Summary:
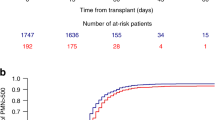
The outcomes of patients who experience the failure to reconstitute a trilineage of blood cells after initial neutrophil engraftment were evaluated in 178 patients with hematologic disorders, who underwent allogeneic HCT. Of 165 qualified patients (five with primary engraftment failure; eight deaths before day 60 of HCT), 43 (26%) satisfied the criteria for the initial (n=22; failure of platelet >20 000/μl or red blood cell transfusion independence/reticulocyte count ⩾1.0% by day 60) or subsequent (n=21, ANC <500/μl for ⩾3 days, platelet <20 000/μl for ⩾7 days, or red blood cells transfusion/reticulocyte <1.0% after initial trilineage reconstitution) failure. GVHD was the most common clinical condition associated with cytopenia (n=24). In all, 20 patients (47%) recovered at least partially with a median of 52 days (range 8–323) later, with 12 of those 20 patients recovering completely. The eventual reconstitution failure rate was 14% (23/163 patients). The number of cell lineages involved in the cytopenia was the only independent variable that predicted partial recovery (1 lineage vs 2–3 lineages with odds ratio of 8.69 (95% CI 1.96–38.60), P=0.004). Five/20 patients with vs 20/23 patients without partial recovery died. Trilineage reconstitution failures after allogeneic HCT need systematic analysis in the future studies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Thomas ED . Marrow transplantation for malignant diseases. J Clin Oncol 1983; 1: 517–531.
Dubovsky J, Daxberger H, Fritsch G et al. Kinetics of chimerism during the early post-transplant period in pediatric patients with malignant and non-malignant hematologic disorders: implications for timely detection of engraftment, graft failure and rejection. Leukemia 1999; 13: 2060–2069.
Nemunaitis J, Singer JW, Buckner CD et al. Use of recombinant human granulocyte-macrophage colony-stimulating factor in graft failure after bone marrow transplantation. Blood 1990; 76: 245–253.
Grandage VL, Cornish JM, Pamphilon DH et al. Second allogeneic bone marrow transplantation from unrelated donors for graft failure following initial unrelated donor bone marrow transplantation. Bone Marrow Transplant 1998; 21: 687–690.
Urbano-Ispizua A, Rozman C, Pimentel P et al. The number of donor CD3+ cells is the most important factor for graft failure after allogeneic transplantation of CD34+ selected cells from peripheral blood from HLA-identical siblings. Blood 2001; 97: 383–387.
Champlin RE, Horowitz MM, van Bekkum DW et al. Graft failure following bone marrow transplantation for severe aplastic anemia: risk factors and treatment results. Blood 1989; 73: 606–613.
Ho VT, Soiffer RJ . The history and future of T-cell depletion as graft-versus-host disease prophylaxis for allogeneic hematopoietic stem cell transplantation. Blood 2001; 98: 3192–3204.
Lee J-H, Lee K-H, Kim S et al. Relevance of proteins C and S, antithrombin III, von Willebrand factor, and factor VIII for the development of hepatic veno-occlusive disease in patients undergoing allogeneic bone marrow transplantation: a prospective study. Bone Marrow Transplant 1998; 22: 883–888.
Deeg HJ, Storb R . Graft-versus-host disease: pathophysiological and clinical aspects. Ann Rev Med 1984; 35: 11–24.
Wang F-Z, Dahl H, Linde A et al. Lymphotropic herpesviruses in allogeneic bone marrow transplantation. Blood 1996; 88: 3615–3620.
Lee J-H, Lee J-H, Choi S-J et al. Changes of isoagglutinin titres after ABO-incompatible allogeneic stem cell transplantation. Br J Hematol 2003; 120: 702–710.
Lee J-H, Lee K-H, Lee J-H et al. Plasminogen activator inhibitor-1 is an independent diagnostic marker as well as severity predictor of hepatic veno-occlusive disease after allogeneic bone marrow transplantation in adults conditioned with busulphan and cyclophosphamide. Br J Haematol 2002; 118: 1087–1094.
Lee K-H, Lee J-H, Lee J-H et al. Non-myeloablative conditioning regimen of fludarabine, busulfan, anti-thymocyte globulin, and methylprednisolone for allogeneic peripheral blood hematopoietic cell transplantation. Haematologica 2001; 86: 999–1001.
Przepiorka D, Weisdorf D, Martin P et al. Meeting report. Consensus conference on acute GVHD grading. Bone Marrow Transplant 1995; 15: 825–828.
Sullivan K . Acute and chronic graft-versus-host disease in man. Int J Cell Clon 1986; 4: 42–93.
McDonald GB, Hinds MS, Fisher LD et al. Veno-occlusive disease of the liver and multiorgan failure after bone marrow transplantation: a cohort study of 355 patients. Ann Intern Med 1993; 118: 255–267.
Lee K-H, Lee J-H, Choi S-J et al. Monthly prospective analysis of hematopoietic chimerism after allogeneic hematopoietic cell transplantation. Bone Marrow Transplant 2003; 32: 423–431.
Bacigalupo A, Hows J, Gluckman E et al. Bone marrow transplantation (BMT) versus immunosuppression for the treatment of severe aplastic anemia (SAA): a report of the EBMT SAA working party. Br J Haematol 1988; 70: 177–182.
Frickhofen N, Rosenfeld SJ . Immunosuppressive treatment of aplastic anemia with antithymocyte globulin and cyclosporine. Semin Hematol 2000; 37: 56–68.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, KH., Lee, JH., Choi, SJ. et al. Failure of trilineage blood cell reconstitution after initial neutrophil engraftment in patients undergoing allogeneic hematopoietic cell transplantation – frequency and outcomes. Bone Marrow Transplant 33, 729–734 (2004). https://doi.org/10.1038/sj.bmt.1704428
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1704428
Keywords
This article is cited by
-
Therapy of posttransplant poor graft function with eltrombopag
Bone Marrow Transplantation (2021)
-
Efficacy and cost analysis of eltrombopag in thrombocytopenia and poor graft function post allogeneic hematopoietic cell transplantation
Bone Marrow Transplantation (2021)
-
Eltrombopag for the treatment of poor graft function following allogeneic stem cell transplant: a retrospective multicenter study
International Journal of Hematology (2021)
-
Eltrombopag: Role in Cytopenias Following Hematopoietic Stem Cell Transplantation
Indian Journal of Hematology and Blood Transfusion (2020)
-
Eltrombopag for post-transplant cytopenias due to poor graft function
Bone Marrow Transplantation (2019)