Abstract
The neurometabolic effects of the hallucinogen psilocybin (PSI; 0.2 mg/kg), the entactogen 3,4-methylenedioxyethylamphetamine (MDE; 2 mg/kg) and the stimulant d-methamphetamine (METH; 0.2–0.4 mg/kg) and the drugs’ interactions with a prefrontal activation task were investigated in a double-blind, placebo-controlled human [F-18]fluorodeoxyglucoseFDG-positron emission tomographicPET study (each group: n = 8). Subjects underwent two scans (control: word repetition; activation: word association) within 2–4 weeks. Psilocybin increased rMRGlu in distinct right hemispheric frontotemporal cortical regions, particularly in the anterior cingulate and decreased rMRGlu in the thalamus. Both MDE and METH induced cortical hypometabolism and cerebellar hypermetabolism. In the MDE group, cortical hypometabolism was more pronounced in frontal regions, with the exception of the right anterior cingulate, which tended to be hyperactive. Cognitive activation-related increases in left frontocortical regions were attenuated under all three psychoactive substances, but less so under MDE. Taking into account performance data and subjective reports on task difficulty, these effects may result from different mechanisms across the three groups. Our PSI data are in line with studies on acute schizophrenic patients suggesting frontal overactivity at rest, but diminished capacity to activate prefrontal regions upon cognitive demand. The MDE data support the hypothesis that entactogens constitute a distinct psychoactive substance class, which takes an intermediate position between stimulants and hallucinogens.
Similar content being viewed by others
Main
Experimental studies of cerebral blood flow and metabolism with psychoactive drugs in humans aim to explore the interaction of these drugs with human brain function. Recent studies with hallucinogenic, “mind-expanding” drugs in healthy subjects provided evidence in favor of an altered functional interhemispheric balance with right hemispheric dominance and an increased activity in frontocortical regions after acute administration of mescaline, psilocybin, or ketamine (Hermle et al. 1992; Vollenweider et al. 1997a, b). The most profound increase in metabolism was found in the anterior cingulate (Vollenweider et al. 1997a, b), which is linked to both emotional and attentional functions (Vogt et al. 1992; Devinsky et al. 1995; Murtha et al. 1996). These functions are, in turn, tightly connected to both the effects of hallucinogens and the symptoms of schizophrenic and schizophrenia-spectrum psychoses.
Hallucinogenic drug-induced states can be used as models for acute endogenous psychotic states in psychiatric research (Hermle et al. 1992; Vollenweider et al. 1997a, b; Gouzoulis-Mayfrank et al. 1998). Within the framework of this model psychosis paradigm neurometabolic data from the above-mentioned studies can be interpreted in the sense that acute psychotic states with prominent positive symptoms are linked to increased activity in frontal neocortical, and limbic areas. This is in contrast to the majority of functional neuroimaging studies with schizophrenic patients, which demostrate hypofrontality both in resting states (Buchsbaum et al. 1982; Farkas et al. 1984; Wolkin et al. 1988; Siegel et al. 1993) and under cognitive tasks believed to employ frontal brain areas (Cohen et al. 1987; Weinberger et al. 1988; Buchsbaum et al. 1990; Andreasen et al. 1992). However, most of these studies were performed with chronically ill patients on various neuroleptic medications, and evidence has accumulated in favor of an association between hypofrontality and negative symptoms (Volkow et al. 1987; Wolkin et al. 1992). Some few studies with acutely ill patients presenting with positive symptoms failed to demonstrate hypofrontality and did, in part, demonstrate hyperfrontal metabolic patterns (Sheppard et al. 1983; Wiesel et al. 1987; Cleghorn et al. 1989; Ebmeier et al. 1993; Parellada et al. 1994). Thus, a general link between acute, pharmacologically induced or naturally occurring psychotic states and hyperfrontal metabolic patterns may be hypothesized.
An important question is, whether the changes in cerebral activity demonstrated under hallucinogens are restricted to these substances. Several studies with other psychotropic substances with both stimulant and sedative properties (cocaine, morphine, benzodiazepines, barbiturates) reported decreased cortical activity (London et al. 1990a,b; Mathew and Wilson 1991). Studies on the effects of stimulant amphetamines are inconsistent with reports of decreases, no effects, or increases of glucose metabolism or cerebral blood flow (Wolkin et al. 1987; Kahn et al. 1989; Metz et al. 1991; Devous et al. 1995; Ernst et al. 1997). A recent study with intravenous d-amphetamine administration reported no global change, but frontal, limbic, subcortical, and cerebellar increases of regional glucose metabolic rates (Ernst et al. 1997). The discrepancies in functional neuroimaging studies with amphetamines may reflect the well-recognized variability of clinical amphetamine effects (Gunne 1977; Angrist 1994) and/or methodological differences among studies including samples (psychiatric patients, healthy controls), cognitive states (resting state, different cognitive tasks), imaging methods and indices of brain activity, as well as drugs, doses, and routes of administration. At present, no clear picture of stimulant amphetamine effects on cerebral activity can be drawn. Preliminary data from an ongoing study with an entactogenic amphetamine derivative (methylenedioxymethylamphetamine = MDMA) indicate that MDMA increases regional cerebral blood flow in prefrontal neocortical regions of the left hemisphere, while reducing it in the posterior cingulate, the right anterior cingulate, and the left caudate nucleus (Gamma et al. 1997). To our knowledge, this is the only experimental neuroimaging study on the acute effects of ecstasy in healthy nonuser subjects.
Recent studies with hallucinogens, entactogens, and stimulants were either open pilot studies or used placebo controls (Hermle et al. 1992; Lahti et al. 1995; Vollenweider et al. 1997a,b; Gamma et al. 1997). However, hallucinogens and entactogens exert very powerful effects in humans; thus, the nature of the administered agent mostly becomes apparent both for the subject and the researcher in the course of placebo-controlled experiments. Furthermore, hallucinogens exert very complex effects in humans, including alterations of perception, cognition, mood, and drive. Therefore, it is difficult to link distinct biological with psychological effects in subjects of placebo-controlled studies. To meet these methodological problems, designs with different psychoactive substances may be helpful.
The design of the present double-blind experimental study includes placebo and three psychoactive substances: the hallucinogen psilocybin, the stimulant d-methamphetamine, and the entactogen MDE (3,4-methylenedioxyethylamphetamine). Effects of entactogens (methylenedioxy-amphetamines = ecstasy group; e.g., MDMA, MDE, MBDB) are mainly emotional in nature, but they have additional significant perceptional and stimulant properties (Gouzoulis-Mayfrank et al. 1996; Pechnick and Ungerleider 1997). Several lines of evidence support the view of a distinct psychoactive substance class, which takes an intermediate position between stimulants and hallucinogens (Nichols 1986; Solowji et al. 1992; Hermle et al. 1993a, 1993b; Gouzoulis-Mayfrank et al. 1996). From a methodological point of view, the overlapping psychological effects of the three drug groups can help to realize a true double-blind design and may help to distinguish between mechanisms specifically related to hallucinogenic effects and mechanisms that pertain to other factors such as increased drive and energy (stimulant effects) and enhanced emotional responses (entactogenic effects).
The objectives of the study were the following:
1. to assess the effects of common recreational doses of psilocybin, MDE, and d-methamphetamine on regional cerebral glucose metabolism and to examine whether there are overlapping neurometabolic effects that correspond to the overlapping psychopathological effects of the drugs;
2. to detect correlations between neurometabolic and psychopathological effects of the drugs; and
3. to study the influence of the drugs on a cognitive activation.
The cognitive challenge was a word association task, compared to a word repetition task. We chose the word association task, because of the following considerations.
1. It is known from functional imaging studies that lateral prefrontal and frontal limbic cortical regions are employed in this task (Petersen et al. 1988). These regions have been shown to be involved in and to display metabolic alterations in both hallucinogenic states and endogenous psychoses (Benes and Bird 1987; Benes et al. 1987; Cleghorn et al. 1992; Liddle et al. 1992; Tamminga et al. 1992; Catafau et al. 1994; Lahti et al. 1995; Vollenweider et al. 1997a,1997b).
2. Hallucinogens induce formal thought disturbances with loosening of associations. Indirect semantic priming, an index of spreading activation in semantic networks, was reported to be increased in healthy volunteers after ingestion of psilocybin (Spitzer et al. 1996).
3. Disturbances of associations are considered a primary symptom of schizophrenia in the classical psychopathological literature (Bleuler 1911). Direct and indirect semantic priming were reported to be increased in thought-disordered schizophrenic patients (Manschreck et al. 1988; Kwapil et al. 1990; Spitzer et al. 1993).
For these reasons, the study of associative performance under hallucinogenic drugs is highly relevant within the frame of the model psychosis paradigm.
METHODS
The study was carried out in accordance with the Declaration of Helsinki and was approved by the local ethics committee of the Medical Faculty of the RWTH Aachen, the Federal Health Administration (BGA, Berlin), and the proper authorities for radiation protection (Bundesinstitut für Strahlenschutz).
Subjects
Thirty-two healthy subjects volunteered for this study (21 men, 11 women; mean age: 34.2 years, range: 27–47). All subjects were physicians (n = 25) or psychologists (n = 7) (self-experiments). They had no current or previous history of significant physical disease, no axis I or II disorders according to DSM-III-R criteria at present or in the past, no family history of major psychiatric disorder in first-degree relatives, and they received no regular medication. Each volunteer gave written informed consent. Before entering the study, subjects were screened by means of a standard psychiatric interview (SCID), a medical history, a clinical examination, electrocardiogram, and laboratory testing including blood cell counts, electrolytes, plasma kreatinin, and liver enzymes.
Substances
All substances were obtained from the Pharmaceutical Institute of the University of Tübingen, and were prepared as capsules of identical appearance. Psilocybin (PSI) and d-methamphetamine (METH) were obtained in 2.5- and 10-mg capsules. MDE was obtained in 100- and 10-mg capsules. The calculated individual dose for each subject was made available by combination of these capsules. If necessary, empty placebo (PLA) capsules were added, so that all volunteers received five capsules. The substances were administered orally with some water in the following doses: PSI: 0.2 mg/kg but not more than a 15-mg total dose (n = 8); MDE: 2 mg/kg but not more than 140-mg total dose (n = 8) ; METH: 0.2 mg/kg but not more than 17.5-mg total dose (n = 4). In an interim evaluation, this initial METH dose was shown to induce only slight clinical effects. Therefore, the METH dose was increased to 0.4 mg/kg but not more than 35-mg total dose. However, the final analysis of the data revealed no clear-cut differences in psychological and physiological effects between the two METH groups. Therefore, data of the two METH groups were pooled together for statistical analysis (n = 8).
Experimental Procedures and Cognitive Activation
Each subject participated in two experiments with the same substance in a double-blind design and pseudorandomized order (PSI, MDE, METH, PLA; each n = 8; total n = 32). The two experiments were performed 2–4 weeks apart. On either occasion, subjects performed a word association task (activation scan) or a word repetition task (control scan) in counterbalanced order. Fasting subjects arrived at the Psychiatric Department between 8:00 and 9:00 a.m. They had free access to water, otherwise they fasted until the end of the experiment. Veins on both lower arms were cannulated for subsequent blood takings. One experienced psychiatrist accompanied the subjects for the entire duration of the experiment and evaluated the psychopathological state. Drugs were administered orally with some water between 10:00 and 11:00 a.m., and subjects were allowed to relax afterward. Vital signs were measured regularly during the entire duration of the experiment. During the peak of the drug experience, subjects were transported to the Department of Nuclear Medicine within the same building. PET scans started 110 to 120 minutes after drug ingestion. All scans were performed in a quiet darkened room with eyes closed, the only background noise being that of the scanner. The headphones required for auditory presentation of task stimuli further attenuated the environmental noise. Stimuli were identical for the two tasks and were selected out of the most frequent nouns of the spoken German language (Ruoff 1990). Six hundred-forty words were recorded and delivered binaurally at a rate of one per 3 seconds over 32 minutes. The activation task consisted of overtly associating one word to every stimulus. The control task consisted of repeating every stimulus word. The words spoken by the subjects in both tasks were tape-recorded and analyzed. After the end of the scan, subjects were transported back to the Psychiatric Department and remained there for at least 2 hours after complete decline of the psychological effects.
Imaging Protocols (MRI and PET)
Magnetic resonance imaging (MRI) was performed on a day before the first experiment with a circular polarized Helmholtz headcoil in a 1.5 Tesla Magnetom (Siemens, Erlangen, Germany). Using a T1-weighted three-dimensional (3-D) flash sequence (TE 5 ms, TR 40 ms, flip angle 40°), a volume dataset of the brain was obtained and reconstructed in coronal, transaxial, and sagittal slices of 3-mm thickness. Positron emission tomography (PET) examinations were performed using an ECAT 953/15 Scanner (Siemens/CTI, Knoxville, TN, USA). A special head holder system and a thermoplastic head mask enabled fixation of the subject's head in the same position in all three examinations (Kaiser et al. 1994). The activation task (word repetition or word association) started 2 minutes before intravenous administration of 132-307 MBq fluorine-18-deoxyglucose (18-FDG), and lasted 32 minutes. Emission scans started 30 minutes PI and were taken for 30 minutes in three successive bed positions, because the scanner had an axial field of view of 5.4 mm. To correct for photon attenuation, a 15-minute transmission scan using eight Ge-68 ring sources was performed for each bed position on another day. The input function was calculated by determining the serum activity of arterialized venous blood samples over time (20 and 40 s; 1, 2, 4, 6, 8, 10, 20, 30, 40, and 60 min PI). Reconstruction of 45 transversal attenuation-corrected slices of 3.375-mm thickness in a 256 × 256 matrix was performed with a Hanning filter (cut-off frequency 0.5). Spatial resolution was 6-mm full width at half maximum (FWHM). Absolute glucose consumption rate was calculated for each pixel (autoradiography method according to Sokoloff et al. 1977 and Phelps et al. 1979) using measured input function, tissue radioactivity concentration, and blood glucose concentration. For quantification of gray and white matter, two sets of rate constants, K1–k4 and a lumped constant of 0.52 were used, according to Reivich et al. (1985).
Analysis of Image Data
After conversion of the data from MRI and PET to a uniform data file structure, data were transferred onto a computed system for image analysis (Unix system: SUN-SPARC 20). For exact realignment of MRI and PET data, a special multipurpose imaging tool was used (Pietrzyk et al. 1994). PET was adapted coronally, transaxially, and sagittally to MRI, and layer thickness was transformed uniformly to 6.75 mm. Using the anatomical atlas of Talairach and Tournoux (1988) cortical (frontal, parietal, temporal, and occipital) and subcortical (basal ganglia and thalamus) structures were defined on each individual MRI with regions of interest (ROIs), which were superimposed on the respective PET data as an MRI/PET overlay. All regions were defined for both the right and the left hemisphere. Altogether, 113 ROIs were defined on each MRI (55 ROIs per hemisphere and three brainstem ROIs). Each evaluated region exceeded the 2.5-fold volume of the FWHM of the PET scanner to minimize the influence of the partial volume effect. Because of the considerable intra- and interindividual variability of cerebral glucose metabolism, the absolute metabolic rate of glucose of each ROI (rMRGlu) was normalized to the global metabolic rate of glucose, which was calculated as the volume-weighted average of rMRGlu of all 113 evaluated regions (Bartlett et al. 1988; Maquet et al. 1990).
For further statistical analysis, the 113 ROIs per brain were summarized into 37 ROI groups: superior prefrontal, middle prefrontal, inferior prefrontal, frontal operculum, precentral, insula, parietal, temporoparietal, superior temporal, inferior temporal, occipital, cerebellum, caudate nucleus, putamen, thalamus, amygdala and parahippocampal cortex, anterior cingulate, posterior cingulate, and brain stem (Figure 1 ). Furthermore, volume-weighted average rMRGlu of larger, composite regions and metabolic ratios were calculated for each hemisphere and for both hemispheres together: frontal neocortex (composed of the three prefrontal ROIs, frontal operculum, precentral, and insula ROIs), posterior neocortex (composed of the parietal, temporal, and occipital ROIs), entire neocortex (composed of frontal and posterior neocortex), subcortical regions (composed of caudate nucleus, putamen, and thalamus), frontal/posterior ratio, and cortical/subcortical ratio.
Schematic presentation of the regions of interest (ROIs), as drawn on the individual MRI of one subject. Abbreviations: sPF: superior prefrontal cortex; mPF: middle prefrontal cortex; iPF: inferior prefrontal cortex; PC: precentral cortex; OP: frontal operculum; PA: parietal cortex; TP: temporoparietal cortex; TS: superior temporal cortex; TI: inferior temporal cortex; INS: insular cortex; CER: cerebellum; PU: putamen; CAU: caudate nucleus; THA: thalamus; AMY: amygdala/parahippocampal gyrus; GCA: anterior cingulate; GCP: posterior cingulate; Brst: brainstem.
Statistical Analysis
Differences in global and normalized regional MRGlu of the control scan between each drug group and placebo were analyzed by Mann–Whitney U-tests. The Spearman correlation coefficient was used to evaluate correlations between metabolic values and psychopathological scores. To limit the explored correlations to a reasonable number, only ROIs and ratios revealing significant or trend deviations from placebo were included in the correlation analyses. Changes in rMRGlu between association and repetition scans within each drug group were analyzed by means of the Wilcoxon matched pairs test. Differences in the total number of words produced in the association and repetition tasks between each drug group and placebo were analyzed by Mann–Whitney U-tests. Differences in the number of words produced in the three equal parts of the whole activation period were analyzed by Friedman tests and Wilcoxon matched pairs tests within each drug group. No type-I error correction for multiple testing was performed, because, with small n, no p value could pass the Bonferroni adjustment for multiple testing for dependent sample tests, in particular. Therefore, the findings should be regarded as exploratory, rather than confirmatory. All statistical analyses were performed with SPSS.
RESULTS
Global Cerebral Metabolism
There were no significant or trend differences of global cerebral metabolism in the four groups. Mean values and standard deviation of global glucose metabolism (μmol/100g/min) during the repetition scan were: PLA (n = 8): 37.58 ± 14.27; METH (n = 6): 32.59 ± 3.12; MDE (n = 7): 32.06 ± 10.23; PSI (n = 8): 31.49 ± 5.30. Missing values were because of technical problems with data acquisition.
Regional, Normalized Cerebral Metabolism
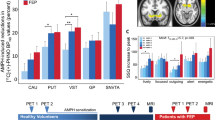
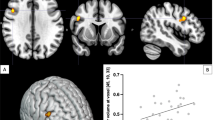
In the PSI group, significant increases of rMRGlu were obtained in the right anterior cingulate (+9.82%, p = .046) and the right frontal operculum (Broca homologous area of the right hemisphere) (+7.74%, p = .046), and a trend increase was seen in the right inferior temporal region (+4.16%, p = .093) compared to placebo. Significant decreases were obtained in the right thalamus (−8.73%, p = .016) and the left precentral region (−6.13%, p = .016), and a trend decrease was obtained in the left thalamus (−5.62%, p = .093) (Figure 2 ).There were trend decreases of rMRGlu in the composite right hemispheric and bilateral subcortical regions (right: −4.87%, p = .093, bilateral: −4.69%, p = .093), and a trend increase of the cortical/subcortical ratio of the right hemisphere (+5.05%, p = .074) (Figure 3 ).
Differences of rMRGlu in ROIs between each of the three drug groups and the placebo group in the control scan.  : right hemisphere, ▪: left hemisphere. Abbreviations: sPF: superior prefrontal cortex; mPF: middle prefrontal cortex; iPF: inferior prefrontal cortex; PC: precentral cortex; OP: frontal operculum; PA: parietal cortex; TP: temporoparietal cortex; TS: superior temporal cortex; TI: inferior temporal cortex; INS: insular cortex; CER: cerebellum; PU: putamen; CAU: caudate nucleus; THA: thalamus; AMY: amygdala/parahippocampal gyrus; GCA: anterior cingulate; GCP: posterior cingulate; Brst: brainstem; *: significant deviation (p < .05); (*): trend deviation (p < .1, Mann–Whitney U-test) from placebo.
: right hemisphere, ▪: left hemisphere. Abbreviations: sPF: superior prefrontal cortex; mPF: middle prefrontal cortex; iPF: inferior prefrontal cortex; PC: precentral cortex; OP: frontal operculum; PA: parietal cortex; TP: temporoparietal cortex; TS: superior temporal cortex; TI: inferior temporal cortex; INS: insular cortex; CER: cerebellum; PU: putamen; CAU: caudate nucleus; THA: thalamus; AMY: amygdala/parahippocampal gyrus; GCA: anterior cingulate; GCP: posterior cingulate; Brst: brainstem; *: significant deviation (p < .05); (*): trend deviation (p < .1, Mann–Whitney U-test) from placebo.
Differences of rMRGlu in composite ROIs and ratios between each of the three drug groups and the placebo group in the control scan. ▪: right hemisphere, ▪: left hemisphere, □ : right and left hemisphere. Abbreviations: PSI: psilocybin; METH: d-methamphetamine; fr C: frontal neocortex; post C: posterior neocortex; C: entire neocortex; subc: subcortical regions; fr C/post C: ratio frontal/posterior cortex; C/subc: ratio cortical/subcortical regions; *: significant deviation (p < .05); (*): trend deviation (p < .1, Mann–Whitney U-test) from placebo.
In the MDE group, metabolic decreases were seen in the left precentral (−7.14%, p = .021) and the right superior prefrontal (−4.58%, p = .037) region. Inspection of mean values revealed a numerical tendency toward metabolic decreases in additional frontal regions (prefrontal, precentral, and insula regions of both hemispheres), except for the frontal operculum (Figure 2). Metabolic increases were found bilaterally in the cerebellum (right: +10.12%, p = .002, left: +7.59%, p = .028) and the right putamen (+6.21%, p = .049). A trend increase of rMRGlu was found in the right anterior cingulate (+7.26%, p = .064). Metabolism in the composite bilateral frontal neocortex and entire neocortex was significantly reduced as compared to placebo (frontal neocortex: −3.19%, p = .006, entire neocortex: −1.58%, p = .037) (Figure 3).
In the METH group, trend decreases of rMRGlu were obtained in the right hemispheric parietal (−6.80%, p = .071), temporoparietal (−5.85%, p = .093), precentral (−5.62%, p = .093), and superior prefrontal (−4.55%, p = .093) ROIs, and metabolic increases were obtained bilaterally in the cerebellum (left: +10.52%, p = .039, right: +9.91%, p = .020) (Figure 2). rMRGlu in the composite bilateral entire neocortex region was slightly, but significantly, reduced (−1.69%, p = .045). Trend decreases were also found in the composite right frontal (−3.48%, p = .053) and bilateral posterior neocortical (−1.74%, p = .071) regions and in the right hemispheric and bilateral cortical/subcortical ratio (right: −6.50%, p = .071, bilateral: −4.98%, p = .093) (Figure 3).
Metabolic values of ROIs and composite regions and ratios displaying significant or trend changes from placebo are summarized in Table 1. Representative scans of single subjects on PLA, PSI, MDE, and METH are shown in Figure 4 .
Representative transaxial FDG-PET images of single subjects under placebo, psilocybin, MDE, and d-methamphetamine while performing a word repetition task. Note the shifted right/left asymmetry, the increased activity of the anterior cingulate and the decreased thalamic activity in the psilocybin subject. Note the decreased cortical and increased cerebellar activity in the MDE and d-methamphetamine subjects.
Correlations Between rMRGlu (Repetition Scan) and Psychopathological Signs
ROIs, composite ROIs, and ratios exhibiting significant or trend deviations from placebo were correlated with psychopathology variables using the following psychometric scores: PANSS Positive Symptom, Negative Symptom, and General Psychopathology scale, and single items P1–7, N1–7, G2, G4, G6, and G11 (Kay et al. 1987); Bech Rafaelsen Mania and Melancholia Scales BRMAS and BRMES (Bech 1988); State anxiety inventory STAI-X1 (Laux et al. 1981); and Hallucinogen rating scale HRS with the subscales: somatesthesia, affect, perception, cognition, volition, intensity, and single items 35 (happy) and 36 (unhappy) (Strassman et al. 1994). Spearman correlation coefficients ranged from 0.00 to 1.00. Significant correlations are summarized in Tables 2, 3, and 4.
In the PSI group, increase of activity in the right anterior cingulate correlated positively with stereotyped thoughts (PANSS N7) and negatively with anxiety (STAI-X1). Increase of metabolism in the right frontal operculum correlated negatively with general activation (BRMAS). Decrease of metabolism in the left thalamus was associated with high general psychopathology (PANSS), tension, anxiety (PANSS G4 and G2) and depressive mood (BRMES) and less stereotyped thoughts (PANSS N7). Decrease of rMRGlu in the composite bilateral subcortical region was also associated with high tension (PANSS G4) and less stereotyped thoughts (PANSS N7).
In the MDE group, cerebellar hypermetabolism correlated with diminished will (HRS volition scale), depressive mood (PANSS G6), cognitive deficits (HRS cognition scale), and anxiety (PANSS G2). Increased metabolism in the right anterior cingulate correlated with attentional deficits (PANSS G11). Decreased metabolism in the left precentral ROI was associated with general psychopathology (PANSS). Decreased rMRGlu in the composite frontal cortex region was associated with cognitive deficits (HRS cognition scale), and decrease in the entire cortex with general psychopathology (PANSS), depressive mood (BRMES, PANSS G6), anxiety (PANSS G2), and somatic sensations (HRS somatesthesia scale).
In the METH group, cerebellar hypermetabolism correlated positively with anxiety (STAI-X1) and negatively with feelings of happiness (HRS A35). Hypometabolism in the right precentral and parietal regions and in the right composite frontal region and diminished cortical/subcortical ratios were associated with cognitive deficits (HRS cognition scale) and anxiety (STAI-X1). Hypometabolism in the posterior cortex was associated with the global intensity of the drug experience (HRS intensity scale), positive symptoms (PANSS), general psychopathology (PANSS), manic state (BRMAS), grandiosity (PANSS P5), tension (PANSS G4), agitation (PANSS P4), hostility (PANSS P7), and thought disturbance (PANSS P2). Global cortical hypometabolism was associated with diminished feelings of happiness (HRS A35).
Metabolic Changes in the Activation vs. Control Scan (Word Association vs. Repetition)
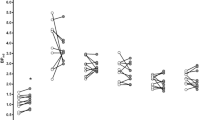
In the PLA group, cognitive activation with the word association task induced significant metabolic increases in the left frontal operculum (Broca region) (+7.13 ± 6.27%, p = .035), the left insula (+5.30 ± 6.16%, p = .025), the left middle prefrontal (+3.51 ± 4.11%, p = .05), and the right occipital region (+1.32 ± 1.75%, p = .05) and a decrease of rMRGlu in the left posterior cingulate (−5.30 ± 4.37%, p = .017). A trend decrease was found in the right superior prefrontal region (−2.37 ± 3.93%, p =.093) (Figure 5 ).
Cognitive activation-related changes of rMRGlu in ROIs (association vs. repetition scan; mean ± SD). ▪: right hemisphere, ▪: left hemisphere. Abbreviations: PLA: placebo; PSI: psilocybin; METH: d-methamphetamine; sPF: superior prefrontal cortex; mPF: middle prefrontal cortex; iPF: inferior prefrontal cortex; PC: precentral cortex; OP: frontal operculum; PA: parietal cortex; TP: temporoparietal cortex; TS: superior temporal cortex; TI: inferior temporal cortex; INS: insular cortex; CER: cerebellum; PU: putamen; CAU: caudate nucleus; THA: thalamus; AMY: amygdala/parahippocampal gyrus; GCA: anterior cingulate; GCP: posterior cingulate; Brst: brainstem; *: significant change (p < .05); (*): trend change (p < .1, Wilcoxon test).
In the PSI group, activation in frontal regions was diminished. There was only a trend increase of rMRGlu in the left frontal operculum (Broca region) (+4.95 ± 6.05%, p = .075). In contrast, metabolism was decreased in the left posterior cingulate (−5.63 ± 5.20%, p = .028), the right putamen (−3.58 ± 2.65%, p = .046), the right anterior cingulate (−3.24 ± 3.36%, p = .046), and the right occipital region (−2.83 ± 3.68%, p = .028). A trend decrease was found in the left occipital region (−1.37 ± 2.10%, p = .075) (Figure 5).
In the MDE group, cognitive activation with the word association task induced significant metabolic increases in the left middle prefrontal (+4.48 ± 1.85%, p = .018), the left superior temporal (+4.55 ± 2.60%, p = .018), and the right caudate nucleus (+5.51 ± 3.36%, p = .018) and a decrease of rMRGlu in the right posterior cingulate (−7.09 ± 5.66%, p+.018). A trend increase was found in the left precentral region (+3.62 ± 4.86%, p = .091), and a trend decrease in the brainstem region (−6.05 ± 6.24%, p = .063) (Figure 5).
In the METH group, frontal activation was diminished and did not reach statistical significance in any region. A significant activation was found in the left thalamus (+4.57 ± 4.58%, p = .046) and a significant decrease of rMRGlu in the right amygdala/hippocampal region (−8.03 ± 5.15%, p = .028). In addition, there was a trend decrease in the right anterior cingulate (−2.18 ± 2.35%, p = .075) and a trend activation in the left caudate nucleus (+4.26 ± 4.74%, p = .075) (Figure 5).
Cognitive Performance
There were no differences in the total number of overtly spoken words in the repetition task (PLA: 98.7 ± 2.0 %, d-METH: 98.9 ± 1.9 %, MDE: 99.9 ± 0.1 %, PSI: 99.6 ± 0.5 % of the total number of possible words). In the association task, subjects on PSI produced significantly fewer words than the placebo group (PLA: 90.2 ± 8.9 %, PSI: 69.4 ± 17.8 %, p = .016). Subjects on MDE produced slightly fewer, and subjects on METH produced slightly more words than the placebo group (MDE: 87.4 ± 11.3 %, METH: 95.6 ± 6.5 %); however, these differences were not significant. There were no significant differences in any group between the number of words produced in the three equal parts of the whole activation periods.
DISCUSSION
Thirty-two healthy volunteers participated in a double-blind neurometabolic study with FDG-PET under psilocybin, MDE, d-methamphetamine, or placebo (n = 6–8 each). Subjects underwent two PET scans on two different occasions while performing a word association or a control word repetition task. This study has some limitations: the number of subjects per drug group is small; statistical analysis includes no correction for multiple testing; drugs were given only in single medium doses, thus permitting no evaluation and comparison of possible effects of the drugs at higher doses; and, finally, the methamphetamine dose was increased during the course of the study because of limited clinical effects. These limitations are related to the apparent difficulties in planning and performing human studies with restricted drugs. Thus, our study must be viewed as a pilot investigation and our results as exploratory. Furthermore, because of the cumulative drug and radiation exposure no third scan under resting conditions was performed. Therefore, drug effects and effects of the word repetition task cannot be sorted out in our baseline control scan. However, resting state is a poorly defined mental condition. Especially under powerful psychoactive substances, resting states might represent completely different mental activities across subjects. Thus, a uniform mental activation with a simple cognitive task such as word repetition may, indeed, contribute to a better comparability of functional imaging scans across substances, beside being an adequate control for the cognitive activation of the association task.
Neurometabolic Effects of the Drugs and Correlations with Psychopathological Symptoms
The metabolic pattern under psilocybin was characterized by relative hypermetabolism in prefrontal and inferior temporal regions of the right hemisphere and relative hypometabolism in subcortical regions as compared to placebo. The most striking finding was a metabolic increase of nearly 10% in the right anterior cingulate. The thalamus and the left precentral region displayed diminished metabolic activity, and the right hemispheric cortical/subcortical ratio was increased. In the methamphetamine group, the most striking finding was an increased metabolic activity of about 10% in the cerebellum as compared to placebo. Otherwise, changes were somewhat opposite to the changes that occurred under psilocybin. There was a tendency for widespread cortical hypometabolism predominantly in right hemispheric frontal, parietal, and temporal regions, and the cortical/subcortical ratio was decreased. The MDE-induced metabolic effects were partly methamphetamine- and partly psilocybin-like. Methamphetamine-like effects included cerebellar hypermetabolism and cortical hypometabolism, which was more pronounced in frontal regions. Despite the over-all diminished frontal activity in the MDE group the right anterior cingulate tended to be hyperactive.
In the psilocybin group, increase of activity in the right anterior cingulate correlated positively with stereotyped thoughts and negatively with anxiety. Increase of metabolism in the right frontal operculum was associated with low general activation. Decrease of metabolism in the left thalamus was linked to general psychopathology, tension, anxiety, and depressive feelings, but less stereotyped thoughts. In the methamphetamine and MDE groups, increased cerebellar and diminished cortical activity were associated with anxiety, negative feelings, cognitive dysfunction, and general psychopathological signs. In the MDE group, both diminished activity in the composite bilateral frontal region and increased activity in the right anterior cingulate were associated with cognitive disturbances. In the methamphetamine group, hypometabolism in the posterior cortical regions was associated with a state of general activation and increased drive, but not with euphoria.
Our psilocybin findings are in line with data from other functional imaging studies with hallucinogens. Hermle et al. (1992) reported a hyperfrontal rCBF pattern under mescaline predominantly in the right hemisphere. In an H215O-PET study with schizophrenic patients under ketamine, Lahti et al. (1995) found an increase of rCBF in the anterior cingulate cortex and decreases in the hippocampus and visual cortex. Vollenweider et al. (1997a, 1997b) examined healthy volunteers and found hyperfrontal metabolic patterns and, particularly, an increased metabolism in the anterior cingulate under psilocybin and ketamine. The anterior cingulate cortex is traditionally viewed as one of the principal limbic structures and has been linked to numerous functions, such as selective attention, anticipation, motivation, emotion, maternal behavior, pain, and selection for action and motor reaction (Vogt et al. 1992; Devinsky et al. 1995; Murtha et al. 1996). An integrative view of cingulate function suggests that the anterior cingulate subserves primarily executive functions related to the emotional control of visceral, skeletal, and endocrine outflow (Vogt et al. 1992). Increased metabolism in the anterior cingulate seemed to be the common denominator of action across the hallucinogen psilocybin and the entactogen MDE. Profound sensory and emotional experiences absorbing the attention of subjects were present under both substances, but not under methamphetamine (Gouzoulis-Mayfrank et al. 1999, in press). Metabolic activity of the anterior cingulate correlated with stereotyped thoughts in the psilocybin group and with deficits of attention in the MDE group. Regarding the correlation data, increased cingulate metabolic activity may be interpreted as a compensatory effort to overcome the apparent difficulties in attending to, selecting, and processing the emotionally significant experiences in the drug states. Diminished metabolic activity in the thalamus was present only in the psilocybin group. Thalamic hypoactivity has not been reported before in studies with hallucinogens. However, in the study of Hermle et al. (1992), inspection of mean data suggests diminished rCBF under mescaline, although this finding was not significant. Furthermore, given the function of the thalamus as a sensory filter or “gate to consciousness” an underactivity of the thalamus intuitively seems to be in line with hallucinogenic states, which are characterized by an increased impressive mode of perception, sensory distortions, absorption by perceptional details, and hallucinations. However, in our correlation analyses, thalamic hypometabolism was not linked to perceptional changes, but rather to general aspects of the drug state, such as tension, anxiety, depressive mood, and other general psychopathological signs. An alternative interpretation of thalamic involvement in the psilocybin state may be provided by the numerous reciprocal connnections of the anterior cingulate and the “limbic” portions of thalamus (Bentivoglio et al. 1993). Changes within this circuitry are likely to influence more than one region. Further studies are needed to clarify the role of the thalamus in the pathophysiology of the hallucinogen-induced states.
From the viewpoint of the model psychosis paradigm, our results are in line with evidence in favor of an association between acute psychotic episodes and hyperactivity in frontal cortical regions (Wiesel et al. 1987; Szechtman et al. 1988; Cleghorn et al. 1989; Ebmeier et al. 1993; Parellada et al. 1994). These findings are in contrast with the hypofrontality, which has repeatedly been reported in studies with chronic schizophrenic patients (Buchsbaum et al. 1982; Farkas et al. 1984; Cohen et al. 1987; Volkow et al. 1987; Weinberger et al. 1988; Wolkin et al. 1988; Buchsbaum et al. 1990; Andreasen et al. 1992; Wolkin et al. 1992; Siegel et al. 1993). In addition, our data corroborate reports on alterations of interhemispheric balance in psychoses (Beaumont and Dimond 1973; Wexler and Heninger 1979; Magaro and Page 1983; West 1984; Gur et al. 1989) and suggest that a functional right hemispheric overactivity may be associated with acute endogenous or hallucinogen-induced psychotic syndromes (Oepen et al. 1987; Hermle et al. 1992). Finally, until recently, the thalamus has played a remarkably minor role in theories on the etiology of schizophrenia. However, evidence from recent studies with schizophrenic patients suggests disturbances in fronto-thalamo-cerebellar circuits (Andreasen 1997). The thalamus holds a key position in the recent integrative theory of “cognitive dysmetria” in the pathogenesis of schizophrenia (Andreasen et al. 1996).
Neocortical hypometabolism and cerebellar hypermetabolism were the common denominators of d-methamphetamine and MDE action. Diminished cortical activity has been described in several studies with both depressant and stimulant drugs of abuse such as benzodiazepines, morphine, amphetamines, and cocaine (Mathew and Wilson 1991; London et al. 1990a, 1990b; Wolkin et al. 1987) and has been viewed as a correlate of euphoria (London et al. 1990a, 1990b; Pearlson et al. 1993). However, in our studies, both cortical hypometabolism and cerebellar hypermetabolism were not associated with positive, but rather with unpleasant feelings such as anxiety and depression, cognitive disturbances, and general psychopathological signs. This finding is difficult to interpret, because MDE and d-methamphetamine elicited either minor or very pleasant emotional effects. Thus, secondary or compensatory mechanisms may be responsible for these neurometabolic effects. The change of cerebellar metabolic activity seems puzzling, because the cerebellum traditionally has been viewed as a motor control region. Increased cerebellar activity as a main psychoactive drug effect has been reported in only one study with tetrahydrocannabinol (Volkow et al. 1991). However, the view of the cerebellum as a motor organ has recently been challenged by a growing body of data on its involvement in mental operations such as selective attention, sensory discrimination, working memory, word processing, timing, learning, and complex problem solving (Akshoomoff and Courchesne 1992; Leiner et al. 1993; Gao et al. 1996; Gibbon et al. 1997; Allen et al. 1997), and in externally generated emotion (Reiman et al. 1997). Moreover, the role of the cerebellum in the pathogenesis of schizophrenic psychoses is the subject of current explorations (Andreasen et al. 1996). Given the enormous enlargement of the cerebellum during the last evolutional steps from nonhuman primates to humans, a broader view of cerebellar function including higher cognitive and emotional operations seems to be reasonable (Andreasen et al. 1996). The role of the cerebellum in psychoactive substance-induced states must be evaluated further.
Nevertheless, neurometabolic effects of MDE were not entirely methamphetamine-like in our study. Although cortical, and particularly frontocortical metabolic activity was diminished, the right anterior cingulate tended to be hyperactive under MDE. This is reminiscent of the psilocybin effects. Taken together, our data support the view that entactogens are a distinct psychoactive substance class, which takes an intermediate position between stimulants and hallucinogens. Furthermore, this conclusion is in line with studies of the psychopathological effects of the three substances (Gouzoulis-Mayfrank et al. 1999, in press). Given the strong emotional effects of MDE, we originally expected to find significant metabolic changes in the amygdala, a limbic region that has been repeatedly linked to the processing of emotional information (for reviews see LeDoux 1995; Rolls 1995). The lack of amygdala activation after ingestion of MDE may be partly attributable to the definition of ROIs, because our amygdala region included not only the amygdala, but also the hippocampus and parahippocampal gyrus. Moreover, a recent study demonstrated an association of amygdala activity only with externally, but not with internally generated emotion (film clips vs. recall of autobiographic material) (Reiman et al. 1997). Although the MDE state is clearly externally (i.e., pharmacologically) induced, the emotional changes taking place during this state may rather be viewed as internally generated. This might also explain the lack of amygdala activation in our study.
Interactions Between Cognitive Activation and Drugs
In the placebo group, the left hemispheric middle prefrontal, frontal operculum (Broca area), and insula regions were significantly activated in the association task. In addition, there was a slight, but significant, activation in the right occipital region and deactivations in the left posterior cingulate and the right superior prefrontal region (Schreckenberger et al. 1998). Metabolic increases of the frontal regions are in line with the classical 15O-H2O-PET studies of Petersen et al. (1988) with similar activation tasks. However, we were not able to demonstrate an activation of the anterior cingulate, as shown in latter studies. Moreover, metabolic changes in the posterior cingulate, occipital, and insular cortex have not been demonstrated before in the 15O-H2O-PET studies. The cognitive activation in 15O-H2O-PET studies typically lasts 2 to 3 minutes. In contrast, our subjects underwent a 32-min-long task, during which they had to respond to 640 words with an association. The equal numbers of associated and spoken words in the three- thirds of the activation period suggests that subjects were engaged with the task until the end of the period. This was also the case in the three substance groups. However, we might expect that cognitive mechanisms during a shorter task differ from those of a longer task that requires sustained attention. During the period of 32 minutes some automaticity may occur and novelty of the task may not be maintained. Thus, the discrepancies between our data and the data from 15O-H2O-PET studies may be partly caused by these differences in cognitive mechanisms because of differences in length of the tasks. This interpretation is in line with data from 15O-H2O-PET studies suggesting an activation of the anterior cingulate during demanding and novel, but not during well-practiced tasks (LaBerge 1990).
In the psilocybin group, the association task-related activation of middle prefrontal cortex was abolished, and the activation of Broca's area was attenuated. Decreases of metabolism were obtained not only in the left posterior cingulate, but also in the right anterior cingulate, occipital cortex, and right putamen. In the MDE group, metabolic increases were significant in the left middle prefrontal and superior temporal cortex as well as in the right caudate nucleus but not in Broca's area, and a metabolic decrease was found in the right posterior cingulate. In the methamphetamine group, metabolic increases did not reach statistical significance in any frontal region. Instead, there were activation-related metabolic increases in subcortical regions (left caudate nucleus and thalamus) and decreases in the right anterior cingulate and amygdala.
Taken together, our data suggest diminished frontal cortical activation by a classical frontal task in the psilocybin and methamphetamine group but less so in the MDE group. Because of the limited number of subjects and the fact that we did not correct for type I error, we refrain from interpreting metabolic alterations in regions outside the frontal cortex, which are not known to be employed in association tasks. The mechanisms of functional hypofrontality may vary in the different drug groups. First, in the methamphetamine and MDE groups, frontal cortical regions were found to be already hypoactive in the repetition scan, although this was not the case in the psilocybin group. Second, the subjective difficulty of the task was different across the drug groups. Although we did not collect these data systematically, most placebo subjects spontaneously reported that the task was “a little hard,” but manageable. Methamphetamine subjects did not report any difficulty with the task, while all but one subject on MDE reported that the task had been easy. In contrast, all but one subject on psilocybin spontaneously reported that the task had been very difficult, and they had had to concentrate hard to stay engaged with it. The total number of associated and spoken words was significantly smaller in the psilocybin group as compared to placebo, which is in line with the subjective difficulty of the task in this group. In contrast, subjects on methamphetamine produced slightly more words in the association task than subjects on placebo, although this difference was not significant. The number of associated and spoken words in the placebo group was about 90% of the total number of possible words. Hence, the lack of significance in that case may have been attributable to a ceiling effect (placebo: 90.2%, methamphetamine: 95.6%). Finally, subjects on MDE produced slightly, but not significantly, fewer words in the association task than did subjects on placebo. These data and observations suggest that different interpretations may be required to explain the diminished frontal activation upon cognitive demand across the different drug groups. In the case of methamphetamine, the subjective easiness and low level of engagement with the task may partly account for the diminished frontal activation, although performance was good. In the case of MDE, this may be also the case, although to a lesser extent. In the psilocybin group, engagement with the subjectively difficult task was high. Despite their high motivation and engagement, subjects on psilocybin did not succeed in activating prefrontal cortical areas sufficiently, and their performance was low.
In summary, subjects in the psilocybin model psychosis displayed hypermetabolism in distinct frontal cortical areas of the right hemisphere (anterior cingulate, frontal operculum) at baseline. However, their ability to increase metabolism in those frontal regions involved in language- and association functions in response to a suitable cognitive task was impaired. These data and data from other studies (Hermle et al. 1992; Vollenweider et al. 1997a,b) suggest that frontal cortical regions may be diffusely hyperactive in hallucinogen states. However, focused frontal activation upon specific cognitive demand is impaired. Within the frame of the model psychosis paradigm, this view may be extended to naturally occurring acute psychotic episodes in schizophrenic and schizophrenia-like psychoses. This interpretation is in line with a recent SPECT study with acute schizophrenic patients in resting state and after a frontal cognitive activation (Catafau et al. 1994) and may help to integrate seemingly contradictory findings in the literature on the pathophysiology of frontal lobe dysfunction in schizophrenia.
References
Akshoomoff NA, Courchesne E . (1992): A new role for the cerebellum in cognitive operations. Behav Neurosci 106: 731–738
Allen G, Buxton RB, Wong EC, Courchesne E . (1997): Attentional activation of the cerebellum independent of motor involvement. Science 275: 1940–1943
Andreasen NC, Rezai K, Alliger R, Swayze VW, Flaum M, Kirchner P, Cohen G, O'Leary DS . (1992): Hypofrontality in neuroleptic-naive patients and in patients with chronic schizophrenia. Assessment with Xenon 133 single-photon emission computed tomography and the Tower of London. Arch Gen Psychiat 49: 943–952
Andreasen NC, O'Leary DS, Cizadlo T, Arndt S, Rezai K, Boles Ponto LL, Watkins GL, Hichwa RD . (1996): Schizophrenia and cognitive dysmetria: A positron-emission tomography study of dysfunctional prefrontal–thalamic-cerebellar circuitry. Proc Natl Acad Sci 93: 9985–9990
Andreasen NC . (1997): The role of the thalamus in schizophrenia. Can J Psychiat 42: 27–33
Angrist B . (1994): Amphetamine psychosis: Clinical variations of the syndrome. In Cho AK, Segal DS (eds), Amphetamine and its analogs. Pharmacology, Toxicology, and Abuse. San Diego, CA, Academic Press, pp 387–414
Bartlett EJ, Brodie JD, Wolf AP, Christman DR, Laska E, Meissner M . (1988): Reproducibility of cerebral glucose metabolic measurements in resting human subjects. J Cereb Blood Flow Metab 8: 502–512
Beaumont JG, Dimond SJ . (1973): Brain disconnection and schizophrenia. Br J Psychiat 123: 661–662
Bech P . (1988): Rating scales for mood disorders: Applicability, consistency, and construct validity. Acta Psychiat Scand 78: 45–55
Benes FM, Bird ED . (1987): An analysis of the arrangement of neurons in the cingulate cortex of schizophrenic patients. Arch Gen Psychiat 44: 608–616
Benes FM, Majocha R, Bird ED, Marotta CA . (1987): Increased vertical axon numbers in cingulate cortex of schizophrenics. Arch Gen Psychiat 44: 1017–1021
Bentivoglio M, Kultas-Ilinsky K, Ilinsky I . (1993): Limbic thalamus: Structure, intrinsic organization and connections. In Vogt BA, Gabriel M (eds), Neurobiology of Cingulate Cortex and Limbic Thalamus: A Comprehensive Handbook. Boston, Birkhäuser, pp 71–122
Bleuler E . (1911): Dementia praecox oder Gruppe der Schizophrenien. Leipzig-Wien, Deuticke. Transl. Ziskin J, Lewis ND (1950): Dementia Praecox or the Group of Schizophrenias. New York, Intern. University Press
Buchsbaum MS, Ingvar DH, Kessler R, Waters RN, Cappelletti J, van Kammen DP, King AC, Johnson JJ, Manning RG, Flynn RM, Mann LS, Bunney WE Jr, Sokoloff L . (1982): Cerebral glucography with positron tomography. Use in normal subjects and in patients with schizophrenia. Arch Gen Psychiat 39: 251–259
Buchsbaum MS, Nuechterlein KH, Haier RJ, Wu J, Sicotte N, Hazlett E, Asarnow R, Potkin S, Guich S . (1990): Glucose metabolic rate in normals and schizophrenics during the continuous performance test assessed by positron emission tomography. Br J Psychiat 156: 216–227
Catafau AM, Parellada E, Lomena FJ, Bernardo M, Pavía J, Ros D, Setoain J, Gonzalez-Monclús E . (1994): Prefrontal and temporal blood flow in schizophrenia: Resting and activation technetium-99m-HMPAO SPECT patterns in young neuroleptic-naive patients with acute disease. J Nucl Med 35: 935–941
Cleghorn JM, Garnett ES, Nahmias C, Firnau G, Brown GM, Kaplan R, Szechtman H, Szechtman B . (1989): Increased frontal and reduced parietal glucose metabolism in acute untreated schizophrenia. Psychiat Res 28: 119–133
Cleghorn JM, Franco S, Szechtman B . (1992): Toward a brain map of auditory hallucinations. Am J Psychiat 149: 1062–1069
Cohen RM, Semple WE, Gross M, Nordahl TE, DeLisi LE, Holcomb HH, King AC, Morihisa JM, Pickar D . (1987): Dysfunction in a prefrontal substrate of sustained attention in schizophrenia. Life Sci 40: 2031–2039
Devinsky O, Morrel MJ, Vogt BA . (1995): Contributions of anterior cingulate cortex to behavior. Brain 118: 279–306
Devous MD Sr, Trivedi MH, Gong W, Harris TS, Rush AJ . (1995): rCBF changes in limbic and limbically innervated brain regions in normal controls following oral amphetamine challenge. J Cereb Blood Flow 15: S829
Ebmeier KP, Blackwood DHR, Murray C, Souza V, Walker M, Dougall N, Moffoot AP, O'Carroll RE, Goodwin GM . (1993): Single-photon emission computed tomography with 99mTc-Exametazime in unmedicated schizophrenic patients. Biol Psychiat 33: 487–495
Ernst M, Zametkin AJ, Matochik J, Schmidt M, Jons PH, Liebenhauer LL, Hardy KK, Cohen RM . (1997): Intravenous dextroamphetamine and brain glucose metabolism. Neuropsychopharmacology 17: 391–401
Farkas T, Wolf AP, Jaeger J, Brodie JD, Christman DR, Fowler JS . (1984): Regional brain glucose metabolism in chronic schizophrenia. A positron emission transaxial tomographic study. Arch Gen Psychiat 41: 293–300
Gamma A, Buck A, Hell D, Vollenweider FX . (1997): 3,4-methylenedioxymethamphetamine (MDMA) alters the pattern of regional cerebral blood flow (rCBF) in drug-naive volunteers. Pharmacopsychiatry 30: 170
Gao J-H, Parsons LM, Bowler JM, Xiong J, Li J, Fox PT . (1996): Cerebellum implicated in sensory acquisition and discrimination rather than motor control. Science 272: 545–547
Gibbon J, Malapani C, Dale CL, Gallistel CR . (1997): Toward a neurobiology of temporal cognition: Advances and challenges. Curr Opin Neurobiol 7: 170–184
Gouzoulis-Mayfrank E, Hermle L, Kovar K-A, Sass H . (1996): The entactogens: Ecstasy (MDMA), Eve (MDE), and other ring-substituted ethamphetamine derivatives. A novel pharmacological class among the illicit designer drugs? Nervenarzt 67: 369–380
Gouzoulis-Mayfrank E, Thelen B, Hermle L, Sass H . (1998): History, rationale, and potential of human experimental hallucinogenic drug research in psychiatry. Pharmacopsychiatry 31 S2: 63–68
Gouzoulis-Mayfrank E, Thelen B, Habermeyer E, Kunert HJ, Kovar K-A, Hermle L, Spitzer M, Sass H . (1999, in press): Psychopathological, neuroendocrine and autonomic effects of 3,4-methylenedioxyethylamphetamine (MDE), psilocybin and d-methamphetamine in healthy volunteers. Results of an experimental double-blind placebo-controlled study. Psychopharmacology
Gunne L-M . (1977): Effects of amphetamines in humans. In Martin WR (ed), Drug Addiction II: Amphetamine, Psychotogen, and Marihuana Dependence. Handbook of Experimental Pharmacology, vol. 45/II. Berlin, Heidelberg, New York, Springer, pp 247–275
Gur RE, Resnick SM, Gur RC . (1989): Laterality and frontality of cerebral blood flow and metabolism in schizophrenia: Relationship to symptom specificity. Psychiatry Res 27: 325–334
Hermle L, Fünfgeld M, Oepen G, Botsch H, Borchardt D, Gouzoulis E, Fehrenbach RA, Spitzer M . (1992): Mescaline-induced psychopathological, neuropsychological, and neurometabolic effects in normal subjects. Experimental psychosis as a tool for psychiatric research. Biol Psychiat 32: 976–991
Hermle L, Gouzoulis E, Oepen G, Spitzer M, Kovar K-A, Borchardt D, Fünfgeld M, Berger M . (1993a): The significance of hallucinogenic research in psychiatry: History and present. Nervenarzt 64: 562–571
Hermle L, Spitzer M, Borchardt D, Kovar K-A, Gouzoulis E . (1993b): Psychological effects of MDE in normal subjects. Are entactogens a new class of psychoactive agents? Neuropsychopharmacology 8: 171–176
Kahn DA, Prohovnik I, Lucas LR, Sackeim HA . (1989): Disassociated effects of amphetamine on arousal and cortical blood flow in humans. Biol Psychiat 25: 755–767
Kaiser HJ, Sabri O, Wagenknecht G, Lege B, Hellwig D, Buell U . (1994): A method of correlating and merging cerebral morphology and function by a special head holder. Nuklearmedizin 33: 123–1261
Kay SR, Fiszbein A, Opler LA . (1987): The positive and negative syndrome scale (PANSS) for schizophrenia. Schizophr Bull 13: 261–276
Kwapil TR, Hegley DC, Chapman LJ, Chapman JP . (1990): Facilitation of word recognition by semantic priming in schizophrenia. J Abnorm Psychol 99: 215–221
LaBerge D . (1990): Thalamic and cortical mechanisms of attention suggested by recent positron emission tomographic experiments. J Cogn Neurosci 2: 358–372
Lahti AC, Holcomb HH, Medoff DR, Tamminga CA . (1995): Ketamine activates psychosis and alters limbic blood flow in schizophrenia. NeuroReport 6: 869–872
Laux L, Glanzmann P, Schaffner P, Spielberger CD . (1981): Das State-Trait-Angstinventar (STAI). Weinheim, Beltz
LeDoux JE . (1995): In search of an emotional system in the brain: Leaping from fear to emotion and consciousness. In Gazzaniga MS (ed), The Cognitive Neurosciences. Cambridge, MA, MIT Press, pp 1049–1061
Leiner HC, Leiner AL, Dow RS . (1993): Cognitive and language functions of the human cerebellum. TINS 16: 444–447
Liddle PF, Friston KJ, Frith CD, Hirsch SR, Jones T, Frackowiack RSJ . (1992): Patterns of cerebral blood flow in schizophrenia. Br J Psychiat 160: 179–186
London ED, Broussole EPM, Links JM, Wong DF, Cascella NG, Dannals RF, Sano M, Herning R, Snyder FR, Rippeton LR, Toung TJK, Jaffe HJ, Wagner HN Jr . (1990a): Morphine-induced metabolic changes in human brain: Studies with positron emission tomography and [fluorine 18] fluorodeoxyglucose. Arch Gen Psychiat 47: 73–81
London ED, Cascella NG, Wong DF, Phillips RL, Dannals RF, Links JM, Herning R, Grayson R, Jaffe JH, Wagner HN . (1990b): Cocaine-induced reduction of glucose utilization in human brain. A study using positron emission tomography and [fluorine 18]-fluorodeoxyglucose. Arch Gen Psychiat 47: 567–574
Magaro PA, Page J . (1983): Brain disconnection, schizophrenia, and paranoia. J Nerv Ment Dis 171: 133–140
Manschreck TC, Maher BA, Milavetz JJ, Ames D, Weisstein CC, Schneyder ML . (1988): Semantic priming in thought-disordered schizophrenic patients. Schizophr Res 1: 61–66
Mathew RJ, Wilson WH . (1991): Substance abuse and cerebral blood flow. Am J Psychiat 148: 292–305
Maquet P, Dive D, Salmon E, von Frenckel R, Franck G . (1990): Reproducibility of cerebral glucose utilization measured by PET and the (18F)-2-fluoro-2-deoxy-d-glucose method in resting, healthy human subjects. Eur J Nucl Med 16: 267–273
Metz JT, de Wit H, Cooper M . (1991): Amphetamine and regional cerebral metabolic rate: Effects of behavioral state and dose. J Cereb Blood Flow 11: S390
Murtha S, Chertkow H, Beauregard M, Dixon R, Evans A . (1996): Anticipation causes increased blood flow to the anterior cingulate cortex. Human Brain Mapping 4: 103–112
Nichols DE . (1986): Differences between the mechanism of action of MDMA, MBDB, and the classic hallucinogens. Identification of a new therapeutic class: Entactogens. J Psychoact Drugs 18: 305–313
Oepen G, Fünfgeld M, Höll T, Zimmermann P, Landis T, Regard M . (1987): Schizophrenia—An emotional hypersensitivity of the right cerebral hemisphere. Int J Psychophysiol 5: 261–264
Parellada E, Catafau AM, Bernardo M, Lomena F, Gonzalez-Monclus E, Setoain J . (1994): Prefrontal dysfunction in young acute neuroleptic-naive schizophrenic patients: A resting and activation SPECT study. Psychiat Res Neuroimag 55: 131–139
Pearlson GD, Jeffery PJ, Harris GJ, Ross CA, Fischman MW, Camargo EE . (1993): Correlation of acute cocaine-induced changes in local cerebral blood flow with subjective effects. Am J Psychiat 150: 495–497
Pechnick RN, Ungerleider JT . (1997): Hallucinogens. In Lowinson JH, Ruiz P, Millman RB, Langrod JG (eds), Substance Abuse. A Comprehensive Textbook, 3rd ed. Baltimore, MD, Williams & Wilkins, pp 230–238
Petersen SE, Fox PT, Posner MI, Mintun M, Raichle ME . (1988): Positron emission tomographic studies of the cortical anatomy of single-word processing. Nature 331: 585–589
Phelps HE, Huang SC, Hoffmann EJ, Selin C, Sokoloff L, Kuhl DE . (1979): Tomographic measurement of local cerebral glucose metabolic rate in humans with (F-18) 2-fluoro-2-deoxyglucose: Validation of a method. Ann Neurol 6: 371–388
Pietrzyk U, Herholz K, Fink G, Jacobs A, Mielke R, Slansky I, Wuerker M, Heiss WD . (1994): An interactive technique for three-dimensional image registration: Validation for PET, SPECT, MRI, and CT brain studies. J Nucl Med 35: 2011–2018
Reiman EM, Lane RD, Ahern GL, Schwartz GE, Davidson RJ, Friston KJ, Yun LS, Chen K . (1997): Neuroanatomical correlates of externally and internally generated human emotion. Am J Psychiat 154: 918–925
Reivich M, Alavi A, Wolf AP, Fowler J, Russell J, Arnett C, MacGregor RR, Shiue C, Atkins H, Anand A . (1985): Glucose metabolic rate kinetic model parameter determination in man: The lumped constant and rate constants for (18-F) fluorodeoxyglucose and (11-C) deoxyglucose. J Cereb Blood Flow Metab 5: 179–192
Rolls ET . (1995): A theory of emotion and consciousness, and its application to understanding the neural basis of emotion. In Gazzaniga MS (ed), The Cognitive Neurosciences. Cambridge, MA, MIT Press, pp 1091–1106
Ruoff A . (1990): Häufigkeitswörterbuch gesprochener Sprache. 2. Auflage. Tübingen, Max Niemeyer Verlag
Schreckenberger M, Gouzoulis-Mayfrank E, Sabri O, Arning Ch Schulz G, Tuttass T, Wagenknecht G, Kaiser HJ, Sass H, Buell U . (1998): Cerebral interregional correlations of associative language processing: a PET activation study using 18-FDG. Eur J Nucl Med 25: 1511–1519
Siegel BV, Buchsbaum MS, Bunney WE, Gottschalk LA, Haier RJ, Lohr JB, Lottenberg S, Najafi A, Nuechterlein KH, Potkin SG, Wu JC . (1993): Cortical-striatal-thalamic circuits and brain glucose metabolic activity in 70 unmedicated male schizophrenic patients. Am J Psychiat 150: 1325–1336
Sheppard M, Gruzelier J, Manchanda R, Hirsch SR, Wise R, Frackowiak R, Jones T . (1983): 15O-positron emission tomography scanning in predominantly never treated acute schizophrenics. Lancet 1983: 1448–1452
Sokoloff L, Reivich M, Kennedy C, Des Rosiers MH, Patlak CS, Pettigrew KD, Sakurada O, Shinobara M . (1977): The C-14-deoxyglucose method for the measurement of local cerebral glucose utilization: Theory, procedure, and normal values in the conscious and anesthetized albino rat. J Neurochem 28: 897–916
Solowji N, Hall W, Lee N . (1992): Recreational MDMA use in Sydney: A profile of “ecstasy” users and their experiences with the drug. Br J Addict 87: 1161–1172
Spitzer M, Braun U, Hermle L, Maier S . (1993): Associative semantic network dysfunction in thought-disordered schizophrenic patients: Direct evidence from indirect semantic priming. Biol Psychiat 34: 864–877
Spitzer M, Thimm M, Hermle L, Holzman P, Schneider F, Gouzoulis-Mayfrank E, Kischka U, Kovar KA . (1996): Increased activation of indirect semantic associations under psilocybin. Biol Psychiat 39: 1055–1057
Strassman RJ, Qualls CR, Uhlenhuth EH, Kellner R . (1994): Dose-response study of N,N-dimethyltryptamine in humans. II. Subjective effects and preliminary results of a new rating scale. Arch Gen Psychiat 51: 98–108
Szechtman H, Nahmias C, Garnett S, Firnau G, Brown GM, Kaplan RD, Cleghorn JM . (1988): Effects on neuroleptics on altered cerebral glucose metabolism in schizophrenia. Arch Gen Psychiat 45: 523–532
Talairach J, Tournoux P . (1988): Coplanar Stereotactic Atlas of the Human Brain. Stuttgart, Thieme
Tamminga CA, Thaker GK, Buchanan R, Kirkpatrick B, Alphs LD, Chase TN, Carpenter WT . (1992): Limbic system abnormalities identified in schizophrenia using positron emission tomography with fluorodeoxyglucose and neocortical alterations with deficit syndrome. Arch Gen Psychiat 49: 522–530
Vogt BA, Finch DM, Olson CR . (1992): Functional heterogeneity in cingulate cortex: The anterior executive and posterior evaluative regions. Cerebr Cortex 2: 435–443
Vollenweider FX, Leenders KL, Scharfetter C, Antonini A, Maguire P, Missimer J, Angst J . (1997a): Metabolic hyperfrontality and psychopathology in the ketamine model of psychosis using positron emission tomography (PET) and [18F]fluorodeoxyglucose (FDG). Euro Neuropsychopharm 7: 9–24
Vollenweider FX, Leenders KL, Scharfetter C, Maguire P, Stadelmann O, Angst J . (1997b): Positron emission tomography and fluorodeoxyglucose studies of metabolic hyperfrontality and psychopathology in the psilocybin model of psychosis. Neuropsychopharmacology 16: 357–372
Volkow ND, Wolf AP, Van Gelder P, Brodie JD, Overall JE, Cancro R, Gomez-Mont F . (1987): Phenomenological correlates of metabolic activity in 18 patients with chronic schizophrenia. Arch Gen Psychiat 144: 151–158
Volkow ND, Gillespie H, Mullani N, Tancredi L, Grant C, Ivanovic M, Hollister L . (1991): Cerebellar metabolic activation by Delta-9-tetrahydrocannabinol in human brain: A study with positron emission tomography and 18F-2-Fluoro-2-deoxyglucose. Psychiat Res Neuroimag 40: 69–78
Weinberger DR, Berman KF, Illowsky BP . (1988): Physiological dysfunction of dorsolateral prefrontal cortex in schizophrenia. III. A new cohort and evidence for a monoaminergic mechanism. Arch Gen Psychiat 45: 609–615
West ED . (1984): Right hemisphere dysfunction and schizophrenia. Lancet 11: 344
Wexler BE, Heninger GR . (1979): Alterations in cerebral laterality during acute psychotic illness. Arch Gen Psychiat 36: 278–284
Wiesel FA, Wik G, Sjögren I, Blomqvist G, Greitz T, Stone-Elander S . (1987): Regional brain glucose metabolism in drug-free schizophrenic patients and clinical correlates. Acta Psychiat Scand 76: 628–641
Wolkin A, Angrist B, Wolf A, Brodie J, Wolkin B, Jaeger J, Cancro R, Rotrosen J . (1987): Effects of amphetamine on local cerebral metabolism in normal and schizophrenic subjects as determined by positron emission tomography. Psychopharmacology 92: 241–246
Wolkin A, Angrist B, Wolf A, Brodie JB, Wolkin B, Jaeger J, Cancro R, Rotrosen J . (1988): Low frontal glucose utilization in chronic schizophrenia: A replication study. Am J Psychiat 145: 251–253
Wolkin A, Sanfilipo M, Wolf AP, Angrist B, Brodie JD, Rotrosen J . (1992): Negative symptoms and hypofrontality in chronic schizophrenia. Arch Gen Psychiat 49: 959–965
Acknowledgements
The authors thank Hiltrud Lindenblatt, Pharmaceutical Institute of the University of Tübingen, for the synthesis and supply of the psychoactive drugs. The authors also thank Klaus Willmes, Department of Neurology of the RWTH Aachen, for his helpful comments on the manuscript. Finally, we greatly acknowledge the assistance of Annette Schürkens in data management and statistics. Some of the results of this article form part of a doctoral dissertation of coauthor Christian Arning at the Medical Faculty of the RWTH Aachen (D 82). This study was supported by grants to the first author from the Deutsche Forschungsgemeinschaft (DFG Go 717/1-1) and from the Interdisciplinary Center for Clinical Research (IZKF) CNS at the Medical Faculty of the University of Technology, Aachen, Germany.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Gouzoulis-Mayfrank, E., Schreckenberger, M., Sabri, O. et al. Neurometabolic Effects of Psilocybin, 3,4-Methylenedioxyethylamphetamine (MDE) and d-Methamphetamine in Healthy Volunteers A Double-Blind, Placebo-Controlled PET Study with [18F]FDG. Neuropsychopharmacol 20, 565–581 (1999). https://doi.org/10.1016/S0893-133X(98)00089-X
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1016/S0893-133X(98)00089-X
Keywords
This article is cited by
-
Neuroimaging in psychedelic drug development: past, present, and future
Molecular Psychiatry (2023)
-
Psilocybin-induced changes in cerebral blood flow are associated with acute and baseline inter-individual differences
Scientific Reports (2023)
-
UNRAVELing the synergistic effects of psilocybin and environment on brain-wide immediate early gene expression in mice
Neuropsychopharmacology (2023)
-
Hallucinations and Hallucinogens: Psychopathology or Wisdom?
Culture, Medicine, and Psychiatry (2023)
-
A Research Domain Criteria (RDoC)-Guided Dashboard to Review Psilocybin Target Domains: A Systematic Review
CNS Drugs (2022)