissue factor (TF) expression on monocytes/macrophages and endothelial cells by various inflammatory stimuli including cytokines is a representative example of the linkage between clotting and inflammation (Grignani and Maiolo, 2000). TF triggers the cascade reaction of clotting factors by forming a complex with clotting factor VII/VIIa (Nemerson, 1988), ultimately yielding thrombin, which converts fibrinogen to fibrin (Mann and Lundblad, 1987). TF actions in blood vessel development (Carmeliet et al, 1996), signal transduction (Masuda et al, 1996), and cell-to-cell contact (Müller et al, 1999) are crucial for repairing injured tissues, thus TF is a multifunctional factor. Besides its central role in clotting, thrombin enhances vascular permeability (DeMichele et al, 1990) and induces endothelial cell adhesion molecule expression (Hattori et al, 1989), leukocyte chemotaxis (Bar-Shavit et al, 1983; Bizios et al, 1986), macrophage IL-1 production (Jones and Geczy, 1990), and T-cell proliferation (Naldini et al, 1993). Fibrin(ogen) degradation products (FDPs) modulate lymphocyte mitogenesis (Janus et al, 1986; Robson et al, 1993), and fibrin is associated with wound healing (Clark, 2001), interaction with VE-cadherin (Martinez et al, 2001), and neutrophil migration (Loike et al, 1999). These data suggest a close interrelationship between the clotting system and inflammation including immune-mediated inflammatory responses. In fact, fibrin deposition is a common feature at the site of delayed-type hypersensitivity (DTH) (Colvin et al, 1973), an antigen-specific, cell-mediated immune response classified as a type IV hypersensitivity reaction. We showed previously that infiltrated macrophages induced clotting by expressing TF on the cell membrane, leading to formation of induration (Imamura et al, 1993), a skin lesion characteristic of DTH reaction and associated with fibrin deposition (Colvin and Dvorak, 1975). With regard to inflammation by nonspecific stimuli, we found TF expression on accumulated neutrophils and fibrin clot in liver sinusoid of rabbits and monkeys that had received intravenous injection of bacterial lipopolysaccharides (LPS) (Higure et al, 1996; Todoroki et al, 1998, 2000), suggesting participation of neutrophils in the clotting in inflammation. However, neutrophils are thought to play a pivotal role in nonimmune biodefense, and in this context, the leukocytes may not express TF in inflammation by antigen-specific immune responses. Whether neutrophils express TF in the site of hypersensitivity inflammation remains to be elucidated.
The Arthus reaction (AR) is a type III hypersensitivity reaction induced by immune complexes and is involved in the pathogenesis of autoimmune diseases such as systemic lupus erythematosus, rheumatoid arthritis, and glomerulonephritis (Ranadive and Movat, 1979). Strong neutrophil accumulation is a characteristic of the AR site (Opie, 1924), in contrast to the DTH reaction site, where macrophages are the major component of accumulated leukocytes (Turk et al, 1966). Little is known to date about activation of the clotting system or fibrin formation in the AR. To study clotting in the AR, we investigated expression of TF and fibrin deposition consequent upon clotting activation in the site of the reaction induced in monkey skin.
Results
Expression of TF Antigen on Neutrophils
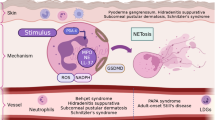
To study activation of the clotting system in the AR site, we examined lesions for the presence of TF by immunohistochemical staining using a TF-specific mAb. We found that most of the accumulated leukocytes were TF positive. In the 6-hour skin lesion of the AR, the main TF antigen-positive cells were polymorphonuclear leukocytes, whereas minor TF-positive mononuclear cells were seen (Fig. 1A). TF appeared to be present on the cell membrane rather than in cytoplasm of both leukocytes (Fig. 1A, inset and the cell indicated by an arrow). Epidermis and trichoepithelium were also TF positive in AR sites (data not shown) similar to normal skin tissue, which is consistent with our previous result (Imamura et al, 1993). In the 24-hour skin lesion, TF-positive polymorphonuclear cells increased in correlation with the increase of accumulated leukocytes, and TF-positive mononuclear cells also increased (Fig. 1B).
Immunohistochemical staining of Arthus reaction (AR) skin tissues using antibodies against either tissue factor (TF) or elastase. A, TF staining of 6-hour AR skin. The arrow shows a typical TF antigen-positive macrophage. Original magnification, × 220. Inset, the area in the smaller square was magnified. Original magnification, × 800. B, TF staining of 24-hour AR skin. Original magnification, × 220. C, Elastase staining of 6-hour AR skin. Original magnification, × 400. D, Control staining of 6-hour AR skin using nonspecific mouse IgG. Original magnification, × 165.
To identify TF-positive polymorphonuclear leukocytes as neutrophils, we stained neutrophil elastase, a lysosomal protease specific for neutrophils. Elastase was positive in most of the accumulated polymorphonuclear leukocytes (Fig. 1C) but negative in mononuclear cells. No cell was stained by nonspecific mouse IgG (Fig. 1D). Since, as shown with human neutrophils (Drake et al, 1989), neutrophils isolated from the monkey peripheral blood did not express TF (not shown), these results indicate that neutrophils infiltrated into the site of AR express TF in situ. Consistent with the previous report (Opie, 1924), neutrophils are the major component of accumulated leukocytes in the present AR site (Fig. 2). TF antigen-positive neutrophils increased from 3 hours to 24 hours of AR and decreased markedly in 48 hours, which was proportional to the amount of accumulated neutrophils (Fig. 2). TF antigen-positive mononuclear cells also increased until 24 hours and decreased slightly at 48 hours (Fig. 2). TF antigen-positive mononuclear cells were larger than small lymphocytes that were TF antigen negative, and the larger mononuclear cells were stained with anti-macrophage mAb (KP1) (not shown), indicating that TF antigen-positive mononuclear cells were macrophages. The percentage of TF antigen-positive cells ranged from about 70% to 90% of each cell type throughout the reaction (Fig. 2).
Time course of the amount of TF-positive neutrophils and TF-positive macrophages and the intensity of fibrin deposition in AR skin sites. Neutrophils (○, TF-positive neutrophils (•), and TF-positive mononuclear cells (▴) were counted in the sections stained immunohistochemically with anti-TF mAb (K108). Macrophages (▵) were counted in the sections stained with an anti-macrophage mAb. Cells were counted in five high-power fields (× 400) at random using a microscope, and the total number of cells are shown. Values were expressed as means ± sd (n = 3). Fibrin deposition in the sections stained immunohistochemically with an anti-fibrin mAb was scored according to the method of Colvin et al (1973).
TF mRNA in Neutrophils
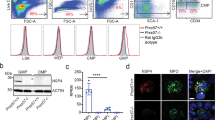
To determine whether neutrophils produce TF through a genetic event of TF mRNA, we performed in situ hybridization for the sections of the dermal AR using sense or antisense TF RNA probes. The antisense TF RNA probe reacted with polymorphonuclear leukocytes (Fig. 3A), whereas no positive cells were seen in the section incubated with the sense TF RNA probe (Fig. 3B). The results indicated that TF was synthesized de novo in neutrophils.
Detection of TF mRNA in neutrophils accumulated in AR skin sites. In situ hybridization of 6-hour AR skin was performed using TF mRNA sense or antisense probes. TF mRNA was shown by FITC-fluorescence, and nuclei were stained with propidium iodide. A, antisense probe (Original magnification, × 980). B, sense probe (Original magnification, × 580).
Activated Factor VII (VIIa) Binding to Neutrophils
To study the clotting initiation activity of TF on neutrophils, the binding of VIIa to neutrophils expressing TF was examined. It was found that labeled VIIa bound to neutrophils (Fig. 4A). Because the treatment of these cells with excess amount of nonlabeled VIIa resulted in pronounced reduction of labeled VIIa binding (Fig. 4B), VIIa is likely to bind specifically to neutrophils in the lesion. These results indicate that TF expressed on neutrophils at the AR site forms a complex with VIIa and suggested that the complex can induce clotting.
Histochemistry for FPR-ck-VIIa binding. The 6-hour AR skin sections were reacted with biotinylated FPR-ck-VIIa after preincubating with or without unlabeled VIIa. A, Preincubated without unlabeled VIIa (Original magnification, × 410). Arrows show typical neutrophils FPR-ck-VIIa bound. B, Preincubated with unlabeled VIIa (Original magnification, × 220).
Fibrin Deposition
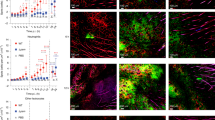
To determine whether plasma clotting occurred in the AR site, we examined the lesions of various reaction periods for fibrin deposition by immunohistochemical staining using a fibrin-specific mAb. In the 3-hour lesion, a coarse mesh-like fibrin deposition was seen in skin interstitial tissues, surrounding the accumulated leukocytes (Fig. 5A). In the 6-hour lesion, the fibrin deposition expanded and the mesh structure of fibrin became fine (Fig. 5B). In the 24-hour lesion, the extent and density of the fibrin deposition was at the maximum level (Fig. 5C), and in the 48-hour lesion the density of the fibrin deposition was reduced and the fibrin mesh became coarse (Fig. 5D). No stain was seen in lesions when nonspecific mouse IgG was used (not shown). These results indicated that the clotting pathway was activated in this hypersensitivity reaction site.
To study whether neutrophil TF expression is associated with fibrin deposition, we scored the degree of fibrin deposition in reaction sites at various AR periods and compared the time courses of the fibrin deposition and the TF-positive neutrophil accumulation. The degree of fibrin deposition correlated with the amount of TF-positive neutrophils but not with that of TF-positive macrophages (Fig. 2). These results suggest a close relationship between TF expressed on neutrophils and the fibrin formation at the site of AR.
A pronounced decrease of fibrin deposition in the 48-hour lesion (Figs. 2 and 5D) despite the presence of TF-positive leukocytes indicated that fibrinolysis coincided in the AR site. Activated neutrophils release elastase, and this lysosomal proteinase has fibrinolytic activity (Plow, 1980). To determine whether the deposited fibrin was elastase digested, the lesion was examined immunohistochemically using an mAb (IF123) specific for neutrophil elastase-digested fibrin(ogen) product (Kohno et al, 2000). The AR lesions were stained by IF123 with a mesh-like structure (Fig. 5, E and F). The anti-fibrin mAb recognizes the amino-terminus of fibrin β-chain (Hui et al, 1983), and the mAb IF-123 reacts neither with fibrinogen nor fibrin products digested by plasmin or cathepsin G (Kohno et al, 2000). It is likely that fibrinolysis by neutrophil-released elastase occurred in the AR site. The stain with IF-123 was similar in time course but was less than the stain with the fibrin-specific mAb in extent and intensity (Fig. 5, E and F), which suggested that some part of the deposited fibrin was elastase digested.
Discussion
The extravascular fibrin formation in the AR site induced in monkey skin (Fig. 5, A to D) revealed that the activation of the clotting cascade occurred in the humoral immunity-mediated inflammation. No fibrin formation was seen in the skin where plasma was leaked by histamine injection (Imamura et al, 1993), indicating that plasma leaked into extravascular skin tissues does not spontaneously clot. It is obvious that a procoagulant factor present in the AR site induced the clotting. In this study, neutrophils were found to express TF (Fig. 1, A and B) as a possible procoagulant factor responsible for the clotting induction. This is a new function of neutrophils in the hypersensitivity inflammation.
In neutrophils infiltrated into the AR site, the TF gene was activated to express its mRNA (Fig. 3), followed by the synthesis of its genetic product and expression onto the cell surface (Fig. 1, A and B). The chronologic correlation between the amount of accumulated TF-expressing neutrophils, not macrophages, and the intensity and extent of fibrin deposition (Fig. 2) showed an association of neutrophil TF with the fibrin, the consequent product. Notably, clotting factors including factor Xa, thrombin, and fibrinogen bind to neutrophils (Gillis et al, 1997), thus assembly of these clotting factors presumably facilitates the cascade reaction of clotting on the neutrophil surface. Furthermore, neutrophils are easily induced apoptosis by various stimuli, including neutrophil elastase (Trevani et al, 1996) and reactive oxygen species (Rollet-Labelle et al, 1998), and apoptotic cells expose phosphatidylserine to the external surface (Martin et al, 1995). This phospholipid, an important cofactor in the clotting pathway, would accelerate the cascade reactions of clotting factors (Dachary-Prigent et al, 1996). In addition, it has been reported that TF activity on endothelial cells and fibroblasts is increased by TF de-encryption, which occurs during apoptosis (Greeno et al, 1996). By putting these together, it is likely that neutrophil TF expression is relevant in terms of the clotting induction in inflammation.
The presence of TF on neutrophils in the AR site (Fig. 1, A and B) is in vivo evidence that neutrophils express TF in inflammation by immune stimuli as in the case of inflammation by nonspecific stimuli (Higure et al, 1996; Todoroki et al, 1998, 2000). Giesen et al (1999) have found TF-bearing neutrophils in ex vivo study using pig arterial media and collagen-coated glass slides exposed to flowing native human blood, while de novo TF production in the neutrophils was not shown. However, Østerud et al (2000) reported that neutrophils did not express TF in vitro by stimulation with LPS or PMA. Because the in vitro mechanism and optimum conditions for neutrophil TF expression have been unknown and are complicated, unlike those of monocytes, it has not been possible to reproduce neutrophil TF expression in vitro. This is the major reason why neutrophil TF expression is a subject of controversy. Because preinjection of an anti-platelet activating factor drug to rabbits before LPS injection resulted in a pronounced suppression of neutrophil TF expression (Todoroki et al, 1998), platelet activating factor is a requisite factor for neutrophil TF expression in this model. Expression of intercellular adhesion molecule-1 (ICAM-1) increased in the liver endothelial cells of LPS-injected monkeys (Todoroki et al, 2000), thus a neutrophil-endothelial cell interaction via ICAM-1 may be necessary in neutrophil TF expression. No neutrophil TF expression was, however, observed in vitro when isolated neutrophils or whole blood cells were cocultured with endothelial cells, which expressed ICAM-1 by stimuli with LPS and/or TNF-α (not shown). It is evident that unknown condition(s) or factor(s) are critical to induce TF expression on neutrophils in vitro.
Although fibrin deposition was present in the AR site, induration is not clear. A possible reason is that TF expressed on neutrophils in the AR site may be less than that on macrophages in the DTH site, resulting in less fibrin deposition in this type III hypersensitivity reaction site. In fact, in guinea pigs, thrombin-like activity in the extracts of AR skin lesions is much lower than that in the extracts of the DTH reaction skin lesions (Imamura and Kambara, 1992). Macrophages, the major leukocyte in the DTH lesion, release plasminogen activator together with TF expression (Chapman et al, 1983); however, they also produce plasminogen activator inhibitors (Ritchie et al, 1995), disturbing plasmin production by macrophage plasminogen activator. Consequently, fibrinolysis by plasmin would be delayed in the DTH reaction site. Indeed, plasmin-like activity in extracts of the guinea pig DTH skin sites increased slowly in comparison to that in the AR sites (Imamura and Kambara, 1992). Thus, intact fibrin may be maintained longer in the DTH site. In contrast, plasmin-like activity in the AR site increased rapidly to the maximum level of activity in the DTH reaction site (Imamura and Kambara, 1992). Neutrophil elastase inactivation of plasminogen activator inhibitor type 1 (Wu et al, 1995) would augment fibrin degradation by plasmin in the AR site. Furthermore, the presence of elastase-digested fibrin (Fig. 5, E and F), shown by immunohistochemical staining for the first time with the availability of IF123 to detect elastase-digested fibrin in vivo, demonstrated a significant contribution of neutrophil elastase to fibrinolysis in the lesion. Oxygen radical species released from neutrophils inactivate α1-proteinase inhibitor (Clark et al, 1981), a potent inhibitor of neutrophil elastase, thus the fibrinolytic activity by neutrophil elastase will be augmented in the Arthus lesions, where a plenty of neutrophils accumulate (Fig. 1C). Because FDPs modulate lymphocyte mitogenesis (Janus et al, 1986; Robson et al, 1993), FDPs by elastase digestion are speculated to regulate immune responses. Elastase digestion of deposited fibrin is a characteristic of the AR site, and consequent FDP may be associated with the development of this hypersensitivity reaction by modulating immune responses.
Taking together the cases of AR and LPS-induced inflammation (Higure et al, 1996; Todoroki et al, 1998, 2000), TF expression and presumably elastase fibrinolysis are likely to be general functions of neutrophils in inflammation and may be associated with inflammation-induced hypercoagulability and subsequent bleed-ing tendency, such as disseminated intravascular coagulation.
Materials and Methods
Materials
BSA, tRNA, RNase, dextran sulfate, and propidium iodide were purchased from Sigma (St. Louis, Missouri). XhoI, T7, and T3 RNA polymerase, BamHI, Biotin RNA Labeling Mix, and DIG RNA labeling kit were purchased from Boehringer Mannheim Biochemicals (Indianapolis, Indiana). FITC-conjugated streptavidin was purchased from Protos Immunoresearch (Burlingame, California). Human factor VIIa, biotin-labeled-Phe-Pro-Arg-chloro-methyl-ketone (biotin-X-FPR-ck), and streptavidin-alkaline phosphatase were purchased from Enzyme Research Laboratories (South Bend, Indiana), Hematologic Technologies Inc. (Essex Junction, Vermont), and Oncogene Research Products (Cambridge, Massachusetts), respectively. The alkaline phosphatase anti-alkaline phosphatase (APAAP) kit was purchased from DAKO Corporation (Carpenteria, California). Other chemicals were purchased from Nacalai Tesque (Kyoto, Japan).
mAbs
Anti-TF murine mAb (K108) (Imamura et al, 1993) recognizes the human TF N-terminal region, TF1-83, and reacts to monkey TF. A murine mAb that reacts only to fibrin but not to fibrinogen (Hui et al, 1983) was obtained from Immunotech S.A. (Marseille, France). Murine mAbs against human neutrophil elastase (Pulford et al, 1988) and human macrophage (KP1) (Pulford et al, 1989) were purchased from DAKO Corporation (Carpenteria, California). The murine monoclonal antibody (IF-123) that reacts only to elastase-digested fibrin(ogen) (Kohno et al, 2000) was kindly donated by Mr. I. Kohno (Iatron Laboratories Inc., Chiba, Japan). For immunohistochemical studies, these antibodies were used at a concentration of 2 μg/ml. Nonspecific IgG was isolated from mouse serum using a HiTrap Protein G column (Pharmacia Biotech, Uppsala, Sweden) according to the manufacturer's instructions.
Induction of AR
Monkeys (Macaca radiata) were sensitized with subcutaneous injections of 10 mg of BSA (20 mg/ml 0.9% saline) emulsified with an equal volume of an adjuvant (TiterMax GOLD; CytRx Corporation, Norcross, Georgia), followed by reinjections of the emulsified BSA 3 weeks later. After 2 weeks, AR was induced by intradermal injections of 0.1 ml of BSA (10 mg/ml 0.9% saline) into shaved skin of the monkeys. Sensitized monkey sera of at least 8-fold dilution made a precipitin line against BSA (0.2 mg/ml) in an Ouchterlony plate.
Tissue Procurement and Preparation
Monkeys were killed under deep anesthesia using Ketaral and Nembutal, a technique which was adopted from the “Guide for the Care and Use of Laboratory Primates” at the primate Research Institute, Kyoto University. Tissue was obtained from the skin lesions after various time periods of AR; 5 × 5-mm blocks were immediately embedded in optimal cutting temperature compound in 15 × 15-mm cryomolds and rapidly frozen in liquid nitrogen and stored at −80° C until use.
Immunohistochemistry
Immunohistochemistry was performed on freshly prepared cryostat sections (4-μm thickness) attached to silane-coated slides. Sections were fixed in acetone at 4° C for 10 minutes and air-dried for 5 minutes at room temperature. After further fixing in 4% paraformaldehyde (pH 7.0) at 4° C for 10 minutes, the sections were washed in 10 mm Tris-HCl, pH 7.4, containing 150 mm NaCl (TBS) for 5 minutes (TBS wash), followed by an incubation in 3% rabbit serum to eliminate nonspecific binding of antibodies. After incubation with an mAb (2 μg/ml TBS) at 4° C overnight, sections were reacted with anti-mouse IgG-rabbit IgG (APAAP kit) for 30 minutes at room temperature and then with an alkaline phosphatase-anti-alkaline phosphatase mouse mAb complex (APAAP kit) for 30 minutes at room temperature. Each step was followed by three TBS washes. Bound alkaline phosphatase was detected using Fast Red TR salt (APAAP kit) incubated at room temperature for 10 minutes. The sections were then washed in distilled water, lightly counterstained with Mayer's hematoxylin, and mounted in Aquatex (Merck, Darmstadt, Germany). As a control, normal mouse IgG was used instead of an mAb.
In Situ Hybridization
RNA probes for TF were prepared from 532 bp (180-712) human TF cDNA ligated into XhoI/BamHI sites of pBluescript KS(+). The antisense and sense RNA probes were synthesized with T7 RNA polymerase after linearization of the plasmid with XhoI and with T3 RNA polymerase after BamHI digestion, respectively. Both probes (1 μg) were transcripted with a DIG RNA Labeling kit (SP6/T) as recommended by the manufacturer using Biotin RNA Labeling Mix instead of NTP Labeling Mixture. After digestion with DNaseI to remove DNA templates, the specificity of the transcripted antisense and sense RNA probes was confirmed by dot hybridization with sense or TF cDNA probe, respectively.
Frozen sections (4-μm thick) were fixed in 4% paraformaldehyde in 10 mm phosphate buffer, pH 7.3, for 15 minutes. The sections were incubated with 5 μg/ml proteinase K in 10 mm Tris-HCl, pH 8.0, at 37° C for 10 minutes and refixed in 4% paraformaldehyde in 10 mm phosphate buffer, pH 7.3, for 10 minutes. After rinsing in 10 mm phosphate buffer, pH 7.3, containing 150 mm NaCl (PBS), the sections were incubated in 0.2 m HCl and again rinsed in PBS, then acetylated with 0.25% acetic anhydride in 0.1 m triethanolamine for 10 minutes. After another rinse in PBS, the sections were dehydrated in a graded series of ethanol. The sections were hybridized with 20 ng/μl biotin-labeled antisense or sense human TF RNA probe in 10 mm Tris-HCl, pH 8.0 (containing 50% deionized formamide, 200 μg/ml tRNA, 1 × Denhardt's solution, 10% dextran sulfate, 0.6 m NaCl, 0.25% SDS, and 1 mm EDTA), for 16 hours at 50° C. Thereafter, the sections were washed subsequently in 2 × SSC containing 50% formamide at 50° C for 30 minutes; in 10 mm Tris-HCl, pH 7.6, containing 0.5 M NaCl, 1 mm EDTA, and 10 μg/ml RNase A at 37° C for 20 minutes; in 2 × SSC at 50° C for 20 minutes; and in 0.2 × SSC at 50° C for 20 minutes. After an incubation in 0.1 mm maleic acid supplemented with 1% skim milk, the sections were incubated with FITC-conjugated streptavidin (0.5 μg/ml) to detect bound TF RNA probes, and with propidium iodide (0.5 μg/ml) to counterstain, for 30 minutes. Fluorescence was detected with Olympus confocal laser scanning microscopy CLSM using Fluo View application software (Olympus, Tokyo, Japan).
FPR-ck-VIIa Histochemistry
To detect functional TF on cells, histochemistry was performed using biotin-labeled FPR-ck-treated VIIa according to the method described previously (Contrino et al, 1994). Briefly, 250 μg of human factor VIIa (5.0 μm) was incubated with biotin-X-FPR-ck (200 μm) in 20 mm HEPES buffer, pH 7.4, containing 0.15 M NaCl at room temperature for 2 hours. Biotin-X-FPR-ck was further added to the mixture to a final concentration of 400 μm and incubated overnight at room temperature. The solution was dialyzed against the aforementioned buffer and stored at −80° C in 50% glycerol (v/v). Successful labeling was determined by examining the appropriate staining (avidin-alkaline phosphatase) of SDS-PAGE electroblots. The frozen sections (5-μm thick) were fixed in acetone at 4° C for 10 minutes and air-dried for 5 minutes at room temperature. After further fixing in 4% paraformaldehyde (pH 7.0) at 4° C for 10 minutes, the sections were washed in TBS for 5 minutes, followed by an incubation in 5% BSA in TBS for 1 hour at room temperature. Sections for specificity control were preincubated with unlabeled VIIa (50 × molar excess) for 1 hour at room temperature. FPR-ck-VIIa (1/100 dilution in TBS/0.5% BSA) was applied to the sections and incubated overnight in moist chambers at 4° C. The sections were incubated with streptavidin-alkaline phosphatase (1/1000 dilution in TBS) for 1 hour. Bound alkaline phosphatase was detected using Fast Red TR salt (0.04% in 0.05 m Tris-HCl buffer, pH 9.0, 0.03% naphthol AS-MX phosphate, 1 mm MgCl2, and 2.7 mm levamisole) incubated in a dark room for 10 minutes at 37° C. The sections were counterstained with Mayer's hematoxylin and mounted in Aquatex.
Histologic Examinations
TF-positive polymorphonuclear leukocytes or mononuclear cells were distinguished morphologically and quantified by counting cells stained with anti-TF mAb (K108). Macrophages were quantified by counting cells stained with anti-macrophage mAb (KP1). In each section, cells were counted in five microscopic high-power fields (magnification × 400), according to the method of Kay (1970). The extent and overall intensity of fibrin stain was graded 0 to 4+, according to the method of Colvin et al (1973).
References
Bar-Shavit R, Kahn A, Fenton LW II, and Wilner GD (1983). Monocyte chemotaxis: Stimulation by specific exosite region in thrombin. Science 220: 728–730.
Bizios R, Lai L, Fenton JW II, and Malik AB (1986). Thrombin-induced chemotaxis and aggregation of neutrophils. J Cell Physiol 128: 485–490.
Carmeliet P, Mackman N, Moons L, Luther T, Gressens P, Van Vlaenderen I, Demunck H, Kasper M, Breier G, Evrard P, Müller M, Risau W, Edgington T, and Collen D (1996). Role of tissue factor in embryonic blood vessel development. Nature 383: 73–75.
Chapman HA, Vavrin Z, and Hibbs JB (1983). Coordinate expression of macrophage procoagulant and fibrinolytic activity in vitro and in vivo. J Immunol 130: 261–266.
Cicala C and Cirino G (1998). Linkage between inflammation and coagulation: An update on the molecular basis of the crosstalk. Life Sci 62: 1817–1824.
Clark RA (2001). Fibrin and wound healing. Ann NY Acad Sci 936: 355–367.
Clark RA, Stone PJ, El Hag A, Calore JD, and Franzblau C (1981). Myeloperoxidase-catalyzed inactivation of α1-protease inhibitor by human neutrophils. J Biol Chem 256: 3348–3353.
Colvin RB and Dvorak HF (1975). Role of the clotting system in cell-mediated hypersensitivity. II. Kinetics of fibrinogen/fibrin accumulation and vascular permeability changes in tuberculin and cutaneous basophil hypersensitivity reactions. J Immunol 144: 377–387.
Colvin RB, Johnson RA, Mihm MC Jr, and Dvorak HF (1973). Role of the clotting system in cell-mediated hypersensitivity. I. Fibrin deposition in delayed skin reaction in man. J Exp Med 138: 686–698.
Contrino J, Hair GA, Schmeizl MA, Rickles FR, and Kreutzer DL (1994). In situ characterization of antigenic and functional tissue factor expression in human tumors utilizing monoclonal antibodies and recombinant factor VIIa as probes. Am J Pathol 145: 1315–1322.
Dachary-Prigent J, Toti F, Satta N, Pasquet JM, Uzan A, and Freyssinet JM (1996). Physiopathological significance of catalytic phospholipids in the generation of thrombin. Semin Thromb Hemost 22: 157–164.
DeMichele MAA, Moon DG, Fenton JW II, and Minnear FL (1990). Thrombin's enzymatic activity increases permeability of endothelial cell monolayers. J Appl Physiol 69: 1599–1606.
Drake TA, Morrissey JH, and Edgington TS (1989). Selective cellular expression of tissue factor in human tissues: Implications for disorders of hemostasis and thrombosis. Am J Pathol 134: 1087–1097.
Giesen PLA, Rauch U, Bohrmann B, Kling D, Roqué M, Fallon JT, Badmon JJ, Himber J, Riederer MA, and Nemerson Y (1999). Blood-borne tissue factor: Another view of thrombosis. Proc Natl Acad Sci USA 96: 2311–2312.
Gillis S, Furie BC, and Furie B (1997). Interactions of neutrophils and coagulation proteins. Semin Hematol 34: 336–342.
Greeno EW, Bach RR, and Moldow CF (1996). Apoptosis is associated with increased cell surface tissue factor procoagulant activity. Lab Invest 75: 281–289.
Grignani G and Maiolo A (2000). Cytokines and hemostasis. Haematologica 85: 967–972.
Hattori R, Hamilton KK, Fugate RD, McEver RP, and Sims PJ (1989). Stimulated secretion of endothelial von Willebrand factor is accompanied by rapid redistribution to the cell surface of the intracellular granule membrane protein GMP-140. J Biol Chem 264: 7768–7771.
Higure A, Okamoto K, Hirata K, Todoroki T, Nagafuchi Y, Takeda S, Itoh H, Osato K, and Nakamura S (1996). Macrophages and neutrophils infiltrating into the liver are responsible for tissue factor expression in a rabbit model of acute obstructive cholangitis. Thromb Haemost 75: 791–795.
Hui KY, Haber E, and Matsueda GR (1983). Monoclonal antibodies to a synthetic fibrin-like peptide bind to human fibrin but not fibrinogen. Science 222: 1129–1132.
Imamura T, Iyama K, Takeya M, Kambara T, and Nakamura S (1993). Role of macrophage tissue factor in the development of the delayed hypersensitivity reaction in monkey skin. Cell Immunol 152: 614–622.
Imamura T and Kambara T (1992). Role of thrombin and plasmin in development of delayed hypersensitivity reaction in guinea pig skin. Inflammation 16: 169–177.
Janus TJ, Braun DP, and Harris JE (1986). Modulation of lymphocyte responsiveness to phytohemagglutinin by micromolecular fibrinogen degradation products. Clin Immunol Immunopathol 41: 26–34.
Jones A and Geczy CL (1990). Thrombin and factor Xa enhance the production of interleukin-1. Immunology 71: 236–241.
Kay AB (1970). Studies on eosinophil leukocyte migration. I. Eosinophil and neutrophil accumulation following antigen-antibody reactions in guinea-pig skin. Clin Exp Immunol 6: 75–86.
Kohno I, Inuzuka K, Itoh Y, Nakahara K, Eguchi Y, Sugo T, Soe G, Sakata Y, Murayama H, and Matsuda M (2000). A monoclonal antibody specific to the granulocyte-derived elastase-fragment D species of human fibrinogen and fibrin: Its application to the measurement of granulocyte-derived elastase digests in plasma. Blood 95: 1721–1728.
Loike JD, Cao L, Budhu S, Marcantonio EE, El Khoury J, Hoffman S, Yednock TA, and Silverstein SC (1999). Differential regulation of β1 integrins by chemoattractants regulates neutrophil migration through fibrin. J Cell Biol 144: 1047–1056.
Mann KGR and Lundblad L (1987). Biochemistry of thrombin, 2nd ed. In: Colman RW, Hirsh J, Marder VJ, and Salzman EW, editors. Hemostasis and thrombosis: basic principles and clinical practice. Philadelphia: JB Lippincott, 148–161.
Martin SJ, Reutelingsperger CP, McGahon AJ, Rader JA, van Schie RC, LaFace DM, and Green DR (1995). Early redistribution of plasma membrane phosphatidylserine is a general feature of apoptosis regardless of the initiating stimulus: Inhibition by overexpression of Bcl-2 and Abl. J Exp Med 182: 1545–1556.
Martinez J, Ferber A, Bach TL, and Yaen CH (2001). Interaction of fibrin with VE-cadherin. Ann NY Acad Sci 936: 386–405.
Masuda M, Nakamura S, Murakami T, Komiyama Y, and Takahashi H (1996). Association of tissue factor with a γ-chain homodimer of IgE receptor type I in cultured human monocytes. Eur J Immunol 26: 2529–2532.
Müller M, Albrecht S, Golfert F, Hofer A, Funk RH, Magdolen V, Flossel C, and Luther T (1999). Localization of tissue factor in actin-filament-rich membrane areas of epithelial cells. Exp Cell Res 248: 136–147.
Naldini A, Carney DH, Bocci V, Klimpel KD, Asuncion M, Soares LE, and Klimpel GR (1993). Thrombin enhances T cell proliferative responses and cytokine production. Cell Immunol 147: 367–377.
Nemerson Y (1988). Tissue factor and hemostasis. Blood 71: 1–8.
Opie EL (1924). Pathogenesis of the specific inflammatory reaction of immunized animals (Arthus phenomenon): Relation of local “sensitization” to immunity. J Immunol 9: 259–268.
Østerud B, Rao LVM, and Olsen JO (2000). Induction of tissue factor expression in whole blood: Lack of evidence for the presence of tissue factor expression in granulocytes. Thromb Haemost 83: 861–867.
Plow EF (1980). The major fibrinolytic proteases of human leukocytes. Biochim Biophys Acta 630: 47–56.
Pulford KA, Erber WN, Crick JA, Olsson I, Micklem KJ, Gatter KC, and Mason DY (1988). Use of monoclonal antibody against human neutrophil elastase in normal and leukaemic myeloid cells. J Clin Pathol 41: 853–860.
Pulford KA, Rigney EM, Micklem KJ, Jones M, Stross WP, Gatter KC, and Mason DY (1989). KP1: A new monoclonal antibody that detects a monocyte/macrophage associated antigen in routinely processed sections. J Clin Pathol 42: 412–421.
Ranadive NS and Movat HZ (1979) Tissue injury and inflammation induced by immune complexes. In: Movat HZ, editor. Inflammation, immunity and hypersensitivity. New York: Harper & Row 409–443.
Ritchie H, Jamieson A, and Booth NA (1995). Thrombin modulates synthesis of plasminogen activator inhibitor type-2 by human peripheral blood monocytes. Blood 86: 3428–3435.
Robson SC, Saunders R, Purves LR, de Jager C, Corrigall A, and Kirsch RE (1993). Fibrin and fibrinogen degradation products with an intact D-domain C-terminal γ chain inhibit an early step in accessory cell-dependent lymphocyte mitogenesis. Blood 81: 3006–3014.
Rollet-Labelle E, Grange MJ, Elbim C, Matquetty C, Gougerot-Pocidalo MA, and Pasquier C (1998). Hydroxy radical as a potential intracellular mediator of polymorphonuclear neutrophil apoptosis. Free Radic Biol Med 24: 563–572.
Todoroki T, Higure A, Okamoto K, Okazaki K, Hirata K, Nagafuchi Y, Takeda S, Itoh H, Osato K, and Nakamura S (1998). Possible role of platelet activating factor in the in vivo expression of tissue factor in neutrophils. J Surg Res 80: 149–155.
Todoroki H, Nakamura S, Higure A, Okamoto K, Takeda S, Nagata N, Itoh H, and Ohsato K (2000). Tissue factor expression in monkey and human neutrophils. Surgery 127: 209–216.
Trevani AS, Andonegui G, Giordano M, Nociari M, Fontan P, Dran G, and Geffner JR (1996). Neutrophil apoptosis induced by proteolytic enzymes. Lab Invest 74: 711–721.
Turk JL, Rudner EJ, and Heather CJ (1966). A histochemical analysis of mononuclear cell infiltrates of the skin. II. Delayed hypersensitivity in the human. Int Arch Allergy Appl Immunol 30: 248–256.
Wu K, Urano T, Ihara H, Takada Y, Fujie M, Shikimori M, Hashimoto K, and Takada A (1995). The cleavage and inactivation of plasminogen activator inhibitor type 1 by neutrophil elastase: The evaluation of its physiologic relevance in fibrinolysis. Blood 86: 1056–1061.
Acknowledgements
This work was supported by grants from The Japanese Ministry of Education and Science (11670219 to TI and 12670984 to SN) and from Welfide Medicinal Research Foundation (to SN).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Imamura, T., Kaneda, H. & Nakamura, S. New Functions of Neutrophils in the Arthus Reaction: Expression of Tissue Factor, the Clotting Initiator, and Fibrinolysis by Elastase. Lab Invest 82, 1287–1295 (2002). https://doi.org/10.1097/01.LAB.0000032374.21141.15
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1097/01.LAB.0000032374.21141.15
This article is cited by
-
Sexual dimorphism in peripheral blood cell characteristics linked to recanalization success of endovascular thrombectomy in acute ischemic stroke
Journal of Thrombosis and Thrombolysis (2023)
-
Severe bleeding tendency caused by a rare complication of excessive fibrinolysis with disseminated intravascular coagulation in a 51-year-old Japanese man with prostate cancer: a case report
Journal of Medical Case Reports (2012)