Abstract
HSP47 is a collagen-specific chaperone that is required for normal collagen synthesis. In animal models of liver injury, hepatic stellate cells (HSC) have been identified as a source of HSP47. Because expression of HSP47 has not been investigated in human liver, the aim of these studies was to characterize expression of HSP47 in human liver and to investigate its regulation in human HSC in vitro. Immunohistochemistry demonstrated staining for HSP47 along the sinusoids of normal and cirrhotic human livers and in fibrous septa. Dual fluorescence confocal microscopy showed colocalization of HSP47 with synaptophysin, a marker for HSC. Levels of immunoreactive HSP47 and its transcript tended to be higher in cirrhotic livers than in normal livers. The abundance of HSP47 protein was unchanged by treatment of cultured human HSC with TGF-β1, angiotensin II, hypoxia and a number of other treatments intended to increase collagen synthesis. A modest reduction in HSP47 was achieved by transfection with antisense oligonucleotides and was associated with a significant decrease in procollagen synthesis. These observations suggest that HSP47 is constitutively expressed in human HSC and that HSP47 may be a target for antifibrotic therapy.
Similar content being viewed by others
Main
HSP47 is a heat shock protein that functions as a specific chaperone for procollagen molecules as they transit through the endoplasmic reticulum.1 Although the precise role of HSP47 in the processing of procollagens has not been established,2, 3 expression of HSP47 is increased in fibrotic human lung, kidney and skin4, 5, 6, 7 and in animal models of lung, kidney and liver fibrosis.8, 9, 10, 11 Recent studies have suggested that levels of procollagen gene expression and rates of procollagen synthesis are regulated coordinately with HSP47.12 In support of this concept, antisense oligonucleotides to HSP47 have been shown to reduce renal collagen accumulation in experimental glomerulonephritis and to inhibit scar formation in a cutaneous wounding model, suggesting that HSP47 plays a pivotal role in the pathogenesis of tissue fibrosis.13, 14
Data from a variety of non-human species implicate hepatic stellate cells (HSC) as the primary source of HSP47 expression in the liver. In chicken livers, HSP47 immunoreactivity was observed in bile ducts, the smooth muscle of arteries and in HSC.15 Subsequent studies in rodent models demonstrated increased hepatic expression of HSP47 during liver fibrogenesis. In carbon tetrachloride-treated rats, hepatic HSP47 transcripts increased in parallel with levels of procollagen α1(I) mRNA; HSC were identified as the source of HSP47 expression by in situ hybridization.10 Similarly, immunoreactive HSP47 increased in the livers of mice treated with carbon tetrachloride or bile-duct ligation.11 Despite the apparent importance of HSP47 in hepatic fibrogenesis, its expression in normal and diseased human liver has not been investigated previously. Accordingly, the aims of this study were to investigate the expression of HSP47 in human liver, its regulation in human HSC and the feasibility of modulating procollagen production by altering expression of HSP47 by human HSC.
Materials and methods
Liver Tissues
Samples of cryopreserved (−80°C) human livers were obtained from patients undergoing liver transplantation for end-stage liver disease due to cirrhosis resulting from various chronic liver diseases. Control samples were derived from normal donor livers obtained from the Liver Tissue Procurement and Distribution System (Fairview University Hospitals and Clinics, Minneapolis, MN, USA). All samples were coded to maintain patient anonymity. Archived blocks of formalin-fixed paraffin-embedded livers were obtained from the Department of Pathology, University of Iowa Hospitals and Clinics. The study was approved by the Institutional Review Board of the University of Iowa.
Immunohistochemistry for HSP47 in Human Livers
Sections (4–5-μm thick) were cut from formalin-fixed, paraffin-embedded tissues. Sections were deparaffinized and rehydrated by passage through a graded series of ethanol and distilled water. For HSP47 immunohistochemistry, the antigen was retrieved by heating the slides in a pressure cooker in 3 mol/l urea in distilled water for 10 min. Endogenous peroxidase activity was quenched by incubation in 0.3% (v/v) H2O2 in methanol for 20 min at room temperature. Sections were incubated for 1 h at room temperature with a monoclonal anti-HSP47 antibody (Stressgen Biotechnologies, Victoria, British Columbia) diluted 1:250 in 150 mM phosphate buffer with 500 mM NaCl and 0.05% Triton X-100, pH 7.2. Biotinylated secondary antibody was used at a dilution of 1:200. Immunostaining was performed using an avidin–biotin–horseradish peroxidase system (Vector Laboratories, Burlingame, CA, USA) with VIP as the chromogen. The sections were lightly counterstained with methyl green. Negative controls included sections in which primary antibody was omitted and/or in which the HSP47 antibody was preincubated with recombinant human HSP47 (Stressgen Biotechnologies) prior to incubation.
For immunofluorescence, liver sections were deparaffinized, rehydrated and antigen-retrieved as described above before incubation with a mixture of the HSP47 antibody (1:250) and a polyclonal rabbit anti-human synaptophysin antibody (Dako Corp., Carpinteria, CA, USA) diluted 1:50 for 2 h at room temperature. The sections were then incubated with a mixture of Texas Red-labeled anti-mouse IgG and fluorescein-labeled anti-rabbit IgG (Vector Laboratories) at a dilution of 1:100 and examined using confocal microscopy.
SDS-PAGE and Immunoblotting
Portions of frozen liver tissue (approximately 100 mg/sample) or cells were homogenized for 1 min in 20 volumes of lysis buffer (50 mmol/l Tris-HCl, pH 6.8, 5% (v/v) β-mercaptoethanol and 1% (w/v) sodium dodecyl sulfate and 10 μl/ml (v/v) protease inhibitor cocktail (Sigma, St Louis, MO, USA) using a Pyrex Tenbroeck tissue grinder (Fisher Scientific, Hanover Park, IL, USA). Homogenates were boiled for 5 min, sonicated (3 × 10 s bursts) and centrifuged at 9000 r.p.m. at 4°C for 10 min. The protein content of the supernatant was quantitated using a modification of the Lowry assay and the indicated quantities were loaded into the wells. Proteins were subjected to electrophoresis in 12% (w/v) polyacrylamide gels (Mini Protean II system; BioRad Laboratories, Richmond, CA, USA). The resolved proteins were electrophoretically transferred to nitrocellulose membranes. Nonspecific binding sites were blocked with 5% nonfat dried milk/0.5% Tween-Tris-buffered saline. After thorough washing, the membrane was first incubated with same monoclonal anti-HSP47 antibody used for immunohistochemistry diluted 1:2000, followed by peroxidase-conjugated anti-mouse IgG diluted 1:5000 (Santa Cruz Biotechnology, Santa Cruz, CA, USA). After extensive washing, bound antibody was detected using chemiluminescence according to the manufacturer's instructions (ECL; Amersham Biosciences UK Ltd., Little Chalfont, Buckinghamshire, UK). β-Actin expression was assessed by similar means, using as primary antibody a polyclonal rabbit antibody (Sigma) diluted 1:2000 in 3% (w/v) bovine serum albumin and peroxidase-conjugated anti-rabbit IgG diluted 1:5000 (Santa Cruz Biotechnology) as a secondary antibody. For procollagen α1(I) Western blots, conditioned media from HSC were concentrated using Amicon YM-100 centrifugal filter devices. Concentrated samples were diluted 1:1 in Laemmli sample buffer and loaded into 6.5% gels, electrophoresed and transferred as described above. The procollagen α1(I) antibody (SP1.D8) was obtained from the Developmental Studies Hybridoma Bank developed under the auspices of the NICHD and maintained by the University of Iowa, Department of Biological Sciences (Iowa City, IA).
RT-PCR Detection of HSP47 mRNA
Total RNA was isolated from the liver samples using the Trizol reagent (Invitrogen Life Technologies, Carlsbad, CA, USA) according to the manufacturer's instructions and quantitated spectrophotometrically. Moloney Murine Leukemia Virus Reverse Transcriptase (Invitrogen Life Technologies) was used to synthesize cDNA from 4 μg total RNA in a reaction containing 250 μM each dATP, DTTP, dCTP and dGTP, 40 U of RnaseIN (Promega, Madison, WI, USA), 250 ng random hexamer oligonucleotide primer, 5 mM DTT, 50 mM Tris-C+HCl pH 8.3, 75 mM KCl, 3 mM MgCl2 in a total volume of 40 μl. The reaction was incubated at 37°C for 60 min, then 70°C for 15 min. The cDNA product was amplified by PCR using 800 nM oligonucleotide primers for human HSP47 (sense: 5′-TTC-TGC-CTC-CTG-GAG-GCG-3′; antisense: 5′-CGC-TCA-GCA-CTG-CCT-TGG-3′), and in a separate tube, for G3PDH5′ and G3PDH3′ (Clontech, Palo Alto, CA, USA). Amplification was carried out for 30 cycles of 94°C for 30 s, 58°C for 30 s, 72°C for 30 s. PCR-amplified DNA was electrophoresed on 2% agarose gels containing 1 μg/ml ethidium bromide, which were photographed with UV transillumination. The 267 bp Hsp47 PCR product was purified using Qiaquick PCR Purification Kit (Qiagen, Chattsworth, CA, USA), and sequenced on the PE-Applied Biosystems Model 3700 Fluorescent Automated DNA Sequencer (the University of Iowa College of Medicine DNA Core Facility) using the same oligonucleotide primers that were used for PCR. The nucleotide sequence of the Hsp47 PCR product was aligned with published nucleotide sequence (GenBank accession number D81374) using BLASTN (National Center for Biotechnology Information, NIH, Bethesda, MD, USA), and was found to be essentially identical (expect value=1 × 10−111).
Real-time quantitation of HSP47 gene expression was assessed using the TaqMan Gene Expression Assay (Applied Biosystems, Foster City, CA, USA). Reverse transcription of total RNA was carried out as described above using 1 μg total RNA in a 20 μl reaction volume. In all, 2 μl of this cDNA product was used as template in a 25 μl reaction mixture containing 12.5 μl 2 × Universal Master Mix (Roche Molecular Systems, Branchburg, NJ, USA), 1.25 μl 20 × HSP47 probe-primer mix (Applied Biosystems, USA), and 9.25 μl water. The HSP47 probe is labeled with 6-FAM and spans the exon 1–exon 2 boundary (position 196) of reference sequence NM001235. The 18S PCR reaction mixture contained 12.5 μl 2 × Universal PCR Master Mix, 100 nM each forward and reverse oligonucleotide primers, 400 nM 18S-VIC-labeled probe (TaqMan Ribosomal RNA Control Reagents, Applied Biosystems, USA), and 2 μl cDNA in a reaction volume of 25 μl. Each sample was assayed in triplicate. Preliminary experiments showed similar amplification efficiencies for the HSP47 and 18S PCRs using these primer and probe concentrations. The reaction mixtures were placed in the ABI/Prism 7700 Sequence Detector System. The thermal cycle was 94°C for 10 min initial denaturation, followed by 40 two-step cycles of 94°C for 15 s, then 60°C for 1 min. For each reaction, the thermal cycle number at which the amount of amplified target rises above a fixed threshold (Ct) was determined using Sequence Detector version 1.7A. The amount of HSP47 mRNA was calculated using the comparative Ct method and is expressed as  .16
.16
Cell Culture
Primary human HSC were obtained from ScienCell Research Labs (San Diego, CA, USA). These cells are provided at passage 1, thus exhibit an activated phenotype. The cells were grown on standard tissue-culture plastic in medium provided by ScienCell Research Labs containing 2% fetal calf serum in a humidified atmosphere containing 95% air, 5% CO2. Cells were used at passages 5–19 and grown to ∼60% confluence for experiments. Cells were grown in the standard serum-containing medium during experiments in which they were exposed to xanthine–xanthine oxidase (1 mM and 1 mU/ml, respectively; Sigma), menadione (5 μM; Sigma), various extracellular matrix substrates (‘Biocoat Variety Pack,’ BD Biosciences,San Jose, CA, USA) or hypoxia for 18–20 h. For the hypoxia treatments, culture dishes were placed in a humidified sealed plastic chamber (Modular Incubator Chamber, Billups-Rothenburg, Del Mar, CA, USA) gassed with a mixture of 1% O2, 5% CO2 and 94% N2 and placed in a standard cell culture incubat or at 37°C. In the experiments in which cells were treated with angiotensin II (10 μM; Sigma), TGFβ1 (1 and 10 ng/ml; R&D) and 4-hydroxynonenal (1 and 10 μM; Cayman Chemical, Ann Arbor, MI, USA), cells were placed in standard HSC medium without serum the night before the experiment and remained in serum-free medium for the duration of the treatments.
Transfection with HSP47 Sense and Antisense Oligodeoxyribonucleotides
Oligodeoxyribonucleotides to HSP47 (sense: 5′CAT GCG CTC CCT CCT GCT TC3′; antisense: 5′GAA GCA GGA GGG AGC GCA TG3′) with phosphorothioate/phosphodiester chimeric backbones were synthesized (Integrated DNA Technologies, Coralville, IA, USA). HSC were seeded in six-well plates in a medium containing 2% fetal bovine serum 1 day before transfection. On the day of transfection, the medium was removed and the cells were rinsed with serum-free medium. The medium was removed and replaced with 1 ml of serum-free medium containing 2 μl Oligofectamine (Invitrogen Life Technologies, USA) and 250 nM oligonucleotide per well. After incubating for 4 h, serum-containing medium was added back to the wells. Cells and conditioned medium were harvested at 24-h intervals up to 96 h following transfection to assess effects on the abundance of HSP47 and procollagen α1(I), respectively.
Results
Immunohistochemistry of HSP47 in Human Liver
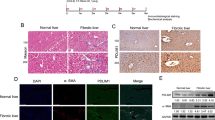
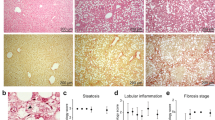
Sinusoidal lining cells of control and diseased livers were reactive with the anti-HSP47 antibody (Figure 1). In nondiseased livers, the sinusoidal HSP47 staining was observed diffusely throughout the lobule without evident zonal accentuation (Figure 1a, b). In addition, slender cells in the portal tract stroma, the endothelium of portal vein branches and hepatic arterioles and scattered cells in the muscular layer of hepatic arterioles were also HSP47-positive (Figure 1c). In cirrhotic livers, intense HSP47 expression was observed in elongated cells within the septa and in cells surrounding proliferating ductules (Figure 1e, f). HSP47-positive cells were also present along the sinusoids of the regenerative nodules in cirrhotic livers, similar to the pattern of sinusoidal cell staining observed in noncirrhotic livers. Dual immunofluorescence confocal microscopy on histologically normal human liver (Figure 2) demonstrated that HSP47 immunoreactivity colocalized with the hepatic stellate cell marker synaptophysin,17 identifying the HSP47-positive cells as hepatic stellate cells.
HSP47 is localized to sinusoidal lining cells in histologically normal and diseased human livers. Sections of livers were immunostained for HSP47 as described in the Materials and methods. (a) Low-power view of control liver showing diffuse HSP47 reactivity along the sinusoids throughout the lobule. (b) Higher magnification view of control liver illustrating the morphology of the HSP47-expressing sinusoidal lining cells. (c) Higher magnification view of a portal tract in control liver demonstrating HSP47 reactivity in the endothelium of the portal vein branch and hepatic arteriole, as well as in slender cells in the surrounding stroma. (d) HSP47-positive cells with a morphology similar to that of the portal tract stromal cells are evident within and surrounding a granuloma in a liver from a patient with primary biliary cirrhosis. (e) Low-power view of a cirrhotic liver showing intense septal HSP47 reactivity as well as a preserved pattern of sinusoidal lining cell HSP47 expression. (f) This higher magnification view of cirrhotic liver shows a portal tract that has been incorporated into fibrous septa; HSP47 reactivity is accentuated along the leading edges of the septa. Original magnifications × 10 (a, e), × 40 (b, d), × 20 (c, f).
Dual immunofluorescence confocal microscopy demonstrates colocalization of HSP47 and synaptophysin, a marker of HSC, in histologically normal human liver. Sections were incubated with a monoclonal antibody to HSP47 and a rabbit polyclonal antibody to synaptophysin, then labeled with Texas Red-tagged anti-mouse IgG and fluorescein-tagged anti-rabbit IgG. (a, d) Red fluorescence indicates HSP47-positive cells. (b, e) Green fluorescence indicates synaptophysin-positive cells. (c, f) Yellow-orange fluorescence on merged image demonstrates colocalization of HSP47 and synaptophysin. Original magnification × 20 (a–c), × 100 (d–f).
Western Blot Analysis of HSP47 in Human Liver
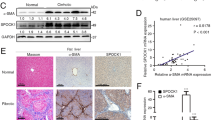
Consistent with the results of the immunohistochemistry, HSP47 was detected in control livers, albeit at a uniformly low level (Figure 3). The abundance of HSP47 was variable but generally higher in cirrhotic human livers.
Immunoreactive HSP47 is detectable in control human liver and increased in abundance in cirrhosis. Detergent extracts of liver homogenates (20 μg protein) were separated in a 12% polyacrylamide gel and transblotted onto a nitrocellulose membrane. Immunoreactive HSP47 was detected using a monoclonal anti-HSP47 antibody as described in the Materials and methods. The signal in the first lane is the 43 kD molecular weight marker; the three lanes labeled ‘control’ are samples from normal donor livers; the remaining lanes are samples from cirrhotic livers removed at the time of liver transplant. ALD, alcoholic liver disease; HCV, chronic hepatitis C infection; PBC, primary biliary cirrhosis.
RT-PCR Detection of HSP47 in Human Liver
HSP47 mRNA was faintly detectable in all livers analyzed. Despite substantial increases in immunoreactive HSP47 in most of the cirrhotic livers, the abundance of the HSP47 transcript was similar in control and cirrhotic livers as assessed by semiquantitative RT-PCR (Figure 4a). As quantitated by real-time PCR, HSP47 transcripts tended to be more abundant in cirrhotic livers compared to controls, but this difference was not statistically significant (P=0.08) (Figure 4b).
(a) RT-PCR detection of HSP47 mRNA and corresponding levels of immunoreactive HSP47 in human livers. Total RNA was isolated from human livers and reversed transcribed. The cDNA products were amplified (30 cycles) using specific primers for HSP47 and GAPDH as described in the Materials and methods. Western analysis was performed as described for Figure 2 and in the Materials and methods. RNA and protein samples were obtained from the same livers for these measurements. The first lane is a ladder (top and middle panels) or molecular weight markers (bottom panel). Control, samples from normal donor livers; ALD, cirrhosis due to alcoholic liver disease; HCV, cirrhosis due to chronic hepatitis C infection. (b) Real-time quantitation of HSP47 mRNA in control and cirrhotic human livers. Total RNA from the same livers used for the semiquantitative RT-PCR shown above was reverse transcribed and subjected to real-time PCR using the TaqMan system as described in the Material and methods. Abundance of HSP47 mRNA was determined using the comparative cycle threshold method. Data are means±s.e.m.; the difference between control and cirrhotic livers was not significant (P=0.08).
Modulation of HSP47 Expression by Human HSC In Vitro
Cultured human HSC were exposed to a variety of treatments that have been reported to alter HSP47 expression in other cell types or that have been previously shown to modulate collagen synthesis in HSC.18, 19, 20, 21, 22 These included superoxide-generating agents (xanthine–xanthine oxidase, menadione), TGF-β1, hypoxia, and culture on a variety of different matrices. As illustrated in Figure 5, HSP47 expression in activated human HSC was similar in the presence or absence of serum, or following treatment with angiotensin II, TGF-β1, xanthine–xanthine oxidase, menadione, or 1% O2 for 24 h. Similarly, no effects on HSP47 abundance were observed in HSC treated with the lipid peroxidation-derived aldehyde 4-hydroxynonenal or grown on plates coated with fibronectin, laminin, or collagen types I or IV (data not shown).
HSP47 expression in activated human HSC is unaltered by profibrogenic agents and superoxide generators. Human HSC were cultivated as described in the Material and methods. After 24 h of the indicated treatments, HSC were lysed and HSP47 analyzed by Western blot as described in the Materials and methods (2 μg protein per well). Top panel, control, HSC cultured in serum-free medium; ANGII, HSC treated with angiotensin II (10 μM); TGFβ1, HSC treated with TGF-β1 (10 ng/ml). Bottom panel, control; HSC cultured in standard serum-containing medium; X/XO, HSC treated with xanthine (1 mM) and xanthine oxidase (1 mU/ml); Mena, HSC treated with menadione (5 μM); 1% O2, HSC cultured at 1% oxygen.
Transfection of Human HSC with HSP47 Sense or Antisense Oligonucleotides
No effect on levels of HSP47 expression were seen following transfection with sense oligonucleotides or in untreated cells or cells subjected to mock transfection (transfection reagent alone) (data not shown). Maximal effects of transfection of HSP47 antisense oligonucleotides on levels of HSP47 were observed at 72–96 h. Even at these time points, the reduction in HSP47 in antisense-transfected cells vs sense controls was modest in magnitude (∼10%) (Figure 6). Interestingly, however, even this relatively small decrease in HSP47 was accompanied by a reduction in levels of procollagen α1(I) in conditioned media from HSC transfected with antisense HSP47 compared to sense-transfected HSC after 72–96 h (Figure 6).
Treatment of human HSC with antisense oligonucleotides to HSP47 lowers levels of HSP47 and is associated with a reduction in secreted α1(I) procollagen in the medium. Human HSC were transfected with sense and antisense oligonucleotides to HSP47 as described in the Materials and methods. HSC were harvested at various time points following transfection; in the experiment illustrated here, HSC and media were harvested 96 h after transfection. Cellular lysates were analyzed for HSP47 and β-actin and concentrated media for α1(I) procollagen by Western analysis as described in the Materials and methods.
Discussion
In this study, we demonstrate that HSP47-expressing sinusoidal lining cells are readily detected in histologically normal human liver. A similar pattern of HSP47 immunoreactivity has previously been reported in normal chicken and mouse liver, which has been attributed to quiescent HSC.11, 15 We have also observed HSP47-positive sinusoidal lining cells in normal rat livers (data not shown). Our finding that HSP47 expression in normal human liver colocalizes with synaptophysin, an established marker of HSC,17 confirms the identity of the HSP47-positive cells as stellate cells. Thus, expression of HSP47 appears to be a common feature of quiescent HSC in a variety of species.
Given the relatively minor amount of fibrillar collagen in healthy liver, the question arises as to the function of HSP47 in normal liver. Observations made in HSP47 knockout mice may provide some clues. HSP47-null mice die in utero, their tissues displaying fragile blood vessels, abnormally oriented epithelia and impaired basement membrane formation resulting from deficiency of mature, processed collagen.23 Although normal human liver lacks a true basement membrane, the subendothelial space of the hepatic sinusoid contains a number of matrix components, including collagen types I, III and IV.24, 25, 26 It is tempting to speculate that the matrix components in the space of Disse serve a scaffolding function in the normal liver and that HSP47 is required for the proper synthesis of these components.
In this context, it is noteworthy that HSP47 gene expression appears to be constitutive in activated human HSC. In human vascular smooth muscle cells, human embryonic lung fibroblasts, murine osteoblasts and rat cardiac fibroblasts, HSP47 expression is inducible by TGF-β1.18, 19, 20, 27 In contrast, we observed no effect of TGF-β1 on HSP47 expression in human HSC, consistent with the results of Kawada et al11 in murine HSC. Likewise, factors known to stimulate HSP47 expression in other cell types were without effect on human HSC. Although we did not compare HSP47 expression in quiescent and activated human HSC, levels of HSP47 in murine HSC have been reported to remain unaltered during activation in vitro.11 These findings are particularly intriguing in view of that fact that the transcriptional regulation of HSP47 in BALB/c 3T3 cells involves the Kruppel-like factor KLF6 (Zf9).28 In rat HSC, KLF6 is rapidly induced in response to liver injury and participates in the regulation of genes associated with the fibrogenic phenotype of HSC.29 Based on these observations, HSP47 expression by HSC might be predicted to be regulated in an activation-dependent manner. The available data do not confirm this prediction and suggest that the transcriptional regulation of HSP47 by HSC may differ from that of 3T3 cells. Further studies are needed to assess this possibility.
Additional investigations are also required to explore the disparity observed between abundance of the HSP47 transcript and levels of the immunoreactive protein in cirrhotic livers. Ours is one of relatively few studies that have directly compared levels of HSP47 mRNA and protein (and/or number of HSP47 immunoreactive cells) from identical tissue samples. In a study involving biopsies obtained from keloids, increased steady-state levels of HSP47 mRNA were associated with increased numbers of HSP47-immunoreactive fibroblasts.7 In contrast, following balloon injury to rat carotid arteries, HSP47 mRNA increased for up to 7 days after injury before declining to control levels at 14 days, while the abundance of HSP47-positive cells in the expanding neointima increased between days 7 and 14.30 Observations made using in situ hybridization in carbon tetrachloride-treated rat livers are also relevant to this question. While the abundance of HSP47 transcripts and HSP47-expressing cells increased throughout the period of CCl4 administration, HSP47 mRNA-expressing cells actually decreased in areas of ‘completed’ fibrosis at 12 weeks of CCl4 treatment.10 We speculate that similar situation may obtain in cirrhotic human livers, in that the fibrogenic process is largely ‘complete’ in the explanted livers we studied. If so, this implies that levels of HSP47 transcripts increase during periods of active fibrogenesis, only to decline as cirrhosis becomes established. A future study examining levels of HSP47 mRNA in liver biopsies at various stages of fibrosis might be helpful to test this possibility.
In any event, the persistence of increased levels of HSP47 protein in the cirrhotic livers suggests that either HSP47 expression is subject to post-transcriptional regulation and/or that the protein turns over rather slowly. The latter possibility might also explain the rather modest effects of antisense oligonucleotides on levels of HSP47 that we observed. Alternatively, it is possible that other methods, such as small interfering RNAs, might be more efficient in reducing levels of HSP47 in HSC. However, our findings that even small reductions in HSP47 are able to reduce procollagen secretion suggest that HSP47 is a rational therapeutic target for antifibrotic therapy. Indeed, given the presumption that HSP47 serves an important function in normal liver, its complete elimination from HSC may be undesirable. Further studies will be necessary to determine the magnitude of reduction in HSC HSP47 required to exert an antifibrotic effect during liver injury in vivo and whether this can be accomplished safely.
References
Nagata K, Saga S, Yamada KM . Characterization of a novel transformation-sensitive heat-shock protein (HSP47) that binds to collagen. Biochem Biophys Res Comm 1988;153:428–434.
Tasab M, Batten MR, Bulleid NJ . Hsp47: a molecular chaperone that interacts with and stabilizes correctly-folded procollagen. EMBO J 2000;19:2204–2211.
Dafforn TR, Della M, Miller AD . The molecular interactions of heat shock protein 47 (Hsp47) and their implications for collagen biosynthesis. J Biol Chem 2001;276:49310–49319.
Razzaque MS, Nazneen A, Taguchi T . Immunolocalization of collagen and collagen-binding heat shock protein 47 in fibrotic lung diseases. Mod Pathol 1998;11:1183–1188.
Razzaque MS, Kumatori A, Harada T, et al. Coexpression of collagens and collagen-binding heat shock protein 47 in human diabetic nephropathy and IgA nephropathy. Nephron 1998;80:434–443.
Kuroda K, Tsukifuji R, Shinkai H . Increased expression of heat-shock protein 47 is associated with overproduction of type I procollagen in systemic sclerosis skin fibroblasts. J Invest Dermatol 1998;111:1023–1028.
Naitoh M, Hosokawa N, Kubota H, et al. Upregulation of HSP47 and collagen type III in the dermal fibrotic disease, keloid. Biochem Biophys Res Comm 2001;280:1316–1322.
Razzaque MS, Hossain MA, Kohno S, et al. Bleomycin-induced pulmonary fibrosis in rat is associated with increased expression of collagen-bind heat shock protein (HSP) 47. Virchows Arch 1998;432:455–460.
Liu D, Razzaque MS, Cheng M, et al. The renal expression of heat shock protein 47 and collagens in acute and chronic experimental diabetes in rats. Histochem J 2001;33:621–628.
Masuda H, Fukumoto M, Hirayoshi K, et al. Coexpression of the collagen-binding stress protein HSP47 gene and the α1(I) and α1(III) collagen genes in carbon tetrachloride-induced rat liver fibrosis. J Clin Invest 1994;94:2481–2488.
Kawada N, Kuroki T, Kobayashi K, et al. Expression of heat-shock protein 47 in mouse liver. Cell Tissue Res 1996;284:341–346.
Rocnik EF, van der Veer E, Cao H, et al. Functional linkage between the endoplasmic reticulum protein Hsp47 and procollagen expression in human vascular smooth muscle cells. J Biol Chem 2002;277:38571–38578.
Sunamoto M, Kuze K, Tsuji H, et al. Antisense oligonucleotides against collagen-binding stress protein HSP47 suppress collagen accumulation in experimental glomerulonephritis. Lab Invest 1998;78:967–972.
Wang Z, Inokuchi T, Nemoto TK, et al. Antisense oligonucleotide against collagen-specific molecular chaperone 47-kDa heat shock protein suppresses scar formation in rat wounds. Plast Reconstr Surg 2003;111:1980–1987.
Miyaishi O, Sakata K, Matsuyama M, et al. Distribution of the collagen binding heat-shock protein in chicken tissues. J Histochem Cytochem 1992;40:1021–1029.
Livak KJ, Schmittgen TD . Analysis of relative gene expression data using real-time quantitative PCR and the 2−ΔΔCt method. Methods 2001;25:402–408.
Cassiman D, van Pelt J, De Vos R, et al. Synaptophysin: a novel marker for human and rat stellate cells. Am J Pathol 1999;155:1831–1839.
Rocnik E, Show LH, Pickering JG . Heat shock protein 47 is expressed in fibrous regions of human atheroma and is regulated by growth factors and oxidized low-density lipoprotein. Circulation 2000;101:1229–1233.
Yamamura I, Hirata H, Hosokawa N, et al. Transcriptional activation of the mouse HSP47 gene in mouse osteoblast MC3T3-E1 cells by TGF-β1. Biochem Biophys Res Comm 1998;244:68–74.
Takeda K, Kusachi S, Ohnishi H, et al. Greater than normal expression of the collagen-binding stress protein heat-shock protein-47 in the infarct zone in rats after experimentally-induced myocardial infarction. Coronary Artery Dis 2000;11:57–68.
Parola M, Pinzani M, Casini A, et al. Stimulation of lipid peroxidation or 4-hydroxynonenal treatment increases procollagen α1(I) gene expression in human liver fat-storing cells. Biochem Biophys Res Commun 1993;194:1044–1050.
Casini A, Ceni E, Salzano R, et al. Neutrophil-derived superoxide anion induces lipid peroxidation and stimulates collagen synthesis in human hepatic stellate cells. Hepatology 1997;25:361–367.
Nagai N, Hosokawa M, Itohara S, et al. Embryonic lethality of molecular chaperone hsp47 knockout mice is associated with defects in collagen biosynthesis. J Cell Biol 2000;150:1499–1505.
Grimaud J-A, Druguet M, Peyrol S, et al. Collagen immunotyping in human liver: light and electron microscope study. J Histochem Cytochem 1980;28:1145–1156.
Hahn E, Wick G, Pencev D, et al. Distribution of basement membrane proteins in normal and fibrotic human liver: collagen type IV, laminins, and fibronectin. Gut 1980;21:63–71.
Voss B, Rauterberg J, Allam S, et al. Distribution of collagen type I and type III and of two collagenous components of basement membrane in the human liver. Pathol Res Pract 1980;170:50–60.
Sasaki H, Sato T, Yamauchi N, et al. Induction of heat shock protein 47 synthesis by TGF-β and IL-1β via enhancement of heat shock element binding activity of heat shock transcription factor 1. J Immunol 2002;168:5178–5183.
Yasuda K, Hirayoshi K, Hirata H, et al. The Kruppel-like factor Zf9 and proteins in the Sp1 family regulate the expression of HSP47, a collagen-specific molecular chaperone. J Biol Chem 277;47:44613–44622.
Ratziu V, Lalazar A, Wong L, et al. Zf9, a Kruppel-like transcription factor up-regulated in vivo during early hepatic fibrogenesis. Proc Natl Acad Sci USA 1998;95:9500–9505.
Murakami S, Toda Y, Seki T, et al. Heat shock protein (HSP) 47 and collagen are upregulated during neointimal formation in the balloon-injured rat carotid artery. Atherosclerosis 2001;157:361–368.
Acknowledgements
KEB was supported by a Merit Review grant from the Veterans Administration. WNS was supported by a grant from the National Institutes of Health (RO1 AA13215-01).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Brown, K., Broadhurst, K., Mathahs, M. et al. Expression of HSP47, a collagen-specific chaperone, in normal and diseased human liver. Lab Invest 85, 789–797 (2005). https://doi.org/10.1038/labinvest.3700271
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.3700271
Keywords
This article is cited by
-
Ligand-tethered lipid nanoparticles for targeted RNA delivery to treat liver fibrosis
Nature Communications (2023)
-
Heat shock protein 47 is up-regulated in conjunctival bleb scarring after filtration surgery in rats
Graefe's Archive for Clinical and Experimental Ophthalmology (2015)
-
Serum heat shock protein 47 levels are elevated in acute interstitial pneumonia
BMC Pulmonary Medicine (2014)
-
Targeting siRNA to arrest fibrosis
Nature Biotechnology (2008)
-
Altered expression of iron regulatory genes in cirrhotic human livers: clues to the cause of hemosiderosis?
Laboratory Investigation (2008)