Abstract
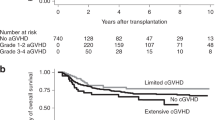
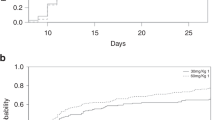
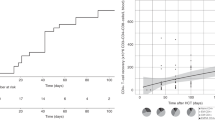
We investigated early immunological reconstitution and the production of circulating inflammatory mediators and their relationship to aGVHD in children during the first 100 days following unrelated UCBT. Nine patients had an underlying malignant disease (ALL, ANLL), and two, non-malignant diseases (SAA, ALD). The median age was 10 years (range: 1.25–21). Seven of 11 patients were alive by day 100, two died from regimen-related toxicity, and two died from severe aGVHD (grade ⩾III). Myeloid engraftment (ANC ⩾500/mm3 × 2 days) occurred at a median of 24 days (range: 14–55), while platelet engraftment (platelet count ⩾20 000/mm3untransfused × 7 days) was delayed and occurred at a median of 52 days (range: 33–95). The mean cell dose of CD34+ cells was 3.3 ± 3.51 × 105/kg, and of CD34+/CD41+ cells was 3.94 ± 3.99 × 104/kg. Acute GVHD (grade II–IV) developed in seven patients (77%), and severe aGVHD (grade III–IV) developed in five patients (55%). Serum levels of IL-2Rα, IL-2, IL-4, IL-7, IL-12, and IFNγ were not significantly different between patients with grades 0–I aGVHD and patients with grades II–IV aGVHD. Evaluation of immunological reconstitution on day 90 post UCBT demonstrated an early recovery of the absolute numbers of B cells (CD19+) and NK cells (CD3−/CD56+). Immunoglobulin levels for IgG, IgM and IgA remained normal throughout the study period. PMN functional studies demonstrated normal superoxide generation, bacterial killing (BK), and chemotaxis (CTX). However, both helper (CD3+/CD4+) and suppressor (CD3+/CD8+) T cell subsets remained low during the first 100 days post UCBT with mean ± s.e.m. values of 120 ± 29/mm3 and 10 ± 50/mm3, respectively (normal = 900–2860/mm3 (CD3/CD4), normal = 630–1910/mm3 (CD3/CD8)). Mitogen response studies showed low blastogenesis to PHA and PWM, with a mean c.p.m. ± s.e.m. value of 1.7 ± 0.67 × 104 for PHA (NL ⩾ 75 × 103) and 8.42 ± 4.1 × 103 for PWM (NL ⩾25 × 103). In conclusion, serum levels of inflammatory mediators were not predictive nor did they correlate with the severity of aGVHD. Recovery of NK cells, B cells, and PMN functions occurred within the first 90 days post transplant. However, T cell subsets, CD3+/CD4+ and CD3+/CD8+, and T cell functional activity remained significantly decreased and may account for the high incidence of infectious morbidity seen during this immediate post UCBT period.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Abu-Ghosh, A., Goldman, S., Slone, V. et al. Immunological reconstitution and correlation of circulating serum inflammatory mediators/cytokines with the incidence of acute graft-versus-host disease during the first 100 days following unrelated umbilical cord blood transplantation. Bone Marrow Transplant 24, 535–544 (1999). https://doi.org/10.1038/sj.bmt.1701921
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1701921
Keywords
This article is cited by
-
Plasma levels of IL-7 and IL-15 in the first month after myeloablative BMT are predictive biomarkers of both acute GVHD and relapse
Bone Marrow Transplantation (2010)
-
Hematopoietic stem cell transplantation using umbilical cord blood progenitors: review of current clinical results
Bone Marrow Transplantation (2004)
-
Transient hematopoietic stem cell rescue using umbilical cord blood for a lethally irradiated nuclear accident victim
Bone Marrow Transplantation (2002)
-
Similar myeloid recovery despite superior overall engraftment in NOD/SCID mice after transplantation of human CD34+ cells from umbilical cord blood as compared to adult sources
Bone Marrow Transplantation (2001)