Key Points
-
Cell–cell and cell–ECM signalling contributes to epithelial structure and function and creates innate anticancer mechanisms that suppress tumorigenicity.
-
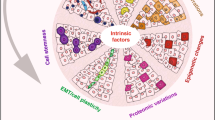
The development of carcinomas involves progressive changes in the malignant cells, in the associated stromal compartment and in the extracellular milieu. These changes lead to an ever-changing functional disorder, in which the aberrant context affects cell–cell and tissue–tissue interactions.
-
The tumour context includes both normal cells and tissues that aid in the progression of the tumour. The tumour, in turn, modifies the behaviour of the 'normal' component of the tumour.
-
The tumour context is both self-sustaining and progressive, but can be modified through alterations in signalling that affect the structure and function of tumour cells; malignant epithelial cells can be reverted to a normal phenotype despite the aberrant genotype.
-
To achieve reversion of a tumour tissue, both the tumour cells and their microenvironment need to be modified. As such, a combination of signalling inhibitors and agents that 'deactivate' the reactive stroma is required.
-
Haematologic tumours develop (and can now be treated) according to many of these same principles.
-
A better understanding of the mechanisms by which the tumour context creates the functional disorder within the tumour organ is a means of potentiating existing anticancer therapies and of developing a new generation of even more successful therapies.
Abstract
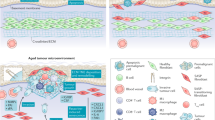
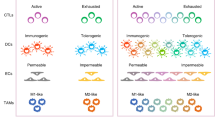
The interactions between cancer cells and their micro- and macroenvironment create a context that promotes tumour growth and protects it from immune attack. The functional association of cancer cells with their surrounding tissues forms a new 'organ' that changes as malignancy progresses. Investigation of this process might provide new insights into the mechanisms of tumorigenesis and could also lead to new therapeutic targets.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Roskelley, C. D., Srebrow, A. & Bissell, M. J. A hierarchy of ECM-mediated signalling regulates tissue-specific gene expression. Curr. Opin. Cell Biol. 7, 736–747 (1995).
Schwartz, M. A. & Baron, V. Interactions between mitogenic stimuli, or, a thousand and one connections. Curr. Opin. Cell Biol. 11, 197–202 (1999).
Giancotti, F. G. & Ruoslahti, E. Integrin signaling. Science 285, 1028–1032 (1999).
Radisky, D., Muschler, J. & Bissell, M. J. Order and disorder: the role of extracellular matrix in epithelial cancer. Cancer Invest. (in the press).
Kumar, N. M. and Gilula, N. B. The gap junction communication channel. Cell 84, 381–388 (1996).
Green, K. J. & Gaudry, C. A. Are desmosomes more than tethers for intermediate filaments? Nature Rev. Mol. Cell. Biol. 1, 208–216 (2000).
Tsukita, S., Furuse, M. and Itoh, M. Multifunctional strands in tight junctions. Nature Rev. Mol. Cell. Biol. 2, 285–293 (2001).
Runswick, S. K., O'Hare, M. J., Jones, L., Streuli, C. H. & Garrod, D. R. Desmosomal adhesion regulates epithelial morphogenesis and cell positioning. Nature Cell Biol. 3, 823—830 (2001).
Christofori, G. & Semb, H. The role of the cell-adhesion molecule E-cadherin as a tumour-suppressor gene. Trends Biochem. Sci. 24, 73–76 (1999).
Raghavan, S., Bauer, C., Mundschau, G., Li, Q. & Fuchs, E. Conditional ablation of β1 integrin in skin. Severe defects in epidermal proliferation, basement membrane formation, and hair follicle invagination. J. Cell Biol. 150, 1149–1160 (2000).
Lochter, A. et al. Matrix metalloproteinase stromelysin-1 triggers a cascade of molecular alterations that leads to stable epithelial-to-mesenchymal conversion and a premalignant phenotype in mammary epithelial cells. J. Cell Biol. 139, 1861–1872 (1997).
Hordijk, P. L. et al. Inhibition of invasion of epithelial cells by Tiam1-Rac signaling. Science 278, 1464–1466 (1997).
Perl, A. K., Wilgenbus, P., Dahl, U., Semb, H. & Christofori, G. A causal role for E-cadherin in the transition from adenoma to carcinoma. Nature 392, 190–193 (1998).Using E-cadherin knockout mice and dominant-negative forms of this protein, the authors show that loss of E-cadherin is associated with pancreatic β-cell carcinogenesis.
Hazan, R. B., Phillips, G. R., Qiao, R. F., Norton, L. & Aaronson, S. A. Exogenous expression of N-cadherin in breast cancer cells induces cell migration, invasion, and metastasis. J. Cell Biol. 148, 779–790 (2000).
Auersperg, N. et al. E-cadherin induces mesenchymal-to-epithelial transition in human ovarian surface epithelium. Proc. Natl Acad. Sci. USA 96, 6249–6254 (1999).
Nicholson, B. J., Weber, P. A., Cao, F., Chang, H., Lampe, P. & Goldberg, G. The molecular basis of selective permeability of connexins is complex and includes both size and charge. Braz. J. Med. Biol. Res. 33, 369–378 (2000).
Hanna, E. A. et al. Gap juncitonal intercellular communication and connexin43 expression in human ovarian surface epithelial cells and ovarian carcinomas in vivo and in vitro. Carcinogenesis 20, 1369–1373 (1999).
Locke, D. Gap junctions in normal and neoplastic mammary gland. J. Pathol. 186, 343–349 (1998).
Saunders, M. M. et al. Breast cancer metastatic potential correlates with a breakdown in homospecific and heterospecific gap junctional intercellular communication. Cancer Res. 61, 1765–1767 (2001).
Temme, A. et al. High incidence of spontaneous and chemically induced liver tumors in mice deficient for connexin 32. Curr. Biol. 7, 713–716 (1997).
Moennikes, O., Buchmann, A., Willecke, K., Traub, O. & Schwarz, M. Hepatocarcinogenesis in female mice with mosaic expression of connexin32. Hepatology 32, 501–506 (2000).
Zhang, Z. Q. et al. Suppression of tumorigenicity of human lung carcinoma cells after transfection with connexin43. Carcinogenesis 19, 1889–1894 (1998).
King, T. J. et al. Reduced levels of connexin43 in cervical dysplasia: inducible expression in a cervical carcinoma cell line decreases neoplastic potential with implications for tumor progression. Carcinogenesis 21, 1097–1109 (2000).
Krutovskikh, V. A. et al. Differential effect of subcellular communication impairing gap junction protein connexin43 on tumor cell grown in vivo. Oncogene 19, 505–513 (2000).
Mesnil, M. et al. Negative growth control of HeLa cells by connexin genes: connexin species specificity. Cancer Res. 55, 629–639 (1995).
Ito, A. et al. A role for heterologous gap junctions between melanoma and endothelial cells in metastasis. J. Clin. Invest. 105, 1189–1197 (2000).
Ronnov-Jessen, L., Petersen, O. W. & Bissell, M. J. Cellular changes involved in conversion of normal to malignant breast: importance of the stromal reaction. Physiol. Rev. 76, 69–125 (1996).
Sager, R. Expression genetics in cancer: shifting the focus from DNA to RNA. Proc. Natl Acad. Sci. USA 94, 952–955 (1997).
Sternlicht, M. D., Kedeshian, P., Shoa, Z. M., Safarians, S. & Barsky, S. H. The human myoepithelial cell is a natural tumor suppressor. Clin. Cancer Res. 3, 1949–1958 (1997).
Stoler, D. L. et al. The onset and extent of genomic instability in sporadic colorectal tumor progression. Proc. Natl Acad. Sci. USA 96, 15121–15126 (1999).
Frame, S. & Balmain, A. Integration of positive and negative growth signals during Ras pathway activation in vivo. Curr. Opin. Genet. Dev. 10, 106–113 (2000).
Deng, G., Lu, Y., Zlotnikov, G., Thor, A. D. & Smith, H. S. Loss of heterozygosity in normal tissue adjacent to breast carcinomas. Science 274, 2057–2059 (1996).
Washington, C., Dalbègue, F., Abreo, F., Taubenberger, J. K. & Lichy, J. H. Loss of heterozygosity in fibrocystic change of the breast. Am. J. Pathol. 157, 323–329 (2000).
Bissell, M. J. et al. Tissue structure, nuclear organization, and gene expression in normal and malignant breast. Cancer Res. 59, 1757–1763 (1999).
Sieweke, M. H. & Bissell, M. J. The tumor-promoting effect of wounding: a possible role for TGF-β-induced stromal alterations. Crit. Rev. Oncog. 5, 297–311 (1994).
Dolberg, D. S., Hollingsworth, R., Hertle, M. & Bissell, M. J. Wounding and its role in RSV-mediated tumor formation. Science 230, 676–678 (1985).
Sieweke, M. H., Thompson, N. L., Sporn, M. B. & Bissell, M. J. Mediation of wound-related Rous sarcoma virus tumorigenesis by TGF-β. Science 248, 1656–1660 (1990).
Mintz, B. & Silvers, W. K. Transgenic mouse model of malignant skin melanoma. Proc. Natl Acad. Sci. USA 90, 8817–8821 (1993).
Barcellos-Hoff, M. H. & Ravani, S. A. Irradiated mammary gland stroma promotes the expression of tumorigenic potential by unirradiated epithelial cells. Cancer Res. 60, 1254–1260 (2000).Radiation-induced mutation of the stromal microenvironment can contribute to neoplastic progression of epithelial cells in vivo , indicating that disruption of solid tissue interactions is a method by which ionizing radiation acts as a carcinogen.
Ehrhart, E. J., Segarini, P., Tsang, M. L., Carroll, A. G. & Barcellos-Hoff, M. H. Latent transforming growth factor β1 activation in situ: quantitative and functional evidence after low-dose γ-irradiation. FASEB J. 11, 991–1002 (1997).
Moinfar, F. et al. Concurrent and independent genetic alterations in the stromal and epithelial cells of mammary carcinoma: implications for tumorigenesis. Cancer Res. 60, 2562–2566 (2000).An examination of loss of heterozygosity (LOH) in microdissected mammary stromal and epithelial tissue samples. LOH at several loci was observed exclusively in stromal cells, indicating that genetic instability in the stroma can be a contributing factor to tumour progression.
Jacoby, R. F. et al. A juvenile polyposis tumor suppressor locus at 10p11 is deleted from nonepithelial cells in the lamina propria. Gastroenterology 112, 1398–1403 (1997).
Howe, J. R. et al. Mutations in the SMAD4/DPC4 gene in juvenile polyposis. Science 280, 1086–1088 (1998).Alterations in stromal function predispose colonic epithelial cells to carcinoma.
Thomasset, N. et al. Expression of autoactivated stromelysin-1 in mammary glands of transgenic mice leads to a reactive stroma during early development. Am. J. Pathol. 153, 457–467 (1998).
Tlsty, T. D. Stromal cells can contribute oncogenic signals. Semin. Cancer Biol. 11, 97–104 (2001).
Vu, T. H. & Werb, Z. Matrix metalloproteinases: effectors of development and normal physiology. Genes Dev. 14, 2123–2133 (2000).
Sethi, T. et al. Extracellular matrix proteins protect small cell lung cancer cells against apoptosis: a mechanism for small cell lung cancer growth and drug resistance in vivo. Nature Med. 5, 662–668 (1999).
Mitsiades, N., Yu, W., Poulaki, V., Tsokos, M. & Stamenkovic, I. Matrix metalloproteinase-7-mediated cleavage of Fas ligand protects tumor cells from chemotherapeutic drug cytotoxicity. Cancer Res. 61, 577–581 (2001).
Yu, Q. & Stamenkovic, I. Cell surface-localized matrix metalloproteinase-9 proteolytically activates TGF-β and promotes tumor invasion and angiogenesis. Genes Dev. 14, 163–176 (2000).
Sternlicht, M. D. et al. The stromal proteinase MMP3/stromelysin-1 promotes mammary carcinogenesis. Cell 98, 137–146 (1999).Shows that sustained expression of stromelysin-1, a stromal enzyme that destroys the basement membrane, can lead to epithelial tumorigenesis.
Wright, J. et al. A switch from stromal to tumor cell expression of stromelysin-1 mRNA is associated with the conversion of squamous to spindle cell carcinomas during mouse skin tumor progression. Mol Carcinog 10, 207–215 (1994).
Boudreau, N., Sympson, C. J., Werb, Z. & Bissell, M. J. Suppression of ICE and apoptosis in mammary epithelial cells by extracellular matrix. Science 267, 891–893 (1995).
Sympson, C. J. et al. Targeted expression of stromelysin-1 in mammary gland provides evidence for proteinases in branching morphogenesis and the requirement for an intact basement membrane for tissue-specific gene expression. J. Cell Biol. 125, 681–693 (1994).
Witty, J. P., Wright, J. H. & Matrisian, L. M. Matrix metalloproteinases are expressed during ductal and alveolar mammary morphogenesis, and misregulation of stromelysin-1 in transgenic mice induces unscheduled alveolar development. Mol. Biol. Cell. 6, 1287–1303 (1995).
Rudolph-Owen, L. A., Chan, R., Muller, W. J. & Matrisian, L. M. The matrix metalloproteinase matrilysin influences early-stage mammary tumorigenesis. Cancer Res. 58, 5500–5506 (1998).
Boulay, A. et al. High cancer cell death in syngeneic tumors developed in host mice deficient for the stromelysin-3 matrix metalloproteinase. Cancer Res. 61, 2189–2193 (2001).
Ha, H.-Y. et al. Overexpression of membrane-type matrix metalloproteinase-1 induces mammary gland abnormalities and adenocarcinoma in transgenic mice. Cancer Res. 61, 984–990 (2001).
Kaplan, D. H. et al. Demonstration of an interferon-γ-dependent tumor surveillance system in immunocompromised mice. Proc. Natl Acad. Sci. USA 95, 7556–7561 (1998).
Nakajima, C. et al. A role of interferon-γ (IFN-γ) in tumor immunity: T cells with the capacity to reject tumor cells are generated but fail to migrate to tumor sites in IFN-γ-deficient mice. Cancer Res. 61, 3399–3405 (2001).
Shankaran, V. et al. IFNγ and lymphocytes prevent primary tumour development and shape tumour immunogenicity. Nature 410, 1107–1111 (2001).
Beatty, G. L. & Paterson, Y. IFN-γ-dependent inhibition of tumor angiogenesis by tumor angiogenesis of tumor-infiltrating CD4+ T cells requires tumor responsiveness to IFN-γ. J. Immunol. 166, 2276–2282 (2001).
Hanson, H. L. et al. Eradication of established tumors by CD8+ T cell adoptive immunotherapy. Immunity 13, 265–276 (2000).
Griffith, T. S. et al. Monocyte-mediated tumoricidal activity via the tumor necrosis factor-related cytokine, TRAIL. J. Exp. Med. 189, 1343–1353 (1999).
Smyth, M. J. et al. Tumor necrosis factor-related apoptosis-inducing ligand (TRAIL) contributes to interferon-γ-dependent natural killer cell protection from tumor metastasis. J. Exp. Med. 193, 661–670 (2001).
Maria, D. A. et al. Resistance to melanoma metastases in mice selected for high acute inflammatory response. Carcinogenesis 22, 337–342 (2001).
Beatty, G. L. & Paterson, Y. IFN-γ can promote tumor evasion of the immune system in vivo by down-regulating cellular levels of an endogenous tumor antigen. J. Immunol. 165, 5502–5508 (2000).
Gati, A. et al. Tumor cells regulate the lytic activity of tumor-specific cytotoxic T lymphocytes by modulating the inhibitory natural killer receptor function. Cancer Res. 61, 3240–3244 (2001).
Ganss, R. and Hanahan, D. Tumor microenvironment can restrict the effectiveness of activated antitumor lymphocytes. Cancer Res. 58, 4673–4681 (1998).
Wei, W. Z., Fulton, A., Winkelhake, J. and Heppner, G. Correlation of natural killer activity with tumorigenesis of a preneoplastic mouse mammary lesion. Cancer Res. 49, 2709–2715 (1989).
Coussens, L. M. et al. Inflammatory mast cells upregulate angiogenesis during squamous epithelial carcinogenesis. Genes Dev. 13, 1382–1397 (1999).
Coussens, L. M., Tinkle, C. L., Hanahan, D. & Werb, Z. MMP-9 supplied by bone marrow-derived cells contributes to skin carcinogenesis. Cell 103, 481–490 (2000).References 70 and 71 showed that mast cells secrete MMP-9 following infiltration of developing squamous epithelial tumours, and that this action stimulates both development of malignancy and subsequent angiogenesis.
Bergers, B. et al. Matrix metalloproteinase-9 triggers the angiogenic switch during carcinogenesis. Nature Cell Biol. 2, 737–744 (2000).
Lin, E. Y., Nguyen, A. V., Russell, R. G. & Pollard, J. W. Colony-stimulating factor 1 promotes progression of mammary tumors to malignancy. J. Exp. Med. 193, 727–739 (2001).Showed that macrophages potentiate neoplastic progression through paracrine factors, indicating that these factors are important to tumorigenesis as genetic mutations.
Fang, K. C. et al. Mast cell expression of gelatinases A and B is regulated by kit ligand and TGF-β. J. Immunol. 162, 5528–5535 (1999).
Coussens, L. M., & Werb, Z. Inflammatory cells and cancer: think different! J. Exp. Med. 193, F23–F26 (2001).
Frank, B. T., Rossall, J. C., Caughey, G. H. & Fang, K. C. Mast cell tissue inhibitor of metalloproteinase-1 is cleaved and inactivated extracellularly by α-chymase. J. Immunol. 166, 2783–2792 (2001).
Mitchell, R. A. & Bucala, R. Tumor growth-promoting properties of macrophage migration inhibitory factor (MIF). Semin. Cancer Biol. 10, 359–366 (2000).
Abe, R., Peng, T., Sailors, J., Bucala, R. & Metz, C. N. Regulation of the CTL response by macrophage migration inhibitory factor. J. Immunol. 166, 747–753 (2001).
Hudson, J. D. et al. A proinflammatory cytokine inhibits p53 tumor suppressor activity. J. Exp. Med. 190, 1375–1382 (1999).Macrophage inhibitory factor (MIF) suppress p53-dependent transcriptional activity and blocks senescence of primary mouse embryonic fibroblasts.
Shao, C. et al. Chromosome instability contributes to loss of heterozygosity in mice lacking p53. Proc. Natl Acad. Sci. USA 97, 7405–7410 (2000).
Cordon-Cardo, C. & Prives, C. At the crossroads of inflammation and tumorigenesis. J. Exp. Med. 190, 1367–1370 (1999).
Maniotis, A. J. et al. Vascular channel formation by human melanoma cells in vivo and in vitro: vasculogenic mimicry. Am. J. Pathol. 155, 739–752 (1999).Microscopic sectioning of uveal (ocular) tumours provided the first evidence that, in addition to directing the behaviour of stromal endothelium, tumours might also develop into functional channels capable of connencting to host vasculature.
Bissell, M. J. Tumor plasticity allows vasculogenic mimicry, a novel form of angiogenic switch. Am. J. Pathol. 155, 675–679 (1999).
Chang, Y. S. et al. Mosaic blood vessels in tumors: frequency of cancer cells in contact with flowing blood. Proc. Natl Acad. Sci. USA 97, 14608–14613 (2000).
Shirikawa, K. et al. Absence of endothelial cells, central necrosis, and fibrosis are associated with aggressive inflammatory breast cancer. Cancer Res. 61, 445–451 (2001).
Sood, A. K. et al. Molecular determinants of ovarian cancer plasticity. Am. J. Pathol. 158, 1279–1288 (2001).
Hendrix, M. J. C. et al. Expression and functional significance of VE-cadherin in aggressive human melanoma cells: role in vasculogenic mimicry. Proc. Natl Acad. Sci. USA 98, 8018–8023 (2001).
Forberg, R., Hendrix, M. J. C. & Maniotis, A. J. Vasculogenic mimicry and tumor angiogenesis. Am. J. Pathol. 156, 361–381 (2000).
Akashi, K., Reya, T., Dalma-Weiszhausz, D. & Weissman, I. L. Lympoid precursors. Curr. Opin. Immunol. 12, 144–150 (2000).
Khan, A. A., Bose, C., Yam, L. S., Soloski, M. J. & Rupp, F. Physiological regulation of the immunological synapse by agrin. Science 292, 1681–1686 (2001).
Yang, F.-C. et al. Rac and Cdc42 GTPases control hematopoietic stem cell shape, adhesion, migration, and mobilization. Proc. Natl Acad. Sci. USA 98, 5614–5618 (2001).
Dror, Y. & Freedman, M. H. Schwachman–Diamond syndrome: an inherited preleukemic bone marrow failure disorder with aberrant hematopoietic progenitors and faulty marrow microenvironment. Blood 94, 3048–3054 (1999).
Damiano, J. S., Cress, A. E., Hazelhurst, L. A., Shtil, A. A. & Dalton, W. S. Cell adhesion mediated drug resistance (CAM-DR): role of integrins and resistance to apoptosis in human myeloma cell lines. Blood 93, 1658–1667 (1999).
Aziz, K. A., Till, K. J., Zuzel, M. & Cawley, J. C. Involvement of CD44–hyaluronan interaction in malignant cell homing and fibronectin synthesis in hairy cell leukemia. Blood 96, 3161–3167 (2000).
Børset, M., Hjertner, Ø., Yaccoby, S., Epstein, J. & Sanderson, R. D. Syndecan-1 is targeted to the uropods of polarized myeloma cells where it promotes adhesion and sequesters heparin-binding proteins. Blood 96, 2528–2536 (2000).
Barillé, S. et al. Metalloproteinases in multiple myeloma: production of matrix metalloproteinase-9 (MMP-9), activation of pro-MMP-2, and induction of MMP-1 by myeloma cells. Blood 90, 1649–1655 (1997).
Kossakowska, A. E. et al. Interleukin-6 regulation of matrix-metalloproteinase (MMP-2 and MMP-9) and tissue inhibitor of metalloproteinase (TIMP-1) expression in malignant non-Hodgkin's lymphomas. Blood 94, 2080–2089 (1999).
Michigami, T. et al. Cell–cell contact between marrow stromal cells and myeloma cells via VCAM-1 and α4β1-integrin enhances production of osteoclast-stimulating activity. Blood 96, 1953–1960 (2000).
Sanz-Rodríguez, F., Hidalgo, A. & Teixidó, J. Chemokine stromal cell-derived factor-1 α modulates VLA-4 integrin-mediated multiple myeloma cell adhesion to CS-1/fibronectin and VCAM-1. Blood 97, 346–351 (2001).
Vacca, A. et al. Bone marrow neovascularization, plasma cell angiogenic potential, and matrix metalloproteinase-2 secretion parallel progression of human multiple myeloma. Blood 93, 3064–3073 (1999).
Padró, T. et al. Increased angiogenesis in the bone marrow of patients with acute myeloid leukemia. Blood 95, 2637–2644 (2000).
Lagneaux, L., Delforge, A., Bron, D., De Bruyn, C. & Styckmans, P. Chronic lympocytic leukemic B cells but not normal B cells are rescued from apoptosis by contact with normal bone marrow stromal cells. Blood 91, 2387–2396 (1998).
Shain, K. H., Landowski, T. H. & Dalton, W. S. The tumor microenvironment as a determinant of cancer cell survival: a possible mechanism for de novo drug resistance. Curr. Opin. Oncol. 12, 557–563 (2000).
Mudry, R. E., Fortney, J. E., York, T., Hall, B. M. & Gibson, L. F. Stromal cells regulate survival of B-lineage leukemic cells during chemotherapy. Blood 96, 1926–1932 (2000).
Cheung, W.-C. & Van Ness, B. The bone marrow stromal microenvironment influences myeloma therapeutic response in vitro. Leukemia 15, 264–271 (2001).
Moreno, A. et al. Interleukin-6 dimers produced by endothelial cells inhibit apoptosis of B-chronic lymphocytic leukemia cells. Blood 97, 242–249 (2001).
Illmensee, K. & Mintz, B. Totipotency and normal differentiation of single teratocarcinoma cells cloned by injection into blastocysts. Proc. Natl Acad. Sci. USA 73, 549–553 (1976).Malignant mouse teratocarcinoma cells, grown through 200 transplant generations over 8 years as in vivo ascites tumours, were microinjected into developing blastocysts. The resulting genetic mosaics were normal, and tumour cells were able to develop into normal tissues.
Dolberg, D. S. & Bissell, M. J. Inability of Rous sarcoma virus to cause sarcomas in the avian embryo. Nature 309, 552–556 (1984).
Stoker, A. W., Hatier, C. & Bissell, M. J. The embryonic environment strongly attenuates v-src oncogenesis in mesenchymal and epithelial tissues, but not in endothelia. J. Cell Biol. 111, 217–228 (1990).
Olumi, A. F. et al. Carcinoma-associated fibroblasts direct tumor progression of initiated human prostatic epithelium. Cancer Res. 59, 5002–5011 (1999).A direct demonstration of the interdependence of the tumour epithelium and the tumour-associated stromal cells.
Szabowski, A. et al. c-Jun and JunB antagonistically control cytokine-regulated mesenchymal–epidermal interaction in skin. Cell 103, 745–755 (2000).
Javaherian, A., Vaccariello, M., Fusenig, N. E. & Garlick, J. A. Normal keratinocytes suppress early stages of neoplastic progression in stratified epithelium. Cancer Res. 58, 2200–2209 (1998).
Barcellos-Hoff, M. H., Aggeler, J., Ram, T. G. & Bissell, M. J. Functional differentiation and alveolar morphogenesis of primary mammary cultures on reconstituted basement membrane. Development 105, 223–235 (1989).
Petersen, O. W., Ronnov-Jessen, L., Howlett, A. R. & Bissell, M. J. Interaction with basement membrane serves to rapidly distinguish growth and differentiation pattern of normal and malignant human breast epithelial cells. Proc. Natl Acad. Sci. USA 89, 9064–9068 (1992).
Weaver, V. M. et al. Reversion of the malignant phenotype of human breast cells in three-dimensional culture and in vivo by integrin blocking antibodies. J. Cell Biol. 137, 231–245 (1997).Showed that progression to tumorigenicity in a mammary epithelial tumour-progression cell-culture model is accompanied by upregulation of β1-integrins, and that β1-blocking antibodies can restore normal phenotype and suppress tumorigenesis.
Wang, F. et al. Reciprocal interactions between β1-integrin and epidermal growth factor receptor in three-dimensional basement membrane breast cultures: a different perspective in epithelial biology. Proc. Natl Acad. Sci. USA 95, 14821–14826 (1998).
Wang, F., Yoneda, T., Barcellos-Hoff, M. H. & Bissell, M. J. Combinatorial modifications of multiple pathways reverts the malignant phenotype of mammary carcinoma cells MDA–MB231. Mol. Biol. Cell 10, 2024 (1999).
Slamon, D. J. et al. Use of chemotherapy plus a monoclonal antibody against HER2 for metastatic breast cancer that overexpresses HER2. N. Engl. J. Med. 344, 783–792 (2001).
Joensuu, H. et al. Effect of the tyrosine kinase inhibitor STI-571 in a patient with a metastatic gastrointestinal stromal tumor. N. Engl. J. Med. 344, 1052–1056 (2001).
Friedman, S. L., Maher, J. J. & Bissell, D. M. Mechanisms and therapy of hepatic fibrosis. Hepatology 32, 1403–1408 (2000).
Bilimora, M. M. et al. Underlying liver disease, not tumor factors, predicts long-term survival after resection of hepatocellular carcinoma. Arch. Surg. 136, 528–535 (2001).
Jacobs, T. W., Byrne, C., Colditz, G., Connolly, J. L. & Schnitt, S. J. Radial scars in benign breast-biopsy specimens and the risk of breast cancer. N. Engl. J. Med. 340, 430–436 (1999).
Mossman, B. T. & Churg, A. Mechanisms in the pathogenesis of asbestosis and silicosis. Am. J. Respir. Crit. Care Med. 157, 1666–1680 (1998).
Sporn, M. B. The war on cancer. Lancet 347, 1377–1381 (1996).
Sporn, M. B. & Suh, N. Chemoprevention of cancer. Carcinogenesis 21, 525–530 (2000).
Bange, J., Zwick, E. & Ullrich, A. Molecular targets for breast cancer therapy and prevention. Nature Med. 7, 548–552 (2001).
Oshima, M. et al. Suppression of intestinal polyposis in ApcΔ716 knockout mice by inhibition of prostaglandin endoperoxide synthase-2 (COX2). Cell, 87, 803–809 (1996).
Tsujii, M. et al. Cyclooxygenase regulates angiogenesis induced by colon cancer cells. Cell 93, 705–716 (1998).
Liu, C. H. et al. Overexpression of cyclooxygenase-2 is sufficient to induce tumorigenesis in transgenic mice. J. Biol. Chem. 276, 18563–18569 (2001).
Williams, C. S., Tsujii, M., Reese, J., Dey, S. K. & DuBois, R. N. Host cyclooxygenase-2 modulates carcinoma growth. J. Clin. Invest. 105, 1589–1594 (2000).Showed that the induction of angiogenesis depends upon COX2 expression within tumour-associated fibroblasts, rather than within the tumour itself.
Herbst, R. S., Lee, A. T., Tran, H. T. & Abbruzzese, J. L. Clinical studies of angiogenesis inhibitors: the University of Texas MD Anderson Center trial of human endostatin. Curr. Curr Oncol Rep 3, 131–140 (2001).
Zucker, S., Cao, J. & Chen, W.T. Critical appraisal of the use of matrix metalloproteinase inhibitors in cancer treatment. Oncogene 19, 6642—6650 (2000).
Hidalgo, H. & Eckhart, S. G. Development of matrix metalloproteinase inhibitors in cancer therapy. J. Natl Cancer Inst. 93, 178–193 (2001).
Reichmann, E. Oncogenes and epithelial cell transformation. Semin. Cancer Biol. 5, 157–165 (1994).
Bilder, D., Li, M. & Perrimon, N. Cooperative regulation of cell polarity and growth by Drosophila tumor suppressors. Science 289, 113–116 (2000).A genetic screen to identify proteins that mediate epithelial polarity in Drosophila identified a network of two known tumour suppressors and a new gene that are involved in the assembly and maintenance of gap junctions.
Bilder, D. & Perrimon, N. Localization of apical epithelial determinants by the basolateral PDZ protein Scribble. Nature 403, 676–680 (2000).
Borg, J. P. et al. ERBIN: a basolateral PDZ protein that interacts with the mammalian ERBB2/HER2 receptor. Nature Cell Biol. 2, 407–414 (2000).
Singer, A. J. and Clark, R. A. Cutaneous wound healing. N. Engl. J. Med. 341, 738–746 (1999).
Dvorak, H. F. Tumors: wounds that do not heal. N. Engl. J. Med. 315, 1650–1659 (1986).
Skobe, M. & Fusenig, N. E. Tumorigenic conversion of immortal human keratinocytes through stromal cell activation. Proc. Natl Acad. Sci. USA. 95, 1050–1055 (1998).
Blobe, G. C., Schiemann, W. P. & Lodish, H. F. Role of transforming growth factor β in human disease. N. Engl. J. Med. 342, 1350–1358 (2000).
Ronnov-Jessen, L., Petersen, O. W., Koteliansky, V. E. & Bissell, M. J. The origin of the myofibroblasts in breast cancer. Recapitulation of tumor environment in culture unravels diversity and implicates converted fibroblasts and recruited smooth muscle cells. J. Clin. Invest. 95, 859–873 (1995).
Okamoto-Inoue, M., Kamada, S., Kimura, G. & Taniguchi, S. The induction of smooth muscle α-actin in a transformed rat cell line suppresses malignant properties in vitro and in vivo. Cancer Lett. 142, 173–178 (1999).
Zajchowski, D. A. et al. Suppression of tumor-forming ability and related traits in MCF-7 human breast cancer cells by fusion with immortal mammary epithelial cells. Proc. Natl Acad. Sci. USA 87, 2314–2318 (1990).
Sager, R., Anisoxicz, A., Neveu, M., Liang, P. & Sotiropoulou, G. Identification by differential display of α6-integrin as a candidate tumor suppressor gene. FASEB J. 7, 964–970 (1993).
Lee, S. W., Reimer, C. L., Oh, P., Campbell, D. B. & Schnitzer, J. E. Tumor cell growth inhibition by caveolin re-expression in human breast cancer cells. Oncogene 16, 1391–1397 (1998).
Hirshi, K. K., Xu, C., Tsukamoto, T. & Sager, R. Gap junction genes Cx26 and Cx43 individually suppress the cancer phenotype of human mammary carcinoma cells and restore differentiation potential. Cell Growth Differ. 7, 861–870 (1996).
Zou, Z. et al. Maspin, a serpin with tumor-suppressing activity in human mammary epithelial cells. Science, 263, 526–529 (1994).
Bani, D., Riva, A., Bigazzi, M. & Sacchi, B. T. Differentiation of breast cancer cells in vitro is promoted by the concurrent influence of myoepithelial cells and relaxin. Br. J. Cancer 70, 900–904 (1994).
Liu, Q. Y. et al. Inhibitory effects of activin on the growth and morphogenesis of primary and transformed mammary epithelial cells. Cancer Res. 56, 1155–1163 (1996).
Acknowledgements
The research performed in the laboratory of M.J.B. and summarized in this review was supported by the United States Department of Energy (DOE), the Office of Biological and Environmental Research, and by the NCI. D.R. was supported by a Distinguished Hollaender Postdoctoral Fellowship from the DOE.
Author information
Authors and Affiliations
Corresponding author
Related links
Related links
DATABASES
FURTHER INFORMATION
Glossary
- ORGAN
-
An anatomically discrete collection of tissues, integrated to perform specific functions.
- TISSUE
-
A relatively homogenous structure, composed of an organized collection of cells of similar morphology and function.
- EXTRACELLULAR MATRIX
-
(ECM). A complex, three-dimensional network of very large macromolecules that provides contextual information and an architectural scaffold for cellular adhesion and migration.
- STROMA
-
Organ compartment serving as the connective tissue framework; includes fibroblasts, immune defence cells and fat cells.
- EPITHELIUM
-
A diverse group of tissues that covers or lines nearly all body surfaces, cavities and tubes, functioning as interfaces between different biological compartments. Epithelial layers provide physical protection and containment, and also mediate organ-specific transport properties.
- BASEMENT MEMBRANE
-
A specialized form of ECM that consists of laminins, collagen IV, nidogen (entactin), proteoglycans and a number of other glycoproteins that separates epithelia from underlying supporting tissues. Different organs have different compositions of basement membrane.
- ADHERENS JUNCTION
-
A physical junction that links apicolaterally localized belts of actin in adjacent epithelial cells.
- GAP JUNCTION
-
An aqueous channel that interconnects the cytoplasms of adjacent cells and allows direct exchange of small cytoplasmic components. It is created by the association of two hemichannels, each a hexamer of connexin subunits.
- TIGHT JUNCTION
-
A component of cell–cell adhesion in epithelial and endothelial cell sheets. Acts as a mediator of the diffusion of solutes through the intercellular space. Also acts as a boundary between the apical and basal plasma-membrane domains.
- DESMOSOME
-
An adhesive junction that anchors intermediate filaments between adjoining cells.
- E-CADHERIN
-
The main adhesion receptor in adherens junctions. Mediates Ca2+-dependent interactions between adjacent epithelial cells and regulates cell proliferation. It also sequesters the transcriptional co-activator β-catenin, a protein that can stimulate cell-cycle entry. The loss of E-cadherin from the cell surface might trigger epithelial–mesenchymal transition.
- EPITHELIAL–MESENCHYMAL TRANSITION
-
Conversion from an epithelial to a mesenchymal phenotype, which is a normal component of embryonic development. In carcinomas, this transformation results in altered cell morphology, the expression of mesenchymal proteins and increased invasiveness.
- CONNEXIN
-
Functions as a subunit of the gap junction hemichannel. Several members of the connexin family have been identified.
- INTERSTITIAL MATRIX
-
The extracellular matrix (ECM) contained within the stroma.
- INTERMEDIATE FILAMENT
-
A component of the eukaryotic cytoskeleton. Intermediate filaments form a dense network extending from the nucleus to the plasma membrane.
- TERATOCARCINOMA
-
A malignant germ-cell tumour arising from the ovary or testis that is composed of embryonal carcinoma cells.
- INTEGRINS
-
A family of more than 20 heterodimeric cell-surface extracellular matrix (ECM) receptors. They connect the structure of the ECM with the cytoskeleton and can transmit signalling information bidirectionally.
- HEPATIC STELLATE CELLS
-
The principal fibrogenic cell type of the liver. They are located in a perivascular orientation and contain long cytoplasmic processes that interact with neighbouring cells.
- HEMIDESMOSOME
-
An adhesion complex located at the interface of epithelial cells with the basement membranes. Responsible for linking keratin intermediate filaments to components of the extra-cellular matrix.
Rights and permissions
About this article
Cite this article
Bissell, M., Radisky, D. Putting tumours in context. Nat Rev Cancer 1, 46–54 (2001). https://doi.org/10.1038/35094059
Issue Date:
DOI: https://doi.org/10.1038/35094059
This article is cited by
-
Periostin–TGF-β feedforward loop contributes to tumour-stroma crosstalk in liver metastatic outgrowth of colorectal cancer
British Journal of Cancer (2024)
-
miRNA-383-5p Regulated Migration and Invasion of Tumor Cells by Inhibiting NCKAP1 Expression in Gastric Cancer
Biochemical Genetics (2024)
-
Tumor matrix stiffness provides fertile soil for cancer stem cells
Cancer Cell International (2023)
-
Host, reproductive, and lifestyle factors in relation to quantitative histologic metrics of the normal breast
Breast Cancer Research (2023)
-
Obesity and prostate cancer — microenvironmental roles of adipose tissue
Nature Reviews Urology (2023)