Abstract
In the present study, we demonstrate that, in a concentration-dependent manner, M100907 (formerly MDL 100907, a highly selective 5-HT2A receptor antagonist and a purported atypical antipsychotic drug [APD]), but not its much less active stereoisomer M100009, completely prevents or markedly reverses the phencyclidine (PCP)-induced blockade of N-methyl-D-aspartate (NMDA) responses in pyramidal neurons of the medial prefrontal cortex (mPFC). Furthermore, the atypical APD clozapine, but not the typical APD haloperidol or raclopride (a selective dopamine D2,3 receptor antagonist), mimicked the action of M100907, preventing the PCP-induced effect. These results suggest that M100907 might be an antidote for treating the PCP-induced psychotomimetic state that closely resembles schizophrenia; they could also account for the antipsychotic potential of M100907. Furthermore, our results suggest that the prototype (clozapine) and a candidate (M100907) atypical APDs might be effective in ameliorating schizophrenic symptoms including cognitive and neuropsychological deficits, which are induced in humans who abuse PCP. We hypothesize that the ability of M100907 and clozapine to prevent or reverse the PCP-induced blockade of the NMDA receptor channel is attributed to their 5-HT2A receptors antagonizing property. Therefore, with further systematic studies, the ability of compounds to prevent or reverse PCP's blockade of NMDA responses may prove to be an effective electrophysiological model for screening potential atypical APDs and predicting their therapeutic efficacy in cognitive deficits.
Similar content being viewed by others
Main
The psychotomimetic state induced by the noncompetitive N-methl-D-aspartate (NMDA) receptor channel blockers, such as PCP and ketamine, in normal human subjects is thought to be a better model for schizophrenia than that produced by amphetamine. In humans, not only does PCP cause hallucinations and delusions, but it also causes an associated apathetic state and a type of formal thought disorder that are more distinctive features of schizophrenia (Allen and Young 1978; Javitt and Zukin 1991; Kristensen et al. 1992; Krystal et al. 1994; Malhotra et al. 1996, 1997a,b; Pearlson 1981). Furthermore, in schizophrenics, NMDA receptor antagonists produce an exacerbation of psychotic symptoms and cognitive impairment (Javitt and Zukin 1991; Lahti et al. 1995; Malhotra et al. 1996, 1997a,b). Cognitive deficits have also been observed in PCP- or ketamine-treated rats (Alessandri et al. 1989; Danysz et al. 1988; Jentsch et al. 1997a; Verma and Moghaddam 1996) and monkeys (Boyce et al. 1991; Jentsch et al. 1997b). In addition, unlike normal subjects, both schizophrenics (Ingvar and Franzen 1974; Weinberger et al. 1986, 1988; Weinberger and Berman 1996) and PCP-abusing humans (Hertzman et al. 1990; Wu et al. 1991) failed to activate frontal cortical regions during performance of frontal-dependent tasks. These observations form the foundation for the glutamate hypothesis of schizophrenia in which it is postulated that an aberrant glutamatergic neurotransmission, particularly NMDA receptor hypofunction, results in both the cognitive and the psychiatric manifestation of the disorder (Carlsson and Carlsson 1990; Deutsch et al. 1989; Kim et al. 1980; Moghaddam 1994; Olney and Farber 1995; Wachtel and Turski 1990).
Although typical APDs, which not only alleviate schizophrenic symptoms but also cause extrapyramidal side effects (EPS), are in general not very effective in treating PCP-induced psychoses (Allen and Young 1978; Pearlson 1981), evidence has been accumulating in animal studies to suggest that some APDs, particularly those atypical ones (which possess antipsychotic activity but lack EPS), are capable of reversing the PCP-induced effect. For example, the potency of a series of neuroleptics in blocking PCP-induced hyperlocomotion in rodents correlated with their affinity for 5-hydroxytryptamine2A (5-HT2A) receptors (Gleason and Shannon 1997; Maurel-Remy et al. 1995). Moreover, the atypical APDs clozapine and olanzapine have been shown to reverse noncompetitive NMDA antagonist-induced social withdrawal in rats (Corbett et al. 1995) and prevent MK-801 neurotoxicity (Farber et al. 1996). Clozapine also ameliorated a long-lasting cognitive deficit induced by repeated administration of PCP in monkeys (Jentsch et al. 1997b). In addition, clozapine, but not haloperidol, has been shown to improve PCP-induced impairment of performance in a water maze (Okuyama et al. 1997). Similarly, it has been demonstrated that clozapine and seroquel, but not haloperidol or risperidone, antagonize PCP-induced deficits in sensorimotor gating of the startle response (Bakshi et al. 1994; Keith et al. 1991; Swerdlow et al. 1996). In contrast, it has been reported that haloperidol reduces significantly both MK-801-induced popping and hyperactivity in mice (Rosse et al. 1995); haloperidol and raclopride, but not SCH 23390, reverse the disruptive effect of ketamine on spatial delayed alternation performance (Verma and Moghaddam 1996); both haloperidol and clozapine reverse PCP-induced increases in striatal neuron firing in free-moving rats (White et al. 1995). At present, the underlying mechanisms by which the aforementioned APDs reverse the PCP/ketamine-induced effect are not clear.
We have previously demonstrated that both clozapine and M100907 [R-(+)-α-(2,3-dimethoxyphenil)-1-[4-fluorophenylethyl)]-4-piperidinemethanol (Kehne et al. 1996; Sorensen et al. 1993); but not raclopride, markedly potentiate NMDA receptor-mediated neurotransmission in pyramidal cells of the mPFC and this effect is antagonized by the selective NMDA receptor antagonist D(−)-2-amino-5-phosphonopentanoic acid (d-AP5) (Arvanov and Wang 1998; Arvanov et al. 1997). Haloperidol was less effective than clozapine and M100907 in potentiating NMDA responses. Furthermore, M100907 and clozapine markedly potentiate; whereas, haloperidol depresses, glutamate neurotransmission elicited by electrical stimulation of the forceps minor (white matter) in the mPFC. The latter finding might be related to the fact that haloperidol, but not M100907 or clozapine, depresses the (±)-α-amino-3-hydroxy-5-methylisoxazole-4-propionic acid (AMPA)-induced response in a concentration dependent manner (Arvanov and Wang 1998; Arvanov et al. 1997). M100907 enhances the release of excitatory amino acids (EAAs) induced by NMDA or electrical stimulation of the forceps minor; EAAs, in turn, activate both NMDA and non-NMDA receptors, depolarize membrane potential, and remove the Mg2+ block of the NMDA receptor–ionophore complex, and thereby dramatically increasing NMDA-induced inward current by 350 to 550% in pyramidal cells (Arvanov and Wang 1998).
Based on our findings, we predict that M100907 is capable of preventing or reversing PCP-induced blockade of NMDA receptor–ionophore complex because: (1) the block of NMDA-induced inward current by ketamine/PCP is highly voltage-dependent; and (2) the onset/offset of ketamine/PCP's blockade of the NMDA receptor channel is a function of repeated presentations of the agonist (Honey et al. 1985; MacDonald et al. 1987). Therefore, experiments were designed to examine this possibility. For comparison, the ability of clozapine, haloperidol, raclopride, and M100009 to prevent/reverse PCP's effect was also investigated.
MATERIALS AND METHODS
Preparation of mPFC Slices
The techniques and procedures for preparation of rat mPFC slices and for standard intracellular recording of presumed pyramidal neurons have been described previously (Arvanov and Wang 1998; Arvanov et al. 1997). Briefly, male Sprague–Dawley rats were decapitated under halothane anesthesia, and their brains were removed and cooled in ice-cold artificial cerebrospinal fluid (ACSF). The coronal (transverse) slices of mPFC (450-μm thick) were cut in ice-cold ACSF containing (in mM: NaCl 117, KCl 4.7, CaCl2 2.5, MgCl2 1.2, NaHCO3 25, NaH2PO4 1.2 and D-glucose 11, aerated with 95% O2/5% CO2 (pH 7.4) and kept submerged at room temperature for at least 1 h to allow for recovery. A single slice was then transferred to a recording chamber (32°C). The chamber was continuously superfused with ACSF at a constant rate of 2 ml/min.
Intracellular Recording and Single-Electrode Voltage Clamp
The procedures for intracellular recording and single-electrode voltage clamp using an Axoclamp 2B amplifier have been described elsewhere (Arvanov and Wang 1998; Arvanov et al. 1997). Sharp electrodes were pulled on a horizontal puller (Model P-87, Sutter Instruments, San Rafael, CA) and filled with 4 M K-acetate or 3 M KCl (tip resistances 55–80 MΩ). In current-clamp mode, the bridge balance was continually monitored and adjusted as necessary. Single-electrode voltage clamp was achieved under discontinuous mode at a sampling rate of 5–6.2 KHz (30% duty cycle), gain of 2.5–5 nA/mV. The efficacy of voltage clamp, electrode “settling time,” and input capacitance neutralization at the head stage were continuously monitored on an oscilloscope. Current and voltage records were acquired using a D/A sampling and acquisition software (pClamp 6, Axon Instruments, Foster City, CA), filtered at 1 KHz, and analyzed off-line. Voltage and current signals were recorded on a Gould Easy Graph Thermal Recorder (TA 240) and two-channel video tape recorder (VR-10B Digital Data Recorder, Instrutech, Elmont, NY). During voltage clamp recordings, tetrodotoxin (TTX, 0.5 μM), glycine (1 μM), and bicuculline (5 μM) were routinely included in the ACSF. All cells were held at −60 mV to minimize activating IM and Ih (Halliwell and Adams 1982). The problems (e.g., space clamping) associated with this method in neurons with extended processes have been discussed elsewhere (Finkel and Redman 1985). As has been pointed out, these problems faced during single-electrode voltage clamp may be less acute when dealing with the relative changes following drug application (Madison et al. 1987; Schweitzer et al. 1993).
Except where noted, drugs were administered via the superfusion medium. PCP was administered in the ACSF for 5 min before repeated application of NMDA (see below). When the ability of M100907 and APDs to prevent PCP's effect was examined, these compounds were superfused 15 min before PCP and then continuously throughout the experiment. NMDA was applied by placing a microdrop (10 μl) of concentrated solution (1 mM with a dilution factor 1:100) on a marked spot in the inflow channel of the chamber (volume 1 ml) as previously described (Arvanov and Wang 1998; Arvanov et al. 1997). Repeated microdrop application of NMDA to the same pyramidal cell with an interapplication interval of approximately 15 min produced a consistent inward current, although the baseline current caused by NMDA varied from cell to cell (30–200 pA). Typically, two or three stable consecutive control responses to NMDA were obtained, the average of which was counted as the baseline of NMDA, prior to any drug tests.
Data Analysis
The percent modulation produced by APDs on NMDA-evoked responses was calculated by subtracting the baseline peak amplitude of the responses from that evoked by bath application of APDs. This value was then divided by the baseline response and multiplied by 100. The results were presented as mean ± SE. Paired t-tests and Student's t-tests were used; 0.05 was selected for testing the level of significance.
In addition, we used SAS’ PROC MIXED for our data analyses. The design of our experiments was as follows; within each cell a drug was given, and the effects were measured at multiple times. Each cell received one drug (or combinations of drugs), and the effect was measured at 15-min intervals. In this design, cells constituted one level of analysis, and the individual time measurements within cells constituted another. Such data are often referred to as repeated measures data. Because of the nature of the design, we have unbalanced data (i.e., some cells had more time measurements than others). Recently developed software such as SAS' PROC MIXED for multilevel modeling produces maximum likelihood estimates of the parameters and the variance covariance matrix of residuals (Bryk and Raudenbush 1992; Diggle 1988; Littell et al. 1996), which is superior to analysis of variance (ANOVA) with repeated measurements in handling unbalanced data.
One of the key assumptions of ANOVA is homoskedasticity of variances in the parameters under study. Because of heteroskedastic variances in the parameters studied, the analysis and significance tests were performed after applying transformations, which included log, square root, reciprocal square root, and reciprocal square (Zar 1996).
Drugs
The compounds raclopride, NMDA, QX 314, and bicuculline methchloride were all purchased from Research Biochemicals International (RBI, Natick, MA). TTX was purchased from Sigma Chemical Co. (St. Louis, MO). M100907 and M100009, clozapine, haloperidol, and PCP were generous gifts from Hoechst Marion Roussel, Inc. (Bridgewater, NJ), Sandoz (Hanover, NJ), McNeil Laboratories (Fort Washington, PA), and National Institute of Drug Abuse (NIDA, Rockville, MD), respectively.
The concentration of stock solution of drugs was prepared 1000-fold higher than that of the final target concentration. As previously described (Arvanov and Wang 1997), drugs were first dissolved in 50 to 100 μl of either 5% lactic acid (e.g., M100907 and haloperidol) or 99% DMSO (e.g., clozapine), and then brought to stock concentration by the addition of purified water. Some compounds were dissolved directly in purified water (e.g., TTX [citrate buffer], (−)-bicuculline methchloride, CNQX-HBC complex, glycine, PCP and raclopride).
RESULTS
Presumed Pyramidal Neurons in the mPFC
All experiments were routinely performed on presumed pyramidal neurons in layers V and VI of the mPFC, an area that contains a high density of both 5-HT2A and NMDA receptors (Blue et al. 1988; Dure and Young 1995; Mengod et al. 1990; Willins et al. 1997) and has been suggested to play a key role in the pathogenesis of schizophrenia (Goldman-Rakic and Selemon 1997; Weinberger and Lipska 1995). The mPFC is located medial to the forceps minor and can be easily identified in the slice.
A total of 58 presumed pyramidal cells has been recorded; the electrophysiological criteria for distinguishing presumed pyramidal versus nonpyramidal cells have been previously published (Arvanov et al. 1997; Cauli et al. 1997; Connors and Gutnick 1990; Kawaguchi and Kubota 1996; McCormick et al. 1985; Yang et al. 1996). Briefly, the interneurons were characterized by a brief spike duration (<1 ms at half-maximum spike amplitude) and a lack of pronounced spike-frequency adaptation in response to constant-current depolarizing pulses. In contrast, the pyramidal cells had a longer spike duration, particularly the second spike (1–3 ms at half-maximum spike amplitude), and showed a pronounced spike-frequency adaptation.
Effect of NMDA in Presumed Pyramidal Cells of the mPFC
As previously reported (Arvanov and Wang 1997; Arvanov et al. 1997), NMDA (10 μM) elicited excitatory postsynaptic potentials (EPSPs) followed by a membrane depolarization (amplitude, 12.6 ± 1.5 mV, range, 8–18 mV) and bursts of action potentials. In the voltage clamp mode, at the holding potential (Vh) of −60 mV, NMDA 10 μM produced an inward current of 30–200 pA (68 ± 8 pA, n = 57).
Effect of PCP on NMDA-Induced Response
We have found that bath application of PCP invariably produced a significant hyperpolarization (4 ± 2.1 mV, n = 17; p < .001, paired t-test) of membrane potential. Accordingly, to avoid interference of voltage-related alteration of ion channels, we have routinely used the techniques of a single-electrode voltage clamp. When the presumed pyramidal neuron was held at −60 mV, bath application of PCP for 5 min produced a dramatic blockade of NMDA responses in a concentration-dependent fashion Figures (1 and 2 ). PCP at 0.2 μM produced a marginal blockade of NMDA responses; whereas, at a concentration of either 1 or 5 μM, PCP completely blocked NMDA-induced inward current (Figure 2A). The blockade produced by 1 μM PCP was use-dependent; i.e., requiring depolarization and current flow (open channels) for block to occur. Thus, 1 μM PCP produced little effect on the initial inward current induced by NMDA (NMDA response was reduced by 15 ± 6.5%, n = 4, which was not significantly different from that of controls, p = .1, paired t-test), but dramatically reduced the second NMDA response by 91.5 ± 1.4% (n = 4, Figure 1A). The blocking effect of 5 μM PCP was less use-dependent, because the blockade of the first and second NMDA-induced inward current by 5 μM PCP reached 56 ± 5% and 98 ± 1.9% (n = 5), respectively. Both NMDA responses were significantly smaller than that of controls (p < .001, paired t-tests). The blockade lasted for 60 ± 15 (n = 4) and 110 ± 15 min. (n = 5) for 1 and 5 μM PCP, respectively, during repeated application of NMDA with an interapplication interval of 15 min (Figure 2A). Overall, there is a significant difference between the effect produced by 5 vs. 1 μM PCP (SAS Proc Mixed multilevel modeling, chi square = 50, df = 3, p < .0001) and between the effect produced by 1 vs. 0.2 μM PCP (SAS Proc Mixed multilevel modeling, chi square = 48.5, df = 5, p < .0001) on the time course of NMDA responses.
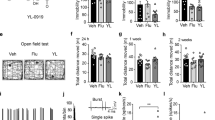
Representative current traces to illustrate that 100 nM M100907 effectively prevents and reverses PCP's blockade of NMDA responses. A: Administration of PCP 5 μM into the ACSF for 5 min partially blocked the first NMDA response and completely prevented the second NMDA responses, reflecting the use-dependent blockade of NMDA receptor-ionophore by PCP. The asterisk indicates that NMDA was applied repeatedly with an interapplication interval of 15 min. It took approximately 2 h for this neuron to recover from PCP's depressant effect. B: Perfusion of M100907 5 min before the administration of PCP and continuously throughout the experiment completely prevented PCP's effect. C: Administration of M100907 following PCP strikingly shortened the duration of the blockade of NMDA receptor channel by PCP.
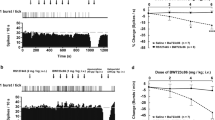
Diagrams illustrating that M100907, but not M100009, prevents and reverses the PCP-induced blockade of NMDA responses. A: PCP reduced and blocked NMDA-induced inward current in a concentration-dependent manner. B: In a concentration-dependent fashion, M100907 either prevented totally or reduced markedly the ability of PCP to block NMDA responses. C: M100907, but not M100009, was capable of reversing the PCP-induced blockade of NMDA responses, when it was administered (arrow) immediately following the onset of PCP's blockade. M100907 markedly reduced the duration of the blockade of NMDA responses by PCP.
As reported Previously (Honey et al. 1985; MacDonald et al. 1987), PCP-induced blockade of the NMDA receptor ion channel is voltage dependent. Thus, when the holding potential was at −40 and −20 mV, PCP produced little or no blockade of the NMDA-induced inward current (n = 3, not shown).
Comparison of Effects of M100907 and M100009 on PCP-Induced Blockade of NMDA Responses
When M100907 was administered 15 min before 5 μM PCP and then continuously throughout the experiment, it markedly reduced or completely prevented the PCP-induced blockade of the NMDA receptor-ionophore complex in a concentration-dependent manner (Figure 1B). Thus, at concentrations of 20 and 100 nM M100907 significantly reduced and completely abolished PCP's effect, respectively (SAS Proc Mixed multilevel modeling, chi square = 44.2 and 83.9, df = 6 and 3 for 20 and 100 nM M100907, respectively; p < .0001 for both concentrations); whereas 4 nM M100907 was without effect (SAS Proc Mixed multilevel modeling, chi square = 5.8, df = 8, p = .695; Figure 2B). Moreover, when M100907 (100 nM), but not the same concentration of M100009, was administered after PCP, it significantly shortened the duration of PCP's blockade of NMDA responses, reversing the PCP effect (50 ± 8 vs. 113 ± 7 min, t-test, p < .001). The recovery time course of PCP with the addition of M100907 is significantly different from that of PCP alone (SAS Proc Mixed multilevel modeling, chi square = 45, df = 2, p < .0001). In contrast, addition of M100009 did not significantly alter the recovery time course of PCP (SAS Proc Mixed multilevel modeling, chi square = 0.64, df = 2, p < .728; Figure 2C).
Comparison of Effects of M100009, M100907, Clozapine, Haloperidol, and Raclopride on PCP-Induced Blockade of NMDA Responses
We have examined and compared the ability of M100907, M100009, clozapine, haloperidol, and raclopride to prevent 1 μM PCP-induced blockade of NMDA responses. The concentration of 1 μM PCP was selected because it closely related to the serum and CSF PCP concentrations detected in humans (Donaldson and Baselt 1979; Pearlson 1981; Walberg et al. 1983). Moreover, 100 nM clozapine was only partially effective (50 ± 13%, n = 4) in preventing the blockade of NMDA responses by 5 μM PCP. The duration of the blockade of NMDA responses by 1 μM PCP lasted less than 65 min, which was too short to examine reliably the ability of the aforementioned compounds to reverse PCP's effect, using our paradigm of repeated application of NMDA at an interapplication interval of 15 min (see Figure 2A). We, therefore, compared the ability of these compounds to prevent PCP's action. The concentration of 100 nM was selected, because we have previously shown that the potentiation of NMDA-induced inward current in pyramidal cells of the mPFC produced by M100907 and clozapine has reached a plateau at this concentration.
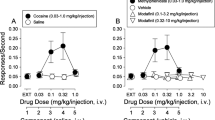
Figures 3 and 4 show that at the concentration of 100 nM, both M100907 (SAS Proc Mixed multilevel modeling, chi square = 65.4, df = 3, p < .0001) and clozapine (SAS Proc Mixed multilevel modeling, chi square = 63.6, df = 4, p < .0001), but not M100009, haloperidol, or raclopride, effectively prevented the PCP-induced blockade of NMDA responses (SAS Proc Mixed multilevel modeling and chi square tests, p > .05; Figure 4).
DISCUSSION
It has been previously reported that the blockade of the NMDA receptor channel by PCP and ketamine is highly voltage dependent, and the onset/offset of the blockade is dependent upon the exposure to agonists (Honey et al. 1985; MacDonald et al. 1987). Therefore, it is no surprise that M100907 is able to effectively antagonize the PCP-induced effect, because we have shown that M100907 enhances NMDA-induced release of EAAs, which activate both NMDA and non-NMDA receptors and depolarize membrane potential and remove Mg2+ blockade of the NMDA receptor channel, thereby potentiating strikingly NMDA responses (Arvanov and Wang 1998). Reminiscent of the action of M100907, the atypical APD clozapine, but not the typical APD haloperidol or raclopride, effectively potentiates the glutamatergic neurotransmission (Arvanov et al. 1997) and prevents the PCP-induced blockade of NMDA responses in pyramid cells of the mPFC. The application of either M100907 or clozapine alone did not alter resting membrane potential and input resistance of presumed pyramidal cells (Arvanov and Wang 1998; Arvanov et al. 1997). However, both clozapine and M100907 markedly potentiated NMDA-induced release of EAAs, which in turn acted upon primarily non-NMDA receptors and caused membrane depolarization, because the potentiating effect produced by M100907 and clozapine could be blocked by CNQX (Arvanov and Wang 1998; Arvanov et al. 1997). This action could account for the ability of these compounds to prevent PCP's blockade of the NMDA receptor channel, analogous to the removal of the Mg2+ blockade of the NMDA receptor channel by depolarization of the membrane potential (Arvanov and Wang 1998). Indeed, we have confirmed the previous finding that the PCP-induced blockade of the NMDA receptor ion channel is voltage dependent (Honey et al. 1985; MacDonald et al. 1987). Thus, when the holding potential was at −40 and −20 mV, PCP produced little or no blockade of the NMDA-induced inward current.
Haloperidol at the concentration of 100 nM also potentiated NMDA-induced inward current. However, haloperidol at concentrations of ⩾100 nM tended to hyperpolarize the membrane potential (Arvanov et al. 1997), which could contribute to the inability of haloperidol in preventing PCP's action.
At present, it is not clear how M100907 reversed PCP's effect by potentiating NMDA-induced release of EAAs if NMDA receptors have already been blocked. Perhaps at the concentration of PCP used in this study, the blockade of the NMDA receptor channel by PCP was incomplete. Even an initial small amount of EAAs being released by NMDA could gradually relieve PCP's blockade by depolarization of membrane potential (see above) and by further increasing the release of EAAs via activation of the glutamate autoreceptor-mediated positive feedback pathway (Arvanov and Wang, 1997; Berretta and Jones 1996; Connick and Stone 1988; Montague et al. 1994). M100907 might have potentiated NMDA-induced release of EAAs and facilitated the process of recovery. Repeated application of NMDA and enhanced release of EAAs should have helped the recovery process, because offset of the blockade of the NMDA receptor channel by PCP is dependent upon the exposure to agonists (Honey et al. 1985; MacDonald et al. 1987).
In agreement with our results are the recent reports indicating that clozapine, but not haloperidol, blunts NMDA antagonist-induced psychosis (Malhotra et al. 1997b; Lahti et al. 1995). The inability of haloperidol to affect PCP's blockade of NMDA responses is consistent with the observations that typical APDs are in general not very effective in treating PCP-induced psychosis (Allen and Young 1978; Pearlson 1981) and PCP-induced behavioral effects (see introductory paragraphs). In view of the dramatic ability of M100907 to prevent/reverse PCP's effect, it is suggested that M100907 may be used as an antidote for the PCP-induced psychotomimetic state; this may also account for, at least partly, the potential antipsychotic action of this compound (M100907 is currently under phase IIB clinical studies as a potential APD; personal communication, Dr. S. Sorensen, Hoechst Marion Roussel). On the other hand, the use of clozapine to treat the PCP-induced psychotomimetic state should be avoided, because it is less potent than M100907 and may lower seizure threshold and/or precipitate severe hypotension (Haller and Binder 1990; Pearlson 1981) and because of the danger of bone marrow toxicity.
As pointed out earlier, in addition to hallucination and delusion, PCP/ketamine induces schizophrenia-like cognitive and neuropsychological deficits, and causes thought disorder (Krystal et al. 1994; Malhotra et al. 1996, 1997a,b; Witkin 1995). Although it has been proposed that cognitive dysfinction in schizophrenia might result from underlying brain structural damage and cognitive symptoms are associated with the poor outcome of schizophrenia (Kay and Sevy 1990), the ability of PCP to induce reversible neuropsychological abnormalities suggests that a deficiency in NMDA receptor-mediated neurotransmission could be critically linked to cognitive and neuropsychological deficits seen in schizophrenia. The ability of the prototype (clozapine) and a candidate (M100907) atypical APD to prevent and reverse the PCP-induced blockade of NMDA responses strongly suggests that these compounds and perhaps other putative atypical APDs might be effective in ameliorating schizophrenic negative symptoms and potentially improving cognitive and neuropsychological deficits. Consistent with this view, we have recently demonstrated that M100907, but not M100009, enhances the induction of long-term potentiation (which has been regarded as a cellular basis for certain forms of learning and memory) in the synapses of CA1 cells of the hippocampal slices (Wang and Arvanov 1998). Moreover, there is supporting evidence that clozapine decreases negative symptoms and improves cognitive function (Fujii et al. 1997; Hagger et al. 1993; Lee et al. 1994; Meltzer 1995; Meltzer et al. 1996; but also see Breier et al. 1994; Goldberg and Weinberger 1994); whereas, typical APDs produced little improvement in negative symptoms and cognitive deficits in schizophrenia (Cassens et al. 1990; Lee et al. 1994).
It is likely that the ability of M100907 and clozapine to prevent or reverse the PCP-induced blockade of the NMDA receptor channel is the result of their 5-HT2A receptors antagonizing property because (1) M100907 is a highly selective 5-HT2A receptor antagonist (Kehne et al. 1996), and (2) clozapine and other putative atypical APDs are known to possess a relatively high affinity to 5-HT2A receptors (Meltzer et al. 1989), and they do not bind directly to the MK-801 site on the NMDA receptor-ionophore complex (Corbett et al. 1995; Lidsky et al. 1993; Lynch and Gallagher 1996; Tarazi et al. 1996). Moreover, neither the typical APD haloperidol nor the dopamine D2,3 ligand raclopride was capable of preventing/reversing PCP-induced blockade of NMDA responses, ruling out the possibility of a major role of dopamine D2,3 and σ receptors (to which haloperidol possesses a high affinity). In concordance with the present results, we have previously demonstrated that clozapine, but not haloperidol or sulpiride, potently blocks the action of the 5-HT2A,2C receptor agonist 1-(2,5-dimethoxy-4-iodophenyl)-2-aminopropane (DOI) in pyramidal cells of the mPFC (Ashby and Wang 1990). Furthermore, M100907, clozapine, and other 5 HT2A-related compounds (e.g., ketanserin, ritanserin, metergoline, and LY 53857), but not haloperidol or raclopride, are capable of potentiating, dramatically, NMDA receptor-mediated neurotransmission (Arvanov and Wang 1998; Liang and Wang unpublished observations). Although the mechanisms by which M100907 and 5-HT2 related compounds modulate glutamatergic neurotransmission are not clear, it is possible that the facilitation of release of EAAs by M100907 and 5-HT2 related compounds may play a major role in their modulatory action. Indeed, we have previously demonstrated that M100907 markedly facilitates NMDA-induced release of EAAs (Arvanov and Wang 1998), which is in consonant with the report showing that activation of presynaptic 5-HT2A receptors inhibits the release of glutamate from cerebellar mossy fiber terminals (Maura et al. 1991). Further systematic examination and comparison of the actions of 5-HT2A receptor antagonists on PCP-induced effect are needed to verify our hypothesis that the ability of M100907 and clozapine to prevent or reverse the PCP-induced blockade of the NMDA receptor channel is attributed to their 5-HT2A receptor antagonizing property.
If 5-HT2A receptors do play a predominant role in modulating PCP's blockade of the NMDA receptor channel, it might be speculated that atypical APDs, that are known to possess a relatively high affinity to 5-HT2A receptors (Meltzer et al. 1989), are a lot more effective than typical APDs in preventing/reversing PCP's blockade of the NMDA receptor channel, although further systematic examinations and comparisons of the ability of various typical and atypical APDs to prevent/reverse PCP's blockade of NMDA responses are needed to verify this view. In fact, this may prove to be an effective electrophysiological model for screening potential atypical APDs and predicting their effectiveness in alleviating some schizophrenic negative symptoms and improving neuropsychological and cognitive deficits.
It should be pointed out that controlled clinical studies of a 5-HT2A,2C receptor antagonist ritanserin in schizophrenia suggest only limited efficacy (Bleeker and Versleger 1990; Gelders et al. 1986). However, recent studies did suggest that ritanserin, either alone (Wiesel et al. 1994) or added to stable treatment with neuroleptics (Duinkerke et al. 1993), may have clinically significant efficacy. The poor efficacy of ritanserin as an APD has been attributed to several factors, including the dose restriction of ritanserin and the potentially propsychotic properties of ritanserin (Martin et al. 1997). A more definitive conclusion on whether a pure 5-HT2A antagonist is an effective APD will have to await the results from clinical studies of M100907.
In conclusion, in the present study, we have demonstrated that both M100907 and clozapine, but not M100009, haloperidol or raclopride, effectively prevent the PCP-induced blockade of the NMDA responses in pyramidal cells of the mPFC. Our results support the hypothesis that M100907 might be an effective atypical APD, and it might be an antidote for the PCP-induced psychotomimetic state in humans. It will be of great interest to determine whether our findings can be generalized to other atypical APDs; this may represent a new electrophysiological model for screening potential atypical APDs and predicting the effectiveness of these compounds for treating negative symptoms and neuropsychological and cognitive deficits associated with schizophrenia.
References
Alessandri B, Battig K, Welzl H . (1989): Effects of ketamine on tunnel maze and water maze performance in the rat. Behav Neural Biol 52: 194–212
Allen RM, Young SJ . (1978): Phencyclidine-induced psychosis. Am J Psychiatry 135: 1081–1084
Arvanov VL, Wang RY . (1997): NMDA-evoked response in pyramidal neurons of the rat medial prefrontal cortex slices consists of NMDA and non-NMDA components. Brain Res 768: 361–364
Arvanov VL, Wang RY . (1998): M100907, a selective 5-HT2A receptor antagonist and a potential antipsychotic drug, facilitates NMDA-receptor mediated neurotransmission in the rat medial prefrontal cortical neurons in vitro. Neuropsychopharmacology 3: 197–209
Arvanov VL, Liang X, Schwartz J, Grossman S, Wang RY . (1997): Clozapine and haloperidol modulate NMDA and non-NMDA receptor mediated neurotransmission in rat prefrontal cortical neurons in vitro. J Pharmacol Exp Ther 283: 226–234
Ashby CR Jr, Wang RY . (1990): Effects of antipsychotic drugs on 5-HT2 receptors in the medial prefrontal cortex: Microiontophoretic studies. Brain Res 506: 346–348
Bakshi VP, Swerdlow NR, Geyer MA . (1994): Clozapine antagonizes phencyclidine-induced deficits in sensorimotor gating of the startle response. J Pharmacol Exp Ther 271: 787–794
Berretta N, Jones RSG . (1996): Tonic facilitation of glutamate release by presynaptic N-methyl-D-aspartate autoreceptors in the entorhinal cortex. Neuroscience 75: 339–344
Bleeker ED, Versleger W . (1990): Ritanserin in the treatment of negative symptoms in chronic schizophrenic patients. Abstracts of the 17th Congress of CINP, Kyoto, Japan, Vol. II, p 221
Blue ME, Yagaloff KA, Mamounas LA, Hartig PR, Molliver ME . (1988): Correspondence between 5-HT2 receptors and serotonergic axons in rat neocortex. Brain Res 453: 315–328
Boyce S, Rupniak NMJ, Stevenson MJ, Cook G, Iversen SD . (1991): Psychomotor activity and cognitive disruption attributable to NMDA, but not sigma, interactions in primates. Behav Brain Res 42: 115–121
Breier A, Buchanan RW, Kirkpatrick B, Davis OR, Irish D, Summerfelt A, Carpenter WT Jr . (1994): Effect of clozapine on positive and negative symptoms in outpatients with schizophrenia. Am J Psychiatry 151: 20–26
Bryk A, Raudenbush S . (1992): Hierarchical Linear Models: Applications and Data Analysis Methods. Newbury Park, CA, Sage Publications
Carlsson M, Carlsson A . (1990): Interactions between glutamatergic and monoaminergic systems within the basal ganglia—implications for schizophrenia and Parkinson's disease. Trends Pharmacol Sci 13: 272–276
Cassens G, Inglis A, Appelbaum P, Gutheil T . (1990): Neuroleptics: Effects on neuropsychological function in chronic schizophrenic patients. Schizophr Bull 16: 477–499
Cauli B, Audinat E, Lambolez B, Angulo MC, Ropert N, Tsuzuki K, Hestrin S, Rossier J . (1997): Molecular and physiological diversity of cortical nonpyramidal cells. J Neurosci 17: 3894–3906
Connick JH, Stone TW . (1988): Quinolinic acid effects on amino acid release from the rat cerebral cortex in vitro and in vivo. Br J Pharmacol 93: 868–876
Connors BW, Gutnick MJ . (1990): Intrinsic firing patterns of diverse neocortical neurons. Trends Pharmacol Sci 13: 99–104
Corbett R, Camacho F, Woods AT, Kerman LL, Fishkin RJ, Brooks K, Dunn RW . (1995): Antipsychotic agents antagonize noncompetitive N-methyl-D-aspartate antagonist-induced behaviors. Psychopharmacology 120: 67–74
Danysz W, Wroblewski JT, Costa E . (1988): Learning impairment in rats by N-methyl-D-aspartate receptor antagonists. Neuropharmacol 27: 653–656
Deutsch SI, Mastrpaolo J, Schwartz BL, Rosse RB, Morihisa JM . (1989): A “glutamatergic hypothesis” of schizophrenia: rationale for pharmacology with glycine. Clin Neuropharmacol 12: 1–13
Diggle PJ . (1988): An approach to the analysis of repeated measurements. Biometrics 44: 959–971
Donaldson JO, Baselt RC . (1979): CSF phencyclidine. Am J Psychiatry 136: 1341–1342
Duinkerke SJ, Botter PA, Jansen AA, van Dongen PA, van Haaften AJ, Boom AJ, van Laarhoven JH, Busard HL . (1993): Ritanserin, a selective 5-HT2,1C antagonist, and negative symptoms in schizophrenia. A placebo-controlled double-blind trial. Br J Psychiatry 163: 451–455
Dure LSIV, Young AB . (1995): The distribution of glutamate receptor subtypes in mammalian central nervous system using quantitative in vitro autoradiography. In Stone TW (ed), CNS Neurotransmitters and Neuromodulators: Glutamate. New York, CRC Press, pp 83–94
Farber N, Foster J, Duhan NL, Olney JW . (1996): Olanzapine and fluperlapine mimic clozapine in preventing MK-801 neurotoxicity. Schizophr Res 21: 33–37
Finkel AS, Redman SJ . (1985): Optimal voltage clamping with single microelectrodes. In Smith TG, Lecar A, Redman SJ, Gage PW (eds), Voltage and Patch Clamping with Microelectrodes. Baltimore, Williams & Wilkins, pp 95–120
Fujii DEM, Ahmed I, Jokumsen M, Compton JM . (1997): The effects of clozapine on cognitive functioning in treatment-resistant schizophrenic patients. J Neuropsychiatry 9: 240–245
Gelders Y, VandenBussche G, Reyntjens A, Janssen P . (1986): Serotonin-S2 receptor blockers in the treatment of chronic schizophrenia. Clin Neuropharmacol 9: 325–327
Gleason SD, Shannon HE . (1997): Blockade of phencyclidine-induced hyperlocomotion by olanzapine, clozapine, and serotonin receptor subtype selective antagonists in mice. Psychopharmacology 129: 79–84
Goldberg TE, Weinberger DR . (1994): The effect of clozapine on neurocognition: An overview. J Clin Psychiatry 55 (suppl B):88–90
Goldman-Rakic PS, Selemon LD . (1997): Functional and anatomical aspects of prefrontal pathology in schizophrenia. Schizophrenia Bull 23: 437–458
Hagger C, Buckley P, Kenny JT, Friedman L, Ubogy D, Meltzer HY . (1993): Improvement in cognitive functions and psychiatric symptoms in treatment-refractory schizophrenic patients receiving clozapine. Biol Psychiatry 34: 702–712
Haller E, Binder RL . (1990): Clozapine and seizures. Am J Psychiatry 147: 1069–1071
Halliwell JV, Adams PR . (1982): Voltage clamp analysis of muscarinic excitation in hippocampal neurons. Brain Res 250: 71–92
Hertzman M, Reba RC, Kotlyarove EV . (1990): Single photon emission computerized tomography in phencyclidine and related drug abuse. Am J Psychiatry 147: 255–256
Honey CR, Miljkovic Z, McDonald JF . (1985): Ketamine and phencyclidine cause a voltage-dependent block of responses to L-aspartic acid. Neurosci Lett 61: 135–139
Ingvar DH, Franzen G . (1974): Distribution of cerebral activity in chronic schizophrenia. Lancet 2: 1484–1486
Javitt DC, Zukin SR . (1991): Recent advances in the phencyclidine model of schizophrenia. Am J Psychiatry 148: 1301–1308
Jentsch JD, Tran A, Le D, Youngren KD, Roth RH . (1997a): Subchronic phencyclidine) administration reduces mesoprefrontal dopamine utilization and impairs prefrontal cortical-dependent cognition in the rat. Neuropsychopharmacology 17: 92–99
Jentsch JD, Redmond DB Jr, Elsworth JD, Taylor JR, Youngren D, Roth RH . (1997b): Enduring cognitive deficits and cortical dopamine dysfunction in monkeys after long-term administration of phencyclidine. Science 277: 953–955
Kawaguchi Y, Kubota Y . (1996): Physiological and morphological identification of somatostatin or vasoactive intestinal polypeptide-containing cells among GABAergic cell types in rat frontal cortex. J Neurosci 16: 2701–2715
Kay SR, Sevy S . (1990): Pyramidal model of schizophrenia. Schizophr Bull 16: 537–545
Kehne JH, Baron BM, Carr AA, Chaney SF, Elands J, Feldman DJ, Frank RA, van Giesbergen PLM, McCloskey TC, Johnson MP, McCarty DR, Poirot M, Senyah Y, Siegel BW, Widmaier C . (1996): Preclinical characterization of the potential of the putative atypical antipsychotic MDL 100907 as a potent 5-HT2A antagonist with a favorable CNS safety profile. J Pharmacol Exp Ther 277: 968–981
Keith VA, Mansbach RS, Geyer MA . (1991): Failure of haloperidol to block the effects of phencyclidine and dizocilpine on prepulse inhibition of startle. Biol Psychiatry 30: 557–566
Kim JS, Kornhuber J, Schmid-Burgk W, Holzmuller B . (1980): Low cerebrospinal fluid glutamate in schizophrenic patients and a new hypothesis on schizophrenia. Neurosci Lett 20: 379–382
Kristensen JD, Svensson B, Gordh T . (1992): The NMDA receptor antagonist CPP abolishes neurogenic “wind-up pain” after intrathecal administration in humans. Pain 51: 249–253
Krystal JH, Karper LP, Seibyl IP, Freeman GK, Delaney R, Bremner JD, Heninger GR, Bowers MB Jr, Charney DS . (1994): Subanesthetic effects of the noncompetitive NMDA antagonist, ketamine, in humans: Psychotomimetic, perceptual, cognitive, and neuroendocrine responses. Arch Gen Psychiat. 51: 199–214
Lahti AC, Koffel B, LaPorte D, Tamminga CA . (1995): Subanesthetic doses of ketamine stimulate psychosis in schizophrenia. Neuropsychopharmacology 13: 9–19
Lee MA, Thompson PA, Meltzer HY . (1994): Effects of clozapine on cognitive function in schizophrenia. J Clin Psychiatry 55: 9 (suppl B) 82–87
Lidsky TI, Yablonsky-Alter E, Zuck L, Banerjee SP . (1993): Antiglutamatergic effects of clozapine. Neurosci Lett 163: 155–158
Littell RC, Milliken GA, Stroup WW, Wolfinger RD . (1996): SAS System for Mixed Models. SAS Institute Inc., Cary, NC
Lynch DR, Gallagher MJ . (1996): Inhibition of N-methyl-D-aspartate receptors by haloperidol: Developmental and pharmacological characterization in native and recombinant receptors. J Pharm Exp Ther 279: 154–161
MacDonald JF, Miljkovic Z, Pennefather P . (1987): Use-dependent block of excitatory amino acid currents in cultured neurons by ketamine. J Physiol 58: 251–266
Madison DV, Lancaster B, Nicoll RA . (1987): Voltage clamp analysis of cholinergic action in the hippocampus. J Neurosci 7: 733–741
Malhotra AK, Pinals DA, Weingartner H, Sirocco K, Missar CD, Pickar D, Breier A . (1996): NMDA receptor function and human cognition: The effects of ketamine in healthy volunteers. Neuropsychopharmacology 14: 301–307
Malhotra AK, Pinals DA, Adler CM, Elman I, Clifton A, Pickar D, Breier A . (1997a): Ketamine-induced exacerbation of psychotic symptoms and cognitive impairment in neuroleptic-free schizophrenics. Neuropsychopharmacology 17: 141–150
Malhotra AK, Adler CM, Kennison SD, Elman I, Pickar D, Breier A . (1997b): Clozapine blunts N-methy-D-aspartate antagonist-induced psychosis: A study with ketamine. Biol Psychiat 42: 664–668
Martin P, Waters N, Carlsson A, Carlsson ML . (1997): The apparent antipsychotic action of the 5-HT2A receptor antagonist M100907 in a mouse model of schizophrenia is counteracted by ritanserin. J Neural Transm 104: 561–564
Maura G, Carbone R, Guido M, Pestarino M, Raiteri M . (1991): 5-HT2 presynaptic receptors mediate inhibition of glutamate release from cerebellar mossy fiber terminals. Eur J Pharmacol 202: 185–190
Maurel-Remy S, Bervoets K, Millan MJ . (1995): Blockade of phencyclidine-induced hyperlocomotion by MDL 100907 in rats reflects antagonism of 5-HT2A receptors. Eur J Pharmacol 280: R9–R11
McCormick DA, Connors BW, Lighthall JW, Prince DA . (1985): Comparative electrophysiology of pyramidal and sparsely spiny neurons of the neocortex. J Neurophysiol 54: 782–806
Meltzer HY . (1995): Clozapine: Is another view valid? Am J Psychiatry 152: 821–825
Meltzer HY, Matsubara S, Lee J-C . (1989): Classification of typical and atypical antipsychotic drugs on the basis of dopamine D-1, D-2 and serotonin2 pKi values. J Pharmacol Exp Ther 251: 238–246
Meltzer HY, Thompson PA, Lee MA, Ranjan R . (1996): Neuropsychologic deficits in schizophrenia: Relation to social function and effect of antipsychotic drug treatment. Neuropsychopharmacology 14 (3S):27S–33S
Mengod G, Pompeiano M, Martinez-Mir MI, Palacios JM . (1990): Localization of the mRNA for the 5-HT2 receptor by in situ hybridization histochemistry. Correlation with the distribution of receptor sites. Brain Res 524: 139–143
Moghaddam B . (1994): Recent basic findings in support of excitatory amino acid hypotheses of schizophrenia. Prog Neuro-Psychopharmacol Biol Psychiatry 18: 859–870
Montague PR, Gancayco CD, Winn MJ, Marchase RB, Friedlander MJ . (1994): Role of NO production in NMDA receptor-mediated neurotransmitter release in cerebral cortex. Science 263: 973–977
Okuyama S, Chaki S, Kawashima N, Suzuki Y, Ogawa S, Kumagai T, Nakazato A, Nagamine M, Yamaguchi K, Tomisawa K . (1997): The atypical antipsychotic profile of NRA0045, a novel dopamine D4 and 5-hydroxytryptamine2A receptor antagonist, in rats. Br J Pharmacol 121: 515–525
Olney JW, Farber NB . (1995): Glutamate receptor disfunction and schizophrenia. Arch Gen Psychiatry 52: 998–1007
Pearlson GD . (1981): Psychiatric and medical syndromes associated with phencyclidine (PCP) abuse. Johns Hopkins Med J 148: 25–33
Rosse RB, Mastropaolo J, Sussman DM, Koetzner L, Morn CB, Deutsch SI . (1995): Computerized measurement of MK-801-elicited popping and hyperactivity in mice. Clin Neurophamacol 18: 448–457
Schweitzer P, Madamba S, Champagnat J, Siggins GR . (1993): Somatostatin inhibition of hippocampal CA1 pyramidal neurons: Mediation by arachidonic acid and its metabolites. J Neurosci 13: 2033–2049
Sorensen SM, Kehne JH, Fadayel GM, Humphreys TM, Ketteler HJ, Sullivan CK, Taylor VL, Schmidt CJ . (1993): Characterization of the 5-HT2A antagonist MDL 100907 as a putative atypical antipsychotic: Behavioral, electrophysiological, and neurochemical studies. J Pharmacol Exp Ther 266: 1–8
Swerdlow NR, Bakshi V, Geyer MA . (1996): Seroquel restores sensorimotor gating in phencyclidine-treated rats. J Pharmacol Exp Ther 279: 1290–1299
Tarazi FI, Floriji J, Creese I . (1996): Regulation of ionotropic glutamate receptors following subchronic and chronic treatment with typical and atypical antipsychotics. Psychopharmacology 128: 371–379
Verma A, Moghaddam B . (1996): NMDA receptor antagonists impair prefrontal cortex function as assessed via spatial delayed alternation performance in rats: Modulation by dopamine. J Neurosci 16: 373–379
Wachtel H, Turski L . (1990): Glutamate: A new target in schizophrenia. Trends Pharmacol Sci 11: 219–220
Walberg CB, McCarron MM, Schulze BW . (1983): Quantitation of phencyclidine in serum by enzyme immunoassay: Results in 405 patients. J Anal Toxicol 7: 106–110
Wang RY, Arvanov VL . (1998): M100907, a highly selective 5-HT2A receptor antagonist and a potential atypical antipsychotic drug, facilitates induction of long-term potentiation in area CA1 of the rat hippocampal slice. Brain Res 779: 309–313
Weinberger DR, Berman KF . (1996): Prefrontal function in schizophrenia: Confounds and controversies. Phil Trans R Soc Lond B 351: 1495–1503
Weinberger DR, Berman KF, Zec RF . (1986): Physiologic dysfunction of dorsolateral prefrontal cortex in schizophrenia. I. Regional cerebral blood flow evidence. Arch Gen Psychiatry 43: 114–125
Weinberger DR, Berman KF, Illowsky BP . (1988): Physiologic dysfunction of dorsolateral prefrontal cortex in schizophrenia. III. A new cohort and evidence for a monoaminergic mechanism. Arch Gen Psychiatry 45: 609–615
Weinberger DR, Lipska BK . (1995): Cortical maldevelopment, antipsychotic drugs, and schizophrenia: A search for common ground. Schizophrenia Res 16: 87–110
White IM, Flory GS, Hooper KC, Speciale J, Banks DA, Rebec GV . (1995): Phencyclidine-induced increases in striatal neuron firing in behaving rats: Reversal by haloperidol and clozapine. J Neural Transmission 102: 99–112
Wiesel FA, Nordstrom AL, Farde L, Eriksson B . (1994): An open clinical and biochemical study of ritanserin in acute patients with schizophrenia. Psychopharmacology 114: 31–38
Willins DL, Deutch AY, Roth BL . (1997): Serotonin 5-HT2A receptors are expressed on pyramidal cells and interneurons in the rat cortex. Synapse 27: 79–82
Witkin JM . (1995): Role of NMDA receptors in behavior and behavioral effects of drugs. In Stone TW (ed), CNS Neurotransmitters and Neuromodulators: Glutamate. New York, CRC Press, pp 323–350
Wu JC, Buchsbaum MS, Bunney WE . (1991): Positron emission tomography study of phencyclidine users as a possible drug model of schizophrenia. Jpn J Psychopharmacol 11: 47–48
Yang CR, Seamans JK, Gorelova N . (1996): Electrophysiological and morphological properties of layers V–VI principal pyramidal cells in rat prefrontal cortex in vitro. J Neurosci 16: 1904–1921
Zar JH . (1996): Biostatistical Analysis. Upper Saddle River, NJ, Prentice Hall
Acknowledgements
We thank Dr. J. Schwartz and Mr. S. Grossman for providing help in statistics. We also thank Hoechst Marion Roussel, Sandoz, McNeil Laboratories, and NIDA for providing M100907 and M100009, clozapine, haloperidol, and PCP, respectively. This research was supported by USPHS grants MH-41440.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Wang, R., Liang, X. M100907 and Clozapine, but not Haloperidol or Raclopride, Prevent Phencyclidine-Induced Blockade of NMDA Responses in Pyramidal Neurons of the Rat Medial Prefrontal Cortical Slice. Neuropsychopharmacol 19, 74–85 (1998). https://doi.org/10.1016/S0893-133X(98)00003-7
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1016/S0893-133X(98)00003-7
Keywords
This article is cited by
-
Persistent effects of chronic clozapine on the cellular and behavioral responses to LSD in mice
Psychopharmacology (2013)
-
The role of serotonin in the NMDA receptor antagonist models of psychosis and cognitive impairment
Psychopharmacology (2011)
-
Clozapine, SCH 23390 and α-flupenthixol but not haloperidol attenuate acute phencyclidine-induced disruption of conditional discrimination performance
Psychopharmacology (2007)
-
Potentiation of the NMDA receptor in the treatment of schizophrenia: focused on the glycine site
European Archives of Psychiatry and Clinical Neuroscience (2007)
-
Assessment of NMDA receptor activation in vivo by Fos induction after challenge with the direct NMDA agonist (tetrazol-5-yl)glycine: effects of clozapine and haloperidol
Journal of Neural Transmission (2007)