Abstract
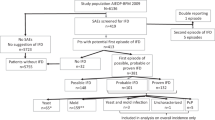
Liposomal amphotericin (AmBisome) 2 mg/kg three times weekly was compared with placebo as prophylaxis against fungal infection in patients undergoing chemotherapy or bone marrow transplantation (BMT) for haematological malignancies. Prophylaxis began on day 1 of chemotherapy and continued until neutrophils regenerated or infection was suspected. Of 161 evaluable patients, 74 received AmBisome and 87 received placebo. Proven fungal infections developed in no patients on AmBisome and in three on placebo (3.4%) (P = NS). Suspected fungal infections requiring intervention with systemic antifungal therapy (usually amphotericin B) occurred in 31 patients on AmBisome (42%) and in 40 on placebo (46%) (P = NS). Suspected deep-seated infections developed in 21 (28.3%) and 31 (35.6%) patients, respectively (P = NS). Time to develop a suspected or proven deep-seated infection showed a trend in favour of AmBisome (P = 0.11). Fifty patients had fungal colonisation (48 with Candida spp, two with Aspergillus spp) of at least one body site during prophylaxis; 15 patients while receiving AmBisome (20%) and 35 while on placebo (40%) (P < 0.01). time to colonisation was significantly delayed in the group receiving ambisome (P < 0.05). treatment-related toxicity was modest and no additional toxicity was observed in patients receiving ambisome. ambisome 2 mg/kg three times weekly is safe and reduces fungal colonisation in patients receiving intensive chemotherapy or bmt. however, despite encouraging trends, prophylactic ambisome did not lead to a significant reduction in fungal infection or in requirement for systemic antifungal therapy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Kelsey, S., Goldman, J., McCann, S. et al. Liposomal amphotericin (AmBisome) in the prophylaxis of fungal infections in neutropenic patients: a randomised, double-blind, placebo-controlled study. Bone Marrow Transplant 23, 163–168 (1999). https://doi.org/10.1038/sj.bmt.1701543
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1701543
Keywords
This article is cited by
-
Liposomal Amphotericin B (AmBisome®): A Review of the Pharmacokinetics, Pharmacodynamics, Clinical Experience and Future Directions
Drugs (2016)
-
Infectious Prophylaxis in Paediatric Oncology and Stem Cell Transplantation
Current Pediatrics Reports (2015)
-
Antifungal Prophylaxis in the Pediatric Intensive Care Unit
Current Fungal Infection Reports (2013)
-
Medical cost analysis for antifungal prophylaxis in neutropenic patients with hematological malignancies: a systematic simulation analysis
Supportive Care in Cancer (2011)
-
Aspergillus to Zygomycetes: Causes, Risk Factors, Prevention, and Treatment of Invasive Fungal Infections
Infection (2008)