Abstract
Objectives:
To assess the effect of two similar olive oils, but with differences in their phenolic compounds (powerful antioxidant compounds), on inflammatory markers in stable coronary heart disease patients.
Design:
Placebo-controlled, crossover, randomized trial.
Setting:
Cardiology Department of Hospital del Mar and Institut Municipal d’Investigació Mèdica (Barcelona).
Subjects:
Twenty-eight stable coronary heart disease patients.
Interventions:
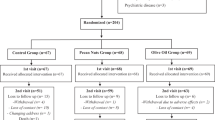
A raw daily dose of 50 ml of virgin and refined olive oil (ROO) was sequentially administered over two periods of 3-weeks, preceded by 2-week washout periods in which ROO was used.
Results:
Interleukin-6 (P<0.002) and C-reactive protein (P=0.024) decreased after virgin olive oil intervention. No changes were observed in soluble intercellular and vascular adhesion molecules, glucose and lipid profile.
Conclusions:
Consumption of virgin olive oil, could provide beneficial effects in stable coronary heart disease patients as an additional intervention to the pharmacological treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Beauchamp GK, Keast RS, Morel D, Lin J, Pika J, Han Q et al. (2005). Phytochemistry: ibuprofen-like activity in extra-virgin olive oil. Nature 437, 45–46.
Berliner JA, Territo MC, Sevanian A, Kim JA, Bamshad B, Esterson M et al. (1990). Minimally modified low density lipoprotein stimulates monocyte endothelial interactions. J Clin Invest 85, 1260–1266.
Bogani P, Galli C, Villa M, Visioli F (2007). Postprandial anti-inflammatory and antioxidant effects of extra virgin olive oil. Atherosclerosis 190, 181–186.
Carluccio MA, Siculella L, Ancora MA, Massaro M, Scoditti E, Storelli C et al. (2003). Olive oil and red wine antioxidant polyphenols inhibit endothelial activation: antiatherogenic properties of Mediterranean diet phytochemicals. Arterioscler Thromb Vasc Biol 23, 622–629.
Covas MI, Nyyssönen K, Poulsen HE, Kaikkonen J, Zunft HJF, Kiesewetter H et al. (2006a). The effect of polyphenols in olive oil on heart disease risk factors. Ann Int Med 145, 333–341.
Covas MI, Ruiz-Gutiérrez V, de la Torre R, Kafatos A, Lamuela-Raventós R, Osada J et al. (2006b). Olive oil minor components: evidence to date of health benefits in humans. Nutr Rev 64 (Supplement 1), 20–30.
Elosua R, Marrugat J, Molina L, Pons S, Pujol E (1994). Validation of the minnesota leisure time physical activity questionnaire in spanish men. The MARATHOM Investigators. Am J Epidemiol 139, 1197–1209.
Esposito K, Marfella R, Ciotola M, Di Palo C, Giugliano F, Giugliano G et al. (2004). Effect of a mediterranean-style diet on endothelial dysfunction and markers of vascular inflammation in the metabolic syndrome: a randomized trial. JAMA 292, 1440–1446.
Estruch R, Martínez-González MA, Corella D, Salas-Salvadó J, Ruiz-Gutiérrez V, Covas MI et al. (2006). Effects of a mediterranean-style diet on cardiovascular risk factors: a randomized trial. Ann Int Med 145, 1–11.
Fito M, Cladellas M, de la TR, Marti J, Alcantara M, Pujadas-Bastardes M et al. (2005). Antioxidant effect of virgin olive oil in patients with stable coronary heart disease: a randomized, crossover, controlled, clinical trial. Atherosclerosis 181, 149–158.
Helsing E (1995). Traditional diets and disease patterns of the Mediterranean, circa 1960. Am J Clin Nutr 61, 1329S–1337S.
Kim JA, Territo MC, Wayner E, Carlos TM, Parhami F, Smith CW et al. (1994). Partial characterization of leukocyte binding molecules on endothelial cells induced by minimally oxidized LDL. Arterioscler Thromb 14, 427–433.
Kris-Etherton PM (1999). Monounsaturated fatty acids and risk of cardiovascular disease. Circulation 100, 1253–1258.
Leger CL, Carbonneau MA, Michel F, Mas E, Monnier L, Cristol JP et al. (2005). A thromboxane effect of a hydroxytyrosol-rich olive oil wastewater extract in patients with uncomplicated type I diabetes. Eur J Clin Nutr 59, 727–730.
Miró-Casas E, Covas MI, Fitó M, Farré-Albadalejo M, Marrugat J, de la Torre R (2003). Tyrosol and hydroxytyrosol are absorbed from moderate and sustained doses of virgin olive oil in humans. Eur J Clin Nutr 57, 186–190.
Murase T, Kume N, Hase T, Shibuya Y, Nishizawa Y, Tokimitsu I et al. (1999). Gallates inhibit cytokine-induced nuclear translocation of NF-kappaB and expression of leukocyte adhesion molecules in vascular endothelial cells. Arterioscler Thromb Vasc Biol 19, 1412–1420.
Perona JS, Cabello-Moruno R, Ruiz-Gutierrez V (2006). The role of virgin olive oil components in the modulation of endothelial function. J Nutr Biochem 17, 429–445.
Ross R (1999). Atherosclerosis – an inflammatory disease. N Engl J Med 340, 115–126.
Schroder H, Covas MI, Marrugat J, Vila J, Pena A, Alcantara M et al. (2001). Use of a three-day estimated food record, a 72-h recall and a food- frequency questionnaire for dietary assessment in a Mediterranean Spanish population. Clin Nutr 20, 429–437.
Tsimikas S, Philis-Tsimikas A, Alexopoulos S, Sigari F, Lee C, Reaven PD (1999). LDL isolated from Greek subjects on a typical diet or from American subjects on an oleate-supplemented diet induces less monocyte chemotaxis and adhesion when exposed to oxidative stress. Arterioscler, Thromb Vasc Biol 19, 122–130.
Tunstall-Pedoe H, Kuulasmaa K, Mahonen M, Tolonen H, Ruokokoski E, Amouyel P (1999). Contribution of trends in survival and coronary-event rates to changes in coronary heart disease mortality: 10-year results from 37 WHO MONICA project populations. Monitoring trends and determinants in cardiovascular disease. Lancet 353, 1547–1557.
Tzoulaki I, Murray GD, Lee AJ, Rumley A, Lowe GD, Fowkes FG (2005). C-reactive protein, interleukin-6, and soluble adhesion molecules as predictors of progressive peripheral atherosclerosis in the general population: Edinburgh Artery Study. Circulation 112, 976–983.
Visioli F, Caruso D, Grande S, Bosisio R, Villa M, Galli G et al. (2005). Virgin Olive Oil Study (VOLOS): vasoprotective potential of extra virgin olive oil in mildly dyslipidemic patients. Eur J Nutr 44, 121–127.
Weinbrenner T, Cladellas M, Isabel CM, Fito M, Tomas M, Senti M et al. (2003). High oxidative stress in patients with stable coronary heart disease. Atherosclerosis 168, 99–106.
Wu D, Koga T, Martin KR, Meydani M (1999). Effect of vitamin E on human aortic endothelial cell production of chemokines and adhesion to monocytes. Atherosclerosis 147, 297–307.
Yaqoob P, Knapper JA, Webb DH, Williams CM, Newsholme EA, Calder PC (1998). Effect of olive oil on immune function in middle-aged men. Am J Clin Nutr 67, 129–135.
Acknowledgements
We thank the Ferderació Cooperatives Agràries de Catalunya for provide the olive oil used in the study. Fondo de investigación Sanitaria:FIS-PI02-0791 and partially supported by CIBER: CB-03-0028.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Guarantor: M Fitó.
SOLOS (Spanish Olive Oil Study) Study Investigators: Alcántara M, Covas MI, Fitó M, Marrugat J, Schröder H, Weinbrenner T, Alcántara M, Muñoz D, Guxens M (Unitat de Lipids i Epidemiologia Cardiovascular, Institut Muncipal d’Investigació Mèdica), de la Torre R, Farré M, Menoyo E, Pujadas-Bastardes M, Closas N, Khymenets O (Unitat de Farmacologia, Institut Muncipal d’Investigació Mèdica), and de la Torre-Boronat C, Gimeno E, Lamuela R and López MC (Departament de Bromatologia i Nutricio, Facultat de Farmacia, Universitat de Barcelona).
Contributors: Drs MF, MC, and MIC had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of analyses; Study concept and design: MF, MC, MIC, RT, JM; Acquisition of the data: MA, DM, MF, MC, MP-B, JM, HS; Analysis and interpretation of data: MF, MC, MIC, RT, MCL-S, JM; Drafting of the manuscript: MF, MC, MIC; Critical revision of the manuscript for important intellectual content: MA, MC, MIC, MF, RT, HS, JM, JM, MCL-S, JB, DM, MP-B; Statistical analyses: MF, MC; Obtained funding: MC, MIC, JB; Administrative, technical and material support: MF, JM, DM, MP-B, HS, MA.
Rights and permissions
About this article
Cite this article
Fitó, M., Cladellas, M., de la Torre, R. et al. Anti-inflammatory effect of virgin olive oil in stable coronary disease patients: a randomized, crossover, controlled trial. Eur J Clin Nutr 62, 570–574 (2008). https://doi.org/10.1038/sj.ejcn.1602724
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1602724
Keywords
This article is cited by
-
Effects of anti-inflammatory dietary patterns on non-alcoholic fatty liver disease: a systematic literature review
European Journal of Nutrition (2023)
-
Extra virgin olive oil high in polyphenols improves antioxidant status in adults: a double-blind, randomized, controlled, cross-over study (OLIVAUS)
European Journal of Nutrition (2022)
-
Effects of canola or olive oil on plasma lipids, lipoprotein-associated phospholipase A2 and inflammatory cytokines in patients referred for coronary angiography
Lipids in Health and Disease (2020)
-
The effects of extra virgin olive oil and canola oil on inflammatory markers and gastrointestinal symptoms in patients with ulcerative colitis
European Journal of Clinical Nutrition (2020)
-
An inverse association between the Mediterranean diet and bladder cancer risk: a pooled analysis of 13 cohort studies
European Journal of Nutrition (2020)