Abstract
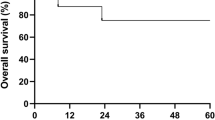
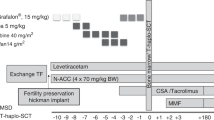
Chronic granulomatous disease (CGD) is a primary immunodeficiency disease symptomized by failure to generate superoxide and recurrent bacterial and fungal infections. Allogeneic bone marrow transplantation (BMT) is one of the therapeutic options available. However, it presents considerable risk to the recipient, especially if the patient is already at an advanced stage of disease, after repeated bacterial and fungal infections and organ damage. We present a case report of a 6-year-old child with long-standing CGD, severe clubbing, and jeopardized pulmonary function after multiple bacterial pulmonary infectious episodes, who had failed treatment with sulphamethazole trimethoprim, multiple antibiotic courses, itraconazole, as well as steroid and interferon-γ therapy. He underwent allogeneic peripheral blood stem cell transplantation (alloPBSCT) from his HLA-matched MLC non-reactive sister following non-myeloablative conditioning. His ANC did not fall below 0.2 × 109/l, his lowest WBC was 0.6 × 109/l, and his platelets did not fall below 28 × 109/l. He had normal engraftment, with no mucositis or organ toxicity. Neither parenteral nutrition nor platelet infusions were necessary. Partial donor chimerism following alloPBSCT was converted to full donor chimerism and superoxide production reverted to normal after donor lymphocyte infusions (DLI) from his HLA-matched sister. Twenty four months post transplant the patient is well, with stable and durable engraftment, 100% donor chimerism, normal superoxide production, no GVHD, and stabilization of his pulmonary condition. We suggest that alloPBSCT preceded by non-myeloablative conditioning and followed by DLI may constitute a successful mode of therapy for patients suffering from advanced CGD with recurrent infectious episodes resulting in organ dysfunction, enabling them to achieve full donor chimerism and normal superoxide production with minimal risk of transplant-related toxicity and GVHD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Nagler, A., Ackerstein, A., Kapelushnik, J. et al. Donor lymphocyte infusion post-non-myeloablative allogeneic peripheral blood stem cell transplantation for chronic granulomatous disease. Bone Marrow Transplant 24, 339–342 (1999). https://doi.org/10.1038/sj.bmt.1701903
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1701903
Keywords
This article is cited by
-
Allogeneic hematopoietic stem cell transplantation using unrelated cord blood or unmanipulated haploidentical donors is effective in pediatric chronic granulomatous disease with inflammatory complications and severe infection
Bone Marrow Transplantation (2020)
-
Successful allogeneic hematopoietic stem cell transplantation for chronic granulomatous disease with inflammatory complications and severe infection
International Journal of Hematology (2011)
-
Allogeneic Haematopoietic Stem Cell Transplantation as Therapy for Chronic Granulomatous Disease—Single Centre Experience
Journal of Clinical Immunology (2011)
-
Successful treatment of chronic granulomatous disease with fludarabine-based reduced-intensity conditioning and unrelated bone marrow transplantation
International Journal of Hematology (2008)
-
Effective donor lymphohematopoietic reconstitution after haploidentical CD34+-selected hematopoietic stem cell transplantation in children with refractory severe aplastic anemia
Bone Marrow Transplantation (2004)