Abstract
Study design:
Assessment of the potential protective effects of inosine on an animal model of spinal cord injury.
Objectives:
Our previous studies have demonstrated that inosine can directly protect neurons in vitro from zinc-induced injury and axotomized retinal ganglion cells of rats in vivo. This investigation was carried out to examine the possible protective effects of inosine on spinal cord secondary degeneration.
Setting:
Institute of Neurosciences, The Fourth Military Medical University, Xi'an, China.
Methods:
Compressive spinal cord injury (95-g load for 1 min) model was established in rats, and inosine was administrated beginning at different time points (2, 12, or 24 h) after spinal cord injury.
Results:
Using terminal deoxynucleotidyl transferase-mediated dUTP-biotin nick end labeling (TUNEL) technique and hematoxylin and eosin staining, our study demonstrated that administration of inosine as late as 12 h after injury significantly reduced the total volume of spinal cord degenerative areas and the number of apoptotic cells 3 days following the trauma.
Conclusion:
Inosine can significantly reduce the spread of secondary degeneration and the cell death following spinal cord injury in adult rats. These findings may find a clinical application in the treatment of acute spinal cord injury.
Similar content being viewed by others
Introduction
Spinal cord trauma initiates a primary injury, which results in immediate necrotic cell death at the lesion epicenter, and a devastating secondary injury which begins within minutes after initial injury and continues for days and weeks.1, 2, 3, 4 Secondary degeneration is one of the main pathological events following spinal cord injury (SCI). Attenuation of secondary degeneration has been considered critical to the outcome of the patients of SCI. Although various pharmacological strategies, such as administrations of protein synthesis inhibitors, free radical scavengers, gangliosides and NMDA receptor antagonists,3, 4, 5, 6 have been developed to reduce secondary injury, only high-dose systemic administration of methylprednisolone within 8 h after injury is proved clinically useful for human SCI.7, 8, 9 However, the use of methylprednisolone is effective only within a relatively narrow time window of 8 h after SCI, which is often impossible in many places around the world. Therefore, it is of great interest to develop more effective strategies for reducing secondary degeneration.
Secondary degeneration is caused by a variety of cellular and molecular mechanisms. Cell death is an important component of secondary injury. Although necrosis has been considered by previous studies as a characteristic of secondary cell death,10 recent studies have revealed that many of the neuronal and glial cell loss may also result from apoptosis.3, 4, 11, 12 Apoptosis is an active process of cell death that can be triggered by both intracellular and extracellular signals and involves a complex cascade of molecular and biochemical reactions in the cell. Interventions targeting at such reactions may therefore be beneficial in prevention of secondary degeneration.
Recently, the purine nucleoside inosine has been shown to play important roles in neuroprotection, glioprotection, promotion of sprouting, neurite outgrowth and axonal regeneration, immunomodulation and anti-inflammatory effects.13, 14, 15, 16, 17, 18, 19, 20, 21 These effects kindle the hope for its use in SCI to conquer secondary degeneration. The aim of the present study was to investigate the possible neuroprotective and ameliorating effects and the time window of inosine in an experimental spinal cord clip compression injury model in adult rats. Our results showed that inosine given intraperitoneally (i.p.) within 12 h after injury remarkably reduced the spinal cord secondary degeneration.
Methods
Animals
In this study, 66 adult male Sprague–Dawley rats (200–220 g) were used. The experimental study was approved by the Animal Care Committee of The Fourth Military Medical University. All efforts were made to minimize the number of animals used and their suffering.
Spinal cord injury and inosine administration
SCI at T8–9 was inflicted by clip compression. The rats were anesthetized with an i.p. injection of 1% sodium pentobarbital (50 mg/kg). A 30–40 mm dorsal midline incision was made and laminectomy was performed at T8–9 level. Compressive injury was produced by transient extradural application of a modified iris clip, which exerts a force of about 95 g on the spinal cord for 1 min. This clipping produced a moderately severe injury with immediate complete paraplegia and delayed partial motor functional recovery by 6 weeks. After removal of the clip, the skin incision was closed and the animals returned to cages with highly absorbent soft bedding in pairs (to reduce isolation-induced stress). The ambient temperature was maintained at 20–23°C. Manual massage of urinary bladder was performed twice daily until an autonomous bladder voidance reflex had developed. The rats were randomly divided into two groups. A SCI group of 36 rats were allowed to survive for 6, 12, 24 h, 3, 7 or 14 days after SCI (n=6 for each time point), respectively. Another group of 30 animals were used for SCI with the treatment of inosine. Inosine (Sigma-Aldrich, St Louis, MO, USA) was given i.p. (75 mg in 0.8 ml saline/kg body weight, once every 8 h), starting at 2, 12 or 24 h after injury (n=6 for each starting-time point). Normal saline used i.p. (0.8 ml/kg once every 8 h) starting at 2 h after injury (n=6) and sham-operation (n=6) served as controls.
Histology
The animals were killed with an overdose of sodium pentobarbital (100 mg/kg) and intracardially perfused with saline followed by 4% cold paraformaldehyde in phosphate buffer (PB, pH 7.4). Following perfusion, a 60 mm spinal cord segment with the lesion site at its center was removed and put into 20% sucrose in PB at 4°C until the blocks sank. Serial 20 μm frozen cross-sections were cut on a cryostat and mounted on slides in six sets. One set was used for routine hematoxylin and eosin (HE) staining, which showed the boundaries and areas of the cord degeneration best. Another set of the sections was used for terminal deoxynucleotidyl transferase-mediated dUTP-biotin nick end labeling (TUNEL) technique.
For TUNEL staining, briefly, the sections were blocked in 3% H2O2 in methanol for 15 min, permeabilized with 0.3% Triton X-100 in phosphate buffer saline (PBS) for 15 min at room temperature, and treated with TUNEL reagent (DeadEnd™ Colorimetric Apoptosis Detection System, Promega, USA) according to the kit instruction. The reaction was terminated by incubating with 2 × SSC for 15 min at room temperature and the product visualized with the glucose-oxidase-DAB-nickel method,22 and counterstained with Eosin. Omission of the terminal transferase served as a negative control.
Although the kit instruction recommended the tissue sections be permeabilized with proteinase K (20 μg/ml in PBS) for 10 min at room temperature, we found in our experiment that proteinase K often caused 20 μm frozen cord sections to detach from the slide they were mounted on, even if the incubation time was reduced to 2 min. Using 0.3% Triton X-100 in PBS for 15 min at room temperature instead, resulted in a distinct staining.
Quantification and statistics
Volume of the degenerative area
The boundary of the degenerative areas was drawn using a camera lucida and the areas were measured with an image analyzing system, as previously described.23 Every cross-section of the 1/6 set was measured. The total volume in mm3 was calculated by summing up the degenerative areas and multiplying 0.02 (the thickness of the section) and 6 (1/6 of the sections in a set).
Number of TUNEL-positive cells
All TUNEL-positive cells were counted and examined for the typical pathological feature of apoptosis under a microscope at a higher magnification (40 × objective) to exclude TUNEL-positive necrotic cells. The numbers in each set of sections were summed up and multiplied by 6 (1/6 of the sections in a set). The mean number of TUNEL-positive cells in each group was calculated.
Statistical analysis
The data were expressed as mean±SD and compared with one-way analysis of variance (ANOVA) followed by Dunnett's test among four different groups (2, 12 or 24 h inosine-treated groups and saline-treated group), and among different time points (6, 12, 24 h, 3, 7 or 14 days) after SCI. The statistical program (Origin ver.7.0, Microcal Corp. Northampton, MA, USA) was used for statistic analysis. P-values <0.05 were considered significant.
Results
Changes in volume of degeneration
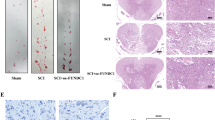
The degenerative area could be easily distinguished from the relatively normal tissue in the spinal cord sections stained with HE. However, it is not easy to clearly demarcate the border between the secondary and primary degenerative areas. Therefore, the whole degenerative areas, which consisted of necrotic tissue, apoptotic cells and cavities of various sizes, were measured (Figure 1).
Volume of degenerative area reduced with inosine
The total volumes of degenerative area of spinal cord with inosine treatment beginning at different time points were shown in Figure 2. The maximum total volume of degenerative area was observed at day 3 after injury when the number of the TUNEL-positive cells reached its peak, as shown in the following section. On the third postoperative day, significant reduction of the total degenerative volume was evidenced in rats which began to received inosine at 2 h (3.03±0.28 mm3, P<0.01) or 12 h (3.65±0.41 mm3, P<0.05) after injury, compared with that in the saline-treated animals (4.48±0.71 mm3, Figures 1 and 2). As expected, spinal cord in the sham-operated animals did not exhibit degenerative area. There was no obvious difference when the volumes of degeneration in rats with inosine administration starting at 24 h and that with saline-treatment were compared. Considering the individual variation in the size of spinal cord, a relative approach by calculating the percentage of the degenerative area in the entire cross-section area of the cord might better reflect the changes. The results were similar to that of absolute volume study (data not shown).
Temporo-spatial distribution of TUNEL-positive cells
At 6 h after injury, a few TUNEL-positive cells could be identified in the dorsal column and the gray matter within 1 mm rostral and caudal to the lesion area. The mean number of TUNEL-positive cells increased when the postoperative time increased to 12–24 h and reached the peak at day 3. The TUNEL-positive cells were distributed throughout the white and gray matter, extending to over 3–4 mm rostral and caudal to the lesion areas. The number decreased at day 7 and remained identifiable at day 14 (Figure 3).
Number of TUNEL-positive cells reduced with inosine
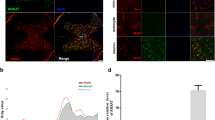
Sections obtained from saline-treated animals showed massive TUNEL-positive cells at day 3 after injury, 13 184.3±1647.1 cells in average (Figure 4). The number of TUNEL-positive cells was reduced and the staining was weaker throughout the injured cord in both the white and gray matter with early administration of inosine. In the group started at 2 h, the number of TUNEL-positive cells was reduced to 7946.5±876.7 (Figure 4). Such number in the 12 h group was 9602.5±1000.7 (Figure 4). In both cases, the number of TUNEL-positive cells was significant smaller than that of the saline-treated group (P<0.01, Figures 4 and 5). No obvious reduction in the number of TUNEL-positive cells was observed in rats treated with inosine starting at 24 h after injury. In the sham-operated rats, no TUNEL-positive cells were observed.
Micrographs illustrating TUNEL staining cross-sections 1.5 mm caudal to the lesion center, at 3 day postoperatively in rats with saline-treatment (a) and inosine treatment starting at 2 h after SCI (b). (a) Large numbers of TUNEL-positive cells were identified in both the white and gray matter along with many cavitations in the cross-section area of the cord. The boxed areas correspond to the amplified white (c) and gray (d) matter areas. (b) Only a few TUNEL-positive cells were identified in the white and gray matter in the cross-section area of the cord. The boxed areas correspond to the amplified white (e) and gray (f) matter areas. Arrows indicate the TUNEL-positive cells with apoptotic bodies or nuclear condensation. Bar=200 μm (a, b) and 25 μm (c, d, e, f)
Discussion
A major clinical concern is to minimize secondary degeneration following SCI.3, 4 An important feature of secondary degeneration in spinal cord trauma is apoptosis.3, 4, 11, 12 In our study, apoptotic cells as detected by TUNEL technique were seen at 6 h after trauma, increased in number and extent of distribution by 24 h, peeked at 3 days and continued to 14 days postinjury. The temporal changes of apoptotic cells following SCI in the present study were similar to those reported from rat SCI with compression or contusion models.11, 12, 24 However, we found that the peak of TUNEL-positive cells (3 days following SCI) was earlier than previously reported (7 days following SCI).11, 12, 24 The early peak of TUNEL-positive cells in our study may be a result of differences in the SCI model used and the force applied to the cord. Many studies employed the weight drop contusion model.11, 12 This kind of model is characterized by a contusive injury without persisting compression. In the present study, we used the extradural clip compression model at T8–9. While many features of this model are similar to the weight drop model, the clip injury does involve a 1-min period of severe compression, resulting in significant ischemia in addition to the primary impact. Therefore, our compressive model produced a severer injury in the cord, thus the extent of apoptosis. Depending on the severity of injury, apoptosis following the SCI affects a much greater extent of area than the primary injury. In addition, similar to the phenomenon in the brain, apoptotic cell death could occur and progress even a few days after the onset of ischemia. Previous studies demonstrated that the maximum number of apoptotic cells in the cerebral ischemia area appears as early as 12–24 h following insult,25, 26 and these findings may explain the early appearance of apoptosis in our study.
Although TUNEL-staining is widely used as an important marker for apoptosis, necrotic cells may also, at a certain stage, be TUNEL-positive.24, 27 To exclude any TUNEL-positive necrotic cells, all TUNEL-positive cells in the present study were not only counted but examined for the typical pathological feature of apoptosis under a microscope at a higher magnification. We found that the distribution of TUNEL-positive cells among different segments of the cord and in different areas of a section varied markedly, but the total number of TUNEL-positive cells of the cord was relatively consistent (data not shown). Therefore, we chose to count the total number of TUNEL-positive cells in the 60 mm-long injury-centered cord, rather than adopting sampling method.
In the recent years, inosine has been reported to have important effects on the injured nervous system. Thus, administration of inosine in vivo can induce massive sprouting of the normal corticospinal tract into the lesioned side of the cord,14 stimulate significant axonal rewiring and improve functional outcome after stroke,28 and protect axotomized retinal ganglion cells from optic nerve transection.19, 20 Inosine is also capable of protecting astrocytes and neurons against hypoxia, ischemia and zinc sulfate in vitro.15, 18, 29 The present study demonstrated that inosine could reduce apoptosis after crushing injury of the spinal cord. Secondary degeneration has been attributed to a number of mechanisms underlying cell death, including ATP-depletion, free radical overproduction, oxidative damage, cytokines and inflammation.1, 2, 3, 4 Inosine may act through an intracellular mechanism against ATP-depletion. It can also be catabolyzed to produce uric acid, an important natural antioxidant and peroxynitrite scavenger.21, 30 Inosine might play protective roles in acute events such as stroke and CNS trauma because of its antioxidant and antifree radical effects. Inosine has a similar structure with NAD, the substrate of Poly(ADP-ribose) polymerase (PARP). PARP is an abundant nuclear enzyme of eukaryotic cells. It is a nuclear nick sensor enzyme that becomes activated in response to DNA damage and oxidant-induced cell death.31 Activated PARP cleaves NAD+ into nicotinamide and ADP-ribose and triggers necrotic cell death. Recent studies suggested that inosine dose dependently inhibit PARP activation in macrophages.17 It is conceivable, therefore, that inosine may exert its neuroprotective effects in SCI by interfering with the PARP activation pathway. Furthermore, post-traumatic inflammation has been implicated in the secondary injury process after SCI.2, 32 Inosine may attenuate secondary damage following the SCI by reducing the production of several proinflammatory cytokines including TNFα, IL-1, IL-12 and IFNγ,16, 21 thus protect the spinal cord against secondary degeneration caused by inflammation.
The time window for effective inosine treatment of secondary degeneration following SCI was found to be at least 12 h, 50% longer than the 8 h window of methylprednisolone treatment. We have shown in vitro that inosine reduced the mortality of PC12 cells significantly in a dose-dependent manner.18 We have also demonstrated that the time window of the protective effect of inosine against apoptosis of retinal ganglion cells after optic nerve transection depends to a certain degree upon its dosage.20 It is possible that higher dosage of inosine may offer a wider time window for SCI treatment.
Conclusion
The present study shows that inosine can significantly reduce secondary degeneration following SCI in adult rats. These findings laid a basis for future clinical application of inosine in treating acute SCI.
References
Tator CH, Fehlings MG . Review of the secondary injury theory of acute spinal cord trauma with emphasis on vascular mechanisms. J Neurosurg 1991; 75: 15–26.
Schwab ME, Bartholdi D . Degeneration and regeneration of axons in the lesioned spinal cord. Physiol Rev 1996; 76: 319–370.
Amar AP, Levy ML . Pathogenesis and pharmacological strategies for mitigating secondary damage in acute spinal cord injury. Neurosurgery 1999; 44: 1027–1039.
Lu J, Ashwell KW, Waite P . Advances in secondary spinal cord injury: role of apoptosis. Spine 2000; 25: 1859–1866.
Geisler FH, Dorsey FC, Coleman WP . Recovery of motor function after spinal-cord injury – a randomized, placebo-controlled trial with GM-1 ganglioside. N Engl J Med 1991; 324: 1829–1838.
Haghighi SS, Johnson GC, de Vergel CF, Vergel Rivas BJ . Pretreatment with NMDA receptor antagonist MK801 improves neurophysiological outcome after an acute spinal cord injury. Neurol Res 1996; 18: 509–515.
Bracken MB et al. Efficacy of methylprednisolone in acute spinal cord injury. JAMA 1984; 251: 45–52.
Bracken MB et al. A randomized, controlled trial of methylprednisolone or naloxone in the treatment of acute spinal-cord injury. Results of the Second National Acute Spinal Cord Injury Study. N Engl J Med 1990; 322: 1405–1411.
Bracken MB et al. Administration of methylprednisolone for 24 or 48 hours or tirilazad mesylate for 48 hours in the treatment of acute spinal cord injury. Results of the Third National Acute Spinal Cord Injury Randomized Controlled Trial. National Acute Spinal Cord Injury Study. JAMA 1997; 277: 1597–1604.
Balentine JD . Pathology of experimental spinal cord trauma. I. The necrotic lesion as a function of vascular injury. Lab Invest 1978; 39: 236–253.
Crowe MJ, Bresnahan JC, Shuman SL, Masters JN, Beattie MS . Apoptosis and delayed degeneration after spinal cord injury in rats and monkeys. Nat Med 1997; 3: 73–76.
Liu XZ et al. Neuronal and glial apoptosis after traumatic spinal cord injury. J Neurosci 1997; 17: 5395–5406.
Benowitz LI et al. Axon outgrowth is regulated by an intracellular purine-sensitive mechanism in retinal ganglion cells. J Biol Chem 1998; 273: 29626–29634.
Benowitz LI, Goldberg DE, Madsen JR, Soni D, Irwin N . Inosine stimulates extensive axon collateral growth in the rat corticospinal tract after injury. Proc Natl Acad Sci USA 1999; 96: 13486–13490.
Litsky ML, Hohl CM, Lucas JH, Jurkowitz MS . Inosine and guanosine preserve neuronal and glial cell viability in mouse spinal cord cultures during chemical hypoxia. Brain Res 1999; 821: 426–432.
Hasko G et al. Inosine inhibits inflammatory cytokine production by a posttranscriptional mechanism and protects against endotoxin-induced shock. J Immunol 2000; 164: 1013–1019.
Marton A et al. Anti-inflammatory effects of inosine in human monocytes, neutrophils and epithelial cells in vitro. Int J Mol Med 2001; 8: 617–621.
Shi M, You SW, Meng JH, Ju G . Direct protection of inosine on PC12 cells against zinc-induced injury. Neuroreport 2002; 13: 477–479.
Wu MM, You SW, Hou B, Jiao XY, Li YY, Ju G . Effects of inosine on axonal regeneration of axotomized retinal ganglion cells in adult rats. Neurosci Lett 2003; 341: 84–86.
Hou B et al. Neuroprotective effect of inosine on axotomized retinal ganglion cells in adult rats. Invest Ophthalmol Vis Sci 2004; 45: 662–667.
Hasko G, Sitkovsky MV, Szabo C . Immunomodulatory and neuroprotective effects of inosine. Trends Pharmacol Sci 2004; 25: 152–157.
Shu SY, Ju G, Fan LZ . The glucose oxidase-DAB-nickel method in peroxidase histochemistry of the nervous system. Neurosci Lett 1988; 85: 169–171.
Liu F et al. Significance of fixation of the vertebral column for spinal cord injury experiments. Spine 2003; 28: 1666–1671.
Casha S, Yu WR, Fehlings MG . Oligodendroglial apoptosis occurs along degenerating axons and is associated with FAS and p75 expression following spinal cord injury in the rat. Neuroscience 2001; 103: 203–218.
Kharlamov A, Uz T, Joo JY, Manev H . Pharmacological characterization of apoptotic cell death in a model of photothrombotic brain injury in rats. Brain Res 1996; 734: 1–9.
Isenmann S, Stoll G, Schroeter M, Krajewski S, Reed JC, Bahr M . Differential regulation of Bax, Bcl-2, and Bcl-X proteins in focal cortical ischemia in the rat. Brain Pathol 1998; 8: 49–62.
Grasl-Kraupp B, Ruttkay-Nedecky B, Koudelka H, Bukowska K, Bursch W, Schulte-Hermann R . In situ detection of fragmented DNA (TUNEL assay) fails to discriminate among apoptosis, necrosis, and autolytic cell death: a cautionary note. Hepatology 1995; 21: 1465–1468.
Chen P, Goldberg DE, Kolb B, Lanser M, Benowitz LI . Inosine induces axonal rewiring and improves behavioral outcome after stroke. Proc Natl Acad Sci USA 2002; 99: 9031–9036.
Haun SE, Segeleon JE, Trapp VL, Clotz MA, Horrocks LA . Inosine mediates the protective effect of adenosine in rat astrocyte cultures subjected to combined glucose-oxygen deprivation. J Neurochem 1996; 67: 2051–2059.
Hooper DC et al. Uric acid, a natural scavenger of peroxynitrite, in experimental allergic encephalomyelitis and multiple sclerosis. Proc Natl Acad Sci USA 1998; 95: 675–680.
Virag L, Szabo C . Purines inhibit poly(ADP-ribose) polymerase activation and modulate oxidant-induced cell death. FASEB J 2001; 15: 99–107.
Hsu CY, Dimitrijevic MR . Methylprednisolone in spinal cord injury: the possible mechanism of action. J Neurotrauma 1990; 7: 115–119.
Acknowledgements
This work was supported by the research Grants from the National Basic Research Program of China (2003CB515031) and Natural Science Foundation of China (30371466). The authors thank Drs Bai-Ren Wang and Wei-Lin Jin for their helpful comments on the manuscript.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Liu, F., You, SW., Yao, LP. et al. Secondary degeneration reduced by inosine after spinal cord injury in rats. Spinal Cord 44, 421–426 (2006). https://doi.org/10.1038/sj.sc.3101878
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.sc.3101878
Keywords
This article is cited by
-
Spatially resolved metabolomics and isotope tracing reveal dynamic metabolic responses of dentate granule neurons with acute stimulation
Nature Metabolism (2023)
-
Serum factors mediate changes in mitochondrial bioenergetics associated with diet and exercise interventions
GeroScience (2023)
-
The antidepressant-like effect of inosine in the FST is associated with both adenosine A1 and A2A receptors
Purinergic Signalling (2013)
-
The Protective Effects of Inosine Against Chemical Hypoxia on Cultured Rat Oligodendrocytes
Cellular and Molecular Neurobiology (2011)
-
Immunomodulatory effect of the purine nucleoside inosine following spinal cord contusion injury in rat
Spinal Cord (2008)