Abstract
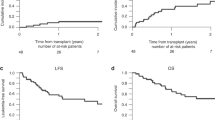
Reinforced chemotherapy based on a double high-dose consolidation regimen could be a different way to enhance in vivo purging prior to autologous stem cell transplantation (auto-SCT) in acute myeloid leukemia (AML). We investigated the impact on outcome of auto-SCT after two different strategies of early intensification performed after an identical induction regimen in adult patients with AML. Between January 1993 and December 1998, 140 consecutive AML patients were enrolled in a program consisting of an identical anthracycline-based induction (ICE) and two different consolidation regimens: one cycle, cytarabine-based (single-NOVIA: 91 patients); two cycles, fludarabine-based (double-FLAN: 49 patients). Seventy out of 91 patients received single-NOVIA consolidation: 60 underwent a transplantation procedure (allogeneic bone marrow transplantation (allo-BMT):16 patients; auto-SCT: 44). Thirty-five out of 49 patients received double-FLAN consolidation: 31 underwent a transplantation procedure (allo-BMT: 10; auto-SCT: 21). The double consolidation regimen was well-tolerated with only minor side-effects. Median follow-up observation time for surviving patients was 38 months (range, 17–71) for the double-FLAN consolidation group and 70 months (range: 48–93) for the single-NOVIA consolidation group. Among the patients who received auto-SCT, the double consolidation strategy produced a superior disease-free survival curve at 36 months (78.6% (95%CI: 59.4–97.8) vs 47.7% (95%CI: 33–62.4)) compared with the single-NOVIA group. This difference was confirmed when the patients were analyzed for intention to treat (P = 0.04). In addition, the double-FLAN consolidation group showed a superior overall survival and lower relapse rate (P = 0.02). We conclude that the double-FLAN reinforcement strategy is safe and enhances the clinical impact of auto-SCT for AML patients in first complete remission. It may provide specific clinical benefit for patients undergoing auto-SCT. Bone Marrow Transplantation (2001) 27, 829–835.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Zittoun RA, Mandelli F, Willemze R et al. Autologous or allogeneic bone marrow transplantation compared with intensive chemotherapy in acute myelogenous leukemia New Engl J Med 1995 332: 217–233
Mayer RJ, Davis RB, Schiffer CA et al. Intensive postremission chemotherapy in adults with acute myeloid leukemia New Engl J Med 1994 331: 896–903
Gorin NC, Dicke K, Lowenberg B et al. High dose therapy for acute myelocytic leukemia treatment strategy: what is the choice? Ann Oncol 1995 4: (Suppl. 1) 59–80
Lowenberg B, Verdonck LJ, Dekker W et al. Autologous bone marrow transplantation in acute myeloid leukemia in first remission: results of a Dutch prospective study J Clin Oncol 1994 8: 287–294
Burnett AK, Goldstone AH, Stevens RMF et al. Randomized comparison of addition of autologous bone-marrow transplantation to intensive chemotherapy for acute myeloid leukemia in first remission: results of MRC AML 10 trial Lancet 1998 351: 700–709
Visani G, Lemoli RM, Tosi P et al. Use of peripheral blood stem cells for autologous transplantation in acute myeloid leukemia patients allows faster engraftment and equivalent disease-free survival compared with bone marrow cells Bone Marrow Transplant 1999 24: 467–472
Mehta J, Powles R, Singhal S et al. Peripheral blood stem cell transplantation may result in increased relapse of acute myeloid leukemia due to reinfusion of a higher number of malignant cells Bone Marrow Transplant 1995 15: 652–653
Laporte JP, Gorin NC, Feuchtenbaum J et al. Relapse after autografting with peripheral blood stem cells Lancet 1997 2: 1993–1999
Schiller G, Lee M, Miller T et al. Transplantation of autologous peripheral blood progenitor cells procured after high dose cytarabine based consolidation chemotherapy for adults with acute myelogenous leukemia in first remission Leukemia 1997 11: 1533–1539
Schlenk RF, Dohner H, Pforsich M et al. Successful collection of peripheral blood progenitor cells in patients with acute myeloid leukemia following early consolidation therapy with granulocyte colony-stimulating factor-supported high-dose cytarabine and mitoxantrone Br J Haematol 1997 99: 386–393
Martin C, Torres A, Leon A et al. Autologous peripheral blood stem cell transplantation mobilized with G-CSF in AML in first complete remission. Role of intensification therapy in outcome Bone Marrow Transplant 1998 21: 375–382
Visani G, Tosi P, Zinzani PL et al. FLAG (Fludarabine + high dose ara-C + G-CSF): an effective and tolerable protocolfor the treatment of ‘poor risk’ acute myeloid leukemias Leukemia 1994 8: 1842–1846
Estey E, Thall P, Andreeff M et al. Use of granulocyte colony-stimulating factor before, during and after fludarabine plus cytarabine induction therapy of newly diagnosed acute myelogenous leukemia or myelodysplastic syndromes: comparison with fludarabine plus cytarabine without granulocyte colony-stimulating factor J Clin Oncol, 1994 12: 671–678
Clavio M, Carrara P, Miglino M et al. High efficacy of fludarabine containing therapy (FLAG-FLANG) in poor risk acute myeloid leukemia Haematologica 1996 81: 513–520
Bennet JM, Catovsky DM, Daniel MT et al. Proposals for the classification of acute leukemias Br J Haematol, 1977 33: 451–458
Cheson BD, Cassileth PA, Head DR et al. Report of National Cancer Institute-sponsored workshop on definitions of diagnosis and response in acute myeloid leukemia J Clin Oncol 1990 8: 813–819
Lemoli RM, Visani G, Leopardi G et al. Autologous transplantation of chemotherapy-purged PBSC collection from high-risk leukemia patients: a pilot study Bone Marrow Transplant, 1999 23: 235–241
Carella AM, Dejana A, Lerma E et al. In vivo mobilization of karyotypically normal peripheral blood progenitor cells in high-risk MDS, secondary or therapy related acute myelogenous leukemia Br J Haematol 1996 95: 127–130
Visani G, Lemoli RM, Tosi P et al. Fludarabine containing-regimens severely impair peripheral blood stem cells mobilization and collection in acute myeloid leukemia patients Br J Haematol 1999 105: 775–779
Miggiano MC, Gherlinzoni F, Rosti G et al. Autologous bone marrow transplantation in late first complete remission improves outcome in acute myelogenous leukemia Leukemia 1996 10: 402–409
Lemoli RM, Fortuna A, Motta MR et al. Concomitant mobilization of plasma cells and haemopoietic progenitors into peripheral blood of multiple myeloma patients: positive selection and transplantation of enriched CD34+ cells to remove circulating tumor cells Blood 1996 87: 1625–1634
Testoni N, Lemoli RM, Martinelli G et al. Autologous PBSCT in acute myeloblastic leukemia and MDS. Evaluation of tumor cell contamination of leukapheresis by cytogenetic and molecular methods Bone Marrow Transplant 1998 22: 1065–1070
Sanz MA, de la Rubia J, Sanz G et al. Busulphan and cyclophosphamide followed by complete remission: a report from a single institution J Clin Oncol 1993 11: 1661–1667
Kaplan EL, Meier P . Non-parametric estimation from incomplete observation J Am Stat Assoc 1958 53: 457–481
Peto R, Pike MC, Armitage NE . Design and analysis of randomized clinical trials requiring prolonged observation of each patient. Part II. Analysis and examples Br J Cancer 1977 35: 1–39
Cassileth PA, Andersen J, Lazarus HM et al. Autologous bone marrow transplantation in acute myeloid leukemia in first remission J Clin Oncol 1993 11: 314–319
Demirer T, Petersen FB, Bensinger WI et al. Autologous transplantation with peripheral blood stem cells collected after granulocyte colony-stimulating factor in patients with acute myelogenous leukemia Bone Marrow Transplant 1996 18: 29–34
Reiffers J, Korbling M, Labopin M et al. Autologous blood stem cell transplantation versus autologous bone marrow transplantation for acute myeloid leukemia in first complete remission J Cell Cloning 1992 7: (Suppl. 1) 111–113
Labopin M, Gorin NC, Ringden O et al. Autologous bone marrow transplantation in 2502 patients with acute leukemia in Europe: a retrospective study Leukemia 1992 6: (Suppl. 4) 95–99
Korbling M, Hunstein W, Fliedner TM et al. Disease-free survival after autologous bone marrow transplantation in patients with acute myelogenous leukemia Blood 1989 74: 1898–1904
McMillan AK, Goldstone AH, Linch DC et al. High-dose chemotherapy and autologous bone marrow transplantation in acute myeloid leukemia Blood 1990 76: 480–488
To LB, Roberts MM, Haylock DN et al. Comparison of hematological recovery times and supportive care requirements of autologous recovery phase peripheral blood stem cell transplants, autologous bone marrow transplants and allogeneic bone marrow transplants Bone Marrow Transplant 1992 9: 277–284
Visani G, Di Nota A, Tosi P et al. Cryopreserved autologous bone marrow transplantation in patients with acute nonlymphoid leukemia: chemotherapy before harvesting is the main factor in delaying the hematological recovery Cryobiology 1990 27: 103–106
Motta RM, Mangianti S, Rizzi S et al. Pharmacological purging of minimal residual disease from peripheral blood stem cell collections of acute myeloblastic leukemia patients: preclinical studies Exp Hematol 1997 25: 1261–1269
Korbling M, Fliedner TM, Holle R et al. Autologous blood stem cell (ABSCT) versus purged bone marrow transplantation (ABMT) in standard risk AML: influence of source and cell composition of the autograft on haemopoietic reconstitution and disease-free survival Bone Marrow Transplant 1991 7: 343–349
Gondo H, Harada M, Miyamoto T et al. Autologous peripheral blood stem cell transplantation for acute myelogenous leukemia Bone Marrow Transplant 1997 20: 821–826
Vellenga E, van Putten WL, Bogaerts MA et al. Peripheral blood stem cell transplantation as an alternative to autologous marrow transplantation in the treatment of acute myeloid leukemia Bone Marrow Transplant 1999 23: 343–349
Acknowledgements
This work was supported in part by MURST ex 40% (S Tura) and MURST ex 60% (S Tura).
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Visani, G., Lemoli, R., Isidori, A. et al. Double reinforcement with fludarabine/high-dose cytarabine enhances the impact of autologous stem cell transplantation in acute myeloid leukemia patients. Bone Marrow Transplant 27, 829–835 (2001). https://doi.org/10.1038/sj.bmt.1703003
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1703003