Abstract
Objective:
To evaluate whether current clinical criteria and confirmatory tests for the diagnosis of ‘brain death’ satisfy the requirements for the irreversible cessation of all functions of the entire brain including the brainstem.
Data sources:
Medical, philosophical and legal literature on the subject of ‘brain death’.
Data extraction/synthesis:
We present four arguments to support the view that patients who meet the current operational criteria of ‘brain death’ do not necessarily have the irreversible loss of all brain (or brainstem) functions. First, many clinically ‘brain-dead’ patients maintain residual vegetative functions that are mediated or coordinated by the brain or the brainstem. Second, it is impossible to test for any cerebral function by clinical bedside exam, because the tracts of passage to and from the cerebrum through the brainstem are destroyed or nonfunctional. Furthermore, since there are limitations of clinical assessment of internal awareness in patients who otherwise lack the motor function to show their awareness, the diagnosis of ‘brain death’ is based on an unproved hypothesis. Third, many patients maintain several stereotyped movements (the so-called complex spinal cord responses and automatisms) which may originate in the brainstem. Fourth, not one of the current confirmatory tests has the necessary positive predictive value for the reliable pronouncement of human death.
Conclusion:
According to the above arguments, the assumption that all functions of the entire brain (or those of the brainstem) in ‘brain-dead’ patients have ceased, is invalidated. Reconsideration of the current concept of ‘brain death’ is perhaps inevitable.
Similar content being viewed by others
Introduction
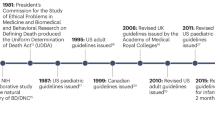
The concept of ‘brain death’ was introduced in the medical literature as a new criterion of death in 1968 by the ad hoc Committee of the Harvard Medical School.1 The Committee defined death in neurophysiological and philosophical terms, as irreversible loss of all brain functions (including those of brain stem) and proposed criteria to reflect that definition.2 The philosophical aspect of the determination of human death has also been stressed by many investigators in past and recent years.
The neuropathologic entity of total brain infarction was first described in 1902 by Cushing, but its clinical findings were first described in 1959 (Fishgold and Mathis, 1959; Jouvet, 1959; Mollaret and Goulon, 1959; Wertheimer et al., 1959);3 however, it is worthwhile mentioning that these investigators did not equate this condition with death itself.3
Machado et al.4 recently argued that the neuropathologic entity of total brain infarction/destruction did not evolve to benefit transplantation of vital organs; nevertheless, the term ‘brain death’ did not enter the medical terminology until the mid-1960s, in response to the rapidly developing field of transplantation medicine.3
The ad hoc Committee of the Harvard Medical School report did not base its neurological criterion of death on any concept of death, but rather ‘was primarily concerned with futility of care and finding ways to help physicians with withdrawal of support’.2 Others have posited, however, that the concept of ‘brain death’ was developed to permit vital organs transplantation.3, 5 Although ‘brain death’ has been accepted by most clinicians, health care workers, legislators and society at large, opinions to the contrary have been expressed both in the distant past and recently. It has been argued that ‘brain death’, either referring to the entire brain or to the brain stem alone, is a concept without precise clinical or pathological basis and, for this reason, the criteria employed in its diagnosis are arbitrary.6
In 1971 the neurosurgeons Mohandas and Chou7 suggested that in patients with known but irreparable intracranial lesions irreversible damage to the brain stem was the ‘point of no return’ and the diagnosis could be based on clinical judgment. Their suggestions became known as the Minnesota criteria and influenced the practice in the United Kingdom considerably.
Practice in the United Kingdom has been based on two memoranda; the first asserted that permanent death of the brainstem constitutes brain death while the second identified brain death with death itself. Additionally, a new document proposed by Christopher Pallis8 was that death can be defined as the ‘irreversible loss of the capacity for consciousness combined with the irreversible loss of the capacity to breathe’.
The stated definition of ‘brain death’ (the complete cessation of all functions of the entire brain) is now acknowledged even by supporters of the concept of ‘brain death’ to be only an approximation.9
Inconsistencies related to the ‘brain death’ concept
According to Bernat10, a formulation of death could be accomplished by determining the assumptions, definition, criterion and tests of death. Determining the assumptions is a philosophical task in which the concept of death is understood. Therefore, the concept of ‘brain death’ must involve (a) a definition of death which, under the whole brain formulation, could be understood as ‘the permanent cessation of functioning of the organism as a whole’ (b) a criterion of death which is defined as ‘the permanent cessation of functioning of the entire brain’ and (c) the tests of death in which two sets of tests are available for evaluating whether the criteria have been satisfied: (1) The cardiorespiratory standard (irreversible absence of circulation and respiration) (2) The neurological standard (presence of coma, documentation of apnea and absence of the brain stem reflexes—excluding reversible conditions). Therefore, ‘Identifying the definition of death is a philosophical task, the specification of the appropriate criterion to determine that the definition has been fulfilled is both a philosophical and medical task while the choice of tests and procedures that show that the criterion has been satisfied is purely a medical task’.
Since its introduction in 1968, the concept of ‘brain death’ has been criticized by many investigators.3, 5, 11, 12 The relevant critique of ‘brain death’ concept includes both definition-criteria and criteria-tests internal inconsistencies. Furthermore, Truog and Robinson13 have recently pointed out that the concept of ‘brain death’ ‘is incoherent in that it fails to correspond to any biological or philosophical understanding of death’.
Definition-criteria inconsistencies
Spinal cord reflexes and automatisms
The criteria for ‘brain death’ determination according to the ad hoc Harvard Committee were drawn up by Professor Raymond Adams14 and included ‘a permanent state of complete unreceptivity and complete unresponsivity’, the latter including all responses, whether brainstem, spinal or cerebral in origin. As a consequence, all spontaneous movements and elicitable reflexes must be absent in the state of ‘brain death’.
However, according to current guidelines for the diagnosis of ‘brain death’, the maintenance of spinal reflexes and other complex (supposedly) spinal responses or automatisms (for example, Lazarus’ sign), elicited in ‘brain dead’ patients, are not incompatible with the diagnosis of ‘brain death’.15 It is also thought that the responses which follow various environmental stimuli are compatible with ‘brain death’;16 some of these responses have recently been characterized as semipurposeful, semidirected and relatively coordinated17 and have been observed in the absence of hypoxia.18 It is, however, surprising that these ‘reflex automatisms’ have never been described in patients with high cervical spinal injuries.19
We argue, however, that these complex (supposedly) spinal cord reflexes and automatisms,20, 21, 22 which are elicited in some ‘brain-dead’ patients, are very similar to some stereotyped movements mediated by the brain stem, such as the rotational movement of the head (controlled by the interstitial nucleus) and the raising and flexing movements (controlled by the prestitial and precommissuralis nuclei, respectively) of the head and body.23 These stereotyped movements are feasible only when the above nuclei of the mesencephalon and lower diencephalon are functioning. Therefore, the similarity of these movements to the above-mentioned stereotyped ones could raise the suspicion that the involved nuclei of the brain stem might be viable in patients, otherwise diagnosed as ‘brain-dead’.
Current criteria for brain death require ‘the complete cessation of all functions of the entire brain, including the brain stem’, but do not require cessation of function of the spinal cord. Many complex movements (such as ‘head rotation, respiratory like movements, spontaneous movements of limbs—other than pathologic flexion or extension—tonic neck reflexes, abdominal reflexes) have been described in several patients diagnosed as ‘brain-dead’.16
Most neurologists claim that these movements originate in the spinal cord, and are therefore, not inconsistent with the diagnosis of ‘brain death’. Nevertheless, in patients with complete high cervical cord transection all skeletal muscle reflexes integrated in the spinal cord are completely blocked in the early phase of the spinal shock; thus, these patients are generally flaccid for 1–4 days after the lesion of the spinal cord,24 while according to Guyton and Hall25, skeletal muscle reflexes do not develop in humans until 2 weeks to several months after spinal cord transection. In addition, Shewmon26 has recently pointed out that the patients with complete cessation of function of the brain (including that of the brain stem)—‘brain-dead’ patients—should be physiologically equivalent to patients with complete high cervical cord transection; therefore, one might expect that ‘brain-dead’ patients should also be generally flaccid for 1–4 days, as it happens in patients with complete spinal cord transection.24
If the brain stem had been dead—as it (supposedly) happens in ‘brain-dead’ patients, neural pathways would have been completely interrupted; in this case it would be impossible for the spinal reflexes to emerge in a few hours as it happens in some ‘brain-dead’ patients.27 Therefore, one might conclude that in many ‘brain-dead’ patients the descending neural pathways are not completely interrupted and consequently the brain stem is not dead.
Thus, according to the above reasoning, the attribution of these complex movements to purely spinal reflexes and automatisms, may be invalid, invalidating in turn the clinical diagnosis of ‘brain death’.
The brain as a critical organ
Truog and Robinson13 have pointed out that ‘The most compelling justification for considering ‘brain-dead’ patients as being dead, is based on the notion that death is the irreversible loss of functioning of the organism as a whole. The relevant argument is that the brain is the central organizer of the body and that when the brain can no longer provide the necessary organizational influence, the body is no longer able to oppose the entropic forces favoring disintegration’.
The problem with this justification is that, as Shewmon28 has clearly shown, if ‘brain-dead’ patients are supported during the acute phase of their illness, cardiac arrest is now not certain. In a particular case, Shewmon has carefully documented prolonged somatic survival for more than 14 years in a patient with a clearly established diagnosis of brain death. The autopsy of this case showed that the brain was destroyed.29 ‘These extreme examples indicate that even if a certain level of neurologic function is necessary to maintain the functioning of the organism as a whole, the brain-dead patients are not necessarily below that threshold’.13 Therefore, recent evidence shows that survival is possible in the environment of modern Intensive Care Units—and even out of these—despite the fact that the whole brain seems destroyed, as happened with a series of patients reported by Shewmon.3, 28
The delivery of healthy infants by ‘brain-dead’ pregnant women up to 107 days after the diagnosis of ‘brain death’ is a strong argument for the presence of organism-level integration in the absence of brain function.3
Shewmon3 has also pointed out that the integrative unity of the human body is due to the mutual, dynamic interaction of its various parts and not to the dominant role of a critical organ over the sum of the organs and tissues. Accordingly, it is thought that the human organism is dead only when a supracritical irreversible damage happens because of which the body losses its inborn capability to oppose entropy.3
The conclusion of the above analysis is that somatic survival is feasible, for various periods of time, even in the presence of a totally destroyed brain; therefore, the destruction of the brain cannot be equated with the human death.
The (putative) irreversible loss of consciousness
One of the three cardinal findings and criteria for diagnosing ‘brain death’, according to the US President's Commission and the 1995 AAN guidelines, is ‘coma’30 (the other two being absence of brain stem reflexes and apnea) which is synonymous to the (irreversible) ‘absence of consciousness’—including both of its components: arousal and content of consciousness.
The content of consciousness includes cognitive and affective mental functions and whatever one is aware of at the moment (active inner awareness), as well as private self-conscious experiences, memories and acquired knowledge, which may remain latent in memory but inactivated.
Most researchers believe that in ‘brain-dead’ patients all cerebral functions—the consciousness with both its forms included—are lost, because all parts of the brain are destroyed; nevertheless, none of the tests required to document ‘brain death’ tests for the destruction of the cerebral hemispheres. Concerning the loss of content of consciousness (awareness) in ‘brain-dead’ patients, there are no criteria for the diagnosis of this loss, since consciousness is, by nature, a subjective experience.31
A more compelling argument against even the notion of absence of cerebral functions is that in the context of brain stem infarction/destruction, which is always part of brain death, it is impossible to test for any cerebral function by clinical bedside examination, because the tracts of passage to and from the cerebrum through the brain stem are destroyed or non-functional.
On the other hand, either the old or the modern confirmatory tests may not be sensitive enough to exclude minimal flow sufficient to maintain viability of some parts of the brain in ‘brain-dead’ patients. So, the confirmation of diffuse brain destruction may not be feasible using confirmatory tests.
Furthermore, in the NIH study of 503 cases involving both coma and apnea (including 146 autopsies for neuropathologic correlation), ‘it was not possible to verify that a diagnosis made before cardiac arrest by any set or subset of criteria would invariably correlate with a diffusely destroyed brain’.32
Regarding the cortical destruction—a common characteristic in both the ‘Brain-Dead’ and PVS patients, Shewmon3 comments on PVS patients pointing out: ‘patients with diffuse cortical destruction do not manifest clinical signs of awareness of self or environment. But there was no positive evidence that such patients are not inwardly conscious … mere absence of evidence does not constitute evidence of absence’.
Therefore, according to the above reasoning, the diffuse destruction of the brain and—by inference—the loss of content of consciousness in ‘brain-dead’ patients may not be possible to be verified before irreversible cardiac arrest.
Criteria-tests inconsistencies
A compelling argument against even the notion of ‘absence of cerebral functions’ is that in the context of brain stem infarction/destruction, which is always part of ‘brain death’, it is impossible to test for any cerebral function by clinical bedside examination, because the tracts of passage to and from the cerebrum through the brain stem are destroyed or nonfunctional.
There is enough evidence from the literature to assert the following in at least some ‘brain-dead’ patients:
(a) The presence of auditory or somatosensory-evoked potentials. Thus, in one ‘brain-dead’ patient there was preservation of the central auditory pathways for 72 h,33 in an infant there was only delay in brain stem conduction and intact left median nerve somatosensory-evoked potential pathways34 and in seven of eleven clinically brain dead patients there were short latency somatosensory-evoked potentials in central subcortical afferent pathways.35
(b) The maintenance of real electrocerebral activity in ‘brain-dead’ patients, even in the absence of measurable cerebral blood flow. According to Grigg et al.,36 the EEG activity was present in 11 out of 56 patients for a mean of 36.6 h and a maximum of 108 h after diagnosis; nine of the eleven patients had low-voltage β or θ EEG activity throughout the observational period. In two of the eleven patients, the EEG activity resembled that of physiologic sleep.
Furthermore, the continuing EEG activity in ‘brain-dead’ patients for many days even in the absence of measurable cerebral blood flow17 substantiates that there are inconsistencies in the tests – criterion relationships.
(c) The uptake of lipophilic radiopharmaceuticals (for example Tc-99m-HMPAO) by viable cerebral cells. These radiopharmaceuticals are taken up by viable cerebral cells (either by neurons, glial cells or both) in the cerebrum and or the cerebellum or in the basal ganglia and in the brain stem.37
Recently, Kurtec et al.38 studied 23 brain dead patients with Tc99m Hexamethylpropylene amine oxime scintigraphy and found both cerebral and cerebellar perfusion, neither cerebral nor cerebellar perfusion, cerebral without cerebellar perfusion and cerebellar without cerebral perfusion. Clinical examination criteria, according to these investigators, correctly predicted brain death only 83% of the time compared with HMPAO scintigraphy.
The afore-mentioned findings, especially the demonstrated posterior fossa perfusion—which might be interpreted that the brain stem was viable—in brain dead patients underline additional inconsistencies in applying cerebral blood flow patterns to confirm ‘brain death’.
(d) The presence of integrated hypothalamic – endocrine functions. Some investigators argue that the pituitary gland is supplied through extracranial circulation, so the maintenance of hypophyseal endocrine activity is not inconsistent with the diagnosis of ‘brain death’.39
Nevertheless, ‘since the hypothalamus is supplied with blood from the circle of Willis and the hypothalamic nuclei provide both the releasing hormones for the anterior hypophysis and the hormones to be liberated by the posterior hypophysis, preserved hypothalamic – hypophyseal function in some patients presumed to be brain dead cannot be explained by a hypothetical collateral blood flow to the anterior hypophysis through the inferior hypophyseal arteries arising extradurally from the internal carotid arteries’.40 Maintaining endocrine activity includes various integrated neuro-endocrinic functions—for example, regulation of salt and water balance, as is seen in high percentage of these patients,11, 41 temperature control, increase of the levels of growth hormone after intravenous injection of insulin42 in which hypothalamus is involved in ‘brain-dead’ patients.
(e) The maintenance of some brain stem reflexes and evidence of response to environmental stimuli. It has been shown that some ‘brain dead’ patients retain the jaw jerk and snout reflex43 while others manifest facial myokymia19or decerebrate-like posturing of the upper limbs.44 All these reflexes ‘impl(y) some living neurons in the brain stem and are thus not compatible with ‘brain death’ diagnosis.44 It has also been noted in ‘brain-dead’ patients that ‘reproducible eye opening, but with only a minimal eyelid elevation barely showing the beginning of an iris in response to twisting of a nipple. The reflex pathway is not known’.16
Also, during the early stages of organ removal lacrimation is a common phenomenon.45 According to Gray's Anatomy, ‘Preganglionic fibres probably arise from a special lacrimatory nucleus in the lower pons … These fibres synapse in the pterygopalatine ganglion which they leave in one of its branches …, to reach the lacrimal nerve. Thus they supply secromotor fibres to the gland’.46
Therefore, lacrimation in ‘brain-dead’ patients is an evidence that the lacrimatory nucleus in the brain stem is viable.
(f) The maintenance of a stable haemodynamic state for a few days in a high percentage of patients (30–78%),47 depending on the time of examination from the outset of diagnosis. Although it was pointed out that the stable hemodynamic state—without pharmacological support—is compatible with the diagnosis of brain death,15 one wonders whether a stable hemodynamic state could be maintained when the brain stem is dead.
(g) It is worthwhile noting that in two of the 25 ‘brain-dead’ patients studied by Mohandas and Chou7—who first suggested that irreversible damage to the brain stem was the ‘point of no return’ and the diagnosis could be based on clinical judgment—there were no pathological changes in the brain stem.
(h) The inadequacy of the clinical tests to accurately diagnose necrosis of the brain stem is further demonstrated by the cases of brain dead infants—diagnosed according to the current clinical criteria—who survived for weeks or months with residual function of the brain and the brainstem.34, 48
Therefore, according to the above arguments, the assumption that all functions of the entire brain (or those of the brainstem) in ‘brain-dead’ patients—diagnosed according to all proposed criteria—have ceased, is invalidated. So, we would agree with the suggestion49 that the concept of ‘brain death’ could be substituted by the more accurate old term ‘irreversible apneic coma’.
The role of the confirmatory tests in brain death diagnosis
Confirmatory tests are useful in the assessment of the electrical activity of the brain (electroencephalography and evoked potentials) as well as in the assessment of blood flow (angiography—classical and digital—radionuclide studies with lipophilic radiopharmaceuticals and transcranial Doppler sonography).
The role of confirmatory tests in the diagnosis of brain death has recently been reviewed by Plum17 and Wijdicks.16 Most investigators consider that the diagnosis of brain death is a clinical one and that confirmatory tests are only useful whenever it is impossible to perform the relevant clinical tests, when a misleading factor can interfere with the clinical examination or in children younger than 1 year of age.
Although the practical application is still limited, the planar or SPECT brain scan with the lipophilic radiopharmaceutical Tc99m-HMPAO which penetrates the intact blood – brain barrier is perhaps the test with the highest positive predictive value (the chance of having a disease given a positive test result) in the diagnosis of ‘brain death’ and has several advantages.37, 38
In a recent study on 20 brain dead patients, the four vessel classic angiography was performed the same day as SPECT of the brain with Tc99m-HMPAO. This study showed the reliability and the complete congruence between classic angiography and the radioisotope study in the demonstration of lack of brain perfusion in 19 out of 20 patients.50
Angiography, which has traditionally been considered the most accurate test in ‘brain death’ diagnosis,17 has several drawbacks6 and several studies indirectly suggest that its positive predictive value in the diagnosis of brain death is not 100%.11, 36 The specificity of electroencephalography in the diagnosis of brain death is in the order of 90%.16, 17 Transcranial Doppler also has several drawbacks.16, 17 The least specific method in the diagnosis of ‘brain death’ is evoked potentials.16 Nevertheless, when brain stem activity is found by BAEPs or SEPs ‘brain death’ diagnosis should be denied.
Therefore, it follows that no form of neurophysiologic testing currently available has 100% ‘positive predictive value’ (the chance of having a disease given a positive test result) in the diagnosis of ‘brain death’, which is necessary for the pronouncement of human death.
Truog and Robinson13 have recently correctly stated that in the absence of a world consensus on the definition of human death, the whole literature on confirmatory testing for brain death is incoherent. Nevertheless, one might argue that there is only one reason—for those who accept the current definition of brain death—for using ‘confirmatory’ testing in patients in deep coma : to prevent misdiagnosis when clinically unsuspected functions or structural integrity are maintained.
Conclusions
-
a)
Scientific knowledge alone is insufficient in determining the necessary criteria for the diagnosis of human death, since the definition of death, at the conceptual level, is a matter of philosophical, religious, legal and policy choice.
-
b)
The definition-criteria and criteria-tests inconsistencies in many patients who meet the current clinical criteria for the diagnosis of ‘brain death’ invalidate this diagnosis. Especially, the new insight presented in this article involves the interpretation of the so-called spinal reflexes and automatisms; it is argued that these movements may originate in the brainstem, thus invalidating the clinical diagnosis of ‘brain death’ in a significant number of ‘brain-dead’ patients.
-
c)
A compelling argument against even the notion of ‘absence of cerebral functions’ is that in the context of brain stem infarction/destruction, which is always part of brain death, it is impossible to test for any cerebral function by clinical bedside exam, because the tracts of passage to and from the cerebrum through the brain stem are destroyed or nonfunctional.
-
d)
Not one of the various ‘confirmatory’ tests has the necessary positive predictive value (100%), for the pronouncement of human death. Nevertheless, brain SPECT with Tc99m-HMPAO might be proved the most accurate and specific test in the diagnosis of ‘brain death’. Confirmatory tests, for the time being, cannot confirm the destruction of every part of the brain or the irreversible absence of every brain function, but only prevent misdiagnosis when clinically unsuspected functions or structural integrity are revealed.
Epilogue
Considering all the above, we wonder whether it is time to abandon the concept of ‘brain death’ and return to the traditional lung – heart criteria for the diagnosis of human death (irreversible cessation of cardiac and lung function).
Although we propose that neither ‘brain death’ nor ‘irreversible apneic coma’ are per se death, we would agree with the suggestion that the concept of ‘brain death’ could be substituted by the more accurate old term ‘irreversible apneic coma’. The expected benefits from the change of terminology and current criteria of ‘brain death’, would be the avoidance of misinformation and confusion of the public regarding the concept of human death as well as avoidance of using utilitarian criteria for its definition.
The main question addressed in this article was whether the concept of ‘brain death’ is still valid. According to the presented arguments, the concept of ‘brain death’ as a synonymous term with human death (diagnosed according to the criterion of irreversible cessation of lung and cardiac function) is invalid.
We consider that the interest of the organ transplantation program would be better served by ‘openness and honesty’. The harvesting of vital organs for transplantation from patients suffering from ‘irreversible apneic coma’ (an identical clinical condition to ‘brain death’)—who had already given their informed consent for this purpose at an unsuspected time—would be socially and morally acceptable in societies which consider that the autonomy of the person justifies such a donation.
However, others consider—on philosophical grounds—that they are not justified in taking their own life for any reason; nevertheless, they would agree with the donation of one of the paired vital organs or part of a single organ from healthy volunteers or of whatever organ from donors who are already irreversibly dead (according to the cardiopulmonary criterion of death) and have given their informed consent at an earlier time.
References
A definition of irreversible coma. Report of the ad hoc committee of the Harvard Medical School to examine the definition of brain death. J Am Med Assoc 1968; 205: 337–340.
Diringer MN, Wijdicks EFM . Brain death in historical perspective. In: Wijdicks EFM (ed). Brain Death. Lippincott Williams & Wilkins: Philadelphia, 2001, pp 5–27.
Shewmon DA . Recovery from ‘brain death’. A neurologist's apologia. Linacre Quarterly 1997, 31–96.
Machado C, Korein J, Ferrer Y, Portela L, de la C García M, Manero JM . The concept of brain death did not evolve to benefit organ transplants. J Med Ethics 2007; 33: 197–200.
Truog RD . Is it time to abandon brain death? Hastings Cent Rep (United States) 1997; 27: 29–37.
Walker AE, Molinari GF . Criteria of cerebral death. A critique. In: The NINCDS Collaborative Study of Brain Death. NINCDS Monography No 24, NIH Publication No 81-2286: Bethesda, Maryland, 1980, pp 181–199.
Mohandas A, Chou SN . Brain death. A clinical and pathological study. J Neurosurg 1971; 35: 211–218.
Pallis C . From brain death to the brain stem death. Br Med J 1982; 285: 1487–1490.
Bernat JL . How much of the brain must die in brain death? J Clin Ethics 1992; 3: 21–26.
Bernat JL . Philosophical and ethical aspects of brain death. In: Wijdicks EFM (ed). Brain Death. Lippincott Williams & Wilkins: Philadelphia, 2001, pp 171–187.
Truog RD, Fackler JC . Rethinking brain death. Crit Care Med 1992; 20: 1705–1713.
Wace J, Kai M . Anaesthesia for organ donation in the brainstem dead. Anaesthesia 2000; 55: 590.
Truog RD, Robinson WM . Role of brain death and the dead-donor rule in the ethics of organ transplantation. Crit Care Med 2003; 31: 2391–2396.
Adams RD . Foreword.: xi. In: Wijdicks EFM, (ed). Brain Death. Lippincott Williams & Wilkins: Philadelphia, 2001, pp xi.
Wijdicks EFM . Determining brain death in adults. Neurology 1995; 45: 1003–1011.
Wijdicks EFM . Clinical diagnosis and confirmatory testing of brain death in adults. In: Wijdicks EFM, (ed). Brain Death. Lippincott Williams & Wilkins: Philadelphia, 2001, pp 61–90.
Plum F . Clinical standards and technological confirmatory tests in diagnosing brain death. In: Youngner SJ, Arnold RM, Schapiro R (eds). The Definition of Death. Contemporary Controversies. The John Hopkins University: Baltimore and London, 1999, pp 34–65.
Heytens L, Verlooy J, Gheunes J, Bossaert L . Lazarus sign and extensor posturing in brain dead patient. J Neurosurg 1989; 71: 449–451.
Awada A . [Uncommon reflex automatisms after brain death]. [Article in French] Rev Neurol (Paris) 1995; 151: 586–588. Abstract.
Mandel S, Arena A, Scasta D . Spinal automatism in cerebral death. Letter to the editor. N Engl J Med 1982; 307: 501.
Ropper AH . Unusual spontaneous movements in brain dead patients. Neurology (Cleveland) 1984; 34: 1089–1092.
Bueri JA, Saposnik G, Maurino G, Saizar R, Garretto NS . Lazarus’ sign in brain death. Mov Disord 2000; 15: 583–585.
Guyton AC, Hall JE . Textbook of Medical Physiology, 9th edn. WB Saunders Co: Philadelphia, 1996, 712.
Diamantopoulos E, Olsen PZ . Excitability of motor neurones in spinal shock in man. J Neurol Neurosurg Psychiatry 1967; 30: 427–431.
Guyton AC, Hall JE . Textbook of Medical Physiology, 9th edn. WB Saunders Co: Philadelphia, 1996, 696.
Shewmon DA . Spinal shock and ‘brain death’. Somatic pathophysiological equivalence and implications for the integrative unitive rationale. Spinal Cord 1999; 37: 313–324.
Crenna P, Conci F, Boselli F . Changes in spinal reflex excitability in brain-dead humans. Electroencephalogr Clin Neurophysiol 1989; 73: 206–214.
Shewmon DA . Chronic ‘brain death’. Neurology 1998; 51: 1538–1545.
Repertinger S, Fitzgibbons WP, Omojola MF, Brumback RA . Long survival following bacterial meningitis-associated brain destruction. J Child Neurol 2006; 21: 591–595.
Plum F, Posner JB . The diagnosis of stupor and coma, 3rd edn. FA Davis Co: Philadelphia, 1987 p 3.
Giacino JT . Disorders of consciousness: differential diagnosis and neuropathologic features. Semin Neurol 1997; 17: 105–111.
Molinari GF . The NINCDS Collaborative Study of Brain Death, NINCDS Monograph No 24, NIH Publication No 81-2286, Bethesda, 1980 pp 1–32.
Barelli A, Della Corte F, Calamidi R, Sandroni C, Proietti R, Magalini SI . Do brainstem auditory evoked potentials detect the actual cessation of cerebral functions in brain dead patients? Crit Care Med 1990; 18: 322–323.
Kohrman MH, Spivack BS . Brain death in infants. Sensitivity and specificity of current criteria. Pediatr Neurol 1990; 6: 47–50.
Anzisca BJ, Cracco RQ . Short latency somatosensory evoked potentials in brain dead patients. Arch Neurol 1980; 37: 222–225.
Grigg MM, Kelly MA, Celesia GG, Ghobrial MW, Ross ER . Electroencephalographic activity after brain death. Arch Neurol 1987; 44: 948–954.
Facco E, Zuchetta P, Munari M, Baratto F, Behr AU, Gregianin M et al. Tc99m HMPAO SPECT in the diagnosis of brain death. Intensive Care Med 1998; 24: 911–917.
Kurtec RW, Lai K K-Y, Tauxe WN, Eidelman BH, Fung JJ . Tc99m Hexamethylpropylene Amine Oxime Scintigraphy in the diagnosis of brain death and its implications for the harvesting of organs used for transplantation. Clin Nucl Med 2000; 25: 7–10.
Wijdicks EFM, Atkinson LD In: Wijdicks EFM (ed). Pathophysiologic Responses to Brain Death: Brain Death. Lippincott Williams & Wilkins: Philadelphia, 2001, pp 29–43.
Coimbra CG . Implications of ishemic penumbra for the diagnosis of brain death. Braz J Med Biol Res 1999; 32: 1479–1487.
Fackler JC, Troncoso JC, Gioia FR . Age specific characteristics of brain death in children. Am J Dis Child 1988; 142: 999–1003.
Schrader H, Krogness K, Aakvaag A, Sortland O, Puruis K . Changes in pituitary hormones in brain death. Acta Neurochirurgica 1980; 52: 239–248.
Allen N, Burkholder JD, Molinari GF, Comiscioni G . Clinical criteria of brain death. In: The NINCDS Collaborative Study of Brain Death. NINCDS, Monography No 24, NIH Publication No 81-2286; Bethesda, Maryland 1980, pp 77–147.
Marti-Fabregas J, Lopez-Navidad A, Caballero F, Otermin P . Decerebrate-like posturing with mechanical ventilation in brain death. Neurology 2000; 54: 224–227.
Fitzgerald RD, Dechtyar I, Temple E, Fridrich P, Lackner FX . Cardiovascular and catecholamine response to surgery in brain dead patients. Anaesthesia 1995; 50: 388–392.
Williams RL, Banner LH, Berry MM, Collins P, Dyson M, Dussek JE, Ferguson MWJ (eds). Gray's Anatomy, 38th edn. Churchill Livingstone: New York, Edinburgh, London, 1995, pp 1233–1236.
Widjicks EFM, Rotcester MN, Bernat JL, Lebanon NH . Letter to the editor. Neurology 1999; 53: 1369–1370.
Okamoto K, Sugimoto T . Return to spontaneous respiration in an infant who fulfilled criteria to determine brain death. Pediatrics 1995; 96: 518–520.
Zamperetti N, Bellomo R, Alberto Defanti C, Latronico N . Irreversible apnoeic coma 35 years later. Towards a more rigorous definition of brain death? Intensive Care Med 2004; 30: 1715–1722.
Munari M, Zucchetta P, Carollo C, Gallo F, De Nardin M, Marzola MC et al. Confirmatory tests in the diagnosis of brain death: comparison between SPECT and contrast angiography. Crit Care Med 2005; 33: 2068–2073.
Acknowledgements
I deeply thank Professors Robert Truog (Harvard Medical School, E-mail address: Robert.Truog@childrens.harvard.edu) and D Alan Shewmon (UCLA School of Medicine, e-mail address: ashewmon@mednet.ucla.edu) for their encouragement and their kind help in the preparation of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
No funds were used to support this work. No conflict of interest with the work.
Rights and permissions
About this article
Cite this article
Karakatsanis, K. ‘Brain death’: should it be reconsidered?. Spinal Cord 46, 396–401 (2008). https://doi.org/10.1038/sj.sc.3102107
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.sc.3102107
Keywords
This article is cited by
-
Irreversibler Hirnfunktionsausfall – Teil 2. Spinalisationsphänomene
Der Nervenarzt (2021)
-
Brain death and management of the potential donor
Neurological Sciences (2021)
-
Neuroscience and Brain Death Controversies: The Elephant in the Room
Journal of Religion and Health (2018)
-
Current controversies in brain death determination
Nature Reviews Neurology (2017)
-
Revisiting the Persisting Tension Between Expert and Lay Views About Brain Death and Death Determination: A Proposal Inspired by Pragmatism
Journal of Bioethical Inquiry (2015)