Abstract
Objective:
This in vitro model was designed to determine whether using a no-touch method for catheter preparation and insertion would affect the degree of contamination transmitted to intermittent urinary catheters.
Setting:
Northview Laboratories, Northbrook, IL 60062, USA.
Methods:
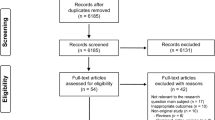
This was a parallel experimental study conducted in vitro at an independent testing laboratory under Good Manufacturing Practices. Six different models of intermittent urinary catheter were tested in triplicate, in accordance with the manufacturer's Instructions For Use (IFU). Gloved hands were contaminated with a known amount of Staphylococcus aureus or Escherichia coli, preparation for insertion was mimicked according to the manufacturer's IFU. The number of bacteria transferred to the catheter was then quantified using a validated technique. The null hypothesis tested was that the bacterial contamination resulting from handling would be the same for all of the catheters. The primary outcome measure was the amount of bacteria, expressed as colony forming units (CFU), recovered from the catheters. The catheter wrappers were sampled to confirm that active transfer of microorganisms had taken place and nonhandled samples served as the negative controls.
Results:
For both test organisms, the number of bacteria recovered from the catheters was significantly lower (P<0.05) for the catheters featuring the no-touch design (∼5 CFU/plate versus 2.1 × 102 to 4.4 × 102 for the traditional hydrophilic catheters). The bacterial recovery from those catheters with the no-touch design often fell below the nominal detection limit.
Conclusion:
The results of this study allow the null hypothesis to be rejected; it can be concluded that the no-touch method provides a significant benefit in reducing the potential for external contamination of an intermittent urinary catheter. This result supports the recent recommendations for aseptic intermittent catheterization promoted within the guidelines issued by the European Association of Urologists (EAU).
Sponsorship:
The study was funded by Hollister Incorporated.
Similar content being viewed by others
Introduction
Intermittent catheterization (IC) is considered to be the gold standard for the management of Neurological Lower Urinary Tract Dysfunction (NLUTD).1, 2, 3, 4, 5 It is effective in patients with detrusor underactivity or acontractility and in patients with detrusor overactivity if the condition is controlled by pharmacological intervention, such as anticholinergic therapy.6 The relative merits of reusable intermittent catheters or single-use disposable catheters, the use of lubricants or which specific lubricant, and aseptic or clean technique continues to be debated.
Guttmann first introduced IC at the end of the Second World War.7 The technique was further adapted by Lapides in 1972,8 who promoted the technique of clean IC, where patients simply wash their hands before holding the catheter, prior to insertion. Currently, the clean technique remains the most common practice of insertion for IC users in the community,9, 10, 11 and some authors have suggested that using hydrophilic-coated catheters may reduce the rates of bacteriuria associated with the clean technique.12 Clean technique as defined by the EAU guidelines is ‘disposable or cleansed reusable catheters, genitals washed’.13 While clean IC remains common practice, concerns have been raised by studies that show complications associated with this method including, urethral trauma and recurrent urinary tract infections.11, 14, 15, 16, 17 The method of simple hand washing prior to insertion as used with the clean technique, may not be sufficient to remove bacteria in some individuals, leading to an increase of contamination.18
Sterile IC, as introduced by Guttmann and Frankel, significantly reduces the risk of contracting a Urinary Tract Infection (UTI) and/or bacteriuria related to clean IC.13, 19, 20, 21 However, previous authors suggest that sterile IC is not widely accepted by patients in the community, as it is considered expensive and impractical.11, 22 Aseptic technique has been proffered as an alternative that reduces the risks associated with clean IC and is also easier for patients to use than sterile IC. The EAU has recently published guidelines for IC stating aseptic technique should be considered the method of choice.6 This group defines aseptic technique as, ‘the catheters remain sterile, the genitals are disinfected, and disinfecting lubricant is used’. Some authors have raised concerns regarding the use of disinfecting lubricants, while other authors have declared that simple sterile lubrication is sufficient for aseptic technique.22, 23 This paper does not address that topic. However, a method has been developed to maintain the sterility of the catheter, which facilitates the use of aseptic technique by the patient. These catheters incorporate a ‘no-touch sleeve’ that enables the user to grip the catheter through the sleeve, avoiding the need to touch the catheter. Other manufacturers promote the no-touch method by adapting the product wrapping for use during handling. Although a number of clinical studies have been reported comparing results for clean and sterile methods of IC, the aseptic method has not yet been subjected to the same scrutiny; data from large randomized controlled trials testing the method have yet to be published. The authors recognized this gap in the evidence and therefore, initial testing by the following in vitro method was performed to prove the principle that the no-touch sleeve can prevent or reduce the potential contamination of the catheter.
Methods
The test protocol was designed, validated and conducted at an independent testing laboratory. Six different models of catheters from four different manufacturers were tested. Catheters A, B, and C are standard hydrophilic catheters from two different manufacturers. Catheter D is a hydrophilic catheter that can be handled, in part, through the wrapper. Catheters E and F are catheters utilizing a self-contained gel lubricant and permit insertion via a ‘no-touch’ sleeve that covers the entire body of the catheter (Catheter A, EasiCath (Coloplast, Humlebæk, Demark); Catheter B, SpeediCath (Coloplast, Humlebæk, Demark); Catheter C, LoFric (Astra Tech, Mölndal, Sweden); Catheter D, LoFric H2O (Astra Tech, Mölndal, Sweden); Catheter E, Advance (Hollister, Illinois, USA); Catheter F, VIALOG Mobile (Medical Service, Bad Liebenzell, Germany)). Prior to performing the microbial contamination study, an Adverse Substance Screening Test was performed to ensure that catheter materials themselves did not interfere with the bacteria recovery and culturing procedures. The prospective acceptance criterion was 70% recovery. The mean recovery of both test organisms for all six catheter samples was at least 82%; therefore the recovery method was considered valid for all catheter types.
Suspensions of test microorganisms Staphylococcus aureus (S. aureus) and Escherichia coli (E. coli) were prepared according to the laboratory's Standard Operating Procedure Preparation and Maintenance of Microorganism Assay Suspensions. The target suspension level was at least 5.0 × 105–5.0 × 106 colony forming units (CFU) per ml. A technician put on sterile, nonlatex powder-free gloves that were then contaminated on each hand with 0.25 ml of each of the suspensions (total 0.5 ml), equivalent to 1.0 × 105–1.0 × 106 CFU. The contaminated hands were then rubbed together to evenly distribute the inoculum over each glove. Each inoculum's level was verified immediately after the test procedure, by direct sampling of the prepared suspension.
The preparation and insertion procedure for each catheter system was simulated according to the IFU provided with the product; this resulted in a total handling time of 30 s. Where the catheter required lubricating with water that was not contained within the packaging (catheters A and B), sterile water was utilized in order to exclude any possible contamination from the water source. The test procedure was performed in triplicate for each catheter model. A fresh set of gloves were used for each test replicate. Another technician wearing sterile gloves and using sterile scissors cut off the first-half of the catheter (used for insertion into the urethra), dropping it into a sterile receptor. An agar contact plate sample was taken of each of the wrappers, immediately after handling, to verify that microbial translocation from the gloves was actively taking place. Catheters of each sample type that had not been handled in any way were used as negative controls.
The numbers of microorganisms present on the catheters was determined according to the laboratory's bioburden extraction and plate count procedure. Briefly, each test catheter was submerged in 100 ml extraction fluid. Samples were placed on a mechanical shaker for 15 min. Serial log dilutions (100–10−3) of 5 ml aliquots were placed in sterile Petri dishes. All dishes were poured with molten tryptic soy agar and allowed to harden. The plates were inverted and incubated at 30–35°C for a minimum of 48 h. At the conclusion of the incubation period, the number of CFU per plate was counted. Any microorganisms recovered on the test plates were verified as the challenge organism via morphology. The number of microorganisms recovered for each test catheter was calculated.
Results
The average number of microorganisms recovered from the catheters expressed in CFU is shown in Table 1.
The data were analysed using two different statistical methods. The first is a nonparametric median test. The results of this test indicated that a statistically significant difference exists among the catheters for both S. aureus (P=0.0210), and E. coli (P=0.0078). For both S. aureus and E. coli, the median values observed for catheters A, B, C, and D were greater than or equal to the grand median, whereas the median values for catheters E and F were less than the grand median.
To obtain more insight, the data were normalized using a log10 transformation, entered into a general linear model, and subjected to an a posteriori comparison of the means to detect differences. The statistical method used was a Student Newman Kuels test where the ranked treatment mean values were divided into subsets which are consistent with the hypothesis of no difference (null hypothesis as tested).
Mean values sharing the same letter are considered statistically similar.
Discussion
The advent of IC has directly resulted in decreased mortality and morbidity associated with NLUTD.11, 24, 25 By enabling the maintenance of low intravesical pressure with frequent bladder emptying, IC remains an excellent option for patients' long-term bladder management. Clean technique was hailed as an advancement for IC, because it costs less and is more practicable for the user, compared to the sterile technique. However, infection remains a concern for those using IC,4, 9, 17, 26, 27, 28 and recently respected professional bodies, such as the EAU, have issued guidelines promoting aseptic technique over traditional clean technique. New products have been introduced recently that facilitate the use of aseptic technique, while maintaining ease of use of the product. These closed system products have been subjected to some initial testing and were found to reduce the number of positive cultures obtained from patients using IC, when compared to open systems.26, 29
The handling of catheters A, B, and C in this study was consistent with guidelines for the clean IC method; however, the use of sterile water, instead of regular tap water, to hydrate the hydrophilic catheters that did not provide water within the packaging (catheters A and B) removed a second source of possible contamination. As a result, this study may underestimate the total bioburden that occurs with those catheters that are commonly hydrated with tap water. The handling of catheter D followed the manufacturer's recommendation to use the product's packaging to limit direct contact between the hands and the catheter. However, it is important to note that there are design issues which may limit the ability of the typical patient to use the product in this manner. Ease of use was not addressed in this study.
The challenge organisms were consistently identified on the wrappers for all catheters, confirming that there was active transfer of microorganisms from the tester's hands, during manipulation by the testers that mimicked insertion. There was some variation between the microbial challenge levels for the different catheter types; this was due to performing the test over a number of days. In all cases, the inoculum level presented a significant microbial challenge and did not have an adverse impact on the results.
Conclusion
In laboratory tests, utilizing a handling technique consistent with each catheter's instructions for use, the number of CFUs for both S. aureus and E. coli found on catheters with a ‘no-touch sleeve’ was significantly lower than all the other products. Bacteria recovery from catheter D was less than that from the traditional hydrophilic catheters but still higher than the two with the true no-touch design. Since Catheter D has not been designed specifically to facilitate no-touch insertion, it may be considered more difficult to handle, particularly for patients with limited dexterity. The utilization of catheters providing a no-touch feature is consistent with the recommendations of the EAU for aseptic IC. More importantly, it may provide a long-term benefit to patients requiring IC by reducing the introduction of exogenous bacteria into the urinary tract.
References
Stöhrer M, Kramer G, Lochner-Ernst D, Goepel M, Noll F, Rubben H . Diagnosis and treatment of bladder dysfunction in spinal cord injury patients. Eur Urol Update Series 1994; 3: 170–175.
Günther M, Löchner-Ernst D, Kramer G, Stöhrer M . Auswirkungen des aseptischen intermittierenden Katheterismus auf die mannliche Harnrohre. Urologe [B] 2001; 41: 359–361.
Schlager TA, Dilks S, Trudell J, Whittam TS, Owen HJ . Bacteriuria in children with neurogenic bladder treated with intermittent catheterisation: natural history. J Pediatr 1995; 126: 490–496.
Bennett CJ, Young MN, Razi SS, Adkins R, Diaz F, McCrary A . The effect of urethral introducer tip catheters on the incidence of urinary tract infection outcomes in spinal cord injured patients. J Urol 1997; 158: 519–521.
Lapides J, Diokno AC, Gould FR, Lowe BS . Further observations on self-catheterization. J Urol 1976; 116: 169–171.
Madersbacher H, Wyndaele JJ, Igawa Y, Chancellor M, Chartier-Kastler E, Kovindha A . Conservative management of neuropathic urinary incontinence. In: Abrams P, Khoury S, Wein A (eds) Incontinence, 2nd edn. Health Publication Ltd: Plymouth 2002 pp 697–754.
Guttmann L, Frankel H . The value of intermittent catheterization in the early management of traumatic paraplegia and tetraplegia. Paraplegia 1966; 4: 63–84.
Lapides J, Diokno AC, Silber SJ, Lowe BS . Clean, intermittent self-catheterization in the treatment of urinary tract disease. J Urol 1972; 107: 458–461.
Prieto-Fingerhut T, Banovac K, Lynne CM . A study comparing sterile and nonsterile urethral catheterization in patients with spinal cord injury. Rehabil Nurs 1997; 22: 299–302.
Goepel M, Stöhrer M, Burgdorfer H, Brueckmann H, Djamali-Lale R . Der intermittierende Selbstkatheterismus – Ergebnisse einer vergleichenden Untersuchung. Urologe [B] 1996; 36: 190–194.
Vapnek JM, Maynard FM, Kim J . A prospective randomized trial of the LoFric hydrophilic coated catheter versus conventional plastic catheter for clean intermittent catheterization. J Urol 2003; 169: 994–998.
Hedlund H, Hjelmas K, Jonsson O, Klarskov P, Talja M . Hydrophilic versus non-coated catheters for intermittent catheterization. Scand J Urol Nephrol 2001; 35: 49–53.
Stöhrer M, Castro-Diaz D, Chartier-Kastler E, Kramer G, Mattiasson A, Wyndaele J . Guidelines on neurogenic lower urinary tract dysfunction. Eur Assoc Urol Guidelines 2003; 1–40.
Waller L, Jonsson O, Norlen L, Sullivan L . Clean intermittent catheterization in spinal cord injury patients: long-term followup of a hydrophilic low friction technique. J Urol 1995; 153: 345–348.
Wyndaele JJ, Maes D . Clean intermittent self-catheterization: a 12-year followup. J Urol 1990; 143: 906–908.
Hirano A, Tanaka H, Kuroda S . Experience with non-aseptic intermittent self-catheterization. Hinyokika Kiyo 1988; 34: 1751–1756.
Perrouin-Verbe B, Labat JJ, Richard I, Mauduyt de la Greve I, Buzelin JM, Mathe JF . Clean intermittent catheterisation from the acute period in spinal cord injury patients: long term evaluation of urethral and genital tolerance. Paraplegia 1995; 33: 619–624.
Ehrenkranz NJ, Alfonso BC . Failure of bland soap handwash to prevent hand transfer of patient bacteria to urethral catheters. Infect Control Hosp Epidemiol 1991; 12: 654–662.
Comarr AE . Intermittent catheterization for the traumatic cord bladder patient. J Urol 1972; 108: 79–81.
Anderson RU . Non-sterile intermittent catheterization with antibiotic prophylaxis in the acute spinal cord injured male patient. J Urol 1980; 124: 392–394.
Pearman JW, England EJ . Urologic follow up of spinal cord injured patients initially managed by intermittent catheterisation. Brit J Urol 1976; 43: 297–310.
Knopf H J, Bruhl P . Einmalkatheterismus – sauber (clean) oder aseptisch durchfuhren. Hyg Med 2002; 27: 33–36.
Kramer A, Rudolph P, Werner HP, Kleningat KJ . Intermittierender Katheterismus der Harnblase – hygienische Anforderungen und Befunde zur Zytotoxizität ausgewählter Katheter und Kathetergleitmittel in vitro. Hyg Med 2001; 26: 14–24.
Weld KJ, Dmochowski RR . Effect of bladder management on urological complications in spinal cord injured patients. J Urol 2000; 163: 768–772.
Perkash I, Giroux J . Clean intermittent catheterisation in spinal cord injury patients: a follow-up study. J Urol 1993; 149: 1068–1071.
Charbonneau-Smith R . No-touch catheterization and infection rates in a select spinal cord injured population. Rehabil Nurs 1993; 18: 296–299, 305.
Erickson RP, Merritt JL, Opitz JL, Ilstrup DM . Bacteriuria during follow-up in patients with spinal cord injury: I. Rates of bacteriuria in various bladder-emptying methods. Arch Phys Med Rehabil 1982; 63: 409–412.
McGuire EJ, Savastano JA . Long-term followup of spinal cord injury patients managed by intermittent catheterization. J Urol 1983; 129: 775–776.
Day RA, Moore KN, Albers MK . A pilot study comparing two methods of intermittent catheterisation: limitations and challenges. Urologic Nursing Apr 2003; 23: 143–147, 158.
Acknowledgements
We wish to thank Ms Jennifer Tenuto and Mr William Ferguson for useful discussion during the development of this methodology, and Mr Thom Nichols for performing the statistical analysis. The test protocol was designed, validated, and conducted at an independent testing laboratory. The study was funded by Hollister Incorporated.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Hudson, E., Murahata, R. The ‘no-touch’ method of intermittent urinary catheter insertion: can it reduce the risk of bacteria entering the bladder?. Spinal Cord 43, 611–614 (2005). https://doi.org/10.1038/sj.sc.3101760
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.sc.3101760
Keywords
This article is cited by
-
Prevalence and Cost of Catheters to Manage Neurogenic Bladder
Current Bladder Dysfunction Reports (2018)
-
Richtlijn intermitterende (zelf)katheterisatie bij kinderen
Tijdschrift voor Urologie (2015)
-
Neurogene Blasenfunktionsstörungen bei Patienten mit Meningomyelozele
Der Urologe (2015)
-
Intermittent self-catheterization habits and opinion on aseptic VaPro catheter in French neurogenic bladder population
Spinal Cord (2012)
-
Die Bedeutung des Katheterismus in der Neurourologie
Der Urologe (2012)