Abstract
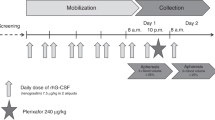
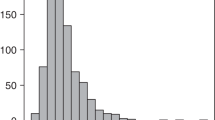
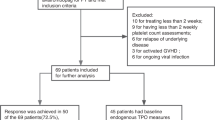
Patients with delayed platelet recovery post-PBPC transplant (PBPCT) are a high-risk group for thrombocytopenic bleeding and platelet transfusion dependence. Total CD34+ cell dosage has been proposed as the most important factor influencing the rate of platelet recovery. To achieve the shortest time to platelet engraftment, a minimum leukapheresis target of 10 × 106 CD34+ cells/kg was established for 30 patients. Of the 29 evaluable patients, 62% had rapid (group I: time to platelets >20 × 109/l ⩽10 days and 50 × 109/l ⩽14 days) platelet recoveries while 38% had delayed (group II: 20 × 109/l >10 days and 50 × 109/l >14 days) recoveries. Groups I and II were compared for: (1) pre-treatment variables; (2) mobilizing capability of CD34+ cells and subsets including megakaryocyte (Mk) progenitors; (3) infused dose of these cells at transplant; (4) changes in endogenous levels of Mpl ligand (or TPO) during mobilization and myeloablative chemotherapy. Group II patients received significantly more platelet transfusions (6 vs 2.1, P = 0.002) post-PBPCT, had a higher proportion of patients with a prior history of BM disease (64% vs 6%, P = 0.001), and showed a reduced ability to mobilize differentiated (CD34+/38+, CD34+/DR+) and Mk progenitors (CD34+/42a+, CD34+/61+). Only the number of Mk progenitors reinfused at transplant was significantly different between the groups (group II vs group I: CD34+/42a+ = 1.02 vs 2.56 × 106/kg, P = 0.013; CD34+/61+ = 1.12 vs 2.70 × 106/kg, P = 0.015). The ability to mobilize Mk progenitors correlated with percentage changes in endogenous levels of TPO from baseline to platelet nadir during mobilization chemotherapy (CD34+/42a+: r = 0.684, P = 0.007; CD34+/61+: r = 0.684, P = 0.007), with group II patients experiencing lower percentage changes. An inverse trend but no correlation was observed between serial TPO levels and platelet counts. TPO levels remained elevated in group II patients throughout a prolonged period of thrombocytopenia (median days to 50 × 109/l = 25 vs 11 for group I), indicating that delayed engraftment was not due to a deficiency of TPO but to a lack of Mk progenitor target cells. Our results show that the number of reinfused Mk progenitors is a better predictor of platelet engraftment than total CD34+ cell dosage. Small changes in endogenous TPO levels during mobilization predict for low Mk progenitor yields.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Maharaj, D., Steinberg, J., Gouvea, J. et al. Changes in endogenous TPO levels during mobilization chemotherapy are predictive of CD34+ megakaryocyte progenitor yield and identify patients at risk of delayed platelet engraftment post-PBPC transplant. Bone Marrow Transplant 23, 539–548 (1999). https://doi.org/10.1038/sj.bmt.1701618
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1701618