Abstract
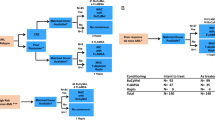
Forty-five patients with metastatic breast cancer without clinically evident disease were treated with thiotepa 750 mg/m2, mitoxantrone 40 mg/m2 and carboplatin 1000 mg/m2 followed by stem cell transplantation to determine the safety and efficacy of CD34+ selection of peripheral blood stem cells. Of these, 15 patients’ (group I) stem cells were processed through Baxter Isolex 300 device for CD34+ selection, whereas 30 patients (group II) received unmanipulated stem cells. Toxicity, progression-free survival and survival were compared between these two groups. There was no difference in transfusion requirements, white cell count and platelet recovery and non-hematologic toxicity between the two groups. The survival of patients in group I was 27 months compared to 38 months in group II (P = 0.8). The progression-free survival was 12 months and 13.5 months for group I and group II patients, respectively (P = 0.6). Our results indicate that while there is no adverse effect, there is also no significant advantage of CD34+ selection in terms of progression-free survival and survival in patients with metastatic breast cancer without clinically evident disease. Bone Marrow Transplantation (2000) 25, 1041–1045.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Antman KH, Rowlings PA, Vaughan-WP et al. High-dose chemotherapy with autologous hematopoietic stem-cell support for breast cancer in North America J Clin Oncol 1997 15: 1870–1879
Demirer T, Buckner CD, Appelbaum FR et al. High-dose busulfan and cyclophosphamide followed by autologous transplantation in patients with advanced breast cancer Bone Marrow Transplant 1996 17: 769–774
Cameron DA, Craig J, Gabra H et al. High-dose chemotherapy supported by peripheral blood progenitor cells in poor prognosis metastatic breast cancer – phase I/II study. Edinburgh Breast Group Br J Cancer 1996 74: 2013–2017
Bezwoda WR, Seymour L, Dansey RD . High dose chemotherapy with hematopoietic rescue as primary treatment for metastatic breast cancer: a randomized trial J Clin Oncol 1995 13: 2483–2489
Laport GF, Grad G, Grinblatt DL et al. High-dose chemotherapy consolidation with autologous stem cell rescue in metastatic breast cancer: a 10 year experience Bone Marrow Transplant 1998 21: 127–132
Bensinger WI, Schiffman KS, Holmberg L et al. High dose busulfan, melphalan, thiotepa and peripheral blood stem cell infusion for the treatment of metastatic breast cancer Bone Marrow Transplant 1997 19: 1183–1189
Razis ED, Samonis G, Cook P et al. TMJ: a well-tolerated high-dose regimen for the adjuvant chemotherapy of high risk breast cancer J Med 1994 25: 241–250
Brenner M . Gene marking Hum Gene Ther 1996 7: 1927–1936
Moss TJ . Tumor contamination in stem cell products from patients with neuroblastoma and breast cancer Bone Marrow Transplant 1996 18: (Suppl 1) S17
Sharp JG, Kessinger A, Mann S et al. Outcome of high-dose therapy and autologous transplantation in non-Hodgkin's lymphoma based on the presence of tumor in the marrow or infused hematopoietic harvest J Clin Oncol 1996 14: 214–219
Ross AA, Cooper BW, Lazarus HM et al. Detection and viability of tumor cells in peripheral blood stem cell collections from breast cancer patients using immunocytochemical and clonogenic assay techniques Blood 1993 182: 2605–2610
Farley TJ, Preti RA, Barton MK et al. The prognostic value of immunocytochemical testing for contaminating breast carcinoma cells: an analysis of infused stem cell products in patients with inflammatory and metastatic breast cancer J Clin Oncol (in press)
Cooper BW, Moss TJ, Ross AA et al. Occult tumor contamination of hematopoietic stem-cell products does not affect clinical outcome of autologous transplantation in patients with metastatic breast cancer J Clin Oncol 1998 16: 3509–3517
Weaver CH, Moss T, Schwartzberg LS et al. High dose chemotherapy in patients with breast cancer: evaluation of infusing peripheral blood stem cells containing occult tumor cells Bone Marrow Transplant 1998 21: 1117–1124
Saarinen UM, Coccia PF, Gerson SL et al. Eradication of neuroblastoma cells in vitro by monoclonal antibody and human complement: method for purging autologous bone marrow Cancer Res 1985 45: 5969–5975
Ben Yosef R, Or R, Naparstek E et al. Should soybean agglutinin purging be performed in breast cancer patients undergoing autologous stem cell transplantation? A retrospective analysis of 48 patients Am J Clin Oncol 1997 20: 419–423
Mapara MY, Korner IJ, Hildebrandt M et al. Monitoring of tumor cell purging after highly efficient immunomagnetic selection of CD34 cells from leukapheresis products in breast cancer patients: comparison of immunocytochemical tumor cell staining and reverse transcriptase-polymerase chain reaction Blood 1997 89: 337–344
Shpall EJ, Jones RB, Bearman SI et al. Transplantation of enriched CD34-positive autologous marrow into breast cancer patients following high-dose chemotherapy: influence of CD34-positive peripheral-blood progenitors and growth factors on engraftment J Clin Oncol 1994 12: 28–36
Farley TJ, Ahmed T, Fitzgerald M et al. Optimization of CD34+ cell selection using immunomagnetic beads: implications for use in cryopreserved peripheral blood stem cell collections J Hematother 1997 6: 53–60
Stiff PJ, Koester AR, Weidner MK et al. Autologous bone marrow transplantation using unfractionated cells cryopreserved in dimethylsulfoxide and hydroxyethyl starch without controlled-rate freezing Blood 1987 70: 974–978
Ross AA, Loudovaris M, Hazelton B et al. Immunocytochemical analysis of tumor cells in pre- and post-culture peripheral blood progenitor cell collections from breast cancer patients Exp Hematol 1995 14: 1478–1483
Antman K, Ayash L, Elias A et al. A phase II study of high dose cyclophosphamide, thiotepa, and carboplatin with autologous marrow support in women with measurable advanced breast cancer responding to standard-dose therapy J Clin Oncol 1992 10: 102–110
Gisselbrecht C, Extra JM, Lotz JP et al. Cyclophos-phamide/mitoxantrone/melphalan (CMA) prior to autologous bone marrow transplantation (ABMT) in metastatic breast cancer Bone Marrow Transplant 1996 18: 857–863
Klump TR, Goldberg SL, Magdalinski AJ, Mangan KF . Phase II study of high-dose cyclophosphamide, etoposide, and carboplatin (CEC) followed by autologous hematopoietic stem cell rescue in women with metastatic or high risk non metastatic breast cancer: multivariate analysis of factors affecting survival and engraftment Bone Marrow Transplant 1997 20: 273–281
Peters WP, Shpall EJ, Jones RB et al. High-dose combination alkylating agents with bone marrow support as initial treatment for metastatic breast cancer J Clin Oncol 1988 6: 1368–1376
Holland HK, Dix SP, Geller RB et al. Minimal toxicity and mortality in high risk breast cancer patients receiving high-dose cyclophosphamide, thiotepa, and carboplatin plus autologous marrow/stem cell transplantation and comprehensive supportive care J Clin Oncol 1996 4: 1156–1164
Kalacioglu ME, Lichtin AE, Andersen SW et al. High dose busulfan and cyclophosphamide followed by autologous bone marrow transplantation and/or peripheral blood progenitor cell rescue for metastatic breast cancer Am J Oncol 1995 18: 491–494
Vaughan WP, Reed EC, Edwards B et al. High dose cyclophosphamide, thiotepa, and hydroxyureas with autologous hematopoietic stem cell rescue: an effective consolidation chemotherapy regimen for early metastatic breast cancer Bone Marrow Transplant 1994 13: 619–624
Todd NW, Peters WP, Ost AH et al. Pulmonary drug toxicity in patients with primary breast cancer treated with high-dose combination chemotherapy and autologous bone marrow transplantation Am Rev Resp Dis 1993 147: 1264–1270
Stadtmauer EA, O'Neill A, Goldstein LJ et al. Phase III randomized trial of high-dose chemotherapy (HDC) and stem cell support (SCT) shows no difference in overall survival or severe toxicity compared to maintenance chemotherapy with cyclophosphamide, methotrexate, and 5-fluorouracil (CMF) for women with metastatic breast cancer who are responding to conventional induction chemotherapy: the ‘Philadelphia’ Intergroup Study (PBT-1) Proc ASCO 1999 18: 1a (Abstr. 1)
Acknowledgements
This work was supported in part by the Baxter Corporation. We thank Albert Hoang for statistical analysis. We also thank the nursing staff, physician assistants, and fellows for providing excellent care to our patients.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Ahmed, T., Kancherla, R., Qureshi, Z. et al. High-dose chemotherapy and stem cell transplantation for patients with stage IV breast cancer without clinically evident disease: correlation of CD34+ selection to clinical outcome. Bone Marrow Transplant 25, 1041–1045 (2000). https://doi.org/10.1038/sj.bmt.1702374
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1702374
Keywords
This article is cited by
-
High-dose therapy in patients with Hodgkin's disease: the use of selected CD34+ cells is as safe as unmanipulated peripheral blood progenitor cells
Bone Marrow Transplantation (2001)
-
High-dose chemotherapy and CD34-selected peripheral blood progenitor cell transplantation for patients with breast cancer metastatic to bone and/or bone marrow
Bone Marrow Transplantation (2001)
-
The potential of marrow stromal cells in stem cell therapy
Eye (2001)