Abstract
Objectives:
The aim of this study was to relate changes in energy expenditure and growth in infants with congenital heart disease (CHD), to the timing of corrective cardiac surgery.
Methods:
Prospective cohort study of infants less than 1 year with CHD admitted for cardiac surgery to Royal Children's Hospital, between January to September 2005. Infants were assessed using anthropometry and indirect calorimetry and compared to healthy age-matched controls.
Results:
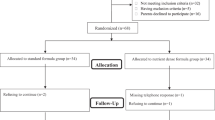
Infants (38) underwent corrective (n=25) or palliative (n=13) cardiac surgery either at ⩽10 days or at >10 days. Infants undergoing corrective surgery after 10 days had deficits in z-scores for weight compared with infants undergoing early surgery (−1.15±1.02 vs −0.24±0.98; CI 95%: −1.736 to −0.085; P<0.05) and height (−1.47±1.16 vs −0.12±0.66; CI 95%: −2.262 to −0.428; P<0.01). However, 6 months following surgery, weight and height were similar in both groups. Resting energy expenditure was increased before surgery compared to healthy controls (247±36 vs 210±22 kJ kg−1day−1; 95% CI: −57.29 to −16.71; P<0.001) however, normalized 1 week following cardiac surgery. Standard equations did not accurately predict measured REE.
Conclusion:
Increased REE observed in infants with CHD normalizes within 1 week following corrective cardiac surgery. Deficits in weight and growth were greater in infants undergoing corrective cardiac surgery>10 days of age compared with infants undergoing surgery in the first 10 days of life.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Ackerman IL, Karn CA, Denne SC, Ensing GJ, Leitch CA (1998). Total but not resting energy expenditure is increased in infants with ventricular septal defects. Pediatrics 102, 1172–1177.
Altman PL, Dittmer DS (1968). Energy metabolism at various weights. Metabolism. Federation of American Societies for Experimental Biology: Bethesda, Maryland. pp 343–345.
Aukburg SJ, Geer RT, Wollman H, Neufeld GR (1985). Errors in measurement of oxygen uptake due to anesthetic gases. Anesthesiology 62, 54–59.
Avitzur Y, Singer P, Dagan O, Kozer E, Abramovitch D, Dinari G et al. (2003). Resting energy expenditure in children with cyanotic and noncyanotic congenital heart disease before and after open heart surgery. JPEN J Parenter Enteral Nutr 27, 47–51.
Barton JS, Hindmarsh PC, Scrimgeour CM, Rennie MJ, Preece MA (1994). Energy expenditure in congenital heart disease. Arch Dis Child 70, 5–9.
Bayer LM, Robinson SJ (1969). Growth history of children with congenital heart defects. Size according to sex, age decade, surgical status, and diagnostic category. Am J Dis Child 117, 564–572.
Bland JM, Altman DG (1986). Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1, 307–310.
Bland JM, Altman DG (1995). Comparing methods of measurement: why plotting difference against standard method is misleading. Lancet 346, 1085–1087.
Butte NF, Wong WW, Ferlic L, Smith EO, Klein PD, Garza C (1990). Energy expenditure and deposition of breast-fed and formula-fed infants during early infancy. Pediatr Res 28, 631–640.
Coss-Bu JA, Jefferson LS, Walding D, David Y, Smith EO, Klish WJ (1998). Resting energy expenditure and nitrogen balance in critically ill pediatric patients on mechanical ventilation. Nutrition 14, 649–652.
Coss-Bu JA, Klish WJ, Walding D, Stein F, Smith EO, Jefferson LS (2001). Energy metabolism, nitrogen balance, and substrate utilization in critically ill children. Am J Clin Nutr 74, 664–669.
Farrell AG, Schamberger MS, Olson IL, Leitch CA (2001). Large left-to-right shunts and congestive heart failure increase total energy expenditure in infants with ventricular septal defect. Am J Cardiol 87, 1128–1131, A1110.
Gebara BM, Gelmini M, Sarnaik A (1992). Oxygen consumption, energy expenditure, and substrate utilization after cardiac surgery in children. Crit Care Med 20, 1550–1554.
Huse DM, Feldt RH, Nelson RA, Novak LP (1975). Infants with congenital heart disease. Food intake, body weight, and energy metabolism. Am J Dis Child 129, 65–69.
Krieger I (1970). Growth failure and congenital heart disease. Energy and nitrogen balance in infants. Am J Dis Child 120, 497–502.
Krovetz LJ (1963). Weight gain in children with patent ductus arteriosus. Dis Chest 44, 274–283.
Lees MH, Bristow JD, Griswold HE, Olmsted RW (1965). Relative hypermetabolism in infants with congenital heart disease and undernutrition. Pediatrics 36, 183–191.
Leitch CA, Karn CA, Ensing GJ, Denne SC (2000). Energy expenditure after surgical repair in children with cyanotic congenital heart disease. J Pediatr 137, 381–385.
Leitch CA, Karn CA, Peppard RJ, Granger D, Liechty EA, Ensing GJ et al. (1998). Increased energy expenditure in infants with cyanotic congenital heart disease. J Pediatr 133, 755–760.
Lucron H, Chipaux M, Bosser G, Le Tacon S, Lethor JP, Feillet F et al. (2005). Complications of prostaglandin E1 treatment of congenital heart disease in paediatric medical intensive care. Arch Mal Coeur Vaiss 98, 524–530.
Mitchell IM, Davies PS, Day JM, Pollock JC, Jamieson MP (1994). Energy expenditure in children with congenital heart disease, before and after cardiac surgery. J Thorac Cardiovasc Surg 107, 374–380.
Naeye RL (1967). Anatomic features of growth failure in congenital heart disease. Pediatrics 39, 433–440.
Nydegger A, Bines JE (2006). Energy metabolism in infants with congenital heart disease. Nutrition 22, 697–704.
Pittman JG, Cohen P (1964). The pathogenesis of cardiac cachexia. N Engl J Med 271, 453–460. CONCL.
Schofield WN (1985). Predicting basal metabolic rate, new standards and review of previous work. Hum Nutr Clin Nutr 39 (Suppl 1), 5–41.
van der Kuip M, Hoos MB, Forget PP, Westerterp KR, Gemke RJ, de Meer K (2003). Energy expenditure in infants with congenital heart disease, including a meta-analysis. Acta Paediatr 92, 921–927.
Wells JC (1998). Energy metabolism in infants and children. Nutrition 14, 817–820.
Witte MK (1996). Metabolic measurements during mechanical ventilation in the pediatric intensive care unit. Respiratory care clinics of North America 2, 573–586.
Acknowledgements
The author (AN) was supported by a grant from the Mach–Gaensslen Foundation, Switzerland.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nydegger, A., Walsh, A., Penny, D. et al. Changes in resting energy expenditure in children with congenital heart disease. Eur J Clin Nutr 63, 392–397 (2009). https://doi.org/10.1038/sj.ejcn.1602956
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1602956
Keywords
This article is cited by
-
Postoperative health-related quality of life in children with congenital heart disease: a short-term follow-up study
Journal of Cardiothoracic Surgery (2023)
-
Effect of feeding with standard or higher-density formulas on anthropometric measures in children with congenital heart defects after corrective surgery: a randomized clinical trial
European Journal of Clinical Nutrition (2022)
-
Nutritional status and associated factors among children with congenital heart disease in selected governmental hospitals and cardiac center,Addis Ababa Ethiopia
BMC Pediatrics (2021)
-
Dietary patterns are associated with central adiposity and carotid intima-media thickness in children and adolescents with congenital heart disease
European Journal of Nutrition (2021)
-
Caloric Intake During the Perioperative Period and Growth Failure in Infants With Congenital Heart Disease
Pediatric Cardiology (2013)