Abstract
Objective:
To investigate the potential of acetic acid supplementation as a means of lowering the glycaemic index (GI) of a bread meal, and to evaluate the possible dose–response effect on postprandial glycaemia, insulinaemia and satiety.
Subjects and setting:
In all, 12 healthy volunteers participated and the tests were performed at Applied Nutrition and Food Chemistry, Lund University, Sweden.
Intervention:
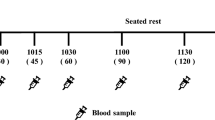
Three levels of vinegar (18, 23 and 28 mmol acetic acid) were served with a portion of white wheat bread containing 50 g available carbohydrates as breakfast in randomized order after an overnight fast. Bread served without vinegar was used as a reference meal. Blood samples were taken during 120 min for analysis of glucose and insulin. Satiety was measured with a subjective rating scale.
Results:
A significant dose–response relation was seen at 30 min for blood glucose and serum insulin responses; the higher the acetic acid level, the lower the metabolic responses. Furthermore, the rating of satiety was directly related to the acetic acid level. Compared with the reference meal, the highest level of vinegar significantly lowered the blood glucose response at 30 and 45 min, the insulin response at 15 and 30 min as well as increased the satiety score at 30, 90 and 120 min postprandially. The low and intermediate levels of vinegar also lowered the 30 min glucose and the 15 min insulin responses significantly compared with the reference meal. When GI and II (insulinaemic indices) were calculated using the 90 min incremental area, a significant lowering was found for the highest amount of acetic acid, although the corresponding values calculated at 120 min did not differ from the reference meal.
Conclusion:
Supplementation of a meal based on white wheat bread with vinegar reduced postprandial responses of blood glucose and insulin, and increased the subjective rating of satiety. There was an inverse dose–response relation between the level of acetic acid and glucose and insulin responses and a linear dose–response relation between acetic acid and satiety rating. The results indicate an interesting potential of fermented and pickled products containing acetic acid.
Sponsorships:
Dr P Håkansson's foundation and Direktör Albert Påhlsson's foundation for research and charity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others

References
Blum AL, Heggelin J, Krejs GJ, Largiadèr F, Säuberli H & Schmid P (1976): Gastric emptying of organic acids in the dog. J. Physiol. 261, 285–290.
Braaten JT, Wood P, Scott FW, Riedel KD, Poste L & Collins W (1991): Oat gum lowers glucose and insulin after an oral glucose load. Am. J. Clin. Nutr. 53, 1425–1430.
Brighenti F, Castellani G, Benini L, Casiraghi MC, Leopardi E, Crovetti R & Testolin G (1995): Effect of neutralized and native vinegar on blood glucose and acetate responses to a mixed meal in healthy subjects. Eur. J. Clin. Nutr. 49, 242–247.
Darwiche G, Stman EM, Liljeberg HGM, Kallinen N, Björgell O, Björck IME & Almér L-O (2001): Measurements of the gastric emptying rate by use of ultrasonography: studies in humans using bread with added sodium propionate. Am. J. Clin. Nutr. 74, 254–258.
Ebihara K & Nakajima A (1988): Effect of acetic acid and vinegar on blood glucose and insulin responses to orally administered sucrose and starch. Agric. Biol. Chem. 52, 1311–1312.
Feinle C, O'Donovan D & Horowitz M (2002): Carbohydrate and satiety. Nutr. Rev. 60, 155–169.
Fushimi T, Tayama K, Fukaya M, Kitakoshi K, Nakai N, Tsukamoto Y & Sato Y (2001): Acetic acid feeding enhances glycogen repletion in liver and skeletal muscle of rats. J. Nutr. 131, 1973–1977.
Gatti E, Noe D, Pazzucconi F, Gianfranceschi G, Porrini M, Testolin G & Sirtori CR (1992): Differential effect of unsaturated oils and butter on blood glucose and insulin response to carbohydrate in normal volunteers. Eur. J. Clin. Nutr. 46, 161–166.
Granfeldt YE, Björck IME & Hagander B (1991): On the importance of processing conditions, product thickness and egg addition for the glycaemia and hormonal responses to pasta: a comparison with bread made from ‘pasta ingredients’. Eur. J. Clin. Nutr. 45, 489–499.
Granfeldt YE, Drews A & Björck IME (1995): Arepas made from high-amylose corn flour produce favourably low glucose and insulin responses in healthy humans. J. Nutr. 125, 459–465.
Hellström PM & Näslund E (2001): Interactions between gastric emptying and satiety, with special reference to glucagon-like peptide-1. Physiol. Behav. 74, 735–741.
Horowitz M, Dent J, Fraser R, Sun W & Hebbard G (1994): Role and integration of mechanisms controlling gastric emptying. Dig. Dis. Sci. 39, 7S–13S.
Hunt JN & Knox MT (1972): The slowing of gastric emptying by four strong acids and three weak acids. J. Physiol. 222, 187–208.
Hunt JN & Knox MT (1969): The slowing of gastric emptying by nine acids. J. Physiol. 201, 161–179.
Jenkins DJA, Wolever TMS, Taylor RH, Barker H, Fielden H, Baldwin JM, Bowling AC, Newman HC, Jenkins AL & Goff DV (1981): Glycemic index of foods: a physiological basis for carbohydrate exchange. Am. J. Clin. Nutr. 34, 362–366.
Johnston CS, Kim CM & Buller AJ (2004): Vinegar improves insulin sensitivity to a high-carbohydrate meal in subjects with insulin resistance or type 2 diabetes. Diabetes Care 27, 281–282.
Liljeberg HGM & Björck IME (1994): Bioavailability of starch in bread products. Postprandial glucose and insulin responses in healthy subjects and in vitro resistant starch content. Eur. J. Clin. Nutr. 48, 151–163.
Liljeberg HGM & Björck IME (1996): Delayed gastric emptying rate as a potential mechanism for lowered glycemia after eating sourdough bread: studies in humans and rats using test products with added organic acids or an organic salt. Am. J. Clin. Nutr. 64, 883–893.
Liljeberg HGM & Björck IME (1998): Delayed gastric emptying rate may explain improved glycaemia in healthy subjects to a starchy meal with added vinegar. Eur. J. Clin. Nutr. 52, 368–371.
Liljeberg HGM, Lönner CH & Björck IME (1995): Sourdough fermentation or addition of organic acids or corresponding salts to bread improves nutritional properties of starch in healthy humans. J. Nutr. 125, 1503–1511.
Liljeberg HGM, Åkerberg AKE & Björck IME (1999): Effect of the glycemic index and content of indigestible carbohydrates of cereal-based breakfast meals on glucose tolerance at lunch in healthy subjects. Am. J. Clin. Nutr. 69, 647–655.
Liljeberg HGM, Åkerberg AKE & Björck IME (1996): Resistant starch formation in bread as influenced by choice of ingredients or baking conditions. Food Chem. 56, 389–394.
Liu S, Willett WC, Stampfer MJ, Hu FB, Franz M, Sampson L, Hennekens CH & Manson JE (2000): A prospective study of dietary glycemic load, carbohydrate intake, and risk of coronary heart disease in US women. Am. J. Clin. Nutr. 71, 1455–1461.
Ludwig DS (2000): Dietary glycemic index and obesity. J. Nutr. 130, 280S–283S.
MacIntosh CG, Holt SH & Brand-Miller JC (2003): The degree of fat saturation does not alter glycemic, insulinemic or satiety responses to a starchy staple in healthy men. J. Nutr. 133, 2577–2580.
McKeown NM, Meigs JB, Liu S, Saltzman E, Wilson PWF & Jaques PF (2004): Carbohydrate nutrition, insulin resistance, and the prevalence of the metabolic syndrome in the Framingham offspring cohort. Diabetes Care 27, 538–546.
Ogawa N, Satsu H, Watanabe H, Fukaya M, Tsukamoto Y, Miyamoto Y & Shimizu M (2000): Acetic acid suppresses the increase in disaccharidase activity that occurs during culture of Caco-2 cells. J. Nutr. 130, 507–513.
Owen B & Wolever TM (2003): Effect of fat on glycaemic responses in normal subjects: a dose-response study. Nutr. Res. 23, 1341–1347.
Salmerón J, Ascherio A, Rimm EB, Colditz GA, Spiegelman D, Jenkins DJ, Stampfer MJ, Wing AL & Willett WC (1997a): Dietary fibre, glycemic load, and risk of NIDDM in men. Diabetes Care 20, 545–550.
Salmerón J, Manson JE, Stampfer MJ, Colditz GA, Wing AL & Willett WC (1997b): Dietary fibre, glycemic load, and risk of non-insulin-dependent diabetes mellitus in women. J. Am. Med. Assoc. 277, 472–477.
Sugiyama M, Tang AC, Wakaki Y & Koyama W (2003): Glycemic index of single and mixed meal foods among common Japanese foods with white rice as a reference food. Eur. J. Clin. Nutr. 57, 743–752.
Wolever TMS, Bentum-Williams A & Jenkins DJA (1995): Physiological modulation of plasma free fatty acid concentrations by diet. Metabolic implications in nondiabetic subjects. Diabetes Care 18, 962–970.
Åkerberg AKE, Liljeberg HGM & Björck IME (1998): Effects of amylose/amylopectin ratio and baking conditions on resistant starch formation and glycaemic indices. J. Cereal Sci. 28, 71–80.
Östman EM, Liljeberg Elmståhl HGM & Björck IME (2002a): Barley bread containing lactic acid improves glucose tolerance at a subsequent meal in healthy men and women. J. Nutr. 132, 1173–1175.
Östman EM, Nilsson M, Liljeberg Elmståhl HGM, Molin G & Björck IME (2002b): On the effect of lactic acid on blood glucose and insulin responses to cereal products: mechanistic studies in healthy subjects and in vitro. J. Cereal Sci. 36, 339–346.
Author information
Authors and Affiliations
Corresponding author
Additional information
Guarantor: E Östman.
Contributors: YG made the design of the experiment with assistance from EÖ and IB. LP did the blood sampling and analysis. YG was in charge of the collection and analysis of data. EÖ had the primary responsibility for writing the manuscript, but YG and IB provided comments on several drafts. None of the authors had any conflicts of interest.
Rights and permissions
About this article
Cite this article
Östman, E., Granfeldt, Y., Persson, L. et al. Vinegar supplementation lowers glucose and insulin responses and increases satiety after a bread meal in healthy subjects. Eur J Clin Nutr 59, 983–988 (2005). https://doi.org/10.1038/sj.ejcn.1602197
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1602197
Keywords
This article is cited by
-
Effect of some traditional processing operations on the chemical, functional, antioxidant, glycaemic index and glycaemic load of groundnut (Arachis hypogea L.) seed flour
Journal of Food Measurement and Characterization (2022)
-
Glycemic response, satiety, gastric secretions and emptying after bread consumption with water, tea or lemon juice: a randomized crossover intervention using MRI
European Journal of Nutrition (2022)
-
Effects of apple cider vinegar on haemato-biochemical parameters of gestating rats and morphometric indices of their pups at delivery
Comparative Clinical Pathology (2021)
-
Lemon juice, but not tea, reduces the glycemic response to bread in healthy volunteers: a randomized crossover trial
European Journal of Nutrition (2021)
-
Short-term Cudrania tricuspidata fruit vinegar administration attenuates obesity in high-fat diet-fed mice by improving fat accumulation and metabolic parameters
Scientific Reports (2020)