Abstract
Total sleep deprivation (TSD) shows powerful but transient clinical effects in patients affected by bipolar depression. Pindolol blocks the serotonergic 5-HT1A autoreceptor, thus improving the antidepressant effect of selective serotonin reuptake inhibitors. We evaluated the interaction of TSD and pindolol in the treatment of acute episodes of bipolar depression. Forty bipolar depressed inpatients were randomized to receive pindolol 7.5 mg/day or placebo for nine days in combination with three consecutive TSD cycles. Pindolol significantly improved the antidepressant effect of TSD, and prevented the short-term relapse after treatment. The response rate (HDRS scores <8) at the end of treatment was 15/20 for pindolol, and 3/20 for placebo. Coadministration of pindolol and TSD resulted in a complete response, which could be sustained for six months with lithium salts alone, in 65% of cases. This results suggest a major role for serotonergic transmission in the mechanism of action of TSD, and makes TSD treatment more effective in the treatment of bipolar depression.
Similar content being viewed by others
Main
Total sleep deprivation (TSD) causes a marked but transient improvement of depressive symptomatology in bipolar depressed patients: it acts rapidly and with a response rate of about 60%, but the dramatic mood improvement is usually followed by an early relapse (i.e., within the first days after TSD) which lessens the clinical usefulness of this treatment (Wu and Bunney 1990). Several studies, indeed, showed better clinical responses with the combination of sleep deprivation and antidepressant drugs (Leibenluft and Wehr 1992). In particular, positive interactions were reported with lithium, fluoxetine, nortryptiline, clomipramine, desipramine, and amitriptyline (e.g., Elsenga and Van den Hoofdakker 1982/1983; Baxter et al. 1986; Shelton and Loosen 1993; Szuba et al. 1994; Kuhs et al. 1996; Benedetti et al. 1997), while negative interactions were observed with trimipramine and amineptine (Holsboer-Trachsler et al. 1994; Benedetti et al. 1996).
Though several hypotheses have been proposed, the mechanism of action of TSD is still unclear. From a neurochemical point of view, sleep deprivation enhances the functioning of several neurotransmitter systems including brain serotonin (5-HT) pathways, which physiologically show the highest activity during behavioral arousal and the lowest during sleep (Fornal and Jacobs 1988). In particular, preclinical research showed that changes in the activity of brain 5-HT pathways after sleep deprivation included an increase in the serotonergic neuronal activity in the dorsal raphe nucleus (DRN) of cats (Gardner et al. 1997), an increase in brain 5-HT turnover in rats and hamsters (Hery et al. 1970; Cramer et al. 1973; Asikainen et al. 1995), and an increase in behavioral responsiveness to 5-HT precursors (Santos and Carlini 1983). In agreement with these findings, a clinical study showed that in human depressed females sleep deprivation led to an enhanced prolactine response to tryptophan, an effect mediated by serotonergic pathways (Salomon et al. 1994).
Preclinical studies showed that changes in 5-HT function due to TSD involve a reduction in sensitivity of 5-HT1A autoreceptors. In rats, Maudhuit et al. (1996) showed that REM sleep deprivation reduced the inhibitory response of serotonergic DRN neurons to citalopram, an effect mediated by 5-HT1A autoreceptors stimulation (Hjorth 1993). In cats, Gardner et al. (1997) showed that the neuronal inhibition produced by the selective 5-HT1A agonist 8-hydroxy-2-(di-n-propylamino)tetralin (8-OH-DPAT) was reduced after TSD. Gardner et al. (1997) then hypothesized that the observed increase in the firing rate of serotonergic DRN neurons could be due to a decrease in the sensitivity of 5-HT1A autoreceptors after TSD.
Several findings are in agreement with the hypothesis of Gardner et al. (1997). In the awake cat the 5-HT1A antagonist WAY-100635 increased 5-HT cell firing (Fornal et al. 1996). In healthy human subjects the administration of the 5-HT1A-beta adrenoreceptor blocker pindolol, but not other beta adrenoreceptor blockers, caused a significant REM sleep suppression with REM rebound after withdrawal (Betts and Alford 1985; Kostis and Rosen 1987), an effect which is similar to that observed after administration of serotonergic antidepressant drugs (e.g., Vogel et al. 1980). In rats, pindolol caused similar changes in sleep and antagonized the effects of 8-OH-DPAT (Monti and Jantos 1994). In rats, the 5-HT1A antagonist NAN-190 suppressed REM sleep and the combination of NAN-190 with citalopram augmented the effect (Neckelmann et al. 1996). Since an enhancement in 5-HT function at the mesopontine level leads to a reduction in REM sleep (Leonard and Llinàs 1994), these findings suggest that manipulation of 5-HT1A autoreceptors directly influence brain serotonergic function.
In another hypothesis, enhancement in 5-HT firing due to TSD could involve enhanced 5-HT1A autoreceptor stimulation, with self-inhibition of 5-HT neurons, and subsequent reduction in the sensitivity of 5-HT1A autoreceptors due to down-regulation mechanisms.
Whether the “primary” effect of TSD on 5-HT pathways is the desentization of 5-HT1A autoreceptors or the enhancement in neuronal firing, the administration of a 5-HT1A antagonist should potentiate the increase in 5-HT function due to TSD.
Pindolol is a 5-HT1A-beta adrenoreceptor blocking drug. In vivo microdialysis and electrophysiological studies showed that pindolol blocks pre- but not postsynaptic 5-HT1A receptors (Romero et al. 1996). Since somatodendritic 5-HT1A autoreceptors are responsible of the self-inhibition of 5-HT on serotonergic neurons, it has been hypothesized that the combination of selective serotonin reuptake inhibitors (SSRIs) with pindolol could reduce the self-inhibition of serotonergic transmission, thus enhancing the antidepressant effect of the former compounds (Artigas 1995; Artigas et al. 1996). Recent double-blind placebo-controlled studies confirmed, with one exception (Berman et al. 1997), that pindolol hastens the antidepressant effect of SSRIs (Perez et al. 1997; Tome et al. 1997a, 1997b; Zanardi et al. 1997; Zanardi et al. 1998), while controversial results have been reported in studies on resistant depression (e.g., Artigas et al. 1994; Blier and Bergeron 1995; Moreno et al. 1997).
Preclinical and clinical evidences suggest that an enhancement in 5-HT function may be a common denominator in the therapeutic action of most antidepressant treatments (Blier et al. 1990; Charney et al. 1984). If TSD exerts its effect through an increase in brain 5-HT activity, the coadministration of pindolol should result in an enhanced antidepressant effect, similar to that observed with pindolol and serotonergic drugs.
The purpose of the present study was to evaluate the effect of the combination of TSD and pindolol in the treatment of acute episodes of bipolar depression.
METHODS
Patients
Eighty-six consecutively admitted inpatients diagnosed as bipolar disorder, type I, depressive episode without psychotic features (DSM-IV criteria) (American Psychiatric Association 1994) were screened. All patients were submitted to physical examinations, laboratory tests and electrocardiograms at admission in order to exclude pregnancy, history of epilepsy, major medical and neurological disorders, medical contraindications to the use of pindolol, history of drug or alcohol dependency or abuse within the last six months. Forty-six out of 86 patients were excluded: 9 because of additional diagnoses on Axis I, 1 because of mental retardation, 29 because of treatment with lithium salts or long-acting neuroleptic drugs in the last six months before admission or with neuroleptics or irreversible MAOIs in the last month before admission, 1 because of history of epilepsy, and 7 because of medical illnesses.
Forty patients met the selection criteria and gave their written informed consent to participate in the study. Previous treatments during the current episode were: SSRIs 8/40, tricyclic antidepressants 10/40, moclobemide 1/40, benzodiazepines 7/40, no medication 14/40.
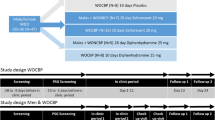
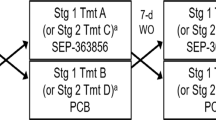
Study Design
Patients underwent a 7-day run-in period with single-blind placebo, during which semi-structured interviews based on DSM-IV for Axis I diagnoses were completed. After the run-in period, all patients had a 21-item Hamilton Depression Rating Scale (HDRS) (Hamilton 1960) score >18 and no response to placebo was observed.
Patients were randomly assigned to two treatment groups (day 0): TSD plus pindolol (Group 1, n = 20) or TSD plus placebo (Group 2, n = 20); randomization was performed by a computer generated schedule. All subjects were administered three TSD cycles, composed of a night of TSD followed by a recovery night. On days 1, 3, and 5 patients were totally deprived of sleep and had to stay awake for 36 hours, from 7:00 a.m. until 7:00 p.m. of the following day. They were then allowed to sleep during the night of days 2, 4, and 6 (Benedetti et al. 1996). From day 1 to day 9 patients were double-blind treated TID with pindolol 2.5 mg or placebo.
Patients’ perceived mood levels were rated by a self-administered 12.5 cm Visual Analogue Scale (VAS) [modified from Aitken (1969)] three times during the day (7 a.m., 1 p.m., and 7 p.m.) from day 1 to day 7. Patients could not see their previous self-ratings when administered VAS. Raw data were converted to a 0–100 rating scale, with 0, 50, and 100 denoting depression, normothymia, and euphoria, respectively. The patient's perceived mood level on each day was calculated as the mean of the three scores for that day.
The 21-item HDRS was administered by trained raters who were blind to treatment option at day 0 and at day 10 (i.e., four days after the last TSD cycle); whenever possible, the same rater conducted admission and following ratings for each patient. Severity of depression was rated over a one-day period except for item #16 (weight loss) which was rated over a period of one week.
Side effects were recorded using Dosage Records and Treatment Emergent Symptoms (DOTES) (NIMH 1976); blood pressure and pulse frequency were recorded three times a day by nursing staff.
If patients showed a complete response to treatment (defined as HDRS score <8 at day 10) and maintained it for the following week without medication, they started a mood stabilizing therapy with lithium carbonate (day 17) and their clinical status was monitored during the following six months (once a week during the first two months, and once a month during the following four). Lithium salts were up-titrated to reach therapeutic levels. Mean ± SD plasma lithium levels were .69 ± .07 after 1 month, .71 ± .06 after three months, and .67 ± .07 after six months. If patients did not respond or relapsed during the follow-up period, they were excluded from the study and administered a drug treatment upon clinical need.
Data Analysis
Baseline clinical and demographic characteristics between groups were compared using χ2 test (with Yates’ correction) and Student's t tests as appropriate. Changes in HDRS scores over time between groups were analyzed with a two-way repeated measures analysis of covariance, with time and treatment (pindolol or placebo) as independent variables, and age, number of previous episodes, and duration of current episode as covariates. Post hoc comparisons were performed with Scheffé test. Homogeneity of variances at time 0 was tested using Levene's test. VAS scores were compared with Student's t tests for independent samples. Between group differences in response rates at day 10 and in relapse rates during the follow up period were tested with χ2 test (with Yates’ correction). Computerized analyses were performed with a commercially available statistical package (Statistica 1993).
RESULTS
Clinical and demographic characteristics of two groups (Group 1 vs. Group 2) were as follows. Sex distribution: 8 males, 12 females vs. 7 males, 13 females; current age (mean ± SD): 44.90 ± 11.47 vs. 51.60 ± 11.97 years; age of onset: 30.90 ± 7.17 vs. 34.15 ± 11.66 years; duration of illness: 14.00 ± 10.60 vs. 17.45 ± 9.28 years; number of episodes: 5.70 ± 3.39 vs. 8.35 ± 5.14; duration of current episode: 8.50 ± 11.55 vs. 13.40 ± 10.84 weeks. No difference between the two groups was statistically significant.
Mean ± SD HDRS scores at day 0 were 24.65 ± 3.30 in Group 1 and 25.70 ± 5.28 in Group 2. Mean ± SD HDRS scores at day 10 were 6.60 ± 5.55 (26.8% of baseline values) in Group 1 and 16.55 ± 6.68 (64.4% of baseline values) in Group 2. Homogeneity of variances at time 0 was successfully tested (F = 1.39; df 1,38; p = 0.25). A two-way repeated measures analysis of covariance on HDRS scores showed a highly significant group effect (F = 13.59; df 1,35; p = .0008), a highly significant time effect (F = 159.89; df 1,35; p = .00001), and a highly significant time per group interaction (F = 17.12; df 1,35; p = .0002). Covariates did not significantly influence HDRS scores. Scheffé test showed a non significant difference between groups at baseline (p = 0.914) and significantly better scores for Group 1 at day 10 (p < .00001).
Mean VAS scores are plotted in Figure 1. A comparison between the two groups showed significant differences after the second TSD (day 4: Student's t = 2.92, df = 38, two-tailed p = .006) and after the last recovery night (day 7: t = 2.17, df = 38, p = .036).
Mean perceived mood levels (VAS scores) in the two groups during TSD treatment. Sleep deprivation schedule (TSD = total sleep deprivation; R = recovery night) is specified on the upper x axis. Scores significantly differed between groups (Student's t test; see levels of significance on the upper x axis) at day 4 and 7
At day 10, 15/20 Group 1 patients were rated as responders (HDRS score <8) versus 3/20 Group 2 patients (χ2 = 12.22, df 1, p = .0005) (Figure 2 ). One week after, 14/20 Group 1 and 1/20 Group 2 patients were still rated as responders (χ2 = 15.36, df 1, p = .0001) and started a mood stabilizing therapy with lithium salts.
No switch into manic phase was observed.
During the follow-up period, one Group 1 responder relapsed (4 weeks after the acute treatment).
No patient showed clinically relevant side effects during pindolol treatment, nor there was any drop out among the 40 patients enrolled into the study. Six patients joined to Group 1 (pindolol) complained hypotension; 4 patients (equally distributed into the two treatment groups) referred headache and 10 patients (8 assigned to pindolol group and 2 to placebo group) complained about a “scarcely restorative sleep” during the recovery nights, without insomnia. A two-way repeated measures analysis of variance showed that pindolol significantly reduced systolic (day 0 131.0 ± 21.7 mmHg; day 4 121.8 ± 26.1; day 9 120.3 ± 23.6) and diastolic blood pressure (day 0 83.8 ± 12.1; day 4 77.3 ± 13.0; day 9 76.0 ± 11.4) and pulse frequency (day 0 76.3 ± 7.7 bpm; day 4 73.2 ± 8.3; day 9 73.2 ± 7.7).
DISCUSSION
At the end of the acute treatment (day 10; i.e., four days after the last TSD cycle) 75% of bipolar depressed patients treated with coadministration of pindolol and TSD (versus 15% of patients treated with placebo and TSD) showed a complete response. One week after 70% and 5% of patients respectively were still rated as responders.
These data confirming the presence of a positive interaction between pindolol and TSD are in agreement with the hypothesis of a major role of 5-HT neurotransmission in the mechanism of action of TSD. Despite the clinical relevance of the effect, detailed psychobiologic explanations must be considered only hypothetical because of the still uncertain status of research about the neurochemical effects of TSD. Basing on the data on 5-HT function summarized in the introduction, pindolol could act sinergistically with TSD via two different but not alternative mechanisms: pindolol could directly enhance 5-HT turnover by blocking somatodendritic 5-HT1A autoreceptors; or pindolol could prevent the self-inhibiting activation of somatodendritic 5-HT1A autoreceptors due to increased 5-HT turnover in brain stem.
Since pindolol is also a beta-blocker, the possibility of a noradrenergic mechanism in explaining our findings cannot be excluded. Up to now no data are available on the interaction between beta-blocking drugs devoid of 5-HT1A antagonism and TSD. When given alone, however, beta-blocking drugs do not show antidepressant properties and can induce depressive symptomatology (e.g., Waal 1967; Petrie et al. 1982). Further researches employing more specific drugs will clarify this point.
Only one Group 1 responder relapsed during the six-month follow-up period. For ethical reasons, all responders were treated with lithium salts, and this is likely to have contributed to a sustained response. Lithium salts have been reported to have acute antidepressant properties in bipolar depression, possibly via a serotonergic mechanism (e.g., Price and Heninger 1994), and to acutely sustain the effect of sleep deprivation (e.g., Szuba et al. 1994). However, since lithium was administered only 11 days after the last TSD cycle, it could not interfere with the acute effect of TSD treatment.
A high rate of switch from depression into mania after TSD has been reported in rapid-cycling bipolar depressed patients (Wehr et al. 1982; Wehr 1992). Few data are available on the occurrence of switch after TSD in other diagnostic cathegories (see review in Wu and Bunney 1990). In the present study we did not observe switches into mania. The possibility of a switch from depression into mania should, however, be considered when treating bipolar depressed patients with antidepressant treatments (e.g., Solomon et al. 1990).
This is the first report about the effect of the combination of pindolol to TSD. American Psychiatric Association practice guidelines suggest the usefulness of sleep deprivation in the treatment of bipolar depression (American Psychiatric Association, 1995), but the high frequency of an early relapse after TSD and the difficulty to carry out the treatment have hampered a broad application of this technique. Whichever the exact mechanism of action, the combination of pindolol to TSD seems to resolve the relapse problem. Given the high response rates in the absence of important side effects, the rapidity of action in responders, and the short time needed to test its efficacy, the use of pindolol in combination with sleep deprivation may represent a tentative first choice therapy in the treatment of bipolar depression.
References
Aitken RCB . (1969): Measurement of feelings using visual analogue scale. Proc R Soc Med 62: 989–993
American Psychiatric Association. (1994): Diagnostic and statistical manual of mental disorders, fourth edition (DSM-IV). Washington, American Psychiatric Association Press
American Psychiatric Association. (1995): Practice guideline for treatment of patients with bipolar disorder. Washington, American Psychiatric Association Press
Artigas F, Perez V, Alvarez E . (1994): Pindolol induces a rapid improvement of depressed patients treated with serotonin reuptake inhibitors. Arch Gen Psychiatry 51: 248–251
Artigas F . (1995): Pindolol, 5-hydroxytryptamine, and antidepressant augmentation. Arch Gen Psychiatry 52: 969–970
Artigas F, Romero L, de Montigny C, Blier P . (1996): Acceleration of the effect of selected antidepressant drugs in major depression by 5-HT1A antagonists. TINS 19: 378–383
Asikainen M, Deboer T, Porkka-Heiskanen T, Stenberg D, Tobler I . (1995): Sleep deprivation increases brain serotonin turnover in the Djungarian hamster. Neurosci Lett 198: 21–24
Baxter LR, Liston EH, Schwartz JM, Altshuler LL, Wilkins JN, Richeimer S, Guze BH . (1986): Prolongation of the antidepressant response to partial sleep deprivation by lithium. Psychiatry Res 19: 17–23
Benedetti F, Barbini B, Campori E, Colombo C, Smeraldi E . (1996): Dopamine agonist amineptine prevents the antidepressant effect of sleep deprivation. Psychiatry Res 65: 179–184
Benedetti F, Barbini B, Lucca A, Campori E, Colombo C, Smeraldi E . (1997): Sleep deprivation hastens the antidepressant action of fluoxetine. Eur Arch Psychiat Clin Neurosci 247: 100–103
Berman RM, Darnell AM, Miller HL, Anand A, Charney DS . (1997): Effect of pindolol in hastening response to fluoxetine in the treatment of major depression: A double-blind, placebo-controlled trial. Am J Psychiatry 154: 37–43
Betts TA, Alford C . (1985): β-blockers and sleep: a controlled trail. Eur J Clin Pharmacol 28(Suppl):65–68
Blier P, Bergeron R . (1995): Effectiveness of pindolol with selected antidepressant drugs in the treatment of major depression. J Clin Psychopharmacol 15: 217–222
Blier P, de Montigny C, Chaput Y . (1990): A role for the serotonin system in the mechanism of action of antidepressant treatments: preclinical evidence. J Clin Psychiatry 51(4 Suppl):14–20
Charney DS, Heninger GR, Sternberg DE . (1984): Serotonin function and the mechanism of action of antidepressant treatment. Arch Gen Psychiatry 41: 359–365
Cramer H, Tagliamonte A, Tagliamonte P, Perez-Cruet J, Gessa GL . (1973): Stimulation of brain serotonin turnover by paradoxical sleep deprivation in intact and hypophysectomized rats. Brain Res 54: 373–375
Elsenga S, Van den Hoofdakker RH . (1982–1983): Clinical effects of sleep deprivation and clomipramine in endogenous depression. J Psychiatry Res 17: 361–374
Fornal CA, Jacobs BL . (1988): Physiological and behavioral correlates of serotonergic single-unit activity. In Osborne NN, Hamon M (eds), Neuronal serotonin. New York, Wiley & Sons, pp 305–345
Fornal CA, Metzler CW, Gallegos RA, Veasey SC, McCreary AC, Jacobs BL . (1996): WAY-100635, a potent and selective 5-hydroxytriptamine(1A) antagonist, increases serotonergic neuronal activity in behaving cats: Comparison with (S)WAY-100135. J Pharmacol Exp Ther 278: 752–762
Gardner JP, Fornal CA, Jacobs BL . (1997): Effects of sleep deprivation on serotonergic neuronal activity in the dorsal raphe nucleus of the freely moving cat. Neuropsychopharmacology 17: 72–81
Hamilton M . (1960): A rating scale for depression. J Neurol Neurosurg Psychiatry 23: 56–62
Hery F, Pujol JF, Lopez M, Macon J, Glowinski J . (1970): Increased synthesis and utilization of serotonin in the central nervous system of the rat during paradoxical sleep deprivation. Brain Res 21: 391–403
Hjorth S . (1993): Serotonin 5-HT1A autoreceptor blockade potentiates the ability of the 5-HT reuptake inhibitor citalopram to increase nerve terminal output of 5-HT in vivo: A microdialysis study. J Neurochem 60: 776–779
Holsboer-Trachsler E, Hemmeter U, Hatzinger M, Seifritz E, Gerhard U, Hobi V . (1994): Sleep deprivation and bright light as potential augmenters of antidepressant drug treatment: neurobiological and psychometric assessment of course. J Psychiatr Res 28: 381–399
Kostis JB, Rosen RC . (1987): Central nervous system effects of β-adrenergic-blocking drugs: The role of ancillary preperties. Circulation 75: 204–212
Kuhs H, Farber D, Borgstadt S, Mrosek S, Tolle R . (1996): Amitriptyline in combination with repeated late sleep deprivation versus amitriptyline alone in major depression. A randomised study. J Affect Dis 37: 31–41
Leibenluft E, Wehr TA . (1992): Is sleep deprivation useful in the treatment of depression? Am J Psychiatry 149: 159–168
Leonard CS, Llinàs R . (1994): Serotonergic and cholinergic inhibition of mesopontine cholinergic neurons controlling REM sleep: An in vitro electrophysiological study. Neuroscience 59: 309–330
Maudhuit C, Jolas T, Chastanet M, Hamon M, Adrien J . (1996): Reduced inhibitory potency of serotonin reuptake blockers on central serotoninergic neurons in rats selectively deprived of rapid eye movement sleep. Biol Psychiatry 40: 1000–1007
Monti JM, Jantos H . (1994): Stereoselective antagonism by the pindolol enantionmers of 8-OH-DPAT-induced changes of sleep and wakefulness. Neuropharmacology 33: 705–708
Moreno FA, Gelenberg AJ, Bachar K, Delgado P . (1997): Pindolol augmentation of treatment resistant depressed patients. J Clin Psychiatry 58: 437–439
National Institute of Mental Health Research (NIMH), Department of Education and Welfare. (1976): ECDEU Assessment Manual. Levin J, Guy W, eds. Rockville, MD, National Institute of Mental Health
Neckelmann D, Bjorkum AA, Bjorvatn B, Ursin R . (1996): Sleep and EEG power spectrum effects of the 5-HT1A antagonist NAN-190. Behav Brain Res 75: 159–168
Perez V, Gilaberte I, Faries D, Alvarez E, Artigas F . (1997): Randomised, double-blind placebo-controlled trial of pindolol in combination with fluoxetine antidepressant treatment. Lancet 349: 1594–1597
Petrie WM, Maffucci RJ, Woosley RL . (1982): Propanolol and depression. Am J Psychiatry 139: 92–94
Price LH, Heninger GR . (1994): Lithium in the treatment of mood disorders. N Engl J Med 331: 591–598
Romero L, Bel N, Artigas F, de Montigny C, Blier P . (1996): Effects of pindolol at pre and postsynaptic 5-HT1A receptors: In vivo microdialysis and electrophysiological studies in the rat brain. Neuropsychopharmacol 15: 349–360
Salomon RM, Delgado PL, Licinio J, Krystal JH, Heninger GR, Charney DS . (1994): Effects of sleep deprivation on serotonin function in depression. Biol Psychiatry 36: 840–846
Santos R, Carlini EA . (1983): Serotonin receptors activation in rats previously deprived of REM sleep. Pharmacol Biochem Behav 18: 501–507
Shelton RC, Loosen PT . (1993): Sleep deprivation accelerates the response to nortryptiline. Prog Neuropsychopharmacol Biol Psychiatry 17: 113–123
Solomon RL, Rich CL, Darko DF . (1990): Antidepressant treatment and the occurrence of mania in bipolar patients admitted for depression. J Affect Disord 18: 253–257
Szuba MP, Baxter LR, Altshuler LL, Allen EM, Guze BH, Schwartz JM, Liston EH . (1994): Lithium sustains the antidepressant effects of sleep deprivation: Preliminary findings from a controlled study. Psychiatry Res 51: 283–295
Statistica 4.5. Windows version. Tulsa, OK, StatSoft Inc., 1993
Tome MB, Isaac MT, Harte R, Holland C . (1997a): Paroxetine and pindolol: A randomized trial of serotonergic autoreceptor blocked in the reduction of antidepressant latency. Int Clin Psychopharmacol 12: 81–89
Tome MB, Cloninger CR, Watson JP, Isaac MT . (1997b): Serotonergic autoreceptor blockade in the reduction of antidepressant latency: Personality variables and response to paroxetine and pindolol. J Affect Disord 44: 101–109
Vogel GW, Vogel F, McAbee RS, Thurmond AJ . (1980): Improvement of depression by REM sleep deprivation. Arch Gen Psychiatry 37: 247–253
Waal HJ . (1967): Propanolol-induced depression. Br Med J 2: 50
Wehr TA, Goodwin FK, Wirz-Justice A, Brietmeier J, Craig C . (1982): 48-hour sleep-wake cycles in manic depressive illness. Naturalistic observations and sleep deprivation experiments. Arch Gen Psychiatry 39: 559–565
Wehr TA . (1992): Improvement of depression and triggering of mania by sleep deprivation. JAMA 267: 548–551
Wu JC, Bunney WE . (1990): The biological basis of an antidepressant response to sleep deprivation and relapse: Review and hypothesis. Am J Psychiatry 147: 14–21
Zanardi R, Artigas F, Franchini L, Sforzini L, Gasperini M, Smeraldi E, Perez J . (1997): How long should pindolol be associated with paroxetine to improve the antidepressant response? J Clin Psychopharmacol 17: 446–450
Zanardi R, Franchini L, Gasperini M, Lucca A, Smeraldi E, Perez J . (1998): Faster onset of action of fluvoxamine in combination with pindolol in the treatment of delusional depression: A controlled study. J Clin Psychopharmacol in press.
Acknowledgements
We thank Mrs P. Erba and all the nursing staff of our psychiatric ward for the precious assistance to the sleep deprivation procedure.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Smeraldi, E., Benedetti, F., Barbini, B. et al. Sustained Antidepressant Effect of Sleep Deprivation Combined with Pindolol in Bipolar Depression: A Placebo-Controlled Trial. Neuropsychopharmacol 20, 380–385 (1999). https://doi.org/10.1016/S0893-133X(98)00129-8
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1016/S0893-133X(98)00129-8