Abstract
Objective:
We designed this study to investigate the effects of oral L-carnitine administration on fasting plasma glucose (FPG), glycosylated hemoglobin (HbA1c) and lipid parameters in patients with diabetes mellitus type II.
Patients and methods:
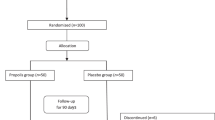
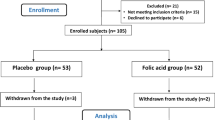
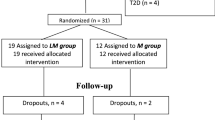
The effect of L-carnitine on FPG and lipid parameters was investigated in 22 male and 13 female type II diabetic patients; the mean age±s.d. was 51.3±3.7 y. The patients were randomly allocated to two groups (L-carnitine and placebo group) and 1 g of L-carnitine or of placebo was given orally three times a day for a period of 12 weeks.
Results:
FPG in the L-carnitine group decreased significantly from 143±35 to 130±33 mg/dl (P=0.03), and we observed a significant increase of triglycerides (TG) from 196±61 to 233±12 mg/dl (P=0.05), of Apo A1 from 94±20 to 103±23 mg/dl (P=0.02), and of Apo B100 from 98±18 to 108±22 mg/dl (P=0.02) after 12 weeks of treatment. There was no significant change in LDL-C, HDL-C, HbA1C, LP(a) or total cholesterol.
Conclusion:
L-Carnitine significantly lowers FPG but increases fasting triglyceride in type II diabetic patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Abdel-aleem S, Karim AM, Zarouk WA, Taylor DA, el-Awady MK & Low JE (1997): Reduced effects of l-carnitine on glucose and fatty acid metabolism in myocytes isolated from diabetic rats. Horm. Metab. Res. 29, 430–435.
Broderick TL, Quinney HA & Lopaschuk GD (1992): Carnitine stimulation of glucose oxidation in the fatty acid perfused isolated working rat heart. J. Biol. Chem. 267, 3758–4636.
Capaldo B, Napoli R, Bonito DP, Albano G & Sacca L (1991): Carnitine improves peripheral glucose disposal in non-insulin-dependent diabetic patients. Diab. Res. Clin. Pract. 14, 191–196.
Davis RA & Hui TY (2001): 2000 George Lyman Duff Memorial Lecture: atherosclerosis is a liver disease of the heart. Arterioscler. Thromb. Vasc. Biol. 21, 887–898.
De Palo E, Gatti R, Sicolo N, Padovan D, Vettor R & Federspil G (1981): Plasma and urine free L-carnitine in human diabetes mellitus. Acta Diabetol. Lat. 18, 91–95.
Derosa G, Cicero FGA, Gaddi A, Mugellini A, Ciccarelli L & Fogari R (2003): The effect of L-carnitine on plasma lipoprotein(a) levels in hypercholesterolemic patients with type 2 diabetes mellitus. Clin. Ther. 25, 1429–1439.
Di Donto S, Garavaglia B, Rimoldi M & Carrara F (1992): Clinical and biomedical phenotypes of carnitine deficiencies. In -Carnitine and its Role in Medicine: From Function to Therapy eds. R Ferrari, S Di Mauro, G Sherwood. London: Academic Press.
Fritz IB & Marquis NR (1965): The role of acyl-carnitine esters and carnitine palmitoyltransferase in the transport of fatty acyl groups across mitochondrial memberanes. Proc. Natl. Acad. Sci. USA 54, 1226–1230.
Gaetano DA, Mingrone G, Castagneto M & Calvani M (1999): Carnitine increases glucose disposal in humans. J. Am. Coll. Nutr. 18, 289–295.
Huang B, Wu P, Popov KM & Harris R (2003): Starvation and diabetes reduce the amount of pyruvate dehydrogenase phosphatase in rat heart and kidney. Diabetes 52, 1371–1376.
Maccari F, Pessotto P, Ramacci T M & Angelucci L (1985): The effect of exogenous L-carnitine on fat diet induced hyperlipidemia in the rat. Life Sci. 36, 1967–1975.
Maebashi M, Kawamura N, Sato M, Imamura A & Yoshinaga K (1978): Lipid-lowering effect of carnitine in patients with type-IV hyperlipoproteinaemia. Lancet 14, 805–807.
Mingrone G, Greco VA, Capristo E, Benedetti G, Giancaterini A, Gaetano A & Gasbarrini G (1999): L-carnitine improves glucose disposal in type 2 diabetic patients. J. Am. Coll. Nutr. 18, 77–82.
Nakai N, Miyazaki Y, Sato Y, Oshida Y, Nagasaki M, Tanaka M, Nakashima K & Shimomura Y (2002): Exercise training increases the activity of pyruvate dehydrogenase complex in skeletal muscle of diabetic rats. Endocr. J. 49, 547–554.
Packard CJ & Sheperd J (1995): Metabolic basis of the atherogenic lipoprotein phenotype. In pp 289–294 Multiple Risk Factor in Cardiovascular Disease eds AM Gotto, C Lenfant, AL Catapano, R Paoletti. Dordrecht, Kluwer Academic Publishers.
Reymond LT, Reynolds AS, Swanson AJ, Patnode AC & Bell PF (1987): The effect of oral L-carnitine on lipoprotein composition in the Watanabe heritable hyperlipidemic rabbit (Oryctolagus cuniculus). Commun. Biochem. Physiol. 88, 503–506.
Rhew TH & Sachan DS (1986): Dose-dependent lipotropic effect of carnitine in chronic alcoholic rats. J. Nutr. 116, 2263–2269.
Rodrigues B, Secombe D & Mcneill JH (1990): Lack of effect oral L-carnitine trearment on lipid metabolism and cardiac function in chronically diabetic rats. Can. J. Phisiol. Pharmacol. 68, 1601–1608.
Rodrigues B, Xiang H & Mcneill HJ (1988): Effect of L-carnitine traerment on lipid metabolism and performance in chronically diabetic rats. Diabetes 37, 1358–1364.
Secombe WD, James L, Hahn P & Jones E (1987): L-Carnitine trearment in the hyperlipidemic rabbit. Metabolism 36, 1192–1196.
Sirtori CR, Calabresi L, Ferrara S, Pazzucconi F, Bondioli A, Baldassarre D, Birreci A & Koverech A (2000): L-Carnitine reduces plasma lipoprotein(a) levels in patients with hyper Lp(a). Nutr. Metab. Cardiovasc. Dis. 10, 247–251.
Stefanutti C, Vivenzio A, Lucani G, Di Giacomo S & Lucani E (1998): Effect of L-carnitine on plasma lipoprotein fatty acids pattern in patients with primary hyperlipoproteinemia. Clin. Ther. 149, 115–119.
Sugden MC & Holness MJ (2002): Therapeutic potential of the mammalian pyruvate dehydrogenase kinases in the prevention of hyperglycaemia. Curr. Drug Immune Endocr. Metabol. Disord. 2, 151–165.
Tamamogullari N, Silig Y, Icagasioglu S & Atalay A (1999): Carnitine deficiency in diabetes mellitus complications. J. Diab. Complic. 13, 251–253.
Uziel G, Garavaglia B & Di Donato S (1988): Carnitine stimulation of pyruvate dehydrogenase complex (PDHC) in isolated human skeletal muscle mitochondria. Muscle Nerve 11, 720–724.
Vacha MG, Giorcelli G, Siliprandi N & Corsi M (1983): Favorable effects of L-carnitine treatment on hypertriglyceridemia in hemodialysis patiants: decisive role of low levels of high-density lipoprotein-cholestrol. Am. J. Clin. Nutr. 38, 532–540.
Yeh GY, Eisenberg DM, Kaptchuk TJ & Phillips RS (2003): Systematic review of herbs and dietary supplements for glycemic control in diabetes. Diabetes Care 26, 1277–1294.
Author information
Authors and Affiliations
Corresponding author
Additional information
Guarantor: AR Rahbar.
Contributors: ARR designed the study, collected and analyzed the data and wrote the manuscript. RS, NS, FT, AP and BG helped in collection and analyzing the dates.
Rights and permissions
About this article
Cite this article
Rahbar, A., Shakerhosseini, R., Saadat, N. et al. Effect of L-carnitine on plasma glycemic and lipidemic profile in patients with type II diabetes mellitus. Eur J Clin Nutr 59, 592–596 (2005). https://doi.org/10.1038/sj.ejcn.1602109
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1602109
Keywords
This article is cited by
-
A methodological quality review of citations of randomized controlled trials of diabetes type2 in leading clinical practice guidelines and systematic reviews
Journal of Diabetes & Metabolic Disorders (2023)
-
Discovery of metabolic biomarkers for gestational diabetes mellitus in a Chinese population
Nutrition & Metabolism (2021)
-
Acetyl-l-Carnitine Ameliorates Metabolic and Endocrine Alterations in Women with PCOS: A Double-Blind Randomized Clinical Trial
Advances in Therapy (2021)
-
Role of carnitine and its derivatives in the development and management of type 2 diabetes
Nutrition & Diabetes (2018)
-
L-Carnitine and extendin-4 improve outcomes following moderate brain contusion injury
Scientific Reports (2018)