Summary:
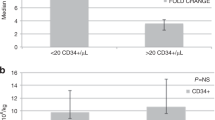
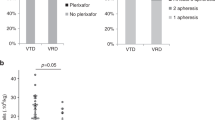
Multiple myeloma (MM) is an incurable hematologic malignancy for which autologous hematopoietic stem cell transplantation (HCT) is a standard therapy. The optimal method of stem cell mobilization is not defined. We evaluated intravenous melphalan (60 mg/m2), the most effective agent for MM, and G-CSF (10 μg/kg/day) for mobilization. End points were safety, adequacy of CD34+ collections, MM response, and contamination of stem cell components (SCC). In total, 32 patients were mobilized. There were no deaths or significant bleeding episodes; 14 patients (44%) required hospitalization for neutropenic fever. Median days of grade 3 or 4 neutropenia or thrombocytopenia were 7 (2–20) and 8 (3–17). Median mobilization days, CD34+ cells/kg and total leukaphereses were 16 (12–30), 12.1 million (2.6–52.8), and 2 (1–5) respectively. Four patients (12.5 %) failed to achieve the target of 4 million CD34+ cells/kg in five leukaphereses. Reduction in myeloma was seen in 11 patients (34%) with 3 (9%) achieving complete response; 15 (47%) maintained prior responses. Estimated MM contamination per SCC (N=48) was 0.0009% (range 0–0.1) and 0.21 × 10 4 cells per kg (range 0–41.2). Increased contamination was associated with increased patient age. This strategy for mobilization is feasible, frequently requires hospitalization and transfusion, and controls disease in most patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Durie BG, Kyle RA, Belch A et al. Myeloma management guidelines: a consensus report from the Scientific Advisors of the International Myeloma Foundation. Hematol J 2003; 4: 379–398.
Berenson JR, Lichtenstein A, Porter L et al. Efficacy of pamidronate in reducing skeletal events in patients with advanced multiple myeloma. Myeloma Aredia Study Group. N Engl J Med 1996; 334: 488–493.
Attal M, Harousseau JL, Stoppa AM et al. A prospective, randomized trial of autologous bone marrow transplantation and chemotherapy in multiple myeloma. Intergroupe Francais du Myelome. N Engl J Med 1996; 335: 91–97.
Goldschmidt H, Hegenbart U, Wallmeier M et al. Peripheral blood progenitor cell transplantation in multiple myeloma following high-dose melphalan-based therapy. Recent Results Cancer Res 1998; 144: 27–35.
Attal M, Harousseau JL . Standard therapy versus autologous transplantation in multiple myeloma. Hematol Oncol Clin N Am 1997; 11: 133–146.
Child JA, Morgan GJ, Davies FE et al. High-dose chemotherapy with hematopoietic stem-cell rescue for multiple myeloma. N Engl J Med 2003; 348: 1875–1883.
Demirer T, Buckner CD, Gooley T et al. Factors influencing collection of peripheral blood stem cells in patients with multiple myeloma. Bone Marrow Transplant 1996; 17: 937–941.
Billadeau D, Quam L, Thomas W et al. Detection and quantitation of malignant cells in the peripheral blood of multiple myeloma patients. Blood 1992; 80: 1818–1824.
Goldschmidt H, Hegenbart U, Wallmeier M et al. Factors influencing collection of peripheral blood progenitor cells following high-dose cyclophosphamide and granulocyte colony-stimulating factor in patients with multiple myeloma. Br J Haematol 1997; 98: 736–744.
Vescio RA, Han EJ, Schiller GJ et al. Quantitative comparison of multiple myeloma tumor contamination in bone marrow harvest and leukapheresis autografts. Bone Marrow Transplant 1996; 18: 103–110.
McCann JC, Kanteti R, Shilepsky B et al. High degree of occult tumor contamination in bone marrow and peripheral blood stem cells of patients undergoing autologous transplantation for non-Hodgkin's lymphoma. Biol Blood Marrow Transplant 1996; 2: 37–43.
Henry JM, Sykes PJ, Brisco MJ et al. Comparison of myeloma cell contamination of bone marrow and peripheral blood stem cell harvests. Br J Haematol 1996; 92: 614–619.
Schiller G, Vescio R, Freytes C et al. Autologous CD34-selected blood progenitor cell transplants for patients with advanced multiple myeloma. Bone Marrow Transplant 1998; 21: 113–115.
Stewart AK, Vescio R, Schiller G et al. Purging of autologous peripheral-blood stem cells using CD34 selection does not improve overall or progression-free survival after high-dose chemotherapy for multiple myeloma: results of a multicenter randomized controlled trial. J Clin Oncol 2001; 19: 3771–3779.
Attal M, Harousseau JL, Facon T et al. Single versus double autologous stem-cell transplantation for multiple myeloma. N Engl J Med 2003; 349: 2495–2502.
Gertz MA, Witzig TE, Pineda AA et al. Monoclonal plasma cells in the blood stem cell harvest from patients with multiple myeloma are associated with shortened relapse-free survival after transplantation. Bone Marrow Transplant 1997; 19: 337–342.
Sharp JG, Kessinger A, Mann S et al. Outcome of high-dose therapy and autologous transplantation in non-Hodgkin's lymphoma based on the presence of tumor in the marrow or infused hematopoietic harvest. J Clin Oncol 1996; 14: 214–219.
Zhou P, Zhang Y, Martinez C et al. Melphalan-mobilized blood stem cell components contain minimal clonotypic myeloma cell contamination. Blood 2003; 102: 477–479.
Zwicky CS, Maddocks AB, Andersen N, Gribben JG . Eradication of polymerase chain reaction detectable immunoglobulin gene rearrangement in non-Hodgkin's lymphoma is associated with decreased relapse after autologous bone marrow transplantation. Blood 1996; 88: 3314–3322.
Dreyfus F, Ribrag V, Leblond V et al. Detection of malignant B cells in peripheral blood stem cell collections after chemotherapy in patients with multiple myeloma. Bone Marrow Transplant 1995; 15: 707–711.
McQuaker IG, Haynes AP, Anderson S et al. Engraftment and molecular monitoring of CD34+ peripheral-blood stem-cell transplants for follicular lymphoma: a pilot study. J Clin Oncol 1997; 15: 2288–2295.
Cremer FW, Kiel K, Wallmeier M et al. A quantitative PCR assay for the detection of low amounts of malignant cells in multiple myeloma. Ann Oncol 1997; 8: 633–636.
Martinelli G, Terragna C, Lemoli RM et al. Clinical and molecular follow-up by amplification of the CDR-III IgH region in multiple myeloma patients after autologous transplantation of hematopoietic CD34 stem cells. Haematologica 1999; 84: 397–404.
Kyle RA, Pierre RV, Bayrd ED . Multiple myeloma and acute myelomonocytic leukemia. N Engl J Med 1970; 283: 1121–1125.
Kyle RA, Pierre RV, Bayrd ED . Multiple myeloma and acute leukemia associated with alkylating agents. Arch Intern Med 1975; 135: 185–192.
Arbuck SG, Ivy SP, Setser A et al. The Revised Common Toxicity Criteria: Version 2.0. CTEP Website. http://ctep.info.nih.gov.
Trotti A, Byhardt R, Stetz J et al. Common toxicity criteria: version 2.0, an improved reference for grading the acute effects of cancer treatment: impact on radiotherapy. Int J Radiat Oncol Biol Phys 2000; 47: 13–47.
Comenzo RL, Wally J, Kica G et al. Clonal immunoglobulin light chain variable region germline gene use in AL amyloidosis: association with dominant amyloid-related organ involvement and survival after stem cell transplantation. Br J Haematology 1999; 106: 744–751.
Willems P, Verhagen O, Segeren C et al. Consensus strategy to quantitate malignant cells in myeloma patients is validated in a multicenter study. Blood 2000; 96: 63–70.
Comenzo RL, Zhang Y, Martinez C et al. The tropism of organ involvement in primary systemic amyloidosis: contributions of Ig VL germline gene use and plasma cell burden. Blood 2001; 98: 714–720.
Cremer FW, Kiel K, Wallmeier M et al. Leukapheresis products in multiple myeloma: lower tumor load after mobilization with cyclophosphamide plus granulocyte colony-stimulating factor (G-CSF) compared with G-CSF alone. Exp Hematol 1998; 26: 969–975.
Kiel K, Cremer FW, Ehrbrecht E et al. First and second apheresis in patients with multiple myeloma: no differences in tumor load and hematopoietic stem cell yield. Bone Marrow Transplantation 1998; 21: 1109–1115.
Cremer FW, Ehrbrecht E, Kiel K et al. Evaluation of the kinetics of the bone marrow tumor load in the course of sequential high-dose therapy assessed by quantitative PCR as a predictive parameter in patients with multiple myeloma. Bone Marrow Transplant 2000; 26: 851–858.
Comenzo RL, Michelle D, LeBlanc M et al. Mobilized CD34+cells selected as autografts in patients with primary light-chain amyloidosis: rationale and application. Transfusion 1998; 38: 60–69.
Rosner B . Hypothesis Testing: Categorical Data. Fundamentals of Biostatistics. Wadsworth: Belmont, CA, 1994, pp 345–442.
McElwain TJ, Powles RL . High-dose intravenous melphalan for plasma-cell leukaemia and myeloma. Lancet 1983; 2: 822–824.
Selby PJ, McElwain TJ, Nandi AC et al. Multiple myeloma treated with high dose intravenous melphalan. Br J Haematol 1987; 66: 55–62.
Lokhorst HM, Sonneveld P, Wijermans PW et al. Intermediate-dose melphalan (IDM) combined with G-CSF (filgrastim) is an effective and safe induction therapy for autologous stem cell transplantation in multiple myeloma. Br J Haematol 1996; 92: 44–48.
Lokhorst HM, Sonneveld P, Cornelissen JJ et al. Induction therapy with vincristine, adriamycin, dexamethasone (VAD) and intermediate-dose melphalan (IDM) followed by autologous or allogeneic stem cell transplantation in newly diagnosed multiple myeloma. Bone Marrow Transplant 1999; 23: 317–322.
Henon P, Donatini B, Eisenmann JC et al. Comparative survival, quality of life and cost-effectiveness of intensive therapy with autologous blood cell transplantation or conventional chemotherapy in multiple myeloma. Bone Marrow Transplant 1995; 16: 19–25.
Moreau P, Milpied N, Mahe B et al. Melphalan 220 mg/m2 followed by peripheral blood stem cell transplantation in 27 patients with advanced multiple myeloma. Bone Marrow Transplant 1999; 23: 1003–1006.
Carstanjen D, Regenfus M, Muller C, Salama A . Interleukin-6 is a major effector molecule of short-term G-CSF treatment inducing bone metabolism and an acute-phase response. Exp Hematol 2001; 29: 812–821.
Dhodapkar MV, Osman K, Teruya-Feldstein J et al. Expression of cancer/testis (CT) antigens MAGE-A1, MAGE-A3, MAGE-A4, CT-7, and NY-ESO-1 in malignant gammopathies is heterogeneous and correlates with site, stage and risk status of disease. Cancer Immunity 2003; 23: 3:9–3:17.
Barlogie B, Shaughnessy JD, Tricot G et al. Treatment of multiple myeloma. Blood 2004; 103: 20–32.
Morris CL, Siegel E, Barlogie B et al. Mobilization of CD34+ cells in elderly patients (⩾70 years) with multiple myeloma: influence of age, prior therapy, platelet count and mobilization regimen. Br J Haematol 2003; 120: 413–423.
Gertz MA, Lacy MQ, Inwards DJ et al. Delayed stem cell transplantation for the management of relapsed or refractory multiple myeloma. Bone Marrow Transplant 2000; 26: 45–50.
Acknowledgements
We thank the MSKCC Cytotherapy Laboratory for assistance with stem cell samples and the Memorial Hospital nurses in the Adult Day Hospital and in-patient services who cared for our patients. This work was supported by NIH Grant CA05826, FDA Grant R01-002174-02 (RLC), the Graziano Fund, the Multiple Myeloma Research Foundation, the Mel Stottlemyre Myeloma Research Fund, the Donald Stein Myeloma Research Fund, the Werner and Elaine Dannheiser Fund for Research on the Biology of Aging of the Lymphoma Foundation, and Amgen.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gupta, S., Zhou, P., Hassoun, H. et al. Hematopoietic stem cell mobilization with intravenous melphalan and G-CSF in patients with chemoresponsive multiple myeloma: report of a phase II trial. Bone Marrow Transplant 35, 441–447 (2005). https://doi.org/10.1038/sj.bmt.1704779
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1704779
This article is cited by
-
Circulating biosignatures in multiple myeloma and their role in multidrug resistance
Molecular Cancer (2023)
-
Improving stem cell mobilization strategies: future directions
Bone Marrow Transplantation (2009)
-
Bendamustine, but not fludarabine, exhibits a low stem cell toxicity in vitro
Journal of Cancer Research and Clinical Oncology (2009)
-
Results of a phase I/II trial adding carmustine (300 mg/m2) to melphalan (200 mg/m2) in multiple myeloma patients undergoing autologous stem cell transplantation
Leukemia (2006)